Male Pelvic Pain
Top Contributors - Stacy Schiurring, Kim Jackson, Lucinda hampton and Jess Bell
Introduction[edit | edit source]
Disclamier: This page aims to provide an introductory discussion of men's health physiotherapy with regards to male pelvic pain. Please note that further training is required through a reputable pelvic health education company before attempting the techniques discussed in this page. See the Resources section at the bottom of this page for links to pelvic and men's health special interest groups.
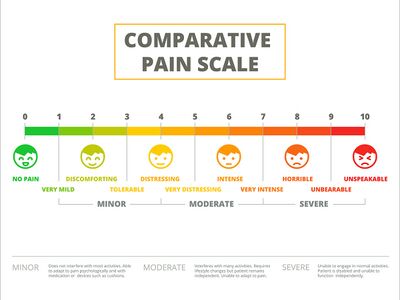
Pain is “an unpleasant sensory and emotional experience associated with, or resembling that associated with, actual or potential tissue damage.” - International Association for the Study of Pain[1]
The International Association for the Study of Pain (IASP) created the new definition for pain, stated above, in 2020. The description of pain continues with the following notes:
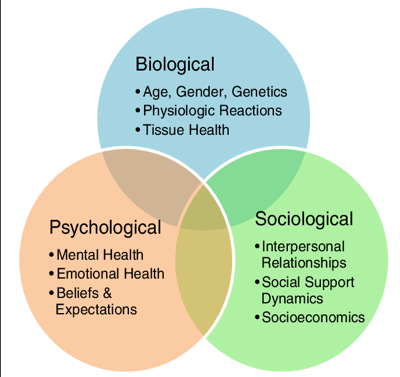
- Pain is always a personal experience to an individual, and it can be influenced by biological, psychological, and social factors
- Pain and nociception are different phenomena, meaning that pain cannot be solely explained by sensory neurons
- The concept of pain is a lifelong experience
- An individual's report of a pain experience should be respected
- Although pain usually serves an adaptive role, it may also have adverse effects on function and well-being
- Verbalisation is only one way to express pain; inability to communicate does not remove the possibility of a pain experience
Pain is subjective and unique to the individual experiencing it. Pain can be physically, mentally, and or psychologically debilitating. The IASP points out that pain is one of the main reasons that people seek out medical care, and chronic pain is a leading cause of human suffering and disability.[2]
Pain Classification Models[edit | edit source]
Classifying pain is a way for clinicians to better understand and design a plan of care to address a patient's pain. Over the years, classification systems have been developed to define, classify, or stratify different presentations or symptoms of pelvic pain. Traditionally, male pelvic pain classification has been based on chronic prostatitis, also known as chronic pelvic pain syndrome (CPPS).[3]
This following 5 minute video discusses the complexities of classifying and diagnosing male pelvic pain.
Chronic Prostatitis Related[edit | edit source]
The chronic prostatitis related classification system was created by the US National Institutes of Health (NIH), which divides chronic prostatitis into different categories: a combination of chronic bacterial prostatitis, CPPS, or asymptomatic prostatitis.[5]
| Category | Description | Bacterial Growth? |
|---|---|---|
| Category I:
Acute bacterial prostatitis |
Due to acute bacterial infection determining prostatitis symptoms, systemic infection, and acute bacterial urinary tract infection (UTI). | Yes |
| Category II: Chronic bacterial prostatitis | Due to chronic bacterial prostatic infection with or without prostatitis symptoms. | Yes |
| Category III: Chronic prostatitis/chronic pelvic pain syndrome |
|
No |
| Category IV: Asymptomatic inflammatory prostatitis | Due to prostate inflammation in the absence of genitourinary tract symptoms, always associated with CPPS. | Yes |
The following 20-minute video discusses the classification of prostatitis, aetiology of the different types of prostatitis, and the process of differential diagnosis between the different classifications and other diagnoses.
The Urinary, Psychosocial, Organ-Specific, Infection, Neurological/Systemic, and Tenderness (UPOINT) system[edit | edit source]
Accounting for more than 90% of all urological outpatients, CPPS is among the most common urologic disorders in men younger than 50 years. The condition is often poorly understood, and its management is challenging[7]. This tool was proposed in 2009 to separately identify the different possible reported symptoms of CPPS.[8]
| Reported Symptoms | Descriptors |
|---|---|
| Urinary symptoms[3][5] |
|
| Psychosocial dysfunction[3][5] |
|
| Organ-specific findings[3][5] |
|
| Infection[3][5] |
|
| Neurological/systemic [3][5] |
|
| Tenderness of muscles[3][5] |
|
| Sexual dysfunction[3] |
|
Anatomically Driven Classification[edit | edit source]
Male pelvic pain can also be grouped based on the symptoms into an anatomical classification.[3] It should be noted that these chronic overlapping pain conditions commonly occur in the same patients simultaneously.[9] Such classification categories can include:
- Prostate pain syndrome
- IBS
- Anal pain syndrome
- Neuromuscular pain
- Bladder pain syndrome
- Scrotal pain syndrome[3]
Biopsychosocial Framework[edit | edit source]
Please read this article for an in-depth review of the biopsychosocial model. Due to the complex nature of pain, a holistic whole-person approach to assessment, treatment, and interventions is required to fully understand the root cause of a person's pain. This is true of male patients with pelvic pain as well, especially given the often intimate and potentially embarrassing nature of pelvic pain diagnoses. Please read this article for an in-depth review of the complexities of treating men's health conditions. A 2021 article by Brandt,[10] published in The South African Journal of Physiotherapy, found that while physiotherapy training regarding the biomedical aspects of pelvic health are well known, the psychological, cognitive, behavioural, social and occupational factors are less integrated into treatments and care plans. Brandt[10] also found that individualised care, communication and therapeutic alliances with other medical professionals are under-investigated and not integrated into research, education and clinical practice.
Physiotherapists are uniquely positioned to utilise the biopsychosocial method as part of everyday practice,[3] especially with patients who have complex pain syndromes. Recommendations on how to integrate the biopsychosocial method into male pelvic floor physiotherapy include:[3]
- Expert knowledge of the male pelvic anatomy, especially innervation and referring pain patterns of the pudendal nerve
- Ability to differentiate between peripheral and central mechanisms of pain
- Ability to recognise diagnostic patterns such as:
- Bladder pain syndrome
- Scrotal pain syndrome
- Pudendal neuralgia / pelvic floor dysfunction
- Ability to perform a differential diagnosis for conditions that have similar clinical presentations:
- Prostate and bladder pain syndrome
- Scrotal pain syndrome
- Appropriate use of patient questionnaires to track patient outcomes over time[3]
Male Pelvic Pain Assessment Overview[edit | edit source]
- The most important part of a male pelvic pain assessment is to screen for dangerous underlying pathologies by looking for clinical red flags during the evaluation process.[3]
Assessment Red Flags
- Haematuria
- Haematospermia
- Smoking
- Occupational petrochemicals
- Pelvic radiation
- Ketamine abuse
- Tuberculosis or schistosomal endemic areas
- NEW onset of urinary incontinence or faceal incontinence
- Determine the diagnosis (taxonomic or phenotypic) using a classification model.[3]
- Determine the emotional, cognitive, behavioural, sexual and functional consequences using questionnaires and or through the subjective interview.[3]
Male Pelvic Pain Assessment: Subjective Interview[edit | edit source]
- Pain Qualifiers
- Where is it?
- What is it like?
- When does it happen?
- What makes it better / worse?
- Do you have any other pain?
- Functional Symptoms
- Bladder
- Incontinence? Urgency? Changes in sensations?
- Bowel
- Constipated? Previous surgeries? Dietary factors?
- Sexual
- Sexual dysfunction or symptoms?
- Neurological
- Changes in sensation or strength of the lower extremities? Changes in balance or coordination?
- Bladder
- Medical History
- Previous investigations
- Previous treatment
- Medical and surgical history
- Medications
- Psychological Features
- Anxiety about the pain
- Impact of the pain
- Use of questionnaires
- Referrals to mental health specialist, psychologist, psychiatrist, or counsellor
Male Pelvic Pain Assessment: Physical Examination[edit | edit source]
- Abdominal
- External genitalia
- Perineum
- Digital rectal examination -- Only qualified therapists with advanced training should perform internal pelvic health examinations. Please see links before in resource section for information on advanced training.
- Lower limb neurological examination: S3 and 4 nerve root dermatome and myotomes, lower extremity reflex examination, anal tone assessment
Examination Red Flags[11]
- Palpable bladder
- Penile or testicular mass
- Exquisite tenderness of the prostate or perineum
- Reduced anal tone
- Lower extremity neurological changes
- Lower extremity oedema
If a red flag is discovered, it is advisable to notify the referring doctor as soon as possible and provide basic education to your patient.
Management[edit | edit source]
Pelvic floor physiotherapy is one of the best studied non-pharmacological treatments of CPPS.[12][13]
- A single intervention will rarely work
- Management is usually multidisciplinary
- Management should be individualised, and phenotype focused
- The strategy may include elements of self-management
- Encourage return to active, healthy lifestyle as able with pain
Male Pelvic Pain Multidisciplinary Team[edit | edit source]
- General practitioner
- Urologist / gastroenterologist / colorectal surgeon
- Pain specialist
- Physiotherapist
- Psychologist / psychiatrist
- Acupuncturist / alternative medicine
- Dietitian
Resources[edit | edit source]
Professional Associations and formal continuing education courses:
- American Physical Therapy Association: Academy of Pelvic Health
- American Physical Therapy Association: On-Demand: Male Pelvic Pain Course
- Australian Physiotherapy Association: Men's Health
- Australian Physiotherapy Association: Male Pelvic Health
Questionnaires[edit | edit source]
- Pain Catastrophizing Scale
- Tampa Scale of Kinesiophobia
- Fear Avoidance Belief Questionnaire
- Rolland-Morris Disability Questionnaire
- Oswestry Disability Index
- Chronic Pain Grade Scale
- Pelvic Floor Distress Inventory (PFDI - 20)
References[edit | edit source]
- ↑ 1.0 1.1 Raja, S. N., Carr, D. B., Cohen, M., Finnerup, N. B., Flor, H., Gibson, S., ... & Vader, K. (2020). The revised International Association for the Study of Pain definition of pain: concepts, challenges, and compromises. Pain, 161(9), 1976-1982.
- ↑ Treede RD, Rief W, Barke A, Aziz Q, Bennett MI, Benoliel R, Cohen M, Evers S, Finnerup NB, First MB, Giamberardino MA. Chronic pain as a symptom or a disease: the IASP Classification of Chronic Pain for the International Classification of Diseases (ICD-11). pain. 2019 Jan 1;160(1):19-27.
- ↑ 3.00 3.01 3.02 3.03 3.04 3.05 3.06 3.07 3.08 3.09 3.10 3.11 3.12 3.13 3.14 3.15 3.16 3.17 3.18 Roscher, P, Male Pelvic Pain. Men's Health. Plus. March 2022.
- ↑ YouTube. Prostate Cancer UK|Chronic prostatitis and chronic pelvic pain syndrome: a new consensus guideline. Available from: https://www.youtube.com/watch?v=Oy8wb8uKIu8 [last accessed 08/032022]
- ↑ 5.0 5.1 5.2 5.3 5.4 5.5 5.6 5.7 Pirola GM, Verdacchi T, Rosadi S, Annino F, De Angelis M. Chronic prostatitis: current treatment options. Research and reports in urology. 2019;11:165.
- ↑ YouTube. Understanding Chronic Prostatitis. Available from: https://www.physio-pedia.com/index.php?title=Male_Pelvic_Pain&action=edit [last accessed 08/03/2022]
- ↑ Song PH. UPOINT System: A Diagnostic/Therapeutic Algorithm for Chronic Prostatitis/Chronic Pelvic Pain Syndrome. Urogenital Tract Infection. 2020 Aug 31;15(2):27-32. Available: https://www.researchgate.net/publication/344096939_UPOINT_System_A_DiagnosticTherapeutic_Algorithm_for_Chronic_ProstatitisChronic_Pelvic_Pain_Syndrome(accessed 24.5.2022)
- ↑ Shoskes DA, Nickel JC, Dolinga R, Prots D. Clinical phenotyping of patients with chronic prostatitis/chronic pelvic pain syndrome and correlation with symptom severity. Urology. 2009 Mar 1;73(3):538-42.
- ↑ Clemens JQ, Mullins C, Ackerman AL, Bavendam T, van Bokhoven A, Ellingson BM, Harte SE, Kutch JJ, Lai HH, Martucci KT, Moldwin R. Urologic chronic pelvic pain syndrome: insights from the MAPP Research Network. Nature Reviews Urology. 2019 Mar;16(3):187-200.
- ↑ 10.0 10.1 Brandt C. Physiotherapy and pelvic floor health within a contemporary biopsychosocial model of care: From research to education and clinical practice. The South African Journal of Physiotherapy. 2021;77(1).
- ↑ Parsons BA, Baranowski AP, Berghmans B, Borovicka J, Cottrell AM, Dinis‐Oliveira P, Elneil S, Hughes J, Messelink BE, de C Williams AC, Abreu‐Mendes P. Management of chronic primary pelvic pain syndromes. BJU international. 2022 May;129(5):572-81.
- ↑ Pena VN, Engel N, Gabrielson AT, Rabinowitz MJ, Herati AS. Diagnostic and management strategies for patients with chronic prostatitis and chronic pelvic pain syndrome. Drugs & aging. 2021 Oct;38(10):845-86.
- ↑ Mardon AK, Leake HB, Szeto K, Astill T, Hilton S, Moseley GL, Chalmers KJ. Treatment recommendations for the management of persistent pelvic pain: a systematic review of international clinical practice guidelines. BJOG: An International Journal of Obstetrics & Gynaecology. 2022 Jul;129(8):1248-60.
- ↑ Masterson TA, Masterson JM, Azzinaro J, Manderson L, Swain S, Ramasamy R. Comprehensive pelvic floor physical therapy program for men with idiopathic chronic pelvic pain syndrome: a prospective study. Translational andrology and urology. 2017 Oct;6(5):910.