Multidisciplinary and Interdisciplinary Management in Cerebral Palsy
Original Editor - Roelie Wolting Top Contributors - Roelie Wolting, Kim Jackson, Leana Louw, Michelle Lee, Laura Ritchie, Shaimaa Eldib, Rucha Gadgil, Rania Nasr, Jess Bell, Admin, Naomi O'Reilly, Simisola Ajeyalemi, Amrita Patro, Evan Thomas and Vidya Acharya
Introduction[edit | edit source]
Children with cerebral palsy present many medical problems that can be treated or prevented.[1] Often, the initial stage of treatment can involve an interdisciplinary team which can consist of a paediatrician, preferably one with experience in neurological developmental disorders, a neurologist (or other neurological practitioner), a mental health practitioner, an orthopaedic surgeon, a physiotherapist, a speech therapist and an occupational therapist.[1][2] Each member of the team has important contributions to make in the care of the affected child.
Here are some of the roles of the multidisciplinary team:
- The physiotherapist evaluates and treats muscle tone, strength and gait (walking).[3]
- The occupational therapist reviews the child's ability to perform tasks of self-help and care - from feeding to manual dexterity.[4]
- The speech therapist evaluates the child's ability to speak, understand speech and communicate.[5]
Each discipline then develops their own intervention plan. The number of people involved may be less and in poly or resourced places less disciplines may be involved.
Physiotherapy Role in Cerebral Palsy Management[edit | edit source]
Physiotherapy helps to increase the strength, muscle endurance and range of motion of children with CP.[6] Physiotherapists’ main aims are to help a child be as mobile and independent as possible. to prevent secondary complications e.g. contractures and chest infections, and to improve the child's quality of life. They also help encourage parents and carers to be involved and are happy to give support and advice on managing problems associated with CP. Physiotherapy can help with stiffness or hypotonia, areas of inactivity, poor control of movement patterns, muscle shortening, contractures and prevention of musculoskeletal deformities.[7] Physiotherapy treatment may involve stretches, strengthening exercises, facilitation of normal movement patterns, advice on postural management, and ways to clear secretions. Physiotherapists also give advice on aids and equipment which may be useful for sitting, standing, walking and getting children involved in everyday activities. Treatment is designed to focus on capabilities, not limitations.
Infant years[edit | edit source]
- Goal setting with family
- Feeding and carrying techniques
- Symmetry limit abnormal movements, midline play
- Encourage the development of functional skills and play
- Sensory-motor development
- Respiratory
- Through School
Medical and Surgical Management[edit | edit source]
There are lots of different medications for CP which can help to reduce symptoms and help with any complications. Drug therapy is used to help control body movements, prevent seizures, relax muscles, and manage pain and many other associated problems.
When choosing which drugs the Consultants or Doctors will consider the benefits and side effects.[8] The most common medications used to treat CP include these categories:
- Anti-cholinergics: to assist with uncontrolled body movements.
- Anti-convulsants: for treatment of seizures.
- Anti-depressants: depression medication.
- Muscle relaxants: to address severe spasms and spasticity.
- Anti-inflammatories: for overuse injury and pain management.
- Laxitives to address constipation.
Surgery may be used to correct problems with bones and joints or muscles and tendons. This tends to be used if there is pain on moving. This can also help to improve the child’s confidence, posture and ability to cope with everyday life. After surgery, an intensive course of physiotherapy will often be required.
An example of a surgery used for children who suffer from severe stiffness in their legs is a SELECTIVE DORSAL RHIZOTOMY. This may only be used after other treatments have failed. It involves cutting some nerves in the spinal column which can help to reduce the stiffness experienced. Extensive physiotherapy will be needed after this type of operation. This will help the child to re-learn how to control their leg muscles.[8]
Models of team practice[edit | edit source]
- In the multidisciplinary approach individuals each approach a situation or problem from their own perspective and then share findings.[2]
- Interdisciplinary teams are similarly interdependent, but efforts are collaborative and team members work together toward a resolution.[12]
- In transdisciplinary teams, disciplinary lines are more blurred and will be explained more in detail below.
Transdisciplinary team[edit | edit source]
A transdisciplinary team is one in which members come together from the beginning to jointly communicate, exchange ideas and work together to come up with solutions to problems. As the prefix "trans" indicates, transdisciplinarity concerns that which is at once between the disciplines, across the different disciplines, and beyond each individual discipline. Transdisciplinary service is defined as the sharing of roles across disciplinary boundaries so that communication, interaction, and cooperation are maximised among team members.[2][13]
This model is seen as a family-friendly approach, operating within a family centered practice model. Families are always members of the team and are respected and valued as equal members. Although all team members participate equally, the family is the final decision-maker.[2][13]
The transdisciplinary team can consist of physiotherapists, occupational therapists, speech therapists, family support workers and educators who work together as a team with the family sharing, learning and working across disciplines, with a key worker for each family to coordinating services. Flexible boundaries and interchangeable roles and responsibilities encourage the exchange of information, knowledge and skills.[2][13]
To be effective each team member needs to be knowledgeable and 'up-skilled' firstly in their own discipline and then in other disciplines (i.e. multi-skilling). Once team members are multi-skilled, the team can 'role release' consistent with the training and expertise of individual member. Role release involves the sharing of expertise. The emphasis is on a more holistic approach in which all team members (including parents) feel comfortable in following through program recommendations across disciplines. It is not possible to work in an effective transdisciplinary model without the upskilling of all staff involved in the teams. This requires management to provide the necessary in-service training time and training for the development of the individuals and teams. Newly-formed teams or ones with relatively inexperienced members will need more time initially. Teams need to work on clear processes and guidelines for assessment and intervention, including feedback to the primary therapist.[2][13]
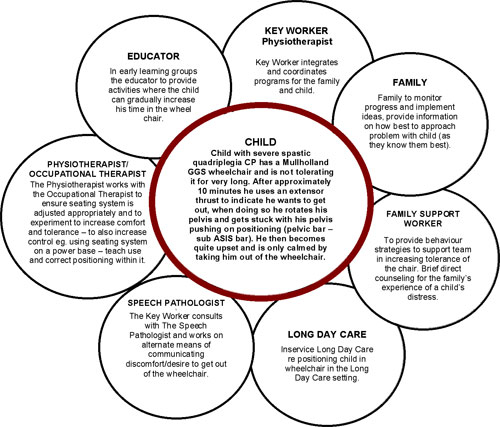
Look at the following image for how a transdisciplinary / multidisciplinary team should look:
The development of a mutual vision among the team and family is one of the most important feature of the transdisciplinary team approach. In addition, team members develop shared meaning about the terminology and principles about disciplines other than their own. This facilitates a shared understanding and good communication for the child, family and team across disciplinary boundaries.[13]
Although all team members may not be involved in direct service delivery for every family, all members are involved in planning and monitoring aspects of intervention. The team works together in an arena assessment where members will take roles either as facilitators or observers / assessors within their own discipline. After assessment and planning, the team meets regularly to share information and to teach and learn across disciplines.[13]
The transdisciplinary approach to service delivery creates a more ideal social situation for genuine inclusion of the family as a 'team member' by appointing a key worker from the outset. The key worker is the primary contact for the team, and it is their role to develop a relationship with the family based on a thorough understanding of their background, situation and needs. There needs to be careful and thoughtful selection of the key worker, taking into consideration the concerns and priorities of the family as much as possible. Ideally, the key worker is chosen in consultation with the family.[15]
The role of the key worker includes advocating with (rather than for) the family within the organisation in order to obtain services and resources within their local community. The key worker also coordinates the assessment process, report and feedback to the family, along with all interventions delivered to the family to meet their needs.[13][15]
Outcomes of transdisciplinary working[edit | edit source]
In low and middle-income countries the team may only consist of the parents (and depending on the age, the child) and a physiotherapist or rehabilitation worker. This puts the heavy responsibility on the shoulder of the professional to become a child-therapist, looking and working beyond the boundaries of the own profession without the back-up and resources of a team.
Research has proven that the transdisciplinary approach gives:[16]
- Positive outcomes for children and families
- Increased parenting capacity
- High parent satisfaction and engagement
- Positive outcomes for staff
Resource allocation[edit | edit source]
Resource allocation is the distribution of resources – usually financial - among competing groups of people or programs. When we talk about allocation of funds for a community-based rehabilitation (CBR) programme, we need to consider three distinct levels of decision-making.[17][18]
- Level 1: Allocating resources to medical rehabilitation services versus other social needs.
- Level 2: Allocating resources within the medical rehabilitation department.
- Level 3: Allocating resources among individual clients.
Use limited resources in the best way possible. This is easy said, but not easy done, but you can only spend it once.
An example is:
A CBR programme in Sri Lanka gets 5000 euro as extra donation, free to spent where most needed. There are many needs within the programme; regular budget is only available to pay staff and rent a building. There are wheelchair adaptations needed for some children with cerebral palsy; the parent association, just starting, needs some training and needs budget for activities; the programme would like to have wheelchairs and walkers in different sizes and shapes in stock which people can borrow or rent.
A qualitative study exploring the facilitators and barriers of active participation of caregivers in the rehabilitation of children with CP in Kano, Nigeria, concludes that there is a need to identify the facilitators and barriers of active involvement of caregivers. Also, rehabilitation services should be accessible and economically sustainable[19].
Whether you are working in a community programme or in a hospital or in a rehabilitation centre: financial resources are always a difficult issue. Do you spend it on people (more staff), do you spend it in people (capacity building), do you spend it on stones (buildings), do you spend it on high-tech equipment (Otto Bock, imported stuff) or on local made equipment; do you want to spend it on a "rolls royce" (imported electric wheelchair) or spend it on many local made tricycles?
Working as a transdisciplinary team (which includes parents and/or people with disabilities) has for resource allocation a lot of advantages:[16][18]
- People do not look just at their own needs, but are used to think with others and so understand needs in other areas better
- The team is already working together to look together for solutions
- It prevents spending money on the “hobby” of one specialist
Conclusion[edit | edit source]
The ultimate proof of all global and national efforts will be local, the test being whether every child with a disability enjoys her or his rights – including access to services, support and opportunities – on a par with other children, even in the most remote settings and the most deprived circumstances.
In The State of the World’s Children 2013: children with disability UNICEF gives 9 key recommendations to realise the promise of equity through inclusion.
Additional Resources[edit | edit source]
References[edit | edit source]
- ↑ 1.0 1.1 Dormans JP, Pellegrino L. Caring for Children with Cerebral Palsy: A Team Approach. Paul H. Brookes Publishing Company, Baltimore, MD 21285-0624; 1998.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 Trabacca A, Vespino T, Di Liddo A, Russo L. Multidisciplinary rehabilitation for patients with cerebral palsy: improving long-term care. Journal of multidisciplinary healthcare 2016;9:455.
- ↑ Anttila H, Autti-Rämö I, Suoranta J, Mäkelä M, Malmivaara A. Effectiveness of physical therapy interventions for children with cerebral palsy: a systematic review. BMC pediatrics 2008;8(1):14.
- ↑ Steultjens EM, Dekker J, Bouter LM, Van De Nes JC, Lambregts BL, Van Den Ende CH. Occupational therapy for children with cerebral palsy: a systematic review. Clinical rehabilitation 2004;18(1):1-4.
- ↑ Pennington L, Goldbart J, Marshall J. Speech and language therapy to improve the communication skills of children with cerebral palsy. Cochrane Database of Systematic Reviews 2004(2).
- ↑ Patel DR, Neelakantan M, Pandher K, Merrick J. Cerebral palsy in children: a clinical overview. Transl Pediatr. 2020;9(Suppl 1):S125-S135.
- ↑ KIDS PHYSIOTHERAPY., 2011. Assessment and treatment. [online].[viewed 14 November 2014]. Available from: http://www.kidsphysiotherapy.co.uk/kids-physiotherapy-assessment-treatment
- ↑ 8.0 8.1 RITTER, T. (1998) Children with cerebral palsy: a parent's guide. Ed Elaine Geralis; Woodbine House
- ↑ Patrick McCallum. Botox/ Phenol Injections for CP Before and After. Available from: http://www.youtube.com/watch?v=HdClr2s4j_g [last accessed 07/08/16]
- ↑ Gillette Children's Specialty Healthcare. WARNING: Graphic Medical Procedure - Selective Dorsal Rhizotomy Surgery. Available from: http://www.youtube.com/watch?v=lsaNdElpmQw [last accessed 07/08/16]
- ↑ back2you2. Before and After Selective Dorsal Rhizotomy- Carter's Journey. Available from: http://www.youtube.com/watch?v=blvi_UcANA0 [last accessed 07/08/16]
- ↑ Loisel P, Durand MJ, Baril R, Gervais J, Falardeau M. Interorganizational collaboration in occupational rehabilitation: perceptions of an interdisciplinary rehabilitation team. Journal of Occupational Rehabilitation 2005;15(4):581-90.
- ↑ 13.0 13.1 13.2 13.3 13.4 13.5 13.6 Woodruff G, McGonigel MJ. Early Intervention Team Approaches: The Transdisciplinary Model. 1988.
- ↑ Australian institute for family studies. Rural beginning team. Available from:http://www.aifs.gov.au/cafca/ppp/profiles/itg_rural_be/ginnings_team.html (accessed 1 July 2019).
- ↑ 15.0 15.1 Rosen C, Miller AC, Pit-ten Cate IM, Bicchieri S, Gordon RM, Daniele R. Team approaches to treating children with disabilities: a comparison. Archives of physical medicine and rehabilitation 1998;79(4):430-4.
- ↑ 16.0 16.1 Mullins LL, Keller JR, Chaney JM. A systems and social cognitive approach to team functioning in physical rehabilitation settings. Rehabilitation Psychology 1994;39(3):161.
- ↑ Murchland S, Wake-Dyster W. Resource allocation for community-based therapy. Disability and rehabilitation 2006;28(22):1425-32.
- ↑ 18.0 18.1 University of Minnesota. Definition: What is resource allocation? Available from: https://www.ahc.umn.edu/img/assets/25857/resource_allocation.pdf (accessed 07 July 2019).
- ↑ Abdullahi A, Isah A. Caregiver’s perspectives on facilitators and barriers of active participation in cerebral palsy rehabilitation in North West Nigeria: a qualitative study. BMC Health Services Research. 2020 Dec;20(1):1-9.