Neurofibromatosis Type I
Original Editors -Nick Pucillo & Cody Russell from Bellarmine University's Pathophysiology of Complex Patient Problems project.
Top Contributors - Nicholas Pucillo, Cody Russell, Lucinda hampton, WikiSysop, Elaine Lonnemann, Wendy Walker, Kim Jackson and Shaimaa Eldib
Introduction[edit | edit source]
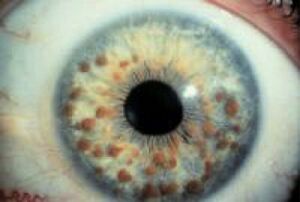
Neurofibromatosis 1 (NF1) is characterized by multiple café au lait spots, axillary and inguinal freckling, multiple cutaneous neurofibromas, iris Lisch nodules, and choroidal (vascular layer of the eye) freckling. About half of people with NF1 have plexiform neurofibromas, but most are internal and not suspected clinically. Learning disabilities are present in at least 50% of individuals with NF1. Less common but potentially more serious manifestations include optic nerve and other central nervous system gliomas, malignant peripheral nerve sheath tumors, scoliosis, tibial dysplasia, and vasculopathy.[1]
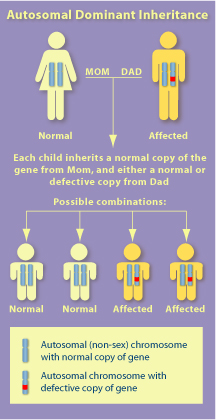
- It is an autosomal dominant disorder on the long arm of chromosome 17. NF1 varies a great deal in presentation and complications, even between immediate family members.[2][3][4]
- Neruofibromatosis type 1 affects approximately 1 in 3,000 peolple worldwide. Neruofibromatosis occurs equally between sexes and races.[5]
- The median life expectancy of individuals with NF1 is approximately eight years lower than in the general population. Malignancy (especially malignant peripheral nerve sheath tumors) and vasculopathy are the most important causes of early death in individuals with NF1.[1]
This is a good 2 minute video on NF1
Characteristics/Clinical Presentation[edit | edit source]
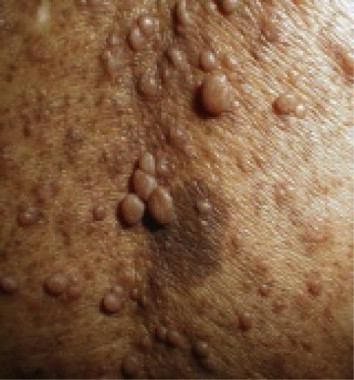
Beginning in early childhood, almost all people with neurofibromatosis type 1 have multiple café-au-lait spots, These spots increase in size and number as the individual grows older. Freckles in the underarms and groin typically develop later in childhood.
Most adults with neurofibromatosis type 1 develop neurofibromas, which are benign tumors that are usually located on/just under the skin.
- They may also occur in nerves near the spinal cord or along nerves elsewhere in the body.
- Some people with neurofibromatosis type 1 develop malignant peripheral nerve sheath tumors that grow along nerves, usually developing in adolescence or adulthood.
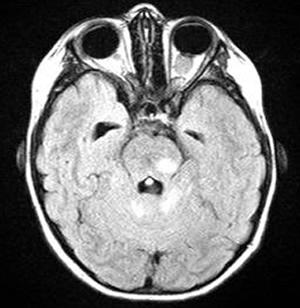
- People with neurofibromatosis type 1 also have an increased risk of developing other cancers, including brain tumors and leukemia.
- During childhood, benign growths (Lisch nodules) often appear in the colored part of the iris), they do not interfere with vision.
- Some with NF1 also develop tumors that grow along the optic nerve (optic gliomas), which may lead to no loss all the way to total vision loss.[2]
Additional signs and symptoms of neurofibromatosis type 1 vary, can include hypertension, short stature, an unusually large head (macrocephaly), and skeletal abnormalities eg scoliosis. Although most people with neurofibromatosis type 1 have normal intelligence, learning disabilities and attention-deficit/hyperactivity disorder (ADHD) occur frequently in affected individuals[2].
Diagnosis[edit | edit source]
The diagnosis of NF1 is usually based on clinical findings. Molecular genetic testing of NF1 is rarely needed for diagnosis.[1]
Etiology/Causes[edit | edit source]
The genetic disorder that is Neruofibromatosis Type 1 originates from the NF1 gene that is located in the long arm of chromosome 17. While the role of the NF1 gene is not fully understood, it is known, however, that it produces the protein product neurofibromin. Neurofibromin indirectly dictates cell growth and division, at especially high levels in the nervous system (predominately as a suppressor). In individuals with Neurofibromatosis Type 1, neurofibromin is not produced in sufficient quantities to inhibit cell growth and thus, neruofibromas form along the nerves. While predominately all neuromas of Neurofibromatosis Type 1 are benign, there is a rare occasion in which a neuroma may be malignant (8-13%, especially so in 20-35 year olds). [3][7]
Management[edit | edit source]
The usual treatment approach for any tumors associated with NF1 is to watch the person closely for signs of tumor growth or whether the person is having such symptoms as pain or weakness ie active surveillance.
- If symptoms develop over time, then surgery may be done to remove the tumor(s). It is usually possible to remove a tumor growing on or from nerves, and to preserve the nerve involved, unless it is a plexiform tumor (more spread out and often get into the nerve).
- A cancerous tumor may be treated with cancer medications, radiation therapy, or a combination of treatments.
- Clinical trials, meaning research studies, for neurofibromatosis are ongoing and currently focus on targeted therapy drugs that affect the ras signaling pathway inside the tumor cell.[8]
Physical Therapy Management[edit | edit source]
- Best practice of physical therapy in individuals with NF1 has not been identified in research. Recognizing and treating impairments that manifest due to the underlying pathology is within our scope and should be considered when evaluating and treating a patient with NF1.
- As a profession it is important to recognize the manifestations and diagnostic criteria of NF1 in order to screen appropriately regarding orthopedic, neurological, cardiovascular, integumentary, and cognitive impairments.
- A series of case reports have been published depicting the benefits of strength training, stretching, postural training, and palliative medicine. [9] [10]
Case Reports/ Case Studies[edit | edit source]
Physical therapy as conservative management for cervical pain and headaches in an adolescent with neurofibromatosis type 1: a case study: www.ncbi.nlm.nih.gov/pubmed/20208466
Effects of a plyometric training program for 3 children with neurofibromatosis type 1.: www.ncbi.nlm.nih.gov/pubmed/22466394
References[edit | edit source]
- ↑ 1.0 1.1 1.2 Friedman JM. Neurofibromatosis 1. 1998 Oct 2 [Updated 2019 Jun 6]. In: Adam MP, Ardinger HH, Pagon RA, et al., editors. GeneReviews® [Internet]. Seattle (WA): University of Washington, Seattle; 1993-2022. Available from: https://www.ncbi.nlm.nih.gov/books/NBK1109/ (accessed 6.3.2022)
- ↑ 2.0 2.1 2.2 medline plus NF1 Available: https://medlineplus.gov/genetics/condition/neurofibromatosis-type-1/(accessed 6.3.2022)
- ↑ 3.0 3.1 Julian N, Edwards NE, DeCrane S, Hingtgen CM. Neurofibromatosis 1: Diagnosis and Management. The Journal for Nurse Practitioners. 2014;10(1):30-35.
- ↑ Genetics Home Reference. Neurofibromatosis type 1. Available at: http://ghr.nlm.nih.gov/condition/neurofibromatosis-type-1. Accessed March 4, 2014].
- ↑ Feldman DS, Jordan C, Fonseca L. Orthopaedic manifestations of neurofibromatosis type 1. J Am Acad Orthop Surg. 2010;18(6):346-57.
- ↑ Neurofibromatosis. Available at:http://www.youtube.com/watch?v=BQBKQB3zq9s
- ↑ Ferner RE, Huson SM, Thomas N, et al. Guidelines for the diagnosis and management of individuals with neurofibromatosis 1. J Med Genet. 2007;44(2):81-8.
- ↑ Cancer net NF1 Available: https://www.cancer.net/cancer-types/neurofibromatosis-type-1 (accessed 6.3.2022)
- ↑ Johnson BA, Salzberg CL, Stevenson DA. Effects of a plyometric training program for 3 children with neurofibromatosis type 1. Pediatr Phys Ther. 2012;24(2):199-208.
- ↑ Helmers KM, Irwin KE. Physical therapy as conservative management for cervical pain and headaches in an adolescent with neurofibromatosis type 1: a case study. J Neurol Phys Ther. 2009;33(4):212-23.