Metabolic Syndrome
Original Editor - Lucinda hampton
Top Contributors - Lucinda hampton, Uchechukwu Chukwuemeka and Kim Jackson
Introduction[edit | edit source]
Metabolic syndrome (MetSyn) is a cluster of conditions that occur together, increasing your risk of CAD, stroke, and type 2 diabetes. These conditions include hypertension, high blood sugar, excess body fat around the waist, and abnormal cholesterol or triglyceride levels. The main diagnostic components are reduced HDL-cholesterol, raised triglycerides, blood pressure, and fasting plasma glucose; all of which are related to weight gain, specifically intra-abdominal/ectopic fat accumulation and large waist circumference[1].
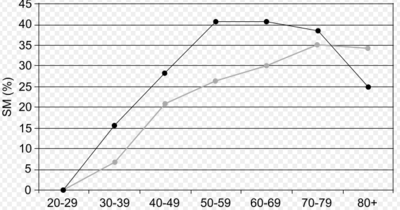
MetSyn prevalence is present in approximately 25% of all adults with increased prevalence in advanced ages. The presence of one component of MetSyn increases the risk of developing MetSyn later in life and likely represents a high lifetime burden of cardiovascular disease risk[2]. Metabolic syndrome now affects 30–40% of people by age 65, driven mainly by adult weight gain, and by a genetic or epigenetic predisposition to intra-abdominal/ectopic fat accumulation related to poor intra-uterine growth. The prevalence of the metabolic syndrome and cardiovascular disease is expected to rise along with the global obesity epidemic: greater emphasis should be given to effective early weight-management to reduce risk in pre-symptomatic individuals with large waists[3][4].
Aetiology[edit | edit source]
Development of metabolic syndrome depends on two elements:
- Adult weight gain, with body fat accumulation
- A predisposition to locate fat in intra-abdominal sites, including ectopic fat in the liver, pancreas, and heart.
- The metabolic syndrome is strongly linked to a lifestyle characterized by easy access to an unlimited supply of high caloric, low nutrient-dense foods, and physical inactivity. This exposure is most potent during the early period of life resulting in childhood obesity which is a major risk for metabolic syndrome in adults.
- Psychosocial stress has also been suggested to contribute, with most metabolic components being more prevalent in socioeconomically deprived populations.
- Not all individuals go on to develop the metabolic syndrome because of the high individual variation and genetic/epigenetic factors are thought to contribute eg. insulin resistance and dyslipidaemia and body composition, their expression varying with changes in the external environment.
- The lifestyle factors that increase intra-abdominal fat and metabolic risk factors are weight gain, a diet high in saturated fat, smoking, inactivity, and excess alcohol intake.
- The predisposition to deposit excess body fat in intra-abdominal and ectopic sites appears mainly to be determined very early in life. Poor intra-uterine growth is a recognized factor, suggesting an epigenetic mechanism (epigenetics - the study of heritable changes caused by the activation and deactivation of genes without any change in DNA sequence[5]).
- There is scattered evidence for other exposures during pregnancy or early infancy, for example, maternal smoking.
- Aside from certain drug effects (e.g. antiretroviral agents promote central fat accumulation, thiazolidinediones reduce it), there is little evidence that any factors in later life can modify fat distribution[3].
Pathophysiology[edit | edit source]
- High plasma glucose and insulin resistance
- Some of the links between components of the metabolic syndrome relate to insulin resistance, although about a third of patients with the metabolic syndrome have normal insulin sensitivity. Insulin resistance is closely related to impaired glucose tolerance, diabetes, and risk of CAD.
2. High blood pressure and insulin resistance
- Many hypertensive individuals have glucose intolerance and hyperinsulinaemia. This association may not be causally linked since controlling hypertension neither improves glucose intolerance or hyperinsulinaemia, and hypertension is not observed in patients with insulinoma. On the other hand, obesity contributes to hypertension and hyperinsulinaemia, while weight reduction usually improves both of these disorders.
3. Dyslipidaemia
- High triglyceride and low HDL cholesterol levels are core components of the metabolic syndrome.
4. Large waist circumference and intra-abdominal fat accumulation
- Increased intra-abdominal fat accumulation, indicated by large waist circumference, may have a direct intermediary role in the development of the metabolic syndrome.[3]
Management[edit | edit source]
Management goal of the metabolic syndrome focuses on lifestyle changes such daily intake of five portions of fruit and vegetables and reduction in regular alcohol consumption to reverse modifiable risk factors for atherosclerotic disease and to prevent health complications including liver disease and cancer.[3]
Lifestyle changes should include the following:[edit | edit source]
- Daily Core Foods
- 5 or more fruit/vegetables
- 1-2 serves pulses, fish, meat.
- 2 cup sized helpings potatoes, rice or pasta
- 1 glass low fat milk
- max alcohol 14 units a week
2. Adhere to WHO physical fitness guidelines
3. Increase daily moderate exercise
4. Smoking cessation[3]
Prevention[edit | edit source]
It is likely that risk factors exist long before overt symptoms of the metabolic syndrome are expressed.
- Some individuals carry their risk from an early age because of childhood obesity while others endured an even longer periods due to their intra-uterine growth retardation.
- A greater emphasis should be given to risk prevention of pre-symptomatic individuals.
- At-risk individuals can be screened from their family history.
- MetSyn prevalence ranges from 5 to 7% in young adults. Low HDL is the most prevalent component of MetSyn in young adults and thus may also be the first detectable component of MetSyn in many young adults. Exploring the importance and significance of low HDL in young adults may have considerable public health benefits as interventions aimed at improving low HDL cholesterol levels could reduce the future incidence of MetSyn and subsequent clinical disease.[2]
- Regular physical activity and modest weight loss is likely to prevent most features of metabolic syndrome and, can even reverse all its components in those with the existing syndrome, thereby reducing its prevalence and incidence, as well as preventing new cases of diabetes.
- Smoking cessation is highly important not only to the individual, but also to their offspring to avoid intra-uterine growth retardation and adverse epigenetic modification leading to adult obesity.
- Anti-obesity drugs or other agents such as PPARγ agonists and GLP-1R agonists may also be considered as primary prevention of metabolic syndrome and CVD.
Physiotherapy[edit | edit source]
Incorporating physical activity as an integral part of treatment strategies for the metabolic syndrome would appear to go a long way toward reducing the adverse health impact of this condition. We as health professionals should promote physical activity in general and in particular at-risk individuals, or people with MetSyn when aver the opportunity arises.
- Recent meta-analyses suggest that exercise training, higher Cardiorespiratory Fitness, or both, improve factors that underlie the metabolic syndrome.
- Among subjects who meet the criteria for the metabolic syndrome, health outcomes are significantly improved by aerobic or resistance training, or their combination.
- An exercise program may improve risk markers to the extent that they no longer meet the criteria for the metabolic syndrome.
- There are numerous physiological, lifestyle, and genetic factors that account for these effects of physical activity or formal exercise programs. These include impact of exercise on insulin resistance, adipose fuel metabolism, inflammation, and epigenetic factors.
- Physical activity interventions clearly have a favorable impact on metabolic disease and the burden it places not only on individuals but also on health care systems.[8]
References[edit | edit source]
- ↑ Grundy SM, Cleeman JI, Daniels SR, Donato KA, Eckel RH, Franklin BA et al. Diagnosis and Management of the Metabolic Syndrome; An American Heart Association/National Heart, Lung, and Blood Institute Scientific Statement: Executive Summary. Circulation. 2005;112(17):e285–e290
- ↑ 2.0 2.1 Nolan PB, Carrick-Ranson G, Stinear JW, Reading SA, Dalleck LC. Prevalence of metabolic syndrome and metabolic syndrome components in young adults: A pooled analysis. Preventive medicine reports. 2017 Sep 1;7:211-5.
- ↑ 3.0 3.1 3.2 3.3 3.4 Han TS, Lean ME. A clinical perspective of obesity, metabolic syndrome and cardiovascular disease. JRSM cardiovascular disease. 2016;5:2048004016633371.
- ↑ The Global Epidemic of the Metabolic Syndrome Saklayen MG. The Global Epidemic of the Metabolic Syndrome. Curr Hypertens Rep. 2018; 20(2): 12. Doi: 10.1007/s11906-018-0812-z
- ↑ Wordnic; Epigenetics. Available from:https://www.wordnik.com/words/epigenetics ( accessed 15 August 2020)
- ↑ Health Link. What is Metabolic Syndrome? Available from: http://www.youtube.com/watch?v=fVMvY_Lsqzw [last accessed 24/8/2020]
- ↑ healthery. What is Metabolic Syndrome? (Syndrome X). Available from: http://www.youtube.com/watch?v=deH1uzXA1ik [last accessed 24/8/2020]
- ↑ Myers J, Kokkinos P, Nyelin E. Physical activity, cardiorespiratory fitness, and the metabolic syndrome. Nutrients. 2019 Jul;11(7):1652. Doi: 10.3390/nu11071652