Headaches and Dizziness
Introduction[edit | edit source]
Headaches and dizziness have numerous causes and there are many different types. This page will explore some of the:
- Key types of headaches and causes of dizziness that may be encountered in clinical practice
- Highlight red flags and other signs / symptoms which warrant referral.
Headache Classification[edit | edit source]
Headaches are grouped into three main areas:[1]
- Primary headaches
- Secondary headaches
- Neuropathies, facial pain and other headaches
Primary Headache[edit | edit source]
Primary headaches are the most common headache type.[2]
- These headaches include migraines, tension headaches, trigeminal autonomic cephalgias, and other primary headache disorders.[3][1]
- They are not caused by other anatomical or physiological abnormalities.
- They are not related to inflammation or infections.[2]
Migraine[edit | edit source]
Migraine is a recurrent headache disorder which affects around 15 percent of the population aged 22-55 years.[4]
- Generally begins in childhood to early adulthood although it can start later in life for some perimenopausal / menopausal women[3]- can be influenced by "female reproductive milestones, including menstruation and perimenopause"[5]
- Estimated that ten percent of children experience migraines[6]
- Affects women more than men[4]
- Tends to run in families thus considered a genetic disorder[4][7]
- Has significant personal and economic effects[1]
- In the 2016 Global Burden of Disease Study - listed as the sixth most prevalent out of 328 diseases and injuries assessed.[8]
Migraines
- Characterised as recurrent episodes of headaches with visual or sensory symptoms.[3]
- In some cases of migraine, a headache will occur with no warning signs and resolve with sleep.[4]
- Sometimes prior to migraine, patients will experience a prodromal phase, with symptoms such as fatigue, euphoria, depression, irritability, food cravings, constipation, neck stiffness, increased yawning, and / or abnormal sensitivity to light, sound, and smell.[4]
- Migraines can also present with transient hemiplegic episodes. These cases require further medical investigation.[3]
- Usually unilateral, have a pulsating quality and are aggravated by activity.
- Last from a few hours up to a few days.[4]
- In children are generally bilateral frontal temporal headaches. It has been considered a red flag symptom if they occur in the occipital region,[3] but this has been disputed in some recent research.[9]
Migraines can occur with or without aura.
- Migraine without aura: will generally last from four to 72 hours. Typically, pain is unilateral and of a moderate to severe pulsing type and it is aggravated by physical activity. Nausea, vomiting, photophobia, and phonophobia often accompany it[1][3]
- Migraine with an aura: an aura refers to a sensory or neurological symptom that occurs before the migraine starts. It is usually visual - typically some type of a zigzagging crescent shape formation that occurs in the visual field,[3] but it can also refer to sensory and / or speech or language symptoms. There is no motor weakness and it develops gradually. Each symptom typically lasts no longer than an hour[1]
Tension Type Headaches[edit | edit source]
Tension type headaches (TTH) are the most prevalent of primary headaches in the general population.[10] There are four types of TTH:[1]
- Infrequent
- Frequent
- Chronic
- Probable
- Lifetime prevalence rates range from 30 to up to 78 percent[1][11]
- TTH are ranked as the third most prevalent condition in the Global Burden of Disease Study of 2016[8]
- More common in women[3]
TTH
- Classified as recurrent episodes of headaches.
- May last a few minutes or continue for weeks.[12]
- Usually consist of a pressing or tightening pain, that is non-throbbing in nature, of mild to moderate intensity that originate in the temporal region.[3][12]
- They are bilateral and do not get worse with activity.
- Nausea and vomiting are usually absent, photophobia and phonophobia can occur.[12]
- Usually accompanied by excessive tone of the suboccipital or neck muscles.
- Manual therapy is usually an effective intervention for this type of headache.[3]
- TTH have previously been associated with stress or psychogenic causes however there are numerous studies that suggest a neurobiological basis.[12][1]
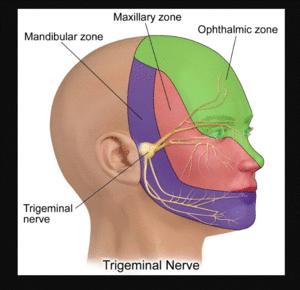
Trigeminal Autonomic Cephalalgias[edit | edit source]
Trigeminal autonomic cephalalgias (TAC)
- Primary headaches that occur with unilateral pain in the trigeminal distribution in the head.
- Occurs with cranial parasympathetic autonomic symptoms (such as eye watering, droopy eyelids or ptosis, nasal congestion), these features are lateralised and ipsilateral to the headache.[1][3]
- Typically of short duration.
There are five different types of TACs:[1]
- Cluster headaches
- Paroxysmal hemicranias
- Short-lasting Unilateral Neuralgiform Headache Attacks (either with conjunctival injection and tearing (SUNCT) or cranial autonomic symptoms (SUNA))
- Hemicrania continua
- Probable TAC
Cluster headache is more common, the other three types of trigeminal autonomic cephalgia are fairly rare.[3]
Cluster headaches
- Recurrent
- Characterised by severe unilateral pain, which has ipsilateral autonomic symptoms and often also causes restlessness and / or agitation.[13][14]
- Due to the severity of the pain, they can have a major impact on a patient’s quality of life.[14]
- The pain is located behind the eye and autonomic symptoms can include eye watering and nasal congestion.[3]
- Can last from 15 minutes to three hours and they occur in clusters.
- Clusters can last from weeks to months or sometimes over a year.[3]
- Cause is unknown, but it is thought to involve a coordinated, abnormal activity in the hypothalamus, the trigeminovascular system and the autonomic nervous system.
- Appears that the hypothalamus has a major part in generating the state that initiates an episode. The attacks themselves likely also require involvement of the peripheral nervous system.[14]
Risk factors for cluster headaches include:[3]
- A history of exposure to tobacco smoke
- A family history of the condition
They can be triggered by alcohol and nitro-glycerine.[3]
New Daily Persistent Headache[edit | edit source]
New daily persistent headache occurs in patients who have no previous history of headache.[1]
- In order to be classified as a new daily persistent headache, it must occur daily for more than three months.
- Usually has a rapid onset from a specific time - this onset has to be recalled by the patient if it is to be considered / classified as a new daily persistent headache.[1]
- Pathogenesis of this condition is not well understood. It may be due to abnormal glial activation with persistent central nervous system inflammation. It may also be associated with patients who have a history of cervical hypermobility.[15]
Secondary Headache[edit | edit source]
Headaches that can be related to an underlying medical condition or process, as well as trauma to the head or neck, infection or other disorders.[16][1]
- Many different types of secondary headaches, including primary exercise headache, occipital headache versus occipital neuralgia, sleep apnoea headaches, external compression headaches, idiopathic carotidynia headache, post-traumatic headache, medication overuse headache, trauma to the head and neck type headache, infections that cause headaches, substance abuse or substance withdrawal type headache and concussion.[1]
Primary Exercise Headache[edit | edit source]
Primary exercise headache (PEH) is a type of headache with no intracranial pathology that occurs during or after exercise or exertional activity, such as a valsalva or strain manoeuvre.[17][3]
- Prevalence of PEH varies across studies, relatively rare compared to other headaches.[17]
- Can occur in hot weather or at altitude
- Exercise is usually sustained, strenuous, and focused on endurance.[3]
- Generally bilateral, pulsating or throbbing without nausea or vomiting.[17]
- Due to its throbbing nature, PEH symptoms can appear similar to subarachnoid haemorrhage symptoms (see below).[3]
- Lasts anywhere from five minutes to 48 hours.[17]
- There is no specific cause or disorder to produce it,[3] but it has been proposed that dysregulated cerebrovasculature may be involved.[17]
- It usually resolves when the specific exertion stops or is avoided.[3]
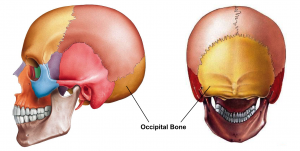
Occipital Headache vs Occipital Neuralgia[edit | edit source]
Current research is still unable to distinguish the cause of occipital headaches.[18]
- Can be a feature of migraine headaches and TTH.
- Thought to be initiated by tension in the shoulder, neck and scalp region that insert in the occipital region.
- May be due to compression, inflammation or irritation of the C2 sensory nerve roots[18]
- May be due to dysfunction of the craniovertebral joints or upper cervical zygapophyseal joints.[3]
- Occipital neuralgia is usually due to trauma or irritation of the occipital nerve .[19]
- Causes a paroxysmal shooting or stabbing pain in the distribution of the greater or lesser occipital nerves or the third occipital nerve.[3]
- Tenderness and sensory changes in the distribution of the nerve can occur.
- If cervical distraction alters an occipital headache, the headache may be due to a cervical structure issue.[3]
Sleep Apnoea Headache[edit | edit source]
Morning headache (i.e. occurring within 30 minutes of waking) has been associated with sleep apnoea.[3][20] However, it is important to remember that morning headaches can have two other causes:[3]
- Possibility of a tumour
- Hypertension - if blood pressure is over 160/100
Sleep apnoea headaches are classified based on the following criteria:[20]
- Morning headache
- Usually bilateral
- Duration of less than 4 hours
- Caused by sleep apnoea but no time restriction is given for improvement of headache following treatment of sleep apnoea
It is not yet clear if the headaches are due to hypoxia (reduced oxygen levels), hypercapnia (increased carbon dioxide levels) or sleep apnoea severity.[3][20]
External Compression[edit | edit source]
This type of headache has not been studied extensively,[21]
- Related to the ongoing stimulation of the cutaneous nerves due to pressure over the forehead or scalp[21] - e.g. due to wearing tight goggles, face masks, helmets, sweatbands, tight hats for a prolonged period of time.[3]
- Pain tends to be constant and worse in the area where the pressure is applied.[21]
- May involve the supraorbital nerve, and can progress to become a migraine if the stimulus is maintained.
- Usually resolves when the pressure is removed.[21][3]
Carotidynia Type Headache[edit | edit source]
- Tends to be considered an idiopathic, benign self-limiting condition.[22]
- Occurs unilaterally in the frontal temporal facial or orbital regions.
- Can be subtle and gradual or instantaneous and, like primary exercise headaches, it can present like a subarachnoid haemorrhage.
- Described as a constant aching, throbbing or sharp.[3]
- Patients tend to report tenderness over the carotid bifurcation in the neck,
- This condition may be associated with a distinct thickening of the wall of the artery in the region. However, this thickening does not have an impact on the blood flow and it is speculated that it may be related to inflammation.[3]
Post-Traumatic Headache[edit | edit source]
Secondary headaches due to trauma - eg subdural haematoma, epidural haematoma, intracranial or intracerebral hematoma, aneurysm, subarachnoid hemorrhage or cerebral contusion.[3]
- If a patient reports that she / he is experiencing the worst headache of his or her life, this is a sign of a serious vascular event. This patient will need to seek medical care urgently.[3]
Headaches Related to Head and Neck Trauma[edit | edit source]
- Some of the most common secondary headaches.
- Tend to resemble migraines or tension type headaches.[1]
Diagnosis is made based on the relationship between headache onset and head / neck trauma. Headache must be reported to have developed:[1]
- Within 7 days following trauma or injury
- Or within 7 days of regaining consciousness
- And / or within 7 days of recovering the ability to sense and report pain
Assessment and Management of Concussion[edit | edit source]
- Concussion does not generally cause severe neurological deficit. However, when there is a loss of consciousness associated with concussion, this means that there has been a temporary lack of activity in the brainstem, and headaches can occur in relation to concussion.[3]
- Headache may occur in conjunction with other symptoms following trauma, such as dizziness, fatigue, reduced ability to concentrate, slowed psychomotor ability, memory problems, insomnia, anxiety, irritability and personality changes. If several of these features occur post injury, the patient may be diagnosed with post-concussion syndrome.[3]
Medication Overuse Headache[edit | edit source]
- Overuse of medication can cause headache.
- Classified as occurring 15 or more days per month.
- Patients have a pre-existing primary headache, but develop a new headache, or worsening of their existing headache as a result of regular overuse of medication (on 10 or more or 15 or more days/month, depending on the medication) for more than three months.
- This headache usually resolves when the medication is stopped.[1][3]
Headache Related to Substance Abuse[edit | edit source]
Headaches can also be related to substance abuse eg alcohol, drug abuse, exposure to toxic substances, medication overviews, or it can be related to substance withdrawal coming down off of drugs or coming down off of alcohol.[3]
Serious Pathologies in Headache[edit | edit source]
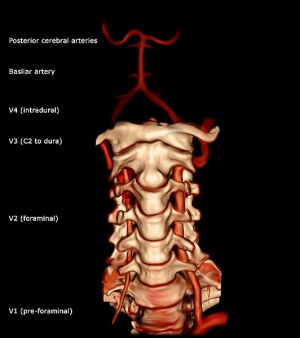
Cerebral Vascular Accidents[edit | edit source]
The presence of headache in a cerebral vascular accident will depend on the size of the haemorrhage or the presence of cerebrovascular disease.[3]
With vertebral artery insufficiency, the patient may have dizziness, visual disturbances and nystagmus when they combine rotation, extension and side flexion of the neck. See Vertebral Artery Test
- Head or neck pain may be one of the first signs of vascular pathology.[3]
- Cerebral ischaemia can be caused by vertebrobasilar insufficiency due to atherosclerosis or arterial compression.
- The vertebral artery can be compromised by degeneration of the joints, osteophyte encroachment, loss of disc height, instability of the cervical spine.[3]
Headache can also be related to hypertension.
- Hypertensive headaches can be diffuse, pulsating and aggravated by activity.[3]
- Some morning headaches are due to hypertension. Patients with blood pressure of over 160/100 may experience confusion, reduced level of consciousness, visual issues, and seizures.
- The headache occurs with the elevation of blood pressure and will resolve when the hypertension is controlled.[3]
Intracranial bleeding (either arterial or venous)
- Can be due to trauma or aneurysm
- Effects can be immediate or occur over a period of a few days.
- Haemorrhage can cause head, facial, eye or neck pain, can be local or diffuse.
- A patient can also present with neck stiffness, nausea and vomiting.[3]
- There can be upper motor neuron symptoms of hyperreflexia, positive plantar responses, positive Babinski, clonus, ataxia as well as photophobia, sensory or motor system disturbance, fainting, and the five Ds may be present:[3]
- Dizziness
- Diplopia
- Dysarthria
- Dysphagia
- Drop attacks - i.e. when a patient collapses but remains alert - they are unable to move and it can involve nystagmus. They tend to remain still with eyes closed
Neoplasm[edit | edit source]
There are four different classifications of brain neoplasms:[3]
- Astrocytoma, which are benign
- Oligodendrogliomas, which are benign
- Meningiomas, which are fast-growing and make up 20% of neoplasms of the brain. Grade three meningiomas are malignant meningiomas
- Metastatic spots - these can be single or multiple, and occur when cancer spreads from other regions in the body
Headache prevalence in patients with intracranial tumours ranges from 32 percent to 71 percent.[1] According to the ICHD-3, this sort of headache will have at least one of the following features:[1]
- It is progressive
- It is worse in the morning and / or when lying down
- It is aggravated by Valsalva-like manoeuvres
- It is accompanied by nausea and / or vomiting
Even if the neoplasm is benign, it is space occupying and, thus, generates pressure on neurological tissue and increases intracranial pressure.[3] 50 percent of headaches associated with neoplasm are occipital, frontal transient and increasing steadily.[3] Headache is not usually the only symptom associated with intracranial tumour (isolated headaches only occur in 2 percent to 16 percent of patients) - there will usually be other symptoms such as neurological deficits and seizures.[1]
Giant Cell Arteritis[edit | edit source]
Giant cell arteritis (formally known as temporal arteritis)
- Occurs almost exclusively in individuals over the age of 50 and increases in frequency with age.
- More prevalent in people of Scandinavian or Northern European descent.[3]
- Of all arteritides and collagen vascular diseases, giant cell arteritis is most often associated with headache (due to to inflammation of cranial arteries, particularly branches of the external carotid artery, as occurs with giant cell arteritis).[1]
Cause
- Caused by inflammation and damage to the blood vessels that supply the head, neck and upper arms.[3]
- Believed to be due in part to a faulty immune response.
- Has been linked with some infections in certain genes[3]
- Related to polymyalgia rheumatica (PMR) in patients aged over 50 years.[23]
- If patients present with temporal headache, it is important to refer them on to a specialist for biopsy of the temporal artery to determine if there is an inflammatory process going on.[3]
NB: Polymyalgia rheumatica is an inflammatory problem associated with hip and shoulder pain. Classic signs of PMR are morning stiffness lasting more than an hour, causing difficulty getting out of a chair.[3]
Presentation
- Headache is the most common symptom for patients with giant cell arteritis
- The actual features of the headache can be varied - it can occur anywhere on the head, and intensity can range from mild to severe. Similarly, it can be either a dull or throbbing type pain.[24]
- Other symptoms can include tenderness of the scalp, especially in the temporal region, fever, malaise, jaw pain with chewing, arm pain after use, muscle aches, pain and stiffness in the neck, upper arms and hips, weakness and fatigue.[3]
- Blurred and or double vision can occur, as can reduced vision and blindness. In this instance, it is essential that a patient is referred immediately to a specialist as this is an ophthalmic emergency.
- A cough, tongue or throat pain, hearing loss and joint stiffness are also possible with this condition. These patients must be referred immediately to a physician or to a rheumatologist.[3]
Takayasu Arteritis (i.e. inflammation of the aorta)[edit | edit source]
- Rare type of vasculitis[3] that can also cause headache.[25]
- Can cause blockage or narrowing of the artery (stenosis) or an abnormality or dilation of artery, such as aneurysms.
- Can also lead to arm and chest pain, high blood pressure, and eventually lead to heart failure or stroke.[3]
Red Flags Associated with Headaches[edit | edit source]
There are various red flags associated with headaches. These include:
- Headaches that worsen over time[26]
- A headache of insidious onset over a period of six months will also heighten the index of suspicion[3]
- Sudden onset of severe headache
- Headaches that occur in conjunction with high fever, stiff neck, or rash
- Headaches that begin after head injury[26]
- Headaches that occur with projectile vomiting in the absence of nausea - this type of headache is often related to an increase in intracranial pressure[3]
- Problems with vision or profound dizziness[26]
- Any kind of sudden, severe, diffuse pain that causes an individual to wake from sleep. This sort of pain is often associated with elevated blood pressure
- Headaches that worsen with activity or when lying down - headaches that are musculoskeletal in origin, tend to improve when lying down
- Focal tenderness over the temporal artery
- Visual changes over the age of 60
- Anything that occurs with a sharp pain of short duration or minimal cause
- A severe pain around the sinuses and teeth.
- Headaches with altered mental faculties, visual changes and altered sensation
- The five Ds (see below)
- Episodes of blacking out
- Strength, coordination, balance and gait disturbances
- Loss of senses such as hearing, smell or taste
- Difficulty swallowing and or tingling around the lips
- Loss of voice and a chronic cough[3]
Specific Considerations When Assessing the Cervical Spine[edit | edit source]
It is important when assessing patients with cervical spine issues, to always ask the following questions:[3]
- Is there any dizziness, vertigo, blackouts, drop attacks or any other of the 5 Ds?
- Is there a history of upper respiratory tract infections? This is especially important in children as they can cause bacterial tracking through the pharyngeal artery system to the carotid arterial arcade around the atlas and can cause temporary instability
- Is there a history of RA or other inflammatory arthritis? These can cause attenuation of the transverse ligament
- Has there been periodic loss of consciousness? This can be a sign of a cerebral or brainstem infraction
- Has there been any hemiparesis or facial paralysis? This again could be due to a brainstem infarction
- Are there any neurological symptoms?
- Are there any bilateral or quadrilateral signs?
- Are there cranial nerve signs, such as dysphasia, dysarthria, visual deficits, diplopia? These can be due to brainstem ischaemia or infarction
- What is the effect of coughing on pain? Any changes in pain may be due to a neoplasm
- And ask about headaches specifically - what causes the headaches? When do they occur? Do they change with lying down? Are they worse in the morning?
The 5 Ds[edit | edit source]
The 5 Ds are:[3]
- Dizziness
- Diplopia - double vision
- Dysarthria - trouble talking
- Dysphagia - trouble swallowing
- Drop attacks
These signs are associated with vertebrobasilar insufficiency (VBI). VBI is defined as inadequate blood flow through the posterior circulation of the brain.[27]
Dizziness[edit | edit source]
There are many different causes of dizziness. It can occur with infections, as well as due to psychological issues, upper cervical spine dysfunction and disorders of the vestibular system (either of peripheral cause (e.g. BPPV) or central origin (e.g. central neurological diseases and cervical artery or vertebral artery insufficiencies)).[3]
There are four key types of dizziness:[3]
- Vertigo - a spinning sensation - either the person feels she / he is spinning or the room is spinning
- Light-headedness - a sense of passing out or feeling faint, which is associated with vascular issues (I.e. hypotension)
- Oscillopsia - a sense that the environment is in motion - it is usually caused by abnormal eye movements or an impaired vestibulo-ocular reflex[28]
- Disequilibrium or feeling off balance or unable to maintain balance - this can be of vestibular origin - either central or peripheral
Cervical Vertebral Artery vs Benign Paroxysmal Positional Vertigo[edit | edit source]
As mentioned above, dizziness can occur due to Benign Paroxysmal Positional Vertigo (BPPV) or cervical vertebral artery dysfunctions. It is important to be able to differentiate between these two conditions.
Before conducting an assessment of the vertebral artery, it is important to consider if there are any risk factors which would alter or contraindicate testing. These include:[3]
- cardiovascular disease
- diabetes
- trauma, or past history of trauma - e.g. has there been a history of motor vehicle accident with whiplash? If the patient has lost his or her balance after getting out of the car, she / he would need to see a vascular surgeon immediately as damage or dissection of the vertebral artery may have occurred
- Anticoagulant use
- Infection
- Postpartum women - some women can have disorders of coagulation immediately postpartum
- Long term steroid use
Testing Sequence[edit | edit source]
If you are assessing a patient and you are not sure their dizziness is vascular or vestibular, it is important to rule out the cervical vertebral artery first.[3] The two key tests used are the cervical artery test and the modified cervical artery test.
The modified test is performed in sitting (see video below). As described by Dent,[3] the procedure for this test is as follows:
- The therapist places his / her hands on both sides of the patient's cervical spine and pulls the patient towards himself / herself. This brings the cervical spine into extension.
- The therapist watches the patient’s eyes for at least 20 seconds.
- If this position is tolerated and there are no symptoms or nystagmus, the therapist brings the patient into cervical rotation.
- Again, the position is held for 20 seconds in one direction, while the therapist watches the patient’s eyes, before returning to the midline still in extension.
- The therapist waits and watches the patient's eyes for another 20 seconds and then rotates.
- The therapist watches the patient’s eyes for a further 20 seconds, before bringing him or her back to the midline and then back into neutral.[3]
This test is, in theory, designed to test the vascular supply to the brain while compromising the vertebral artery circulation.[30] This enables the tester to see if any symptoms are reproduced.[3] There is not, however, sufficient evidence to support this test as a means of ruling vertebrobasilar insufficiency out,[30] but it is considered the best test at present.[3] If cervical artery insufficiency is suspected, the patient must be referred to a physician for further testing.[3]
Benign Paroxysmal Positional Vertigo[edit | edit source]
BPPV is a peripheral disorder of the vestibular system.
- The most common inner ear disorder that can cause dizziness or vertigo.[31]
- Caused by either canalithiasis or cupulolithiasis.[31]
- In theory, it can affect any of the three semicircular canals in the vestibular system, however it is very rare for the superior canal to be involved.[31]
BPPV is a short, episodic, mild to intense case of dizziness, which may involve nausea and vomiting.[3]
- In 90 percent of patients, the posterior canal is involved and the cause is believed to be canalithiasis.[3][31]
- BPPV commonly occurs at ages 50 to 70 years.[3]
- Usually (50-70%) found in isolation and is classified as primary or idiopathic BPPV.[31]
- Secondary BPPV is usually caused by head trauma - this makes up around 7-17% of cases.[31] It tends to be more commonly connected to trauma or infection (i.e. of the inner ear) in patients aged less than 50 years.[3]
- There is no imaging option for BPPV. The Dix Hallpike manoeuvre is the gold standard test used to screen for BPPV of the posterior canal.[31] A positive response is nystagmus and the complaint of vertigo. The intensity of the vertigo tends to correlate to the degree of nystagmus.[31]
The Dix-Hallpike
- Will generally enable the therapist to determine which side is affected; the downbeat nystagmus will go to the positive ear.[3]
- If the Dix-Hallpike manoeuvre is not conclusive, the supine roll test can be performed (see video below). A positive response will indicate lateral horizontal canal BPPV, which occurs in about 10 to 50 percent of BPPV patients.[3]
Unlike cervical artery testing, the Dix-Hallpike has been found to have a sensitivity of 82 percent, and specificity of of 71 percent if done by experienced clinicians.
- Positive predictive values in the primary care setting are 83 percent, but negative predictive values are low at only 52 percent.
- This means that a negative result cannot rule out a posterior BPPV.[34]
Summary[edit | edit source]
- There are many different types of headaches and dizziness, which can be encountered in clinical practice.
- Some signs require urgent referral and review and should always be considered when assessing a patient who has head or neck pain and dizziness.
References[edit | edit source]
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 1.16 1.17 1.18 1.19 1.20 Headache Classification Committee of the International Headache Society (IHS) The International Classification of Headache Disorders, 3rd edition. Cephalalgia. 2018; 38(1): 1-211.
- ↑ 2.0 2.1 Manzoni GC, Stovner LJ. Epidemiology of headache. Handb Clin Neurol. 2010;97:3-22.
- ↑ 3.00 3.01 3.02 3.03 3.04 3.05 3.06 3.07 3.08 3.09 3.10 3.11 3.12 3.13 3.14 3.15 3.16 3.17 3.18 3.19 3.20 3.21 3.22 3.23 3.24 3.25 3.26 3.27 3.28 3.29 3.30 3.31 3.32 3.33 3.34 3.35 3.36 3.37 3.38 3.39 3.40 3.41 3.42 3.43 3.44 3.45 3.46 3.47 3.48 3.49 3.50 3.51 3.52 3.53 3.54 3.55 3.56 3.57 3.58 3.59 3.60 3.61 3.62 3.63 3.64 3.65 3.66 3.67 3.68 3.69 3.70 3.71 3.72 3.73 3.74 3.75 Dent D. Headaches and Dizziness Course. Plus. 2020.
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 Burstein R, Noseda R, Borsook D. Migraine: multiple processes, complex pathophysiology. J Neurosci. 2015;35(17):6619-6629.
- ↑ Ornello R, De Matteis E, Di Felice C, Caponnetto V, Pistoia F, Sacco S. Acute and preventive management of migraine during menstruation and menopause. J Clin Med. 2021 May 24;10(11):2263.
- ↑ Rao R, Hershey AD. An update on acute and preventive treatments for migraine in children and adolescents. Expert Review of Neurotherapeutics. 2020. Published online.
- ↑ Bron C, Sutherland HG, Griffiths LR. Exploring the hereditary nature of migraine. Neuropsychiatr Dis Treat. 2021 Apr 22;17:1183-94.
- ↑ 8.0 8.1 GBD 2016 Headache Collaborators. Global, regional, and national burden of migraine and tension-type headache, 1990-2016: a systematic analysis for the Global Burden of Disease Study 2016. Lancet Neurol. 2018;17(11):954-976.
- ↑ Genizi J, Khourieh-Matar A, Assaf N, Chistyakov I, Srugo I. Occipital Headaches in Children: Are They a Red Flag?. J Child Neurol. 2017;32(11):942-946.
- ↑ Jensen RH. Tension-Type Headache - The Normal and Most Prevalent Headache. Headache. 2018;58(2):339-345.
- ↑ Bentivegna E, Luciani M, Paragliola V, Baldari F, Lamberti PA, Conforti G, et al. Recent advancements in tension-type headache: a narrative review. Expert Rev Neurother. 2021 Jul;21(7):793-803.
- ↑ 12.0 12.1 12.2 12.3 Chowdhury D. Tension type headache. Ann Indian Acad Neurol. 2012;15(Suppl 1):S83-S88.
- ↑ Russell MB. Epidemiology and genetics of cluster headache. Lancet Neurol. 2004;3(5):279-283.
- ↑ 14.0 14.1 14.2 Hoffmann J, May A. Diagnosis, pathophysiology, and management of cluster headache. Lancet Neurol. 2018;17(1):75-83.
- ↑ Rozen TD. New daily persistent headache: an update. Curr Pain Headache Rep. 2014;18(7):431.
- ↑ McGeeney B. Secondary headache: concepts and examples. Techniques in Regional Anesthesia and Pain Management. 2009; 13: 58-64.
- ↑ 17.0 17.1 17.2 17.3 17.4 Upadhyaya P, Nandyala A, Ailani J. Primary Exercise Headache. Curr Neurol Neurosci Rep. 2020;20(5):9.
- ↑ 18.0 18.1 Noseda R, Melo-Carrillo A, Nir RR, Strassman AM, Burstein R. Non-Trigeminal Nociceptive Innervation of the Posterior Dura: Implications to Occipital Headache. Journal of Neuroscience. 2019; 39(10): 1867-1880;
- ↑ Vanelderen P, Lataster A, Levy R, Mekhail N, Van Kleef M. and Van Zundert J. 8. Occipital Neuralgia. Pain Practice. 2010; 10: 137-144.
- ↑ 20.0 20.1 20.2 Suzuki K, Miyamoto M, Miyamoto T, et al. Sleep apnoea headache in obstructive sleep apnoea syndrome patients presenting with morning headache: comparison of the ICHD-2 and ICHD-3 beta criteria. J Headache Pain. 2015;16:56.
- ↑ 21.0 21.1 21.2 21.3 Krymchantowski, A.V. Headaches Due to External Compression. Curr Pain Headache Rep. 2010; 14, 321–324.
- ↑ Sempere Campello G, Arias Medina A, De Miguel P, Pilar D, Elena A et al. Carotidynia Syndrome. How to see it? Available from https://epos.myesr.org/poster/esr/ecr2015/C-2392 (accessed 7 September 2020).
- ↑ Buttgereit F, Dejaco C, Matteson EL, Dasgupta B. Polymyalgia Rheumatica and Giant Cell Arteritis: A Systematic Review. JAMA. 2016;315(22):2442–2458.
- ↑ Rozen TD. Brief sharp stabs of head pain and giant cell arteritis. Headache. 2010;50(9):1516-1519.
- ↑ Li-xin Z, Jun N, Shan G, Bin P, Li-ying C. Neurological manifestations of Takayasu arteritis. Chin Med Sci J. 2011;26(4):227-230.
- ↑ 26.0 26.1 26.2 Page P. Cervicogenic headaches: an evidence-led approach to clinical management. Int J Sports Phys Ther. 2011;6(3):254-266.
- ↑ Pirau L, Lui F. Vertebrobasilar Insufficiency. [Updated 2020 Jul 21]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK482259/
- ↑ Tilikete C, Vighetto A. Oscillopsia: causes and management. Curr Opin Neurol. 2011;24(1):38-43. doi:10.1097/WCO.0b013e328341e3b5
- ↑ TSPT Blog. Vertebral Artery Test. Available from: https://www.youtube.com/watch?time_continue=16&v=sxXZzUomTuQ&feature=emb_logo [last accessed 07/09/2020]
- ↑ 30.0 30.1 Alshahrani A, Johnson E, Cordett T. Vertebral artery testing and differential diagnosis in dizzy patients. Physical Therapy and Rehabilitation. 2014; 1(1): 3.
- ↑ 31.0 31.1 31.2 31.3 31.4 31.5 31.6 31.7 Parnes LS, Agrawal SK, Atlas J. Diagnosis and management of benign paroxysmal positional vertigo (BPPV). CMAJ. 2003;169(7):681-693.
- ↑ BMJ Learning. Vertigo - Dix-Hallpike Manoeuvre from BMJ Learning. Available from https://www.youtube.com/watch?v=8RYB2QlO1N4 [last accessed 07/09/2020]
- ↑ EducatedPT. Supine Roll Test for Horizontal Canal BPPV. Available from https://www.youtube.com/watch?v=ns8XZ4rKiJc [last accessed 07/09/2020]
- ↑ Hwang E, Tse D. Evidence-Based Practice. In Rudmik L editor. Evidence-Based Clinical Practice in Otolaryngology. Elsevier. 2018. p1-14.