Diplopia
Definition[edit | edit source]
Diplopia means seeing double and is a symptom with both ophthalmological and neurological causes.[1] The images may present themselves side by side, on top of one another, or both. This disorder can impact a person's balance, movement, and ability to read.
Types and presentation[edit | edit source]
Monocular.
If only one eye is impacted by diplopia(one eye sees two images), it is called monocular double vision (diplopia). When the patient covers the unaffected eye, diplopia persists, and when covers the affected eye, diplopia disappears.[1]
Binocular.
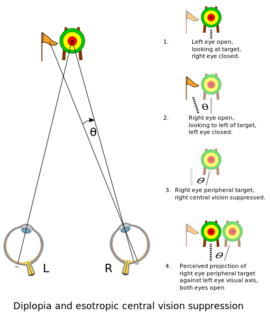
If both eyes are impacted by diplopia, it is called binocular double vision (diplopia). Binocular diplopia occurs when someone with misaligned eyes sees an object, then it falls over the fovea in 1 eye and an extrafoveal location in the other eye. Normally, when someone sees an object, the image falls over the fovea of each eye, and a single image is recognized. The patient has visual blurring that clears up by covering either eye.[2]
Causes[edit | edit source]
Monocular
The causes of monocular diplopia are usually ophthalmological or intraocular pathology with refractive error, including Refractive error, Cataract, Media opacity, Iris injury, Macular disease, Primary or secondary visual cortex disorder (usually bilateral monocular diplopia), and Corneal disease (for example, irregular astigmatism).[1] It also may occur due to eye muscle weakness, behavioral (psychogenic) disorders, dry eye, or Dislocated lenses, to name a few.
The muscles that are affected and cause diplopia are the extraocular muscles of the eye (that move the eyeball and upper eyelid), which are supplied by 3 cranial nerves (oculomotor nerve CN III, trochlear nerve CN IV, and abducens nerve CN VI). The oculomotor nerve CN III innervates the superior rectus as well as the levator palpebrae superioris by its upper-division and innervates the medial rectus, inferior rectus, and inferior oblique muscles by lower division. The trochlear nerve CN IV innervates The superior oblique muscle. And the abducens nerve CN VI innervates lateral rectus muscle.[4]
Binocular
The most common cause of binocular diplopia is the neurologic cause.[5] Neurogenic diplopia occurs with paralysis of 3 cranial nerves (oculomotor nerve CN III, trochlear nerve CN IV, and abducens nerve CN VI)[6], especially abducens nerve (CN VI) are the most common causes of binocular diplopia.[7] It also may occur due to Thyroid dysfunction, Aneurysm, Diabetes, Brain tumors and cancers, Multiple sclerosis, and head injury, to name a few.
Evaluation[edit | edit source]
Diplopia may be the first symptom of life-threatening or serious vision neurologic disease. Its correct diagnosis is essential, with a careful history and clinical examination, to notice the patterns of diplopia that show the location of dysfunction.[8] and differentiate diplopia caused by dysfunction of orbital extraocular muscle versus cranial nerves, or neuromuscular junction.[2] The onset of diplopia is always sudden.[5] Intermittent diplopia with associated ptosis and diurnal variation indicates a neuromuscular junction disorder, such as myasthenia gravis, and progression of diplopia indicates current pathology, such as a compressive lesion.[1]
In monocular diplopia: A complete ophthalmological assessment of the ocular media including cornea, lens, and retina, and a detailed examination of refraction should be done.[1]A pinhole test may resolve Lens disease or refractive error in monocular diplopia.[1]
In Binocular diplopia: We need a clinician to detect the cause of (ocular misalignment).[1]
Physiotherapy assessment[edit | edit source]
Observation[edit | edit source]
- Sit in front of the patient and ask him to look behind you and observe the eyes (redness - swelling - discharge).
- Ask the patient to look up to the ceiling with only his eyes and not to move his head and observe.
Physical tests[edit | edit source]
- Red reflex test:
Using an ophthalmoscope for examination. Put it in front of the patient's eye and ask him to look behind you. Repeat with the other eye.
- Light reflex test.
- Accommodation reflex test:
Put your finger in front of the patient's eye and ask him to look to your ginger and then look behind you. Repeat about 3 times.
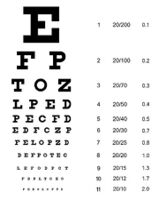
- Visual acuity check:
- Using the Snellen chart.
- Finger counting method:
The patient covers one eye with his hand and the therapist raises his fingers with a certain number and asks the patient about the number. Repeat with the other eye.
- Move your finger in front of the patient from left to right or from right to left and up and down and ask him to follow your finger with his eyes only without moving his head. The patient covers one eye and ask him if sees double anywhere. Then repeat with the other eye.
Saccadic and smooth pursuit function test[8]
- Saccades are quick eye movements (eyes jump from 1 position to another).
- Pursuits are smooth eye movements (eyes follow a target with the same target's speed).
They are important to understand what's happening in the environment around us.
- Saccades are controlled contralaterally by the frontal eye field area 8.
- Pursuits are controlled ipsilaterally by the parietal occipital temporal lobe.
Treatment[edit | edit source]
Treatment may include eye exercises, specially designed glasses, and surgery.
Physiotherapy Management[edit | edit source]
- Treatments may include eye muscle exercise.
- Saccades and Pursuits exercises.[11]
Saccades exercises
- Put a sheet in front of you at the level of your eyes, with a horizontal dots line.
- Make sure that the middle dot is centered in front of you.
- Start with the left or the right end dot.
- Look from one dot to a dot and focus on each dot for one second.
- Continue in the other direction until reaching your beginning dot.
- Repeat this exercise with orient the sheet vertically and then diagonally.
- Repeat 3-5 rounds for each exercise.
- Repeat this exercise 3-4 times/day.
Pursuits exercises
- Exercise has been done horizontally, vertically, and diagonally.
- Horizontally, extend your arms with thumbs up in front of you.
- Move your right thumb slowly to the right side, and follow the movement with your eyes.
- Repeat with your lift thumb.
- Each round should take 15 seconds.
- , Do it vertically and diagonally.
- Repeat the exercise and gradually speed up.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 Danchaivijitr C, Kennard C. Diplopia and eye movement disorders. Journal of Neurology, Neurosurgery & Psychiatry. 2004 Dec 1;75(suppl 4):iv24-31.
- ↑ 2.0 2.1 Rucker JC, Tomsak RL. Binocular diplopia: a practical approach. The neurologist. 2005 Mar 1;11(2):98-110.
- ↑ Informational - Differentiating Between Monocular and Binocular Diplopia. Available from: https://www.youtube.com/watch?v=mad5RjiyNMI [last accessed 24/4/2022]
- ↑ Tsutsumi S, Nakamura M, Tabuchi T, Yasumoto Y, Ito M. An anatomic study of the the the inferior oblique nerve with high-resolution magnetic resonance imaging. Surgical and Radiologic Anatomy. 2013 Jul;35(5):377-83.
- ↑ 5.0 5.1 Glisson CC. Approach to diplopia. CONTINUUM: Lifelong Learning in Neurology. 2019 Oct 1;25(5):1362-75.
- ↑ Sowka J. Neurogenic diplopia: paralysis of cranial nerves III, IV, and VI. Optometry Clinics: the Official Publication of the Prentice Society. 1996 Jan 1;5(3-4):53-76.
- ↑ Merino P, Fuentes D, de Liaño PG, Ordonez MA. Binocular diplopia in a tertiary hospital: aetiology, diagnosis, and treatment. Archivos de la Sociedad Española de Oftalmología (English Edition). 2017 Dec 1;92(12):565-70.
- ↑ 8.0 8.1 Dinkin M. Diagnostic approach to diplopia. continuum: Lifelong Learning in Neurology. 2014 Aug 1;20(4):942-65.
- ↑ Diplopia Examination. Available from: https://www.youtube.com/watch?v=8SKt2QC17Yw&t=217s [last accessed 24/4/2022]
- ↑ Saccades Vs Pursuit. Available from: https://www.youtube.com/watch?v=LxozCFflNqo [last accessed 24/4/2022]
- ↑ 11.0 11.1 Pursuit and Saccade Exercises. Available from: https://www.youtube.com/watch?v=UsQROCcU1f4 [last accessed 24/4/2022]