Finger Dislocation
Original Editor - Puja Gaikwad
Top Contributors - Puja Gaikwad, Kim Jackson, Anas Mohamed, Shaimaa Eldib, Rucha Gadgil and Wanda van Niekerk
Introduction[edit | edit source]
Finger dislocation is a common hand injury that can occur at the proximal interphalangeal (PIP), distal interphalangeal (DIP), or metacarpophalangeal (MCP) joints and can also occur in the dorsal, volar, or lateral planes.[1] With numerous articulated joints connecting multiple small bones, the fingers are mostly at risk of dislocation when exposed to high impact activities and forced overstretching. Such forces are most typically experienced during sports, especially full-contact sports like rugby, basketball and football. However, progressive, repetitive strain on the joints during daily activities can weaken the joints increasing the possibility of dislocation.
A dislocated finger usually involves excessive forces exerted on the joint above the connective tissue tensile strength. This causes the tissue (often ligaments) going into partial or complete tear allowing the bony surfaces of the joint to slide far away from each other.[2] The remaining connective tissue, tendons, nerves, and blood vessels can get impinged by this movement causing excruciating pain. Depending on the severity of the dislocation the displaced bone can cause damage to the surrounding tissues in addition to damage experienced during its dislocation.
The foremost common joint to be dislocated is the proximal interphalangeal joint (PIPJ) of the middle joint in the finger.[3] When the forces involved are too much and beyond the capacity what the connective tissue and supporting muscles can withstand, one or more small bones of the fingers can displace or ‘pop out’ of their normal position. When this happens, the condition is called a "dislocated finger" and it may affect one or more IP or MCP joints. Forces applied at the time of the injury will depend on the direction of dislocation. Some dislocations may be associated with a fracture or damage to the ligament that supports the sides and front of the joint with the risk of long-term instability.[4]
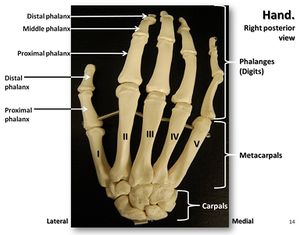
Clinically Relevant Anatomy[edit | edit source]
Fingers consist of three joints: Metacarpophalangeal (MCP) joints, proximal interphalangeal (PIP) joints, and the distal interphalangeal (DIP) joints. The MCP joint is located between metacarpals and proximal phalanges. The PIP and DIP joints are hinge joints between proximal and middle phalanges and between the middle and distal phalanges respectively. These PIP and DIP joints allow flexion and extension, which help in grasping, pinching, and clawing or reaching functions. The middle phalanx range of motion available at the PIP joint is 105° ± 5° and accounts for the fingertip flexion during grasping. Flexion and extension of the digit are also possible at the metacarpophalangeal joint; however, the MCP joint performs flexion, extension, adduction, abduction, and circumduction.[2]
The phalangeal joints have stabilizers that provide support during motion. There are static and dynamic joint stabilizers. Static stabilizers involve non-contractile tissue, collateral ligaments, volar plate, dorsal capsule, sagittal bands, ulnar, and radial collateral ligaments, etc. The volar plate is an important stabilizer as it holds up the volar side of the joint capsule and maintains stability and thereby prevents hyperextension of the finger joints.[1] The collateral ligaments provide stabilization against the radial and ulnar deviation of the IP joints. Sagittal bands encircle the metacarpophalangeal joint to keep the extensor tendon centralized and thereby prevent bowstringing. Dynamic stabilizers include extrinsic and intrinsic muscles and tendons. Two major dynamic stabilizers are central slip and lateral bands. The central slip tendon is placed dorsally and provides a PIP joint extension, and the lateral bands provide a DIP joint extension. Lastly, digital arteries and nerves are found in the volar aspect and appear on both ulnar and radial sides of the digits.[2]
Types Of Dislocation[edit | edit source]
There are three types of finger dislocation, based on the finger joint involvement. They are as follows:
- Distal interphalangeal (DIP) joint dislocation – occurs in the joints closest to the fingertip.
- Proximal interphalangeal joint dislocation – occurs in the joints in the middle of the finger and It's the most common sports injury, also called "jammed finger".
- Metacarpophalangeal (MCP) joint dislocation –occurs at the base of the finger. These types of joint dislocations are relatively rare, compared to the other two types.[5]
Also, there are three types of finger dislocations classified based on the displacement of the bones as follows:
- Dorsal dislocation: The phalanx near to the fingertip is displaced toward the back of the hand.
- Volar dislocation: The phalanx close to the fingertip is displaced toward the palm of the hand.
- Lateral dislocation: The phalanx proximal to the tip of the finger is displaced to the side.[5]
DIP Joint Dislocation[edit | edit source]
DIP joint dislocations classically present with a deformity at the fingertip. Dorsal, lateral, and volar DIP joint dislocations are all possible sites. Dorsal DIP joint dislocations occur most often and are related to fractures and skin injuries. They're not always related to flexor tendon avulsions but can have an interposed volar plate causing a non-reducible dislocation. Volar DIP joint dislocations are similar to dorsal PIP joint dislocations and both are associated with extensor tendon injuries. The lateral DIP joint is more likely to have post-reduction instability compared to volar or dorsal dislocations. Isolated DIP joint dislocation without related injuries like soft tissue or fractures is rare and is commonly managed with closed reduction and splinting in the emergency departments.[2][6]
PIP Joint Dislocation[edit | edit source]
PIP joint dislocation is a very common dislocation due to sporting activities and is also known as “coach’s finger.” The classical signs and symptoms of PIP joint dislocation is a deformity, reduced range of motion, and pain. PIP joint dislocations can be classified into dorsal, volar, and lateral dislocations. Dorsal dislocations are common; however, volar dislocation correlates with an increased rate of complications and often difficult reductions.[2][5]
- Dorsal PIP joint dislocation occurs most commonly at the middle finger and is associated with volar plate, collateral ligament, and dorsal joint capsule injuries. Dorsal dislocation results from longitudinal compression and hyperextension commonly occur by a ball hitting the tip of the finger. Swan neck deformity occurs mostly in dorsal dislocations and results from volar plate injury. Trapping of the volar plate inside the joint can occur, causing malalignment and oblique rotation resulting in challenging reductions.
- Volar dislocation of the PIP joint may result with and without rotation of the intermediate phalanx. It is rare but can occur in combination with injury to the central slip of the extensor tendon. If left untreated, after PIP joint dislocation rupture of the central slip is often associated with pseudo-boutonniere PIP flexion contracture. (Pseudo-boutonniere is a chronic PIP flexion with the absence of a DIP extension.)
- Lateral PIP dislocation may occur and involves the disruption of the collateral ligaments. The patient presents with joint instability and the widening of the joint space seen on x-ray. Finally, rotary volar dislocations can occur when the phalanx displaces and rotates around one of the collateral ligaments, allowing the proximal phalanx to wedge itself between the lateral band and extensor tendon. In the classic lateral radiographic finding, it has been known as the “Chinese finger-trap.”[2]
Metacarpophalangeal Joint Dislocation[edit | edit source]
Hyperextension or high-energy axial loads at the metacarpophalangeal joint may result in dislocation. MCP joint dislocation infrequently occurs due to the protection against hyperextension by the volar plate and radial and ulnar deviation by the collateral ligaments. The foremost common MCP joint dislocation occurs in the index finger. Dislocation of the MCP joint of the middle finger happens when it's subjected to ulnar stress while in hyperextension.[1] The common MCP joints usually dislocate dorsally.[5] The clinical presentation of MCP joint dislocation is with the IP joint in flexion and MCP joint in extension. A nonreducible dislocation with dimpling on the volar surface shows volar plate interposition.[2]
Etiology[edit | edit source]
Finger dislocation is caused by a "jamming" force applied to the end of the finger, or the finger could also be forced into hyperextension. Either of these situations or a combination of both may result in a dislocation. The possible causes of a dislocated finger can include:
- Sports injuries: They are common causes of dislocated fingers. According to a research review, around half of all sports-related hand injuries affect the fingers.[2] Sports with the highest incidence of hand injuries include football, cricket, netball, gymnastics, basketball, lacrosse, and wrestling, etc. are at higher risk of finger dislocation due to the increased exposure to jarring and overstretch forces. Especially sports played with a ball, can lead to the high impact of the IP joints in the fingertips and overstretch forces to the MCP joints when catching.[8] Fingers can also get accidentally trapped in clothing or equipment during tackles or experience jarring impacts from collisions or falls or even seen in martial arts.
- Fall: Finger dislocation is the result of excessive force applied to the joints of the fingers. It can happen to those trying to hold back themselves during an awkward fall onto an outstretched finger. The impact from the fall can push fingers beyond their normal range of motion and out of their joints and thereby causing dislocation.[9]
- Accidents: Rarely dislocations can occur during a violent incident or during a road accident.
- Genetics: Some people are born with weak ligaments. Ligaments are tissues that connect bones at the joint and give structural support.
- Comorbidities: People with health conditions that weaken joints and ligaments could also be at greater risk of dislocations.
In all incidences, the key factor is that excessive force is applied to the joint, very commonly seen in hyperextension but can also be involved with a lateral force.
Clinical Presentation[edit | edit source]
Patients with a dislocated finger often experience a sudden onset of excruciating finger pain during the acute incident or causative activity. This is commonly associated with an obvious bump or deformity of the finger due to the displacement of the finger bones. An "audible pop" or tearing sound can be heard at the time of injury.
Pain could be felt on the front, back, or sides of the affected finger joint. Occasionally pain can also be referred further along the finger or into the hand on the affected side. Swelling can occur immediately or can progressively develop after a few hours of injury. The patient will not be able to bend or straighten the finger. Sometimes, a break in the bone may accompany the dislocation and will require prompt medical attention.
If the nerve is impinged or damaged as a result of the displaced finger then the patient may experience some of the following:
- Referred pain into adjacent fingers, palm, or even in the arm.
- Numbness felt especially distally to the site of dislocation.
- Altered sensations, such as pins and needles or heat sensitivity can be noted.
- The injured finger can appear pale.
Following the finger joints relocation, the patient will continue to experience symptoms as a result of the effects of dislocation. These symptoms may include:
- The patient may experience pain and stiffness which will increase with specific activities or with rest (particularly in the morning time).
- Symptoms could also be exacerbated with activities that involve the use of the hand and fingers like opening jars or doors, writing, typing, lifting heavy objects, basic gripping activity, cooking, household chores, or transferring weight through the affected hand and fingers.
- It's also possible for patients to experience tenderness around the affected region and a feeling of weakness or ‘instability’ such that the finger may easily "pop out" again.
- Bruising can also occur following injury, however, it can take a couple of days to develop.
Physical Examination[edit | edit source]
Examiners must perform a complete history, which incorporates risk factors like Ehlers-Danlos syndrome, mechanism of injury, timing and progression of symptoms, hand dominance, previous finger injuries, occupation, and hobbies. A physical examination is crucial within the assessment of finger injuries. The most common signs of injury are local edema, erythema, pain, deformity, and tenderness to palpation. The assessment should also include finger alignment, ligament integrity, neurovascular status, and Range of motion of the joints. The stability assessment is important for the appropriate management of dislocated joints. A systematic approach to the injured finger assessment avoids missed diagnoses, potential complications, and poor outcomes. Radiographic evaluation with a minimum of three views(i.e. anteroposterior, true lateral, and oblique) is essential if any fracture or dislocation is suspected.
Ample lighting should be used to assess the hand for skin integrity, ecchymosis, edema, or bony deformity. If skin integrity is compromised due to laceration or abrasion, the examiner should evaluate the patient in a bloodless field if possible. Finger ROM examination must be through its complete active and passive range. The examiner can use finger tourniquets or, in patients with sufficient circulation, an anesthetic with epinephrine can be used.[10]
A thorough neurovascular examination of the injured hand is essential. The injured digit should be checked with the same digit of the unaffected hand for light-touch, pinprick, and 2-point discrimination to recognize any potential digital nerve injury. The digital artery can be evaluated by the use of a capillary refill in comparison to an unaffected digit of the opposite hand. If the examiner notices a deformity, he/she should also determine if there is any rotation or angulation. To assess for rotation or angulation, the patient is asked to make a fist if possible, and each fingertip must point toward the scaphoid. Overlapping or “scissoring” shows a rotational component to the injury. Hyperextension of the finger joint should also be checked to assess the competency of the volar plate and the lateral stress of the finger joint is performed to check the collateral ligaments. The Elson test is performed to assess the integrity of the central band/ slip of the extensor tendon complex. Palpation can also be used to determine the site of maximal tenderness.[5]
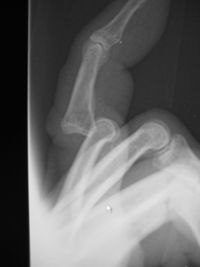
Diagnostic Procedures[edit | edit source]
A thorough subjective and objective evaluation from a physiotherapist is often sufficient to diagnose a dislocated finger. The standard of care for evaluating injuries to the hand is plain film imaging to confirm the dislocation and also to rule out associated fractures of the bones of the finger which may make the reduction of the dislocation difficult or cause complications later in the healing process. For each affected digit, true lateral, anterior-posterior, and oblique views are required. Examiners should keep in mind that rotational deformities are most commonly diagnosed on the physical examination rather than on plain X-rays.[5] In addition to plain radiographs, ultrasound (US) continues to be an area of research regarding the detection of fractures and tendon ruptures.[12]
Differential Diagnosis[edit | edit source]
Fracture-dislocation for example a distal phalanx fracture (tuft fracture)
Collateral ligament injuries- commonly referred to as "finger sprains”
Tendon avulsion, For example, Flexor digitorum profundus avulsion fracture, Mallet fingers, etc.
Medical Management[edit | edit source]
Treatment of MCP, PIP, and DIP joint dislocation can be managed surgically or conservatively depending on the ease of reduction, post-reduction stability, or involvement of the volar plate or other stabilizing structures. Before any reduction, a digital nerve block using lidocaine, bupivacaine, or tetracaine injected at the dorsal base of the injured dislocated finger will provide immediate anesthesia.[13] Most of the dislocations are simple and can be easily manipulated back into the normal position.
Metacarpophalangeal (MCP) Joint Dislocation[edit | edit source]
It can be managed with operative and non-operative options depending on the severity of the injury.
Non-Operative Management[edit | edit source]
This consists of a closed reduction with splinting. The clinician performs closed reduction by extension and applies axial compression on the proximal phalanx with relocating pressure over the phalangeal base to glide it into position. This approach is different from the traction technique used in PIP joint dislocation. Multiple reduction attempts should be avoided because the inability to reduce might indicate volar plate interposition and have the possible complication of displacing the volar plate between articular surfaces, lumbricals, or flexor tendons. The injured finger should be splinted with the wrist extended to 30° and MCP joint in 30° to 60° of slight flexion to prevent terminal extension for 3 to 6 weeks, followed by additional two weeks of buddy taping.[9]
Operative Management[edit | edit source]
This is indicated for non-reducible MCP joint dislocations as there is a high chance of volar plate involvement in these cases. Open reduction of MCP joint dislocation can be done using either a dorsal or volar approach; however, the dorsal approach is more preferable as it lowers the risk of neurovascular injury. After surgery, the wrist is splinted in 30° of extension with slight flexion of the MCP joint for two weeks to prevent terminal extension. The recommendation is that the PIP and DIP joints should not be immobilized. Recovery to a pre-injury range of motion typically occurs between 4 to 6 weeks.[14]
Proximal Interphalangeal Joint Dislocation[edit | edit source]
PIP joint dislocations are also manageable with operative and nonoperative options unlike MCP joint dislocations, but practitioners must determine if the PIP joint dislocation is dorsal, volar, lateral, or rotary as the treatment may differ.
Closed Reduction Of Dorsal PIP Joint Dislocation can be performed by slight extension and longitudinal traction with the other hand applying pressure to the dorsal aspect of the proximal phalanx to relocate the displaced finger. After reduction, the examiner must assess for joint instability in all planes and obtain an x-ray. The normal contour of the dorsal PIP joint on lateral radiographs is “C” shaped. If, after reduction, this contour takes on a “V” shape, it might indicate persistent dorsal subluxation, which results in severe stiffness.[1] PIP joint dislocation is mostly stable after reduction and is treated by dorsal splinting in 30° of flexion.
Volar PIP dislocations are least common, but the reduction of the volar PIP joint dislocation is usually successful. The reduction takes place by applying mild traction with slight flexion at the PIP and MCP joints. After the reduction, the injured digit is splinted for six weeks.
Lateral dislocations often require operative intervention. Closed reduction needs relaxation of the extensor tendon and lateral bands by wrist extension and MCP flexion, respectively then the middle phalanx is gently rotated back into its position. If reduction provides a full range of motion without subluxation, then the joint is not grossly unstable and in these cases, splinting and reassessment in two or three weeks is suggested. All unstable dislocations require orthopaedic referral for evaluation and possible open repair. Indications for surgery include joint instability, significant ligament, soft tissue or tendon injury, or dislocations that are non-reducible.
Splinting remains the mainstay of emergency treatment post-reduction. A research study compared buddy taping vs aluminum orthosis for the treatment of Eaton grades I and II hyperextension type injuries and found no difference in strength, pain, or function at three weeks. However, buddy tape did show an improved range of motion and decreased swelling.[15]
Distal Interphalangeal Joint Dislocation[edit | edit source]
DIP joint dislocation treatment is less complex than PIP joint dislocation. Dorsal DIP joint dislocation is reduced with longitudinal traction, relocating dorsal pressure on the distal phalanx with flexion of the DIP joint. The open reduction occurs easily within the ER setting, followed by splinting of DIP in 10 to 20-degree flexion for 2-3 weeks.[6] If there is persistent DIP joint instability, like those found more commonly in lateral dislocation, then it's often treated with 4-6 weeks of K-wire fixation after concentric reduction. Irreversible dislocation is usually due to volar plate interposition and needs surgical intervention.
Examination and Management of Finger Dislocations[edit | edit source]
| Diagnosis | Examination and initial Treatment | Management | Recommendations for referral |
| PIP dislocation | Identify direction (dorsal, volar, lateral)
Attempt reduction Check for neurovascular status and soft tissue injuries (volar plate in dorsal dislocation, central slip in volar dislocation) Obtain post-reduction radiographs |
Dorsal: Splint and early range of motion
Volar: Splint in extension if there is an associated central slip |
Fractures involving greater than 30 to 40 percent of the intra-articular surface, the reduction is difficult or unsuccessful, the patient is unable to obtain full extension following reduction |
| DIP Dislocation | Attempt reduction
Check for neurovascular status and soft tissue injuries Obtain post-reduction radiographs |
Splint and early range of motion | Complicated injuries |
Physiotherapy Interventions[edit | edit source]
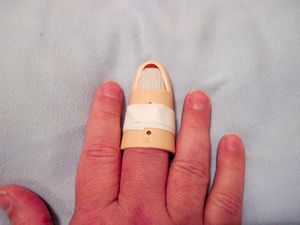
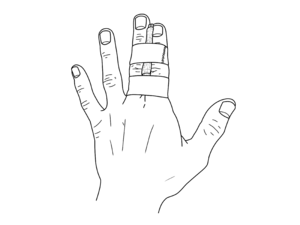
Following relocation, most patients heal well with appropriate physiotherapy management. The success rate of intervention is largely dictated by patient compliance. Treatment usually involves an initial period of immobilization in a buddy splint for a couple of weeks to permit the damaged connective tissue to heal and form ‘scar tissues’. During the initial phase, Ice therapy can be used to alleviate pain and edema, and the injured hand should be elevated to further help reduce swelling. During this period of immobilization, gentle exercises to maintain mobility and strength can be permitted.
Once the splint has been removed physiotherapist can then begin rehabilitation of the affected finger. This will initially involve gentle mobilizations to maintain flexibility and muscle strength which will help in accelerating the healing process Physiotherapy treatment may comprise of:
- Ice therapy and elevation to reduce swelling and pain.
- Finger bracing or splinting.
- Soft tissue release and gentle joint mobilization to reduce pain and stiffness around joints.
- Active-assisted range of motion exercises while finger heals: Gently assist the injured finger to flex and extend with the help of the other hands in an available pain-free range.
- Advice on how to modify everyday activities and prevent re-injury.
- Once the splint is removed Progress to moderate intensity exercises to improve strength in the wrist and hand. This includes the following exercises:
- Finger lift: With palm flat on a table and fingers straight, lift each finger up individually and hold it for few seconds.
- Fist making: Make a fist. Assist with an uninjured hand and try to help it bent into the fist and hold it for 5-10 seconds.
- Object pick-up: Pick up small objects like coins, marbles, pins, or buttons with the injured finger and thumb.
- Passive stretching to lengthen tight muscles.
- Dexterity exercises to improve functional strength and mobility.
- Strengthening of Lumbricals and intrinsic muscles of the hand.
- Eccentric training with a resistance band for wrist and hand to improve stability.
Following this, patients must perform pain-free mobility and strengthening exercises as part of their rehabilitation to ensure an optimal outcome. Particular emphasis needs to be placed on strengthening the finger and hand muscles to improve the stability of the affected joint.
In the final stages of rehabilitation, a gradual return to activity or sports participation is indicated as guided by a physiotherapist provided there is no increase in signs and symptoms. This often includes the use of Protective Taping, particularly upon resumption of ball sports or contact sports.
Return To Play[edit | edit source]
According to a recent review, dislocated fingers usually heal within 4 to 6 weeks.[16] Factors that affect recovery time can include:
- The severity and location of the dislocation.
- Damage to ligaments and tendons.
- Bone fractures.
- Requiring surgery.
Return to your normal activities, including sports, can be possible following injury within a few weeks as symptoms allow with protection (buddy tape, splint) following injury. Protect the injured finger until radiographs show signs of healing also monitor for signs of loss of reduction or malrotation. But it can take up to six months to completely heal. In a few cases, particularly when the dislocation is accompanied by a fracture or medical treatment is not prompt, pain and stiffness can be long-lasting or even permanent.
Prevention Strategies[edit | edit source]
Most patients will recover from a dislocated finger with no permanent effects. However, the fingers may be prone to get dislocated again in the future, so it’s important to practice prevention.
- Always wear proper sporting equipment, and splint fingers to protect it from another injury when playing a sport.
- Perform the hand exercises regularly to promote mobility.
- Remove tripping hazards from your floors to prevent the risk of falls.
- Whenever possible, avoid getting finger's stuck in objects like athletic jerseys, basketball nets, and football helmets, etc.
- Wear protective gloves.
- Remove rings or other jewelry before participating in gaming events.
After a dislocated finger has been treated, prevention of re-injury can be done by focusing on using a protective splint, taping, and continue strengthening of hand and finger muscles[2].
Prognosis[edit | edit source]
The long-term outlook is usually good, although it can take up to 4-6 months for the finger pain to disappear. In a few cases, there is also a small amount of permanent swelling around the injured joint, especially an injured proximal interphalangeal joint and there might be a chance of re-injury in some cases.
- MCP joint dislocations have a high likely hood of requiring operative intervention, and recovery to preinjury ranges takes approximately 4 to 6 weeks.[14]
- PIP joint dislocations are stable after reduction/ relocation except for lateral PIP joint dislocation as they usually require surgical intervention.
- Isolated DIP joint dislocation is rare, and the same as PIP joint dislocation, lateral DIP joint dislocation more often needs surgical intervention.[6]
Complications[edit | edit source]
- Chronic stiffness is often common after DIP dislocation treatment.
- Overtreatment, such as prolonged splinting and multiple attempts of reduction of volar PIP joint dislocations, increases the chances of volar plate scarring and flexion contractures.
- Chronic pain.
- Missed or delayed volar plate injuries are commonly associated with boutonniere deformity, swan neck deformity, laxity, and contractures.
- Swan neck deformity, PIP flexion contracture, mallet finger deformity can also occur if the dislocations of the finger are chronically undiagnosed.[18]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 Sundaram N, Bosley J, Stacy GS. Conventional radiographic evaluation of athletic injuries to the hand. Radiologic Clinics. 2013 Mar 1;51(2):239-55.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 2.8 Prucz RB, Friedrich JB. Finger joint injuries. Clinics in sports medicine. 2015 Jan 1;34(1):99-116.
- ↑ Ramponi D, Cerepani MJ. Finger proximal interphalangeal joint dislocation. Advanced emergency nursing journal. 2015 Oct 1;37(4):252-7.
- ↑ Miller EA, Friedrich JB. Management of Finger Joint Dislocation and Fracture-Dislocations in Athletes. Clinics in Sports Medicine. 2020 Apr 1;39(2):423-42.
- ↑ 5.0 5.1 5.2 5.3 5.4 5.5 Hile D, Hile L. The emergent evaluation and treatment of hand injuries. Emergency Medicine Clinics. 2015 May 1;33(2):397-408.
- ↑ 6.0 6.1 6.2 Johnson BA, Wang QC. Fingertip injuries. American family physician. 2001 May 15;63(10):1961.
- ↑ Dislocations of the finger Available from https://www.youtube.com/watch?v=Os_E4BGUGr8
- ↑ Clesham K, Piggott RP, Sheehan E. High-energy traumatic proximal and distal interphalangeal joint dislocation in the same finger. BMJ Case Reports. 2020 Jun 1;13(6).
- ↑ 9.0 9.1 Nalbantoglu U, Tok O. Isolated Finger Injuries in Basketball. In Basketball Sports Medicine and Science 2020 (pp. 303-311). Springer, Berlin, Heidelberg.
- ↑ Ilicki J. Safety of epinephrine in digital nerve blocks: a literature review. The Journal of Emergency Medicine. 2015 Nov 1;49(5):799-809.
- ↑ Elson's test Available from https://www.youtube.com/watch?v=wyHSKgAZ1eA
- ↑ Tayal VS, Antoniazzi J, Pariyadath M, Norton HJ. Prospective use of ultrasound imaging to detect bony hand injuries in adults. Journal of Ultrasound in Medicine. 2007 Sep;26(9):1143-8.
- ↑ Yin ZG, Zhang JB, Kan SL, Wang P. A comparison of traditional digital blocks and single subcutaneous palmar injection blocks at the base of the finger and a meta-analysis of the digital block trials. Journal of Hand Surgery. 2006 Oct;31(5):547-55.
- ↑ 14.0 14.1 Calfee RP, Sommerkamp TG. Fracture–dislocation about the finger joints. The Journal of hand surgery. 2009 Jul 1;34(6):1140-7.
- ↑ Paschos NK, Abuhemoud K, Gantsos A, Mitsionis GI, Georgoulis AD. Management of proximal interphalangeal joint hyperextension injuries: a randomized controlled trial. The Journal of Hand Surgery. 2014 Mar 1;39(3):449-54.
- ↑ Ashby D, Gutierrez G, Khodaee M. Finger. In Sports-related Fractures, Dislocations, and Trauma 2020 (pp. 291-316). Springer, Cham.
- ↑ Finger Buddy Taping Available from https://www.youtube.com/watch?v=qqCt-yR3LdY&feature=emb_logo
- ↑ Kamnerdnakta S, Huetteman HE, Chung KC. Complications of proximal interphalangeal joint injuries: prevention and treatment. Hand clinics. 2018 May 1;34(2):267-88.