Functional Anatomy of the Hip-Bones and Ligaments
Original Editor - Ewa Jaraczewska based on course of Rina Pandya
Top Contributors - Ewa Jaraczewska, Jess Bell, Kim Jackson, Lucinda hampton and Kirenga Bamurange Liliane
Description[edit | edit source]
The hip joint is considered one of the largest joints of the human body. It connects the pelvis to the lower extremities. The primary roles of the hip joint are to allow weight-bearing through the lower extremities and stability in standing and during mobility (i.e. walking or running).
"Our goal as therapists turns out to be that we alleviate the pain, enhance the movement mechanics, and also to reduce the work of the body, the energy expenditure, in order for the body to move effortlessly, seamlessly as much as possible". Rina Pandya
Structure[edit | edit source]
The hip joint is a ball-and-socket joint that provides stability for the body and is able to withstand forces that exceed total body weight many times. The hip joint is able to accept these large loads because of the combined work of the static and dynamic elements of the joint paired with proper body alignment.
- The static stabilisers include bones, ligaments, capsules and bursae.
- Muscles, fascia, tendons, nerves and vascular supply are all dynamic elements of the hip joint.
The movements that occur in the hip joint are:
- Sagittal plane: flexion/extension
- Frontal plane: abduction/adduction
- Transverse plane: medial/lateral rotation
Hip (thigh) circumduction is a movement performed in two planes: sagittal and frontal
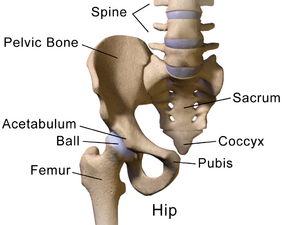
Bones[edit | edit source]
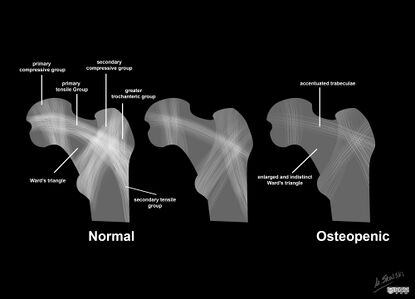
The hip joint has two bony structures: the acetabulum and the femoral head connected to the femoral shaft via the femoral neck. They contain the trabeculae (i.e. the supportive, connective tissue element that forms in cancellous bone). The growth of the trabeculae follows the lines of stress along the bone and it accepts the high forces that cross the joint.[1] During single-leg stance, these forces are two and a half times bodyweight, and during running, they increase to five times body weight. Wolff's law explains the formation of the trabecular pattern.
Wolff's law: a living bone will react to the mechanical forces exerted on it. These forces can be static or dynamic, internal or external. Internal forces are dynamic. External forces can be dynamic or static. Gravity is an example of static force. Weight-bearing is considered a dynamic force. The bone will go through a process of remodelling when the load is increased. As a result, it becomes stronger and can resist loading.[1][2]
"Knowledge of the trabeculae is extremely important because it will teach us and the body how to dissipate weight in the most energy-efficient manner". Rina Pandya
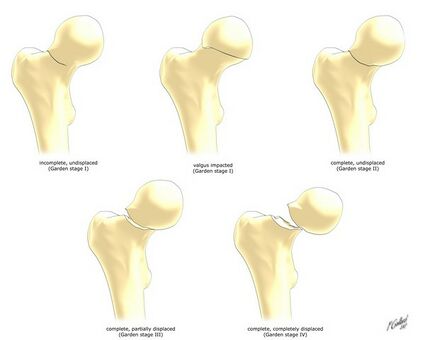
Garden Classification of Femoral Neck Fractures:
In this classification system, displacement is graded based on where the medial compressive trabecular sits:[2]
- Stage one: the medial trabeculae create an angle of 180 degrees.
- Stage two: the femoral head medial trabeculae create an angle of around 160 degrees with the femoral neck.
- Stage three: the medial trabeculae are not aligned with the trabeculae in the pelvis.
- Stage four: the medial trabeculae are aligned with the trabeculae in the pelvis.
Ward's triangle is located in the femoral neck at the intersection of three trabecular bundles. It is the area of the lowest bone mineral density and is, thus, susceptible to trauma. A systematic review and meta-analysis of over 20 randomised controlled trials by Zhou et al.[3] found that some forms of exercises (eg. Tai Chi) can improve bone mineral density in Ward's triangle.
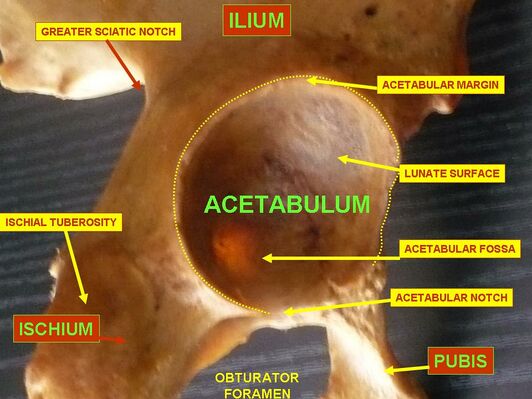
Acetabulum[edit | edit source]
The acetabulum is a lateral part of the pelvis. Its concave shape allows for the fitting of the femoral head. The femoral head is located at the proximal aspect of the femoral bone which connects distally to the tibia and the fibula.
A "normal" pelvis and acetabulum are difficult to define.[4] A better understanding of the topographic map of the acetabulum is important for creating a good anatomic implant design when replacement or reconstruction of the acetabulum is needed.[4] The superior and posterior walls of the acetabulum are in anteversion and abduction. The face of the acetabulum has an average of 20.7 degrees of anteversion and 39.8 degrees of abduction. The anterior portion of the acetabulum is flat while the posterior portion is angled with its highest point at the sciatic notch.[4]
75% of the margin of the acetabulum is a circle. The remaining part is the acetabular notch on the anteroinferior aspect. The transverse ligament of the hip closes the circle at this notch. This is where the acetabular labrum attaches, allowing for an increase in the articular area of the acetabulum. Because of this anatomical structure, 50% of the femoral head can fit into the acetabulum.[5]
The acetabulum is divided into anterior and posterior columns. The anterior column includes the anterior ilium, anterior wall, the anterior dome of the acetabulum, and superior pubic ramus. The posterior column consists of greater and lesser sciatic notches, posterior wall, the posterior dome of the acetabulum, and ischial tuberosity.[5]
Femoral Head[edit | edit source]
The femoral head completes the proximal aspect of the femur, which is the strongest bone in the human body. The head is pointed in a medial, superior, and slightly anterior direction. There are two bony protrusions on the femur known as the greater and the lesser trochanters. They serve as attachment points to the muscles responsible for hip and knee motion. The femoral head connects to the femur via the femoral neck which extends to the femoral shaft. The shaft has a mild anterior arch. Distally, the medial and lateral condyles join the femur to the tibia. The inclination angle is the angle between the femoral shaft and neck. On average, this angle is 128 degrees, but it tends to decrease as we age.[6]
Ligaments[edit | edit source]
The ligaments reinforcing the hip are divided into intra-articular and extra-articular ligaments.
There are two intra-articular ligaments:
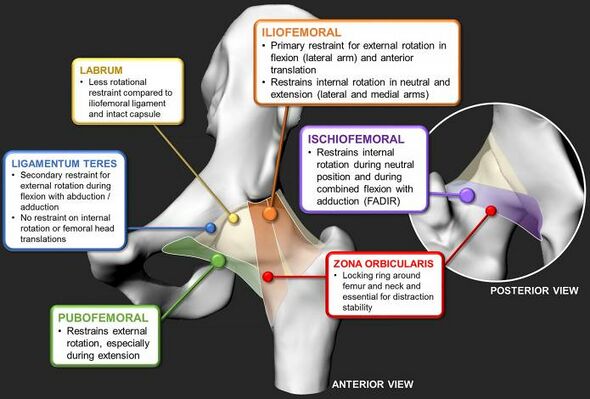
- Ligament of the femoral head (also known as the round ligament of the femur, ligamentum teres femoris (in above diagram), or the foveal ligament). This ligament attaches between the peripheral inferior acetabular notch and the fovea of the femoral head. The main functions include carrying small vessels and nerves to the femoral head and providing proprioception and structural stability to the hip joint by limiting abduction and external rotation when the hip is flexed.
- Transverse ligament of the acetabulum is in fact a fibrous structure that transforms the acetabular notch into a foramen. It channels nerves and vessels into the joint.[7]
The extra-articular ligaments are primary hip joint stabilisers and they include:[1]
- Iliofemoral ligament (also known as the Y ligament of Bigelow) contains lateral and medial fibrous branches. It stretches between the anterior inferior iliac spine, the acetabular rim and the intertrochanteric line/ the greater trochanter. The primary function of this ligament is to prevent hip hyperextension and external rotation in an upright position. In addition, it serves as a reinforcer of the anterior capsule.
- Ischiofemoral ligament is the weakest of the four ligaments and consists of a triangular band of fibres that form the posterior hip joint capsule. It inserts in the ischium, behind the acetabulum and attaches to the femur, medial to the greater trochanter. The ligament has two roles: it limits internal rotation and extension and reinforces the posterior portion of the capsule during internal rotation.
- Pubofemoral ligament originates at the pubic part of the acetabular rim and the superior pubic ramus and attaches to the lower part of the femoral neck. It limits abduction and external rotation during hip extension and reinforces the inferior capsule.
- Zona orbicularis is primarily a stabiliser of the hip joint. This ligament is formed by the circular fibres from the capsule, which contains fibres from all extra-articular ligaments. [7]
Joint Capsule[edit | edit source]
The hip joint capsule has two layers:
- External layer: The fibrous joint capsule is a supporting structure of the hip joint, contributing to the joint's overall stability.[8] It contains mechanoreceptors that monitor vibration and tensile loading in the hip joint. Pacinian corpuscles (i.e. large mechanoreceptors, which are sensitive to mechanical pressure and vibrations[9]) and Ruffini corpuscles (i.e. small, spindle-shaped receptors[9]) have the largest representation in the hip joint capsule, particularly in its superior-lateral aspect. In addition to Pacinian and Ruffini corpuscles, there are a smaller number of the Golgi Tendon Organs. The capsule, therefore, plays a role in pain perception and the fast muscular responses to the movements required to maintain stability.[10] Some research data suggests that there is a reduction in mechanoreceptor density in hip osteoarthritis, but no relationship to demographic information has been found.[10]
- Internal layer: Consists of the synovial membrane, which produces synovial fluid that lubricates the joint and carries the nutrients to the hip joint. It stretches between the margin of the articular surface of the femoral head and the ligament of the head of the femur covering the internal surface of the capsule.
Bursae[edit | edit source]
There are five bursae in the hip joint. Their primary role is to reduce friction between the bony components of the joint and the surrounding muscles.
The following is a list of hip bursae and their locations:[11]
- Trochanteric bursa: lateral insertion of the medial gluteus muscle and posterior trochanteric facet.
- Ischial bursa: between the ischial tuberosity and the gluteus maximus.
- Subgluteus medius bursa: between the tendon of gluteus medius and the lateral facet.
- Subgluteus minimus bursa: between the gluteus minimus tendon and the anterior facet of the femur.
- Iliopsoas bursa: between the musculotendinous part of the iliopsoas muscle and the anterior capsule of the hip.
Clinical relevance[edit | edit source]
- Coxa profunda is a pathology related to an increased depth of the acetabular socket.[12] This is a problem more commonly found in females.
- Acetabular retroversion refers to an abnormal posterior angulation of the superolateral acetabular rim. This pathology causes the femoral head to be excessively covered and predisposes individuals to femoroacetabular impingement. It is also considered a risk factor for osteoarthritis of the hip.[1]
- Deficits in the passive structures of the hip joint may lead to increased femoral head translation or shearing forces.[13]
- Development of larger cross-sectional areas and tighter capsular ligaments can be the result of progressive arthritis.[7]
- Freeman et al.[8] have found that a surgical procedure involving capsular closure restores the biomechanics of the hip.[8]
- Pathology of the iliopsoas bursa can be a consequence of hip osteoarthritis, hip inflammatory disease, or primary bursitis.[10]
Resources[edit | edit source]
- Hip Joint. The Lecturio Medical Concept Library: https://www.lecturio.com/concepts/hip-joint/
- Hip Joint. Radiology Reference Article: https://radiopaedia.org/articles/hip-joint-1
- Anatomy, Bony Pelvis and Lower Limb, Hip Joint: https://www.ncbi.nlm.nih.gov/books/NBK470555/
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 Pandya R. Anatomy of the Hip Course. Plus. 2022.
- ↑ 2.0 2.1 Shetty A, Hacking C. Trabecular pattern of proximal femur [Internet]. Radiopaedia.org. 2020 [cited 3 March 2022]. Available from: https://radiopaedia.org/articles/trabecular-pattern-of-proximal-femur
- ↑ Zhou Y, Zhao ZH, Fan XH, Li WH, Chen Z. Different training durations and frequencies of Tai Chi for bone mineral density improvement: A systematic review and meta-analysis. Evidence-Based Complementary and Alternative Medicine. 2021 Mar 16;2021.
- ↑ 4.0 4.1 4.2 Krebs V, Incavo SJ, Shields WH. Tthe anatomy of the acetabulum: what is normal? Clin Orthop Relat Res. 2009 Apr;467(4):868-75. doi: 10.1007/s11999-008-0317-1. Epub 2008 Jul 22.
- ↑ 5.0 5.1 Bannai M, Rock P. Acetabulum. Reference article. Radiopaedia.org. Available at https://radiopaedia.org/articles/acetabulum (last access 20.02.2022).
- ↑ Chang A, Breeland G, Hubbard JB. Anatomy, Bony Pelvis and Lower Limb, Femur. [Updated 2021 Jul 26]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK532982/
- ↑ 7.0 7.1 7.2 Ng KCG, Jeffers JRT, Beaulé PE. Hip Joint Capsular Anatomy, Mechanics, and Surgical Management. J Bone Joint Surg Am. 2019 Dec 4;101(23):2141-2151.
- ↑ 8.0 8.1 8.2 Freeman KL, Nho SJ, Suppauksorn S, Chahla J, Larson CM. Capsular Management Techniques and Hip Arthroscopy. Sports Med Arthrosc Rev. 2021 Mar 1;29(1):22-27.
- ↑ 9.0 9.1 Doll J. Peripheral mechanosensory receptors [Internet]. Kenhub. 2022 (cited 4 March 2022). Available from: https://www.kenhub.com/en/library/anatomy/peripheral-mechanosensory-receptors
- ↑ 10.0 10.1 10.2 Tomlinson J, Zwirner J, Ondruschka B, Prietzel T, Hammer N. Innervation of the hip joint capsular complex: A systematic review of histological and immunohistochemical studies and their clinical implications for contemporary treatment strategies in total hip arthroplasty. PLoS One. 2020 Feb 26;15(2):e0229128.
- ↑ Ivanoski S, Nikodinovska VV. Sonographic assessment of the anatomy and common pathologies of clinically important bursae. Journal of Ultrasonography. 2019 Nov;19(78):212.
- ↑ Anderson LA, Kapron AL, Aoki SK, Peters CL. Coxa profunda: is the deep acetabulum overcovered?. Clin Orthop Relat Res. 2012;470(12):3375-82.
- ↑ Retchford TH, Crossley KM, Grimaldi A, Kemp JL, Cowan SM. Can local muscles augment stability in the hip? A narrative literature review. J Musculoskelet Neuronal Interact. 2013 Mar 1;13(1):1-2.