Low Back Pain and Pregnancy
Original Editors - Timothy Assi
Top Contributors - Lynse Brichau, Aiko Deckers, Admin, Brenda Walk, Corin Arundale, Timothy Assi, Christine Utskot, Joanne Garvey, Kim Jackson, Lauren Lopez, Nicole Hills, Chris Slininger, Rachael Lowe, Temitope Olowoyeye, Joshua Samuel, Evan Thomas, Uchechukwu Chukwuemeka, Laura Ritchie, George Prudden, 127.0.0.1 and Jeremy Brady
Search Strategy[edit | edit source]
For our study we used a list of keywords and synonyms: Pregnancy, low back pain, low back pain AND pregnancy, pelvic girdle pain, pelvic girdle pain pregnancy, pelvic girdle pain AND treatment, pregnancy AND physical therapy, aquatic physiotherapy, physical therapy, physiotherapy,… Terms like AND, OR, and NOT allowed us to combine different aspects of the topic and find specific information. We applied this search process on different databases: Pubmed, PEDro, eMedicine, Medscape and Cochrane Database.
Definition/Description
[edit | edit source]
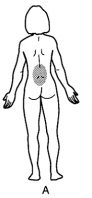
Pregnancy related low back pain is a common complaint that occurs in 60-70% of pregnancies [1] and can be defined as pain between the 12th rib and the gluteal folds/pubic symphysis during the course of pregnancy, possibly radiating to the posterolateral thigh, to the knee and calf, but not to the foot. [2] This pain is not the result of a known pathology such as disc herniation[3] and can begin at any point during pregnancy. Although most cases are mild, approximately one third of women experience severe pain.[4] Pregnancy related low back has been coined multiple times and can be referred to as one of the following patters:Low Back Pain (LBP), Peripartum Posterior Pelvic Pain (PPPP), Pregnancy-related low back pain (PLBP) or pregnancy-related pelvic girdle pain (PPGP). The last two patterns can occur separately or combined.[1]
Unfortunately, there is limited research available regarding physical therapy intervention for pregnant women experiencing Low Back Pain, so a homogenous approach tends to be used. However, back pain is not homogenous; therefore special considerations and precautions should be taken when treating this population.
Clinically Relevant Anatomy[edit | edit source]
The lumbar region is constituted of five unique vertebrae that are designed to withstand increased weight and retain a lordotic curve. The vertebral canal of the lumbar region houses the tail end of the spinal cord and the Cauda Equina.
To maintain stability and provide support, the lumbar region is connected and held secure by an intricate web of ligaments: ligamentum longitudinale anterior and superior, ligamentum flava, ligamentum interspinata, ligamentum intertransversarium and the ligamentum supraspinale. All the mentioned ligaments will provide stability, whereas the longitudinal ligament will also be attached to the intervertebral disc in order to keep the discs in position. Additionally, the lumbar region is supported by strong low back muscles, pelvic muscles and abdominal muscles.
Epidemiology /Etiology
[edit | edit source]
A number of reviews investigated the prevalence of low-back pain during pregnancy in different populations. The results are inconsistent, ranging from 8% to more than 89% of women who complain of low back pain during pregnancy.[6][7][8][1][9][10][11][12][13][14]
The prevalence of pregnancy related low-back pain is the highest during the third trimester.[15][11] The discomfort starts mostly between the fifth and seventh month of pregnancy. The influence of the postural change and body weight rises at this moment. [16][13][14]
The cause of pregnancy related LBP can be due to a combination of mechanical, hormonal, circulatory and psychosocial factors. [16][12][13][14]
Mechanical:
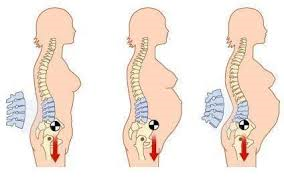
During pregnancy, the enlarging gravid uterus changes the load and body mechanics. It’s shifts the centre of gravity forwards, increasing the stress on the lower back. Postural changes can be used to balance the anterior shift possibly causing an extra lordosis. This increases the natural inward curvature of the spine, which increases the mechanical strain on the lower back. It also puts an extra stress on the intervertebral disc, possibly causing a decreased height an overall compression of the spine. [12][13][14]
The abdominal muscles also stretch to accommodate the expanding uterus. As they stretch, the muscles become tired and lose their ability to maintain normal body posture, causing the lower back to support the majority of the increased weight of the torso. [13][14]
Hormonal:
A significant portion of women first experience pain during the first trimester of pregnancy. At that moment mechanical changes do not yet play a significant role in the onset of pain. This suggests that hormonal changes during pregnancy can cause inflammation and pain in the back. It has been suggested that the hormone relaxin increases 10-fold in concentration during pregnancy, softening the collagen and causes ligamentous laxity and discomfort. The sacroiliac ligaments, but also other ligaments who surround the pelvic girdle become loose. This causes a decrease in the stability and brings on a potential strain in the pelvic girdle and low back area. [16][12][13][14]
Circulatory:
The expanding uterus can press on the vena cava, particularly at night when the patient is lying down. The pain is possibly severe enough to wake the patient up. This combined with the increased fluid volume from fluid retention during pregnancy leads to venous congestion and hypoxia in the pelvic and lumbar spine. [13][14]
Psychosocial factors:
Psychosocial factors can also increase low back pain. Pain-related catastrophizing, depression, pain intensity and time result in an increases in pain interference. The findings support the potential utility of the biopsychosocial model. Pain catastrophizing can be considered as a risk factor in the third trimester of pregnancy. [12]
Risk factors:
| Risk factors [17][15][18][1][9][19][12][13][14] | No risk factors [10][8][1][13] |
|---|---|
| LBP history | Age |
| Multiple abortions | Fetal weight |
| Smoking | Oral contraceptives |
| Pain during previous pregnancy | |
| Number of pregnancies | Number of pregnancies |
| History of hypermobility | |
| Periods of amenorrhea | |
| Increased physical workload | |
| High body mass index | High body mass index |
| Lack of exercise/sedentary lifestyle | |
| Pain catastrophizing |
There is a relative agreement that excessive body weight may be a risk factor for LBP during pregnancy however, there are studies claiming that being overweight is not a risk. The same goes for number of pregnancies before the current one. [1][12][13][14]
Characteristics/Clinical Presentation[edit | edit source]
There are several possible mechanisms of injury which could be causing pregnancy related LBP. During pregnancy, changes occur in the facet joints, in the back muscles, and in ligaments. This is mainly caused by the increased release of the hormone Relaxin,[4] which causes ligament laxity, and therefore can affect the stability of the spine and lead to back pain.[20]
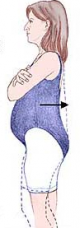
Another contributor is the increase in weight. On average, about 11-15 kilograms are gained during pregnancy.[20] The weight gain increases the amount of force placed across joints, changes the center of gravity, and forces the patient into an anterior pelvic tilt. The anterior displacement of the center of gravity will cause women to shift their heads and upper body posteriorly over the pelvis, causing hyperlordosis of the lumbar spine. This in turn, places additional stress on the intervertebral discs, ligaments, and facet joints and can lead to joint inflammation.[21][22] In addition, abdominal muscles are stretched and weakened, and the added weight can compress on the lumbosacral plexus.[23]
The most common onset tends to be during the 5th and 6th month of pregnancy, and the pain is usually worse in the evening. About 67% of women experience pain at night. Factors that aggravate the pain include: standing, sitting, coughing or sneezing, walking, and straining during a bowel movement.[22] However pain and a disability of the lumbopelvic region are usually proven to be experienced as mild to moderate, except for a minor part (20%) of the pregnant women that will describe the pain as severe.[24]
The localization of pain is deep. It’s even possible that localization of the pain changes over time.
Pelvic girdle pain has been described as “stabbing’’ , pain in the lower back as a “dull ache’’ and the pain in the thoracic spine is rather “burning’’. Other pain-descriptions are: shooting pain, feeling of oppression and a sharp twinge.
Often, the onset of pain occurs around the 18th week and reaches peak intensity between the 24th and 36th week of pregnancy. The pain can spontaneously disappear within 3 months, but 7-8% of the patients have a persisting, chronic pain. However it may start as early as the first trimester or be delayed as late as 3 weeks after delivery. [25] [26] [27] [28]
Pregnancy-related low back pain is characterized by a dull pain [29] [30] and is more pronounced in forward flexion with associated restriction in spine movement and palpation of the erector spinae muscles exacerbates pain. [31]
Several factors have been associated with the development of low back pain during pregnancy. More specifically, laborious work, a history of low back pain before pregnancy, and a previous history of pregnancy-related low back pain have been identified as risk factors for the development of pregnancy-related low back pain. Pain syndromes during pregnancy impact the abdominopelvic musculoskeletal system, thereby causing abnormal strain on the axial low back elements. [32]
Differential Diagnosis[edit | edit source]
Some other diagnoses that can be commonly mistaken for pregnancy related low back pain are: Sciatica, Meralgia Paresthetica, thoracic/rib pain, hip pain, coccygodynia, spontaneous abortions, osteomyelitis, osteoarthritis of spine or hip, Cauda Equina Syndrome, Osteitis Condensans Ilii, metastatic cancers, and Diastasis Rectus Abdominis. Other more common differential diagnoses are: disc disease, facet joint involvement and sacroiliac joint involvement. It is important to be able to recognize the subtle differences and differentiate between the comorbidities.[33][30]
“Disc Disease - Morning pain and stiffness, pain when weight bearing, pain with increased abdominal pressure, history of repeated micro trauma, pain when going uphill, pain with prolonged sitting, pain with sit to stand activity. Sleep is usually undisturbed, pain eases as day progresses and then gets worse again, movement eases pain but not for long (e.g. fidgets).”[33]
“Facet Joint Involvement - Non weight bearing pain, pain with related to movement (specifically rotation), pain increased by lateral compression, history of minor injury, pain is not usually referred to an extremity, pain eases with rest, not affected by coughing or sneezing”[33]
“Sacroiliac Involvement - Pain is usually unilateral and does not midline, can refer to lower extremities, turning while in supine provokes pain, getting out of the car provokes pain, pain is referred to the groin or genitals, pain is related to menstruation prior to pregnancy because of the effects of cyclic hormones on pre-pregnant SIJ ligaments.”[33]
It is also important to differentiate between pregnancy-related low back pain (PLBP) and pregnancy-related pelvic girdle pain (PPGP), as the management and prognosis of the two conditions may differ. [2] Useful methods of differentiation include the site of pain, its character and severity, provoking factors, resultant disability, and the pain provocation tests. Recommended provocation tests are the posterior pelvic pain provocation test, Patrick’s Faber test, and the long dorsal sacroiliac ligament test. [34] In PPGP, the pain is typically concentrated under the posterior superior iliac spine, in the gluteal area, the posterior thigh, and the groin, meanwhile patients with PLBP show the pain to be concentrated in the lumbar region above the sacrum. [34]
Diagnostic Procedures[edit | edit source]
In order to formulate the correct diagnosis, the patient should be questioned about her past medical history. It is important to concentrate on experienced symptoms, limitations in activities, and movement possibilities. Questions about past pregnancies such as – "Have you experienced any complications with prior pregnancy(s)?" are appropriate. This will help the therapist understand the patient’s health problems and needs. Knowledge of the anatomical and functional disorders, activity limitations and restriction of participation will help the therapist determine her/his role and the need for appropriate interventions. It is important to recognize red flag complaints and contact a doctor to seek further investigation, if they are present.[15]
It is important at the time of initial assessment to differentiate between the lumbar spine and pelvic dysfunction. This can be done during the subjective by enquiring about aggravating factors. Activities such as turning in bed, getting out of a car, walking and climbing stairs may indicate that the origin of pain may be due to pelvic dysfunction. This can then be confirmed with a range of tests for assessing the sacroiliac joint and pubic symphasisis.
Outcome Measures[edit | edit source]
Several validated instruments to assess back pain exist for general population who can be used in the diagnosis to estimate the complaints more objectively:
-Visual Analogue Scale (VAS)[6],
-Roland Disability Questionnaire (RDQ) [35],
-Québec Pain disability index (QPDI) [36]
-PHotograph series Of Daily Activities (PHODA),
-Impact on Participation and Autonomy (IPA),
-Pain Behavior Scale (PBS).
But we can also use more detailed measured instruments. However, for a pregnant population such an instrument does not really exist.
For that reason, a pregnancy-specific self-report questionnaire assessing mobility in relation to both back and pelvic pain, called the Pregnancy Mobility Index (PMI), was developed and validated. [37]
-Oswestry Disability Index. [16]
Examination
[edit | edit source]
During an examination of a pregnant patient, positioning is a key consideration. Excessive time in supine is not recommended due to the weight of the uterus on the vena cava and vital structures.[33] Based on the level of pain and disability of the patient, and potentially the size of the pregnant abdomen, certain tests and measures may need to be modified for this population.Excessive time in supine is not recommended due to the weight of the uterus on the vena cava and vital structures.[33]
Questionnaires
The visual analogue scale (VAS) is often used to measure the pain. [13]
The Oswestry Disability Index (ODI) can be used to measure the level of disability in activities of daily living in those rehabilitating from low back pain. The ODI is a self-administered questionnaire consisting of 10 items, graded from 0 to 5. Low score indicate low disability. [16]
Van De Pol et al. developed the Pregnancy Mobility Index (PMI) to assess the ability of doing normal household activities. The patient can answer on a scale from ‘no problem’ to ‘impossible’ or ‘only with aid of others’. The PMI is used to evaluate the mobility and quality of life of pregnant women who suffer from LBP. [13][37]
Examination should include observation of the posture and gait, neurologic screen to rule out underlying pathology, range of motion, muscle tests, palpation, muscle length tests, and assessment of joint mobility.
It’s important to distinguish posterior pelvic pain from low back pain during physical examination. Recommended provocation tests are the Posterior Pelvic Pain Provocation (PPPP) test, FABER test, long dorsal sacroiliac ligament test and standing on one leg. As mentioned above, the pain is typically concentrated under the posterior superior iliac spine, in the gluteal area, the posterior thigh and the groin in case of PPGP. Patients with PLBP show pain concentrated in the lumbar region above the sacrum. [38][39][13][34] Palpation over soft tissue of the sacroiliac, pubic symphysis, and gluteal regions can also distinguish pelvic pain from tenderness over the back above the waist. Studies show that both methods are effective although pain provocation tests are more reliable than palpation tests. [13]
The following findings are commonly revealed: Paravertebral muscles are tender to palpation, back muscles weakness, decreased ROM in flexion. The description of the pain is often not localized and may be intermittent. It is possible for the pain to radiate down as far as the calf.[17]
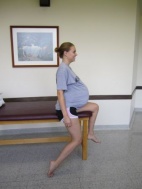
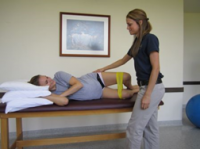
Hip Flexor Length: To modify the test position of the ‘Thomas Test’ the patient will have to sit on the edge of a table or mat, and extend the test leg as much as possible, while maintaining slight knee flexion. The pelvis should be kept in a neutral alignment. A patient with non-impaired flexibility should be able to extend her hip perpendicular to the floor.
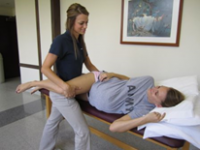
SI Joint Examination: If the patient is unable to stand, instruct the patient to lie in supine and perform a pelvic bridge. The bridge will place the pelvis in neutral - the ASIS’ can be palpated for symmetry.
Figure B: Walk B. Texas State University's Evidence-based Practice project.
Medical Management[edit | edit source]
It is important to encourage the patient to receive regular checkups by her obstetrician. During the therapy session, continually check on pain levels and any aches radiating from the low back or stomach. Some patients tolerate pain and discomfort better than others and will therefore mask their distress – Use a chart for Rate of Perceived Exertion to determine the patient's true status and take note of any changes that occur between the begging and end of the session.
Although there are numerous interventions promoted for low back pain during pregnancy, the most common and widely used is a specific exercise program designed by a physical/physiotherapist (see below)[43](Level of evidence:2A) [44](Level of evidence:1B). Another intervention that is getting tractions and shows prominent research is acupuncture. Recent studies show that a week of continuous acupuncture at specific auricular points can decrease pain and increase the capacity for some physical activity which can help diminish the need for drugs.[45](Level of evidence:3B)
Other Interventions:
- side lying while sleeping or resting using a wedge shaped pillow to support stomach
- use of pillow between the legs while side lying (squeeze the pillow/legs together while rolling)
- compression socks to promote venous return and decrease edema
- support belt (The Love Comfort support belt is covered by Medicaid) [33](Level of evidence:3A)
- soft tissue massage
- acetaminophen as proscribed by physician
- yoga [46](Level of evidence:2C)
- aerobic therapy
- aquatherapy[47](Level of evidence:1B)
Intra-articular sacroiliac joint injections (under imaging guidance) for ankylosing spondylitis can be recommended. There are indications that acupuncture during pregnancy may reduce pain, but high quality studies are required for sacroiliac joint therapeutic injection therapy. [34](Level of evidence:3A) [32](Level of evidence:2A)
Most therapeutic strategies encourage preventive measures among pregnant women and those who are planning to become pregnant. It has been shown that women who participate in prophylactic education and strengthening programs during early pregnancy can avoid problems from low back pain. [13](Level of evidence:4)
When treatment is necessary for low back pain, conservative management is the ideal option. Treatment starts with education and activity adjustments. Educational strategies focus on back care measures, such as ergonomics, which teaches women correct posture; pregnant women learn how to stand, walk, or bend properly, without causing stress on the spine. Accurate posture is essential to improve low back pain. Braces that ensure correct body posture are also available if the instructions are not enough. In regard to activity modifications, scheduled rest during the day is helpful for relieving muscle spasms and acute pain. During this time, posture is again important as both feet should be elevated, which will help flex the hips and decrease the lumbar lordosis of the spine. [32](Level of evidence:2A) [48](Level of evidence:4)
Studies have found that pregnant women with low back pain, who participate in both education and physical therapy, have less pain and disability, higher quality of life, and improvement on physical tests. Physical therapy encompasses several factors such as postural modifications, back strengthening, stretching, and self-mobilization techniques. Functional stability can be maintained throughout pregnancy by strengthening the muscles around the lumbar spine through various back exercises. [32](Level of evidence:2A) [48](Level of evidence:4)
Physical Therapy Management
[edit | edit source]
“Red flags”[5](Level of evidence:2A)
Vaginal bleeding, dizziness/feeling faint, shortness of breath, chest pain, headache, muscles weakness, calf pain or swelling, uterine contractions, decreased fetal movement, vaginal fluid leakage, neurological involvement.
Physical therapy goals:[43](Level of evidence:1A)
• Restore biomechanics during daily activities
• Lumbo- Pelvic stabilization
• Advise and prevention
Physical therapy should be focused on the following Strategies:[49](Level of evidence:1B)
1) Patient instructions[edit | edit source]
It’s important to communicate with the patient and provide information about the relevant anatomy, ergonomics, back education (to prevent unnecessary mechanical stress on the back), and how to manage ADL activities (walking, standing, sitting, lying, and work position, learning how to control pain). Research shows that when the symptoms are explained, patients can feel more at ease and their anxiety may decrease. [50](Level of evidence:3A)
- Using a small pillow between the legs while sitting and rolling in order to stabilize the back.[39](Level of evidence:2A)
- Postural correction by standing upright with a neutral posture, avoiding hyperlordosis
- Do not sit or stand for a long time, alternate it with walking or stretching
- Taking breaks and resting in a comfortable position, with the back supported to relieve tired muscles[39](Level of evidence:2A)
- Sleeping lying on one side with the top leg on a pillow
- “Use of a small footstool for one foot in sitting or standing, alternate feet”[49](Level of evidence:1B)
- Avoiding spine twisting while lifting
2) Physical therapy[edit | edit source]
Stability, coordination and functional preservation should be trained with active back exercises – endurance training for back muscles stabilization.[17(Level of evidence:1B)] Pelvic tilts, knee pull, straight leg raising, curl up, lateral straight leg raising and water aerobics are recommended because these exercises could relieves lumbar pain in pregnancy.[20(Level of evidence:2C)] Relaxation exercises while paying close attention to proper respiration also show to be beneficial.[30(Level of evidence:3A)]
Management includes specific interventions to address pain, weakness, and mobility in the low back region. The Ottawa Panel also recommends massage therapy in order to treat subacute and chronic low back pain. [51](Level of evidence:1B)
Manual therapy techniques
| Posterior/Anterior mobilizations in side lying position | Addresses pain and mobility (Grades 1-4). |
Figure C: Walk B. Texas State University's Evidence-based Practice |
| Muscle Energy Technique by resisting hip flexion in side laying while stabilizing the sacrum | Corrects anterior innominate rotation. |
Figure D: Walk B. Texas State University's Evidence-based Practice |
| Spinal manipulation [39](Level of evidence:2A) | Are used to relax soft tissues |
Active Exercises
| Strengthening Gluteus Medius |
Position the patient in a side lying and place an elastic around both legs above the knees. Ask the patient to perform an external rotation of her leg in order to strengthen the Gluteus Medius. Perform this exercise on both sides. Feet need to be kept together during the whole exercise. Also, prevent the pelvis from externally rotating. |
Figure E: Walk B. Texas State University's Evidence-based Practice |
| Abdominal Drawing in Maneuver with Physioball (ADIM). |
Ask the patient to sit on a physioball and simulate a walk movement with the lower extremities. This will encourage the back muscle memory to stabilize back during ADL's.
|
Figure F: Walk B. Texas State University's Evidence-based Practice |
| Latissimus dorsi pull-downs |
The patient will be positioned on a physioball, which will force the pelvic, abdomen and back muscles to stay active in order to find a balanced sitting position. This part of the exercise will provoke a contraction of the glutei to increase the strength of the posterior oblique sling muscles which compress the SIJ. Keep the back straight during the whole exercise. |
Figure G: Walk B. Texas State University's Evidence-based Practice |
| Angry Cat [20](Level of evidence:5) | Starting from the hands-and knees-position the patient will move her back up and down. During this exercise it is important to keep the arms stretched out with the hands positioned right under the shoulders and to keep the stomach muscles tight throughout the entire exercise. |
Figure H: [20](Level of evidence:5) |
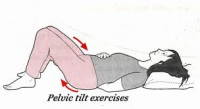
| Pelvic Tilt [20](Level of evidence:5) | Lay down with flexed knees and move the pelvic in an anterior and posterior position. |
Figure I: Women health clinic. Post Natal Exercises. Available at: http://www.pregnancyandchildcare. info/pregnancy_articles/ postnatalexer.html |
Even though most pregnant patients will be advised to exercises within their safe and pain free range, studies show that less than 50% will actually do so. [52](Level of evidence:1A) Furthermore it has also been proven that training the rectus abdominus muscles will be useless due to his weakness during the pregnancy.
TENS
There is no strong evidence on the benefits of Tens on Low back pain in pregnancy but it can be used as a supplementary therapy. It’s important to use a low intensity and avoid the acupuncture points which may induce throes. Precautions and contra-indications must be respected.[30](Level of evidence:3A)[53](Level of evidence:1A)
Patients should take caution when using ultrasound and electrical stimulation and avoid placing those modalities anywhere near the stomach or low back.
Yoga (Level of evidence: 1B)
Yoga can effectively decrease low back pain intensity. [54](Level of evidence:1B)
Stretching (Level of evidence:1B)
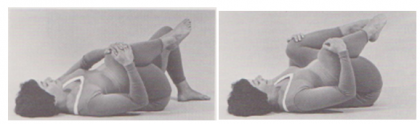
1. Lower Back Stretch: it is plausible that stretching lower back and hip extensor muscles can lead to increased lower back and pelvic flexibility.[20](Level of evidence:5)
Figure J + K: [20](Level of evidence:5) Stahmann Dilfer C.; Your Baby, Your Body (Fitness during pregnancy); Crown publishers, inc., New York, 1977'
Instructions:[20](Level of evidence:5)
a) Clasp your fingers around your right knee.
b) Gently pull your knee as close to your chest as possible. Relax your lower back and try to let your gluts (butt) roll of the floor as you pull.
c) Hold for a slow count of 3.
d) Release.
e) Repeat steps b-d 12-15 times.
f) Now, grasp your left knee, put the right foot flat on the floor and repeat steps b-e
g) Finally, grasp both knees with your hands, and pull both knees close to your chest (or outside your stomach).
h) Repeat steps b-e.
2. Combined squat stretch, back and hamstrings stretch: strengthens thighs (upper legs) and gluts, stretches hamstrings, inner thighs, pelvic floor muscles and back.[20](Level of evidence:5)
Figure L + M: [20](Level of evidence:5) Stahmann Dilfer C.; Your Baby, Your Body (Fitness during pregnancy); Crown publishers, inc., New York, 1977
Instructions:[20](Level of evidence:5)
a) Squat down on your feet, feet pointing at a 45° angle to the sides, heels on the floor.
b) Open your knees wide using thigh muscles and push them apart until they are directly over your feet.
c) Keep your knees back over your feet, and slowly raise your gluts – keep on extending your knees – until your legs are as straight as possible (do not lock out your knees).
d) Relax your head, neck and shoulders.
e) Hold position for 10 counts.
f) Try to keep your knees over your feet and slowly lower your gluts until you return to starting position.
3) Aerobic exercises (Level of evidence: 1B)[edit | edit source]
Walking, swimming1B,Tai chi, recumbent bicycle (or nu-step), are plausible to be beneficial at a low to moderate intensity. The stress on the back should be minimal.[55](Level of evidence:2A)
4) Home exercises [edit | edit source]
The exercises explained above could also be performed at home if both the patient and therapist feel confident that the exercises will be performed correctly without supervision.
Back tuck arch [20](Level of evidence:5): Lean with the back against the wall and alternate between anterior and posterior pelvic tilt.
Figure N: Hughston clinic. Excercising during pregnancy. Available at : http://www.hughston.com/a-11-3-4.aspx
Prognosis [30]Level of evidence:3A)
Patients recover from LBP in pregnancy within a few weeks or a few months after childbirth, but symptoms may return during a future pregnancy. Between 8% and 10% of women will continue to experience pain for up to 2 years post-delivery.[30](Level of evidence:3A)
Key Research[edit | edit source]
Low back pain pregnancy/pregnant, LBP pregnancy, pregnancy back pain, maternal low back pain, gestation low back pain, pregnancy exercise(s), low back pain causes, low back pain physical therapy.
Resources
[edit | edit source]
Clinical Bottom Line[edit | edit source]
The majority of pregnant women experience low back pain. Appropriate examination, interventions and follow up, can help in managing the pain. There are many physiotherapy treatments for pregnant woman with low back pain. Our research suggested a combination of instructions, manual therapy, active exercises, aerobic exercises and stretching. Key questions must be asked and special modifications must be made for more complex patient experiencing pregnancy related back pain. As patient centered practitioners, it is our job to research and implement evidence based practice to increase outcomes with minimal number of treatments.
We concluded there is a dearth in good quality research. Future studies should more concentrate on the specific low back pain of pregnant woman.
Recent Related Research (from Pubmed)
[edit | edit source]
1. Glinkowski, Wojciech M., et al. Posture and low back pain during pregnancy—3D study. Ginekologia Polska 87.8 (2016): 575-580. (Level of evidence: 2B)
2. Chang, Hao‐Yuan, et al. Factors associated with low back pain changes during the third trimester of pregnancy. Journal of advanced nursing 70.5 (2014): 1054-1064. (Level of evidence: 2B)
3. Hensel, Kendi L., Michael S. Carnes, and Scott T. Stoll. Pregnancy Research on Osteopathic Manipulation Optimizing Treatment Effects: The PROMOTE Study Protocol. The Journal of the American Osteopathic Association 116.11 (2016): 716. (Level of evidence: 1B)
4. Kaplan, Şeyhmus, et al. Short-Term Effects of Kinesio Taping in Women with Pregnancy-Related Low Back Pain: A Randomized Controlled Clinical Trial. Medical science monitor: international medical journal of experimental and clinical research 22 (2016): 1297. (Level of evidence: 1B)
5. Liddle, Sarah D., and Victoria Pennick. Interventions for preventing and treating low‐back and pelvic pain during pregnancy. The Cochrane Library(2015). (Level of evidence: 1A)
Presentations[edit | edit source]
 |
Pelvic Physiotherapy - to Kegel or Not?
This presentation was created by Carolyn Vandyken, a physiotherapist who specializes in the treatment of male and female pelvic dysfunction. She also provides education and mentorship to physiotherapists who are similarly interested in treating these dysfunctions. In the presentation, Carolyn reviews pelvic anatomy, the history of Kegel exercises and what the evidence tells us about when Kegels are and aren't appropriate for our patients. |
References
[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 Mogren IM, Pohjanen AI. Low back pain and pelvic pain during pregnancy: prevalence and risk factors. Spine . 2005 Apr 15;30(8);983-91. (Evidence level: 2C)
- ↑ 2.0 2.1 Östgaard, H. C., et al. Reduction of back and posterior pelvic pain in pregnancy. Spine 19.8 (1994): 894-900. (Evidence level: 1B)
- ↑ Jeffcoat H. Exercises for low back pain in pregnancy. Int J Childbirth Educ. 2008; 23: 9-12. (Evidence level: 5)
- ↑ 4.0 4.1 Hall J, Cleland J, Palmer J. The Effects of Manual Physical Therapy and Therapeutic Exercise on Peripartum Posterior Pelvic Pain: Two Case Reports. Journal of Manual and Manipulative Therapy. 2005;13(2): 94-102 (Evidence level: 3B)
- ↑ 5.0 5.1 Perkins J, Hammer RL, Loubert PV. Identification and management of pregnancy-related low back pain. J Nurse Midwifery. 1998;43:331–340. [PubMed] (Evidence level: 2A)
- ↑ 6.0 6.1 M. Ronald, J.R. Jenner. Back pain New approaches to rehabilitation and education. Manchester university press. 1989;258 pages (Evidence level: 2B)
- ↑ Endresen EH. Pelvic pain and low back pain in pregnant women – an epidemiological study. Scan J Rheumatol. 1995; 24: 135–41. (Evidence level: 3A)
- ↑ 8.0 8.1 Bastiaanssen JM, de Bie RA, Bastiaenen CH, Essed GG, van den Brandt PA. A historical perspective on pregnancy-related low back and/or pelvic girdle pain. Eur J Obstet Gynecol Reprod Biol. Maastricht. 2005 (Evidence level: 2C)
- ↑ 9.0 9.1 Ostgaard HC, Andersson GBJ, Karlsson K. Prevalence of back pain in pregnancy. Spine 1991; 16: 549–52. (Evidence level: 2C)
- ↑ 10.0 10.1 Orvieto R, Achiron A, Ben-Rafael Z, Gelernter I, Achiron R. Low back pain of pregnancy. Acta Obstet Gynaecol Scand. 1994; 73: 209–14. (Evidence level: 4)
- ↑ 11.0 11.1 Ansari NN, Hasson S, Naghdi S, Keyhani S, Jalaie S. Low back pain during pregnancy in Iranian women: Prevalence and risk factors. Physiotherapy Theory and Practice, 26(1):40–48, 2010 (Evidence level: 2C)
- ↑ 12.0 12.1 12.2 12.3 12.4 12.5 12.6 Chang, Hao‐Yuan, et al. Factors associated with low back pain changes during the third trimester of pregnancy. Journal of advanced nursing 70.5 (2014): 1054-1064. (Evidence level: 2B)
- ↑ 13.00 13.01 13.02 13.03 13.04 13.05 13.06 13.07 13.08 13.09 13.10 13.11 13.12 13.13 13.14 Sabino, Jennifer, and Jonathan N. Grauer. Pregnancy and low back pain. Current reviews in musculoskeletal medicine 1.2 (2008): 137-141. (Evidence level: 4)
- ↑ 14.0 14.1 14.2 14.3 14.4 14.5 14.6 14.7 14.8 Katonis, P., et al. Pregnancy-related low back pain. Hippokratia 15.3 (2011): 205-210. (Evidence level: 4)
- ↑ 15.0 15.1 15.2 GE Bekkering PT MSc, HJM Hendriks PT PhD, BW Koes PhD, RAB Oostendorp PT MT PhD, RWJG Ostelo PT MSc, JMC Thomassen PT, MW van Tulder PhD.; National practice guidelines for physical therapy in patients with low back pain (Evidence level: 2C)
- ↑ 16.0 16.1 16.2 16.3 16.4 Glinkowski, Wojciech M., et al. Posture and low back pain during pregnancy—3D study. Ginekologia Polska 87.8 (2016): 575-580. (Evidence level: 2B)
- ↑ 17.0 17.1 Sneag D, Bendo J. Pregnancy-related low back pain. Orthopedics. 2007; 30: 839-845. (Evidence level: 1A)
- ↑ Horst Eggen M., Stuge B., Mowinckel P. , Smee Jensen K., Hagen K.B. . Can Supervised Group Exercises Including Ergonomic Advice Reduce the Prevalence and Severity of Low Back Pain and Pelvic Girdle Pain in Pregnancy? A Randomized Controlled Trial. PHYS THER. 2012; 92:781-790. (Evidence level: 1B)
- ↑ (26) Ostgaard HC, Andersson GBJ. Previous back pain and risk of developing back pain in a future pregnancy. Spine 1991; 16: 433–6. (Evidence level: 2C)
- ↑ 20.00 20.01 20.02 20.03 20.04 20.05 20.06 20.07 20.08 20.09 20.10 20.11 Stahmann Dilfer C.; Your Baby, Your Body (Fitness during pregnancy); Crown publishers, inc., New York, 1977 (Evidence level: 5)
- ↑ (14) Russell R.,Reynolds F. Back pain, pregnancy, and childbirth. British medical journal. 1997;1059-1064. (Evidence level: 5)
- ↑ 22.0 22.1 To W. W. K., Wong M. W. N. . Factors associated with back pain symptoms in pregnancy and the persistence of pain 2 years after pregnancy. Acta Obstetricia et Gynecologica Scandinavica. 2003; 1086-91.(Evidence level: 2B)
- ↑ Gilleard W. L., Brow J.M. Structure and function of the abdominal muscles in primigravid subjects during pregnancy and the immediate postbirth period. Physical Therapy, 1996; 750-62 (Evidence level: 2B)
- ↑ Mens JM, Huis YH, et al. Severity of signs and symptoms in lumbopelvic pain during pregnancy. Manual Therapy 17 (2012) 175e179 (Evidence level: 2C)
- ↑ E.H. Verstraete, G. Vanderstraeten, W. Parewijck. Pelvic Girdle Pain during or after Pregnancy: a review of recent evidence and a clinical care path proposal: a systematic review. Pubmed 2013; 5(1); 33-43 (Evidence level: 3A)
- ↑ Wu WH, Meijer OG, Uegaki K, Mens JMA, Van Dieën JH, Wuisman PIJM, Östgaard HC. Pregnancy-related pelvic girdle pain (PPP), I : Terminology, clinical presentation, and prevalence. European Spine Journal Nov 2004; 13(7) : 575-589. (Evidence level: 3A)
- ↑ Gutke A, Ostgaard HC, Oberg B. Pelvic girdle pain and lumbar pain in pregnancy: a cohort study of the consequences in terms of health and functioning. Spine (Phila Pa 1976) 2006;31:E149–E155. doi: 10.1097/01.brs.0000201259.63363.e1. (Evidence level: 2B)
- ↑ Bergström C, Persson M, Mogren I. Pregnancy-related low back pain and pelvic girdle pain approximately 14 months after pregnancy-pain status, self-rated health and family situtation. BMC Pregnancy Childbirth 2014. A0.AA86/1471-2393-14-48. (Evidence level: 2B)
- ↑ Sturesson B, Uden G, Uden A. Pain pattern in pregnancy and “catching” of the leg in pregnant women with posterior pelvic pain. Spine (Phila Pa 1976) 1997;22:1880–1883. doi: 10.1097/00007632-199708150-00013. discussion 1884. (Evidence level: 4)
- ↑ 30.0 30.1 30.2 30.3 30.4 Vermani E., FRCA*; Mittal R, FRCS†; Weeks A., MRCO Pelvic Girdle Pain and Low Back Pain in Pregnancy: A Review, Pain Practice, Volume 10, Issue 1, 2010 60–71 (Evidence level: 3A)
- ↑ Ostgaard HC, Roos-Hansson E, Zetherstrom G. Regression of back and posterior pelvic pain after pregnancy. Spine (Phila Pa 1976) 1996;21:2777–2780. doi: 10.1097/00007632-199612010-00013. (Evidence level: 2A)
- ↑ 32.0 32.1 32.2 32.3 Shah S, Banh T.E, Koury K, Bhatia G, Nandi R, Gulur P. Pain management in pregnancy: multimodal approaches. Pain Res Treat 2015. 10.1155/2015/987483. (Evidence level: 2A)
- ↑ 33.0 33.1 33.2 33.3 33.4 33.5 33.6 Sandler SE. The Management of Low Back Pain in Pregnancy. Manual Therapy. 1996; 1(4):178-1857 Diagnostic Procedures15 Recent Related Research [PubMed] (Evidence level: 3A)
- ↑ 34.0 34.1 34.2 34.3 Vleeming, Andry, et al. European guidelines for the diagnosis and treatment of pelvic girdle pain. European Spine Journal 17.6 (2008): 794-819. (Evidence level: 3A)
- ↑ Sandra Brouwer; Reliability ad stability of the Roland Morris Disability Questionnaire; Disability and rehalbilitation; 2004; 26(03):162-165 (Evidence level: 2B)
- ↑ Mens, Jan MA, et al. Responsiveness of outcome measurements in rehabilitation of patients with posterior pelvic pain since pregnancy. Spine 27.10 (2002): 1110-1115. (Evidence level:3B)
- ↑ 37.0 37.1 Van De Pol, G., et al. The Pregnancy Mobility Index: a mobility scale during and after pregnancy. Acta obstetricia et gynecologica Scandinavica 85.7 (2006): 786-791. (Evidence level: 2B)
- ↑ 38.0 38.1 Mens JM, Huis YH, et al. Technical and measurement report: The Active Straight Leg Raise test in lumbopelvic pain during pregnancy. Manual Therapy 17 (2012) 364e368 (Evidence level: 2C)
- ↑ 39.0 39.1 39.2 39.3 39.4 Katonis P., Review article: Pregnancy-related low back pain. Hippokratia 2011, 15, 3: 205-210 (Evidence level: 2A)
- ↑ de Groot, Mirthe, et al. The active straight leg raising test (ASLR) in pregnant women: differences in muscle activity and force between patients and healthy subjects. Manual Therapy 13.1 (2008): 68-74. (Evidence level: 3B)
- ↑ 41.0 41.1 Roussel, Nathalie A., et al. Low back pain: clinimetric properties of the Trendelenburg test, active straight leg raise test, and breathing pattern during active straight leg raising. Journal of manipulative and physiological therapeutics 30.4 (2007): 270-278. (Evidence level: 4)
- ↑ Cullaty M. Suspected Sacroiliac Joint Dysfunction: Modifying Examination and Intervention During Pregnancy. Journal of Women's Health Physical Therapy. 2006; 30(2): 18-24 (Evidence level: 2C)
- ↑ 43.0 43.1 Stuge B., Hilde G., Vollestad N. . Physical therapy for pregnancy-related low back and pelvic pain: a systematic review. Acta Obstet Gynecol Scand 2003: 82: 983—990 (Evidence level: 1A)
- ↑ Mens JM, Snijders CJ, Stam HJ. Diagonal trunk muscle exercises in peripartum pelvic pain: a randomized clinical trial. Phys Ther. 2000;80:1164–1173. [PubMed] (Evidence level: 1B)
- ↑ Wang SM, Dezinno P, Lin EC, Lin H, Yue JJ, Berman MR, et al. Auricular acupuncture as a treatment for pregnant women who have low back and posterior pelvic pain: a pilot study. Am J Obstet Gynecol. 2009;201:271–e271. [PMC free article] [PubMed] (Evidence level: 3B)
- ↑ Ehrlich G., Low Back pain. Bulletin of the World Health Organization 2003, 81 (9) (Evidence level: 2C)
- ↑ Granath AB, Hellgren MS, Gunnarsson RK, Water aerobics reduces sick leave due to low back pain during pregnancy. J Obstet Gynecol Neonatal Nurs. 2006 Jul-Aug;35(4):465-71 (Evidence level: 1B)
- ↑ 48.0 48.1 Borg-Stein J., Dugan S. A. Musculoskeletal disorders of pregnancy, delivery and postpartum. Physical Medicine and Rehabilitation Clinics of North America. 2007;18(3):459–476. doi: 10.1016/j.pmr.2007.05.005. (Evidence level: 4)
- ↑ 49.0 49.1 Haugland K. S. , Rasmussen S., Daltveit A. K. .Group intervention for women with pelvic girdle pain in pregnancy. A randomized controlled trial, Acta Obstetricia et Gynecologica. 2006; 85: 1320 1326 (Evidence level: 1B)
- ↑ Oswald C, Higgins C. eta al. , Optimizing pain relief during pregnancy using manual therapy. Canadian Family Physician August 2013 vol. 59 no. 8 841-842. [PubMed] (Evidence level: 3A)
- ↑ Brosseau L., Wells G., et al. Ottawa Panel evidence-based clinical practice guidelines on therapeutic massage for low back pain. Journal of Bodywork and Movement TherapiesfckLRVolume 16, Issue 4 , Pages 424-455, October 2012 (Evidence level: 1B)
- ↑ George JW, Skaggs CD, Thompson PA, Nelson DM, Gavard JA, Gross GA. A randomized controlled trial comparing a multimodal intervention and standard obstetrics care for low back and pelvic pain in pregnancy. Am J Obstet Gynecol 2013;208(4):295.e1-7. Epub 2012 Oct 23. (Evidence level: 1B)
- ↑ Khadilkar A, Odebiyi DO, Brosseau L, Wells GA. Transcutaneous electrical nerve stimulation (TENS) versus placebo for chronic low-back pain. Cochrane Database Syst Rev. 2007;3:CD003008. (Evidence level: 1A)
- ↑ Martins, Roseny Flávia, and João Luiz Pinto e Silva. Treatment of pregnancy-related lumbar and pelvic girdle pain by the yoga method: a randomized controlled study. The Journal of Alternative and Complementary Medicine 20.1 (2014): 24-31. (Evidence level: 1B)
- ↑ Field T., Prenatal exercise research, Infant Behavior & Development 35 (2012) 397– 407 (Evidence level: 2A)