Models of Foot Function
Original Editor - Mariam Hashem
Top Contributors - Mariam Hashem, Tarina van der Stockt, Jess Bell, Kim Jackson, Simisola Ajeyalemi and Claire Knott
Introduction[edit | edit source]
There are many theories on how the ankle foot complex functions in weight bearing and non weight bearing tasks. However, because the foot structure is so complex, it has been difficult to model the foot.[1] Thus, some theories of foot function are outdated and others are in need of further investigations.[2]
This challenges clinical practice and complicates the assessment and management process. It is important to not just understand the models of foot function, but also to be critical and develop questions in regards with their applicability and functionality. Four models will be discussed in this page: Root theory, Sagittal Plane Facilitation Theory, Subtalar Joint Axis Location and Rotational Equilibrium Theory, and the Tissue Stress Model.
Root Theory[edit | edit source]
The root theory was originally developed by Dr.Merton L. Root during the late 1950s through early 1960s. It is also known as “the foot morphology theory,” “the subtalar joint neutral theory,” or simply “Rootian theory”[3]. The root theory is based on a series of static measurements that is believed by the author to predict kinematic function. In order for the foot to be normal, the subtalar joint (STJ) should be in neutral position with the midtarsal joint fully locked,[4] this occurs between mid-stance and heel-off during walking[5]. Any deviations from the stated STJ alignment is considered to be abnormal and should, therefore, exhibit mechanical dysfunction.
It is a popular method, used in the design of foot orthoses for flexible flatfoot deformities.[6] However, despite its clinical popularity and being utilised in much podiatry and orthopedic literature, the root theory is questioned with regards to its reliability, validity and practicality[3][5]. In the 1950s and 60s advanced measuring equipment wasn't available. In addition, most of the research done using this method has been conducted with techniques different from those proposed by Dr. Root. It is also worth to note that Dr. Root has prescribed orthotics in his practice, but the exact methods weren't published or documented, therefore, interpretations of such methods cannot be reliable.[3]
A 2017 study by Jarvis et al.[7] was conducted to investigate foot kinematics between normal and abnormal feet classified according to Root et al, determine if the degree of structural deformity is associated with the degree of compensations and finally to measure subtalar joint position during gait in pain free feet. The results of the kinematic analysis of this study reported no association between the deformities proposed by Root et al. and the differences in foot kinematics during gait. STJ inversion in neutral calcaneal standing position (NCSP ) has no relation to rearfoot kinematics, this means that the clinical use of “subtalar joint neutral” might not provide clinicians with realistic information. Jarvis et al also found the first MPJ dorsiflexion during gait propulsion much less than 65°as proposed by Root. It is evident that not all feet with structural deformities should exhibit symptoms and their function will be affected, therefore the root's classification seems to be invalid and believed to be no longer suitable for professional practice. A simple explanation of why static assessment doesn't necessary reflect kinematic characteristics is that it is taken in non-weight bearing position which may not mimic the applied external and muscular force in weight bearing.
Watch this video if you want to learn more:
Sagittal Plane Facilitation Theory[edit | edit source]
The center of the body mass translates anteroposteriorly during each step. For this to occur, approximately 75° of the step motion is required during the single limb support and about 15° of simultaneous internal and external rotation of the weight bearing side. Therefore, the amount of sagittal plane motion required with every step is 500% that of transverse or frontal plane motion.
For the motion to be transmitted smoothly and efficiently through the sagittal plane, the movement passes through three pivotal sites:
- The rocker bottom side of the calcaneum, to allow motion from heel strike to forefoot contact.
- 10° dorsiflexion of tibia on talus prior to heel-off.
- Metatarsophalangeal joints rocker are the final pivotal site with heel-off, providing foot stability through the windlass mechanism.
Based on this, the sagittal plane movement could be affected by three types of blockages:
- Ankle equinus, or limited weight bearing ankle dorsiflexion to 10° or less[9]
- Forefoot equinus, or a lower forefoot on the ground plane relative to the heel.
- Loss of metatarsophalangeal joints motion that could be structural or functional as in hallux limitus or hallux rigidus. In functional hallux limitus, there is a relationship between hallux dorsiflexion and first metatarsal plantarflexion. The dorsiflexion restriction is limited to weight bearing positions. Because other structures may get involved to compensate the insufficient movement, it makes it hard to be detected by clinical gait observation (occurs for a very short time 100 msec)[10]. The loss of MTP movement can possibly explain late-midstance excessive foot pronation, the timing and direction of knee and hip motion, and improper flexion motions of the torso[11].
In order to understand compensations of the lower limb, Howard Dananberg explained the lower limb joints functioning as a scissor-jack. The hip, knee, ankle, and MTP joints all extend and flex in an opposite direction from their adjacent joints. Restriction in the movement specific to propulsion during gait at any level will consequently affect the other joints and compensations will be required to occur either proximally and/or distally. For example, limited hip extension was found to be associated with functional hallux limitus[12].
Dysfunction of foot mechanisms can be compensated by: apropulsive gait with delayed heel lift-off after contralateral foot contact, vertical lift of the foot off the supporting surface, the avoidance of first ray loading by adopting inversion and loading of the lateral column of the foot, propulsion with foot adduction or abduction and flexed body posture[10].
The sagittal plane facilitation theory role is highlighted in the conservative treatment of functional hallux limitus by facilitating plantarflexion and eversion movement at the first metarsal level with hallux dorsiflexion[10].
The Dananberg theory was further confirmed by Nester et al[13]. The study measured the 3D kinematics using a 6 segment model; leg, calcaneus, midfoot (navicular and cuboid), lateral forefoot (fourth and fifth metatarsals), medial forefoot (first metatarsal) and hallux (Salford foot model) in a population of 100 pain free aged 18-45. They reported high variations in kinematic data and multi articular mechanism that result from interaction of all three body planes, however, the greatest contribution was notes at the sagittal plane from the ankle and sub talar joints (calcaneus-tibia in our data) and the hallux-medial forefoot joint.
Swing phase kinematics were also highlighted in this study. It comprised primarily of dorsiflexion (except for the hallux), eversion and abduction, especially at the lateral and medial forefoot-midfoot joints. These movements resulted from both active muscle forces (e.g. concentric action of anterior tibialis and long toe extensor muscles) and passive elastic forces, e.g. plantar flexion of the hallux after toe off due to elastic energy stored in the plantar facia and long toe flexor muscle/tendons during propulsion. Passive forces are necessary to control the active forces, prepare a safe next step and avoid injuries.
Subtalar Joint Axis Location and Rotational Equilibrium Theory[edit | edit source]
The oblique triplanar orientation of the subtalar joint (STJ) allows pronation and supination of the foot. Pronation is important during weight bearing activities to allow foot adaptation to irregular surfaces, while supination increases stability in the sagittal plane in the propulsive phase of the gait.
The STJ plays a significant role in hindfoot movement and posture in the frontal plane.[14] It is a complex joint that is believed to have multiple axes of rotation that depends on the joint's rotational position. Determining the spatial location of the STJ axis was investigated by several authors[15][16][17][18], their work suggests that the anatomical structure of the articulating surfaces; talus and calcaneus, integrate with each other in a three-dimentional relationship within the STJ range of motion to determine the spatial location of the STJ[19]. In a study by Manter[15], the average STJ axis was placed in a 16° angulation from the sagittal plane and 42° from the transverse plane. However, other researchers found great variations between individuals in the STJ axis angulation in the sagittal and in the medial and/or lateral position directions in relation to the plantar foot.
The weight bearing structures of the foot are: the medial calcaneal tubercle, the first through the fifth metatarsals and the base of the fifth metatarsal. Ground reaction force (GRF) and muscles (the posterior tibial, gastrocnemius, soleus, anterior tibial, flexor hallucis longus, and flexor digitorum longus) acting on the medial tubercle causes supination of the STJ. The opposite is true for GRF and muscles (the peroneus brevis, peroneus tertius, and extensor digitorum longus) exerting forces over the second through fifth metatarsals and the fifth metatarsal base cause pronation of the subtalar joint. On the other hand, Intrinsic muscles cannot produce either pronation or supination moments directly, since none of them cross the STJ. Their effect becomes prominent in resisting deformities and stabilising the subtalar joint[19]. Regardless of the force location, rearfoot or forefoot, acting medial or lateral to the subtalar joint it produces supination or pronation.
Watch this video if you want to learn more:
The palpation method is used to determine the axis of the STJ.
| [22] | [23] |
Normally, in relaxed bipedal stance, the STJ is slightly pronated from neutral with its axis passing through the postero-lateral calcaneus. A medial deviation in the STJ axis is likely to increases the pronation moment, resulting in pronated foot in standing. On the other hand, when the axis deviates laterally the supination moment increases and the foot is displaced neutrally or in supination[19].
Based on this, any translation or deviation (as little as 1-2 mm) from the spatial location of the subtalar joint axis from the normal position will result in changes in moment arm lengths of the attached muscles and eventually disturb the STJ balance and the loading forces and patterns acting on foot and lower extremity during weight bearing activities[19].
Medially deviated subtalar joint can be identified clinically by three characteristics:
- A convex shaped midfoot at the transverse plan, seen from above.
- A more medially positioned and internally rotated soft-tissue contour of the talar head and neck in relation to the calcaneus, also seen from above.
- A concavity in the medial midfoot and anterior t the medial malleolus, viewd from behind.
The medial longitudinal arch height might be normal or lower than normal. These feet will tend to have increased compression of interosseous forces between lateral process of the talus and the floor of the sinus tarsi. Medially deviated STJ is associated with conditions as: plantar fasciitis, hallux limitus, second metatarsophalangeal joint capsulitis, abductor hallucis muscle strain, sinus tarsi syndrome, posterior tibial tendinopathy, posterior tibial tendon dysfunction, medial tibial stress syndrome, chondromalacia patellae, and pes anserinus bursitis.
Lateral deviation of STJ is less common. It is more evident at the rearfoot than the forefoot in STJ palpation technique. GRF and muscular force will increased magnitude of STJ supination moment and decrease that of pronation.
Clinical characteristics:
- From above: concave medial border of the midfoot
- The shape of the talar head and neck at the anterior ankle area will be more laterally positioned than normal
- From posterior: increased concavity in the medial mallelous
- Higher than normal longitudinal arch and pes cavus deformity
- During standing, one or both of the peroneal tendons may be under tension (Bowstring) when observed from the side
The peroneal muscle tension is neccessary to counteract the excessive STJ supination moment to prevent the invidual from walking on the lateral aspect of the feet and also to prevent inversion ankle sprains. Inversion ankle sprains and peroneal tendinopathy are both associated with laterally deviated STJ[19].
Tissue Stress Model[edit | edit source]
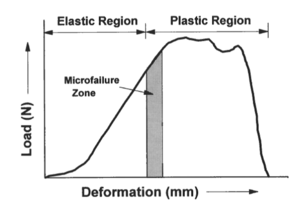
This theory was considered by researchers and clinicians in the management of foot conditions as an alternative to the root theory. It could be explained using the load deformation curve. Consisting of two regions; an elastic region and a plastic region. The area separating the elastic and plastic regions is considered the microfailure zone. the first region represent the area of normal tissue elasticity or the "give-and-take" of soft tissues, where regular loading and unloading occurs without inflammation or at tolerable level. Increasing levels of activity, deformation could occur beyond the zone of microfailure in the plastic region resulting in overuse injuries. Levels of tolerance are different among individuals according to their level of function and daily activities[5].
Assessment and Management[edit | edit source]
Based on the tissue stress model, the aims of examination are:
- Identify over stressed tissue through history, symptoms and subjective examination methods.
- Apply controlled stress to further test injured tissue by: weight bearing and non-weight bearing tests, as well as palpation, range of motion, and muscle function/strength assessment.
- Based on the evaluative findings, determine if the cause of the symptoms is secondary to excessive mechanical loading.
Build your management protocol with the aim of:
- Reducing tissue stress to a tolerable level through rest, footwear, and foot orthoses;
- Promote tissue healing using soft tissue mobility techniques;
- Restore flexibility and muscle strength to facilitate recovery
Clinically relevant tests[edit | edit source]
Navicular drop test: a positive test along with tibial bending varus stress are associated with medial tibial stress syndrome, particularly in runners (although this test does not reflect the foot's dynamic motion during weight-bearing activities[25]).
Single leg squat test: is able to detect patellofemoral pain syndrome.
Supination resistance test: used by orthotists and podiatrists for orthotics and foot cast modeling to determine the appropriate amount of force needed for correction[26].
Jack test[27]: to measure hallux dorsiflexion - relevant to sagittal plane facilitation theory.
Knee to wall (Lunge test)
| [28] | [29] |
| [30] | [31] |
Outcome measures[edit | edit source]
Case Study[edit | edit source]
A 29-year-old female college student presents with left heel pain for the past 2 months. Radiographic examination was negative. Her symptoms started one week after she began working as a waitress (standing 10-12 hours daily, 5 days a week). Before this job, the patient stated that she had a sedentary office job. Her current pain has become worse over the past 4 weeks particularly in the morning and resolves after 20-30 minutes of activity. It then starts again after 3-4 hours of constant walking and standing. the pain is relieved whenever she sat down for rest but revisits again as she stands up and resume working.
The area of most pain was anterior and medial to the bottom of the heel. It is the first time for her to experience similar pain. her physician prescribed anti-inflammatory. When her footwear was examined, they were found to be extremely worn as well as poor fitting. The patient is also slightly overweight.
From the history examination: it seems that this patient has over stressed her plantar fascia, resulting in tissue inflammation.The increased activity level (from sedentary job to a relatively demanding weight bearing job) appears to be related to the onset of symptoms.
A moderate genuvalgum was noted bilaterally and excessive pronation. The patient was then asked to walk approximately 15 feet independently. She demonstrated a slight antalgic gait with minimal decrease in weight bearing on the left foot. Her ROM of the STJ, midtarsal articulations, MTPJ extension were normal and painless. Palpation over the anterio-medial aspect of the left calcaneus triggered marked discomfort. The windlass effect over the plantar fascia was tested by passively extending the first MTPJ from standing and was associated with a slight discomfort after 45" of extension
These clinical tests aims to stress the involved tissue in both weight-bearing and nonweight-bearing positions.
Based on the evaluative findings, plantar fasciitis is caused by excessive mechanical loading resulting in over stressed tissue of the plantar aponeurosis. At this stage, the use of foot orthoses to reduce tissue stress might help with symptom-modulation. However, a more effective strategey should be integrated to correct pronation on the long term.
Management Approach:
A- For short-term/immediate stress reduction:
- The patient was asked to amend her working schedule to decrease the consecutive working hours.
- Invest in a proper footwear with cushioned midsoles, leather uppers with at least 5 to 6 eyelets, and a firm heel counter to assist in controlling excessive foot pronation
- Immediate use of over-the-counter foot orthoses or have her foot strapped with adhesive tape to control the amount of foot pronation
B- Symptomatic relief treatment is introduced once tissue stress is reduced. This include; modalities, soft tissue mobilisation, and massage.
C- Prevent recurrence of plantar fascia e.g; soft tissue mobility exercises to facilitate restricted the 1st MTPJ extension and strengthening exercises of the intrinsic and extrinsic muscles of the leg and foot to provide dynamic stabilisation. The patient was also given recommendations to see a dietitian regarding a weight control program.
Conclusion[edit | edit source]
The models of foot function face uncertainty and there is still a gap between research and practice that needs to be addressed. Although the root theory has been doubted and questioned, it is still hasn't faded in the clinical use and in the research. Can we assume that this theory has become an accepted 'clinical function'despite being considered as a clinical fiction[3]?
Until research comes with answers, it is important to keep an open mind and consider various philosophies in the realm of evidence.
Recources[edit | edit source]
Interview with Kevin Bruce about the role of the podiatrist in the multidisciplinary MSK team in managing conditions of the foot and ankle and he provides his perspective on the latest developments in orthotic use and treatments
References[edit | edit source]
- ↑ Williams LR, Ridge ST, Johnson AW, Arch ES, Bruening DA. The influence of the windlass mechanism on kinematic and kinetic foot joint coupling. J Foot Ankle Res. 2022 Feb 16;15(1):16.
- ↑ Leardini A, Caravaggi P, Theologis T, Stebbins J. Multi-segment foot models and their use in clinical populations. Gait & Posture. 2019;69:50-9.
- ↑ 3.0 3.1 3.2 3.3 Harradine P, Gates L, Bowen C. If it doesn't work, why do we still do it? The continuing use of subtalar joint neutral theory in the face of overpowering critical research. journal of orthopaedic & sports physical therapy. 2018 Mar;48(3):130-2.
- ↑ Root ML. Normal and abnormal function of the foot. Clinical biomechanics. 1977;2.
- ↑ 5.0 5.1 5.2 McPoil TG, Hunt GC. Evaluation and management of foot and ankle disorders: present problems and future directions. Journal of Orthopaedic & Sports Physical Therapy. 1995 Jun;21(6):381-8.
- ↑ Hajizadeh M, Desmyttere G, Ménard AL, Bleau J, Begon M. Understanding the role of foot biomechanics on regional foot orthosis deformation in flatfoot individuals during walking. Gait Posture. 2022 Jan;91:117-125.
- ↑ Jarvis HL, Nester CJ, Bowden PD, Jones RK. Challenging the foundations of the clinical model of foot function: further evidence that the root model assessments fail to appropriately classify foot function. Journal of foot and ankle research. 2017 Dec;10(1):7.
- ↑ Many Inaccuracies in Root Biomechanics Theory. Available from: https://www.youtube.com/watch?v=rDcG224Zqi4
- ↑ Gatt A, De Giorgio S, Chockalingam N, Formosa C. A pilot investigation into the relationship between static diagnosis of ankle equinus and dynamic ankle and foot dorsiflexion during stance phase of gait: Time to revisit theory? Foot (Edinb). 2017;30:47-52.
- ↑ 10.0 10.1 10.2 Petcu D, Colda A. Foot Functioning Paradigms. Proceedings of the Romanian Academy. 2012 Jan 4:212-7.
- ↑ Dananberg HJ. Sagittal plane biomechanics. American Diabetes Association. Journal of the American Podiatric Medical Association. 2000 Jan;90(1):47-50.
- ↑ Dananberg HJ. Lower extremity mechanics and their effect on lumbosacral function. SPINE-PHILADELPHIA-HANLEY AND BELFUS-. 1995;9:389-.
- ↑ Nester CJ, Jarvis HL, Jones RK, Bowden PD, Liu A. Movement of the human foot in 100 pain free individuals aged 18–45: implications for understanding normal foot function. Journal of foot and ankle research. 2014 Dec;7(1):51.
- ↑ Peña Fernández M, Hoxha D, Chan O, Mordecai S, Blunn GW, Tozzi G et al. Centre of Rotation of the Human Subtalar Joint Using Weight-Bearing Clinical Computed Tomography. Sci Rep. 2020;10:1035.
- ↑ 15.0 15.1 Manter JT. Movements of the subtalar and transverse tarsal joints. The Anatomical Record. 1941 Aug;80(4):397-410.
- ↑ Root ML, Weed JH, Sgarlato TE, Bluth DR. Axis of motion of the subtalar joint. J Am Podiatry Assoc. 1966;56(4):149-55.
- ↑ van Langelaan EJ. A kinematical analysis of the tarsal joints. An X-ray photogrammetric study. Acta orthopaedica Scandinavica. Supplementum. 1983;204:1.
- ↑ Benink RJ. The constraint-mechanism of the human tarsus: a roentgenological experimental study. Acta Orthopaedica Scandinavica. 1985 Jan 1;56(sup215):1-35.
- ↑ 19.0 19.1 19.2 19.3 19.4 Kirby KA. Subtalar joint axis location and rotational equilibrium theory of foot function. Journal of the American Podiatric Medical Association. 2001 Oct;91(9):465-87.
- ↑ Subtalar Joint Axis Spatial location changes with subtalar joint rotational motions. Available from: https://www.youtube.com/watch?v=6yHMuLunyTo
- ↑ Importance of rotational equlibrium in subtalar joint kinematics. Availbale from: https://www.youtube.com/watch?v=warWUdHE96k
- ↑ Subtalar joint axis palpation technique. Available from: https://www.youtube.com/watch?v=nQxdVKf_qXU
- ↑ Kevin Kirby. Patient D Clinician Ann STJ Axis Palpation. Available from:https://www.youtube.com/watch?v=McVNIxWdjpY
- ↑ Development of soft tissue theory. Available from: https://www.youtube.com/watch?v=nQxdVKf_qXU
- ↑ Akuzawa H, Oshikawa T, Nakamura K, Kubota R, Takaki N, Matsunaga N, Kaneoka K. Difference in the foot intersegmental coordination pattern between female lacrosse players with and without a history of medial Tibial stress syndrome; a cross-sectional study. J Foot Ankle Res. 2022 Jan 31;15(1):8.
- ↑ Noakes H, Payne C. The reliability of the manual supination resistance test. Journal of the American Podiatric Medical Association. 2003 May;93(3):185-9.
- ↑ Sánchez-Gómez R, Becerro-de-Bengoa-Vallejo R, Losa-Iglesias ME, Calvo-Lobo C, Navarro-Flores E, Palomo-López P, et al. Reliability study of diagnostic tests for functional hallux limitus. Foot Ankle Int. 2020 Apr;41(4):457-62.
- ↑ what a single leg assessment can tell you. Available from:https://www.youtube.com/watch?v=A9pi7_JRgwQ
- ↑ the navicular drop test. Available from:https://www.youtube.com/watch?v=BejuNMmD7-Y
- ↑ supination resistance test. Available from:https://www.youtube.com/watch?v=XfwpgKD_1MM
- ↑ assessing foot flexibility toe raise (jack test). Available from: https://www.youtube.com/watch?v=R1AGYMt329k
- ↑ the weight bearing lunge test. Available from:https://www.youtube.com/watch?v=U7woPNLUT3Q