Musculoskeletal Injury Risk Screening
Top Contributors - Wanda van Niekerk, Jess Bell, Kim Jackson, Tarina van der Stockt, Uchechukwu Chukwuemeka and Lucinda hampton
Introduction[edit | edit source]
Screening is a valuable process for athletes and is commonly practised in several elite sports. One of the common elements of a periodic medical assessment of athletes, is the musculoskeletal screening or examination. For many years, physiotherapists have screened athletes with the aim of identifying the athletes at risk for injury, so that they can then implement injury prevention programmes for these athletes. More recently, the focus has, however, shifted from using screening to predict injuries to rather using screening to identify possible predispositions to injury.
Reasons for the Periodic Medical Assessment of Athletes[edit | edit source]
The main reason for the periodic medical assessment of athletes is to safeguard sports participation, but there are many other additional benefits, including:[1][2]
- Identification of medical conditions that contraindicate sports participation
- Assessment of known injuries and illnesses
- Review of current medications and supplements
- Athlete education
- Baseline testing
- Developing rapport with the athlete
- Specific screening
- Cardiac screening
- Screening for unknown illnesses
- Screening for risk factors for future injury
Read more: Screening in sport and Pre-participation Screening
Why Screen for Injury Risk?[edit | edit source]
Injury rates in sports are increasing despite the increased professionalism of sports science and the use of sports medicine support teams. Although participation in sport is encouraged as part of a healthy lifestyle, the sport-related injury burden is high.[3]
Consequences of Injuries in Sport[edit | edit source]
- Financial implications for the club[4]
- The cost of player injuries on sports leagues and organisations mainly fall into two categories: the direct medical costs and the opportunity cost of time loss injuries and shortened careers. This has led to professional teams offering players contracts contingent upon medical evaluations - players with high injury risk may then be offered short-term contracts.[5]
- Team performance[4]
- A significant relationship between injury rates and time-loss with performance in elite team sports is reported.[6]
- Financial implications for the healthcare system
- Financial costs for the individual
- Implications for long term health
- Career progression in sports
Injury Prediction[edit | edit source]
Can we predict injuries? In literature, there is the issue of prediction or association. Most of the available literature looks at retrospective studies where an association between a certain physical factor and an injury is seen, as opposed to using a certain physical factor in a retrospective manner to investigate if it can actually predict an injury.[12]
In recent years, much of the literature on screening tests suggests that these tests are not able to predict which athlete will sustain an injury, so clinicians are moving away from this idea.[13] However, this does not mean that screening should not be performed, as "screening remains essential in our efforts to protect athletes’ health."[14] The following video provides a good explanation on injury risk and screening.
An infographic explaining prediction versus association in sports injuries can be found here.
Factors Involved in the Development of Injuries[edit | edit source]
There are various factors that play a role in the risk of injury occurrence, and these factors can interact with each other:[16]
- Training-related factors
- Training volume, load, intensity
- Type of training
- Training and competition schedule
- Rest
- Motor control factors
- Posture
- Movement patterns
- Muscle tone
- Technique
- Sport specific movements
- Psychological factors[17]
- Beliefs
- Fears
- Coping strategies
- Self-efficacy
- Catastrophising
- Emotional status (stress, depression, anxiety)
- Health-related factors
- Diet
- Medication
- General health
- Fatigue
- Sleep patterns
- Environmental factors
- Training/competition surface
- Equipment
- Clothing
- Weather
- Coaching
- Conditioning factors
- Strength
- Endurance
- Muscle length
- Joint range of motion
- Chronic capacity
- Additional demands
- Home
- Work
- Family
- Social
- Leadership
- Media
- Sponsors
- Other factors
- Sport specific skill level
- Ranking and status
- Goals of athlete – short- and long-term
When considering injury screening, it is important to consider the myriad of factors that can influence injury occurrence. Furthermore, it is unlikely that these can be reduced to a single factor that may lead to injury.[16] Factors that are commonly screened for in musculoskeletal injury risk screening are:
- Strength and conditioning
- Movement quality
- Stability/alignment
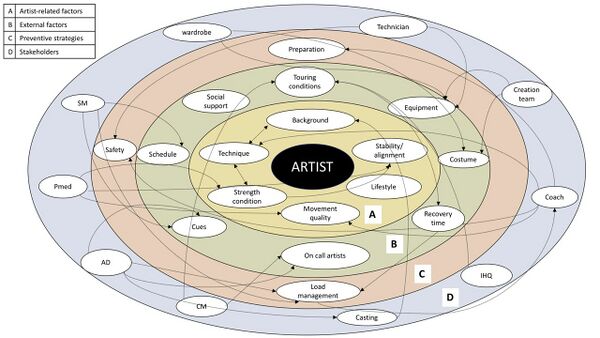
From the map by Bolling et al[18] it is evident that these factors are just a few of the many factors that can be involved in injury occurrence.[18]Athlete-related factors can also include background, technique, lifestyle.[18] External factors can include: recovery time, equipment, social support, schedules.[18] Preventative strategies can include: preparation and load management.[18] See the map below for more detail and read the complete article: From the safety net to the injury prevention web: applying systems thinking to unravel injury prevention challenges and opportunities in Cirque du Soleil.[18]
Predisposition to Injuries[edit | edit source]
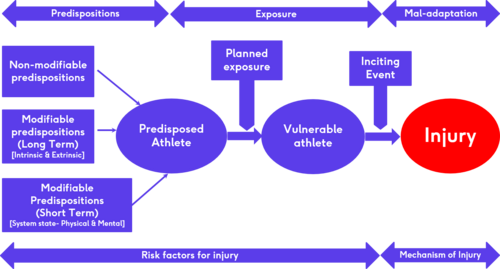
Instead of trying to predict injury occurrence, it may be more appropriate to identify athletes who are predisposed and where possible modify the predisposition.
- Non-modifiable predispositions include:
- Anatomy
- Genetics
- Previous injury
- Environmental factors
- Modifiable predispositions include:
- Strength
- Movement
- Skill
- Flexibility
- State of the athlete e.g. tired or stressed?
This flow diagram created by Dr Lee Herrington illustrates how predispositions and exposure to load can lead to vulnerability in an athlete and, in combination with an inciting event, can lead to injury mechanisms and occurrences.
Considerations in Identifying Predisposed Athletes[edit | edit source]
- Understand the nature of the sport and the injuries occurring
- Common injuries vs catastrophic injuries (for example hamstring injuries vs ACL injuries soccer)
- Identify which injury needs to be targeted as this will determine what type of screening tests will be used
- Do these specific injuries have modifiable factors?
- Are there clearly definable physical qualities related to the injury? Can these modifiable factors be clearly defined in terms of certain physical qualities?
- Can these physical qualities be identified with reliable screening tests?
- Can these physical qualities be influenced, modified or changed? (For example – blue eyes may be a predisposing factor to a certain type of injury and can easily and reliably be screened for, but eye colour cannot be changed, modified or influenced.)
- Traumatic injuries in the sport – how influenceable are traumatic injuries through screening and training?
Screening for Neuromuscular Control of Movement[edit | edit source]
Neuromuscular control is the ability to perform a movement in the best possible way to minimise loading stress or maximise the distribution of loading stresses on the tissue involved.[16] An important part of “movement screening” is to identify the high-risk movement tasks and determine if these tasks can be broken down into closed skills. A closed skill is undertaken in a controlled environment where the athlete only focuses on that specific skill (e.g. single leg squat or single-leg landing).[16] An open skill is undertaken in a very chaotic and random environment (e.g. single-leg landing in the middle of a sporting environment such as competition or match). The context in which these movements take pace will have an influence on performance, as well as the risk for injury. For example, an athlete may pass a closed skill test/task such as single-leg landing at the pre-season screening, but still get injured (i.e. ACL injury) as a result of a single-leg landing in a sporting environment such as a competition.
Selecting a Screening Test/Task[edit | edit source]
Factors to consider when selecting a screening test or task include:[16]
- Nature of activities undertaken in the specific sport
- Nature of the major injuries in the specific sport (are these linked to specific movements or activities?)
- Athlete’s injury history (can previous injuries be linked to specific movements or activities?)
Factors Influencing Neuromuscular Control of Movement[edit | edit source]
Various factors can have an impact on an athlete's ability to perform a specific screening test or task. These include:[16]
- Strength
- Joint range of motion
- Muscle length – flexibility
- Proprioception – joint position sense
- Movement dissociation
- Sport specific skill
Building a Paradigm for Injury Risk Screening[edit | edit source]
- Consider predisposition versus prediction of injuries
- Screening tests cannot predict if an athlete will get injured, but we can screen and look for predisposed athletes. Remember that being predisposed to a certain injury does not mean that an athlete will get injured. Also, if an athlete does not have a predisposition to an injury, this is not a guarantee that the athlete will not be injured. Athletes become vulnerable to injury when they are exposed to load and inciting events (see flow diagram above).
- Identify if force generation, force absorption or movement skill are an issue in predisposition
- Identify the predisposing movement task/s
- Break down the identified movement task into closed skills that can be measured reliably
- If the athlete fails the test/task, identify the reasons for failure
- Build ways to improve the skill in a controlled environment, but then also in training and competition environments
Examples of Screening Tests[edit | edit source]
- Lower quadrant tests
- Upper quadrant tests
- Glenohumeral Internal Rotation Deficit (GIRD)
- Closed chain upper limb test
- Functional Movement Screen (FMS)
- United States Tennis Association High Performance Profile
- Nine Test Screening Battery[19]
- Athletic Ability Assessment[20]
- Boksmart pre-participation screening of players
- This website has various documents that can be downloaded such as the musculoskeletal assessment form and protocol as well as various other assessment documents.
Resources[edit | edit source]
- Risk factors and injury mechanisms in sports injuries
- Rod Whiteley, Sports Physiotherapist. Aspetar. If screening is a waste of time as Roald Bahr tells us, why should you still be doing it?
- Below are two videos you can watch on injury risk screening
References[edit | edit source]
- ↑ Targett S, Clarsen B. Periodic medical assessment of athletes. In: Brukner P, Clarsen B, Cook J, Cools A, Crossley K, Hutchinson M, McCroy P, Bahr R, Khan K. Brukner and Khan's Clinical Sports Medicine: Injuries, Volume 1, 5e. Sydney: McGraw Hill Education. 2017
- ↑ Nabhan D, Taylor D, Lewis M, Bahr R. Protecting the world’s finest athletes: periodic health evaluation practices of the top performing National Olympic Committees from the 2016 Rio or 2018 PyeongChang Olympic Games. British Journal of Sports Medicine. 2021 Sep 1;55(17):961-7.
- ↑ Emery CA, Pasanen K. Current trends in sport injury prevention. Best Practice & Research Clinical Rheumatology. 2019 Feb 1;33(1):3-15.
- ↑ 4.0 4.1 Eliakim E, Morgulev E, Lidor R, Meckel Y. Estimation of injury costs: financial damage of English Premier League teams’ underachievement due to injuries. BMJ Open Sport & Exercise Medicine. 2020 May 1;6(1):e000675.
- ↑ Walia B, Boudreaux CJ. The cost of players’ injuries to professional sports leagues and other sports organizations. Managerial Finance. 2020 Jul 31.
- ↑ Hägglund M, Waldén M, Magnusson H, Kristenson K, Bengtsson H, Ekstrand J. Injuries affect team performance negatively in professional football: an 11-year follow-up of the UEFA Champions League injury study. British journal of sports medicine. 2013 Aug 1;47(12):738-42.
- ↑ 7.0 7.1 Finch CF, Kemp JL, Clapperton AJ. The incidence and burden of hospital-treated sports-related injury in people aged 15+ years in Victoria, Australia, 2004–2010: a future epidemic of osteoarthritis?. Osteoarthritis and cartilage. 2015 Jul 1;23(7):1138-43.
- ↑ Secrist ES, Bhat SB, Dodson CC. The financial and professional impact of anterior cruciate ligament injuries in National Football League athletes. Orthopaedic journal of sports medicine. 2016 Aug 30;4(8):2325967116663921.
- ↑ Poulsen E, Goncalves GH, Bricca A, Roos EM, Thorlund JB, Juhl CB. Knee osteoarthritis risk is increased 4-6 fold after knee injury–a systematic review and meta-analysis. British journal of sports medicine. 2019 Dec 1;53(23):1454-63.
- ↑ Snoeker B, Turkiewicz A, Magnusson K, Frobell R, Yu D, Peat G, Englund M. Risk of knee osteoarthritis after different types of knee injuries in young adults: a population-based cohort study. British journal of sports medicine. 2020 Jun 1;54(12):725-30.
- ↑ 11.0 11.1 Larruskain J, Lekue JA, Martin-Garetxana I, Barrio I, McCall A, Gil SM. Injuries are negatively associated with player progression in an elite football academy. Science and Medicine in Football. 2021 Jun 16(just-accepted)
- ↑ McCall A, Fanchini M, Coutts AJ. Prediction: the modern-day sport-science and sports-medicine “quest for the holy grail”. International journal of sports physiology and performance. 2017 May 1;12(5):704-6.
- ↑ Bahr R. Why screening tests to predict injury do not work—and probably never will…: a critical review. British journal of sports medicine. 2016 Jul 1;50(13):776-80.
- ↑ Verhagen E, van Dyk N, Clark N, Shrier I. Do not throw the baby out with the bathwater; screening can identify meaningful risk factors for sports injuries. British journal of sports medicine. 2018;52(19):1223-4.
- ↑ Clinical Athlete. Injury risk and screening. Available from https://www.youtube.com/watch?v=lvP_KtQf3Xc [last accessed 25/8/2021]
- ↑ 16.0 16.1 16.2 16.3 16.4 16.5 Herrington LC, Munro AG, Jones PA. Assessment of factors associated with injury risk. In: Performance Assessment in Strength and Conditioning 2018 Oct 9 (pp. 53-95). Routledge.
- ↑ Chang C, Putukian M, Aerni G, Diamond A, Hong G, Ingram Y, Reardon CL, Wolanin A. Mental health issues and psychological factors in athletes: detection, management, effect on performance and prevention: American Medical Society for Sports Medicine Position Statement—Executive Summary. British journal of sports medicine. 2020 Feb 1;54(4):216-20.
- ↑ 18.0 18.1 18.2 18.3 18.4 18.5 18.6 Bolling C, Mellette J, Pasman HR, Van Mechelen W, Verhagen E. From the safety net to the injury prevention web: applying systems thinking to unravel injury prevention challenges and opportunities in Cirque du Soleil. BMJ open sport & exercise medicine. 2019 Feb 1;5(1):e000492.
- ↑ Flodström F, Heijne A, Batt ME, Frohm A. The nine test screening battery-normative values on a group of recreational athletes. International journal of sports physical therapy. 2016 Dec;11(6):936.
- ↑ McKeown I, Taylor‐McKeown K, Woods C, Ball N. Athletic ability assessment: a movement assessment protocol for athletes. International journal of sports physical therapy. 2014 Dec;9(7):862.
- ↑ Aspetar. Why screening to predict injury doesn’t work and probably never will. Available from https://www.youtube.com/watch?v=y0HroNZWmT8 [last accessed 19/5/2022]
- ↑ Aspetar. From athlete screening to injury risk management -Prof Roald Bahr. Available from https://www.youtube.com/watch?v=jXWWc3wML3o&t=3s [last accessed 19/5/2022]