Digital Health
Introduction[edit | edit source]

Digital health (DH) alludes to information and communication technologies in healthcare. [2] It can be used to assess or manage health disorders or for health promotion. Digital health has a wide reach including devices that can be worn, mobile health, telehealth, health information technology, and telemedicine.[2]
Digital health has gained popularity in the recent post-pandemic years because of its ability to provide healthcare delivery and healthcare systems functions alternatives. [3] For example, through the enablement of patients, E-health solutions have been suggested to address the healthcare providers' workforce estimated reduction by 10% despite the 45% increase in the number of patients with chronic diseases by 2025. [4]
DH is not a new concept. It has been long acknowledged by policymakers as a transformational tool for improving global health outcomes, targeting at promoting universal access, especially in low- to-middle-income countries (LMICs). [5]
The WHO Global Health Strategy for Digital Health [6] acknowledges the crucial role of digital health in healthcare delivery, addressing global health issues, and improving healthcare systems and outcomes. Its action plan emphasises the need to:
- Develop and adopt appropriate, accessible, affordable, scalable and sustainable person-oriented solutions to respond to current healthcare needs
- Develop the infrastructure and applications so that each country can use health data
- Use trained healthcare providers in health informatics (HI) by integrating DH into education and training programmes.
- Promote an appropriate enabling environment for digital health transformation, ensuring equity and trust
- Engage with key stakeholders and leverage regional networks to foster DH development and knowledge-sharing
- Provide evidence-informed investments for the implementation, evaluation and scale up of digital solutions.
Aspects of Digital Health[edit | edit source]
DH refers to healthcare aspects which involve the following: [7]
Health Information Technology (HIT)[edit | edit source]
Health Information Technology (HIT) is an area of information technology dedicated to the design, development, creation, use and maintenance of information systems for healthcare. [8] This may comprise hardware, software, telecommunication, data systems, but also human resources and procedures that involve the input, transmission, use, extraction, and analysis of information in the healthcare sector. [9] At a national level, HIT infrastructures are implemented by policy makers to promote adoption of digital services by health professionals and patients in order to improve healthcare efficiency. For example, electronic medical records (EMRs) and electronic prescribing are used in healthcare instead of paper records and prescriptions to facilitate data sharing and reduce time and costs.
Telehealth / Telemedicine / Telecare[edit | edit source]
Telehealth / telemedicine / telecare involve the delivery of health-related services and information via electronic communication. [10] Although all three terms may be used interchangeably, they have different meanings. Telemedicine uses electronic communication to support the remote delivery of medical and treatment-related services such as diagnostic testing, patient monitoring and specialist consultations. [11] Telehealth includes a wider variety of services delivered remotely by health professionals other than doctors e.g. physiotherapists, psychologists, nurses. [11] Telecare refers to digital solutions that patients use to stay safe and independent in their own homes e.g. health and fitness apps and sensors, exercise tracking tools, digital medication reminder systems or early warning and detection technologies. [11]
Mobile Health (mHealth)[edit | edit source]
Mobile health (mHealth) involves the use of devices and mobile apps in patient care, especially chronic diseases. [12] For example, mobile devices are used for the development and implementation of exercise programmes in musculoskeletal physiotherapy. [13] To promote adherence, applications using web-based input from clinicians enable monitoring of the exercise regime and its quality of completion from the comfort of the patient's home. [13] However, in order for these to be effective, healthcare professionals need to provide ongoing feedback. [13] mHealth technologies are also popular in the cardiopulmonary field. By providing real-time feedback on important physiological measurements and key parameters, mHealth interventions have demonstrated benefit in prevention, monitoring, and management of atrial fibrillation, heart failure, and myocardial infraction. [14]
Wearable devices[edit | edit source]
Wearable technology refers to electronic and other products that can be worn or mated with human skin to enable monitoring of basic human functions or activities. [15] These devices are commonly used for preventive or diagnostic purposes, but their use has also been extended to rehabilitation. Examples of wearables used in rehabilitation include virtual reality (VR) and augmented reality systems, activity trackers and functional electrical stimulation (FES). [16]
Personalised Medicine[edit | edit source]
Personalised medicine refers to targeted treatment based on individual characteristics, patient preferences and social and economic factors. [17] In rehabilitation, personalised neuroprosthetics for patient-specific impairments use brain-to-body interfaces to form electronic bridges that enable neural function.[17]
Taxonomy[edit | edit source]
Taxonomy (classification) for DH interactions may vary depending on different areas of technology and type of care. [18] For clinical practice, Pronovost et al. 's taxonomy [19] dividing DH into the following 3 categories of value seems to be most relevant:
- Digital access: scheduling and access to a health system through online, virtual, or other digital means to gain admission to a health care system or provider.
- Digital healthcare delivery (telehealth): this refers to virtual patient visits, with interaction between healthcare provider and patient
- Digital monitoring: sustaining the digital bond with patients on their care journey without direct interaction with them.
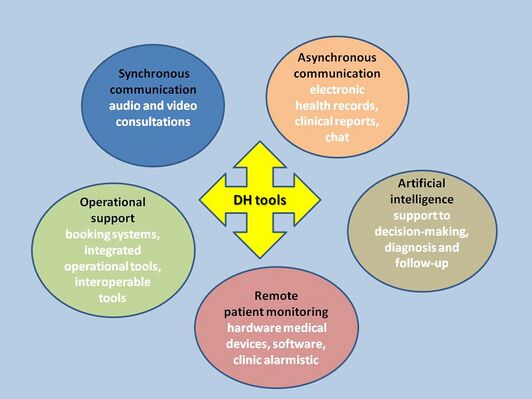
Digital Health Tools[edit | edit source]
DH tools refer to the digital means though which DH is delivered. [3]
- Synchronous digital health technologies use audio, video, and health information interfaces to provide real-time remote interventions [20]
- Asynchronous digital communication involve the exchange of information at a later time e.g. instant messaging (IM), email and electronic/paper-based health records, avoiding disruptions to workflow [21]
- Artificial intelligence (AI) refers to a collection of technologies (machine learning, natural language processing, rule-based expert systems, robotics) that analyse data and find patterns which facilitate decision-making, diagnosis, treatment recommendations and follow-up [22]
- Operational support (e.g. booking systems, integrated operational tools, interoperable tools) keep health systems running, efficient and sustainable [23]
- Remote patient monitoring (RPM) technology allow clinicians to gather and analyse information about their clients without face-to-face interaction [24]
Advantages of Digital Health in Physiotherapy[edit | edit source]
Health professionals see high potential for digitalisation of elements of their practice and are in favour of digital adaptation. [25][26][27]
Some of the advantages of DH in healthcare are:
- Expansion of preventive care: more efficient use of predictive algorithms, improved genomics
- Personalised plans: development of tools that focus more on personal health needs
- Integrated care: better interdisciplinary communication through electronic documentation, connectivity and inter-operability of systems and devices
- Digitalisation and innovation: novel technologies that save human time and resources, opportunities for tailored simulations in education, decentralised research
- Standardisation of practice: through digital tools that objectively measure, monitor and deliver [28]
- Remote management: enabling accessibility and maximisation of efficiency of available resources [29][30]
- Faster development of drugs and devices: using digital twins[31]
Challenges[edit | edit source]
Digital health brings with it some challenges. An example is misinformation, networks being saturated with medical sites presenting advice and treatment options, often these are not reputable sites, potentially leading to patients making poor choices. Another aspect is data safety i.e. if third parties get hold of sensitive information and make use of it illegally. [2]
Moving Towards Digital Health Maturity in Healthcare[edit | edit source]
Digitising healthcare is a complex process. DH has been evolving at different rates across coutries, and the state of DH is variable due to factors such as the wide-ranging nature of healthcare systems (regarding initiatives, infrastructure, implementation). In view of this variation, IQVIA has proposed maturity indicators so that the readiness of Health Systems can be quantitatively assessed. [32]
Below, you can find the most important prerequisites for DH maturity.
Dedicated digital strategy[edit | edit source]
A clear vision and time-bound goals by policy makers is needed.
Designated funding[edit | edit source]
Funding for the purpose of advancing DH is required.
Well-managed data[edit | edit source]
Data protection safeguards along with flexible access management.
National Electronic Health Records[edit | edit source]
Development of a national platform for rich data coverage.
Empowered institutions[edit | edit source]
Allowing room for setting their policy, governance and enforcing standards.
Interoperability[edit | edit source]
Ensuring the ability to store, use and tranfer data across different applications and platforms.
Innovation[edit | edit source]
Commitment in buiding new data sources which expand the scope of health data.
Experimentation[edit | edit source]
Initiation of new projects between public and private sector.
Resources[edit | edit source]
WHO 's page on Digital Health, including the Global Strategy on Digital Health 2020-2025
Digital Health Global: an editorial project aiming at disseminating and promoting the Digital Health culture.
Global Digital Health Index: a tool for assessing maturity in digital health
PhysioFuturist, a blog exploring key technology trends and their impact on physiotherapy.
References[edit | edit source]
- ↑ <a href="https://www.freepik.com/free-photo/female-doctor-with-smart-glasses-touching-virtual-screen-medical-technology_17122969.htm#query=digital%20health&position=3&from_view=keyword">Image by rawpixel.com</a> on Freepik [accessed 4-1-2023]
- ↑ 2.0 2.1 2.2 Ronquillo Y, Meyers A, Korvek SJ. Digital Health. 2023 May 1. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan–.
- ↑ 3.0 3.1 D'Anza B, Pronovost PJ. Digital Health: Unlocking Value in a Post-Pandemic World. Popul Health Manag. 2022 Feb;25(1):11-22.
- ↑ Alpay LL, Henkemans OB, Otten W, Rövekamp TA, Dumay AC. E-health applications and services for patient empowerment: directions for best practices in The Netherlands. Telemed J E Health. 2010 Sep;16(7):787-91.
- ↑ National Academies of Sciences, Engineering, and Medicine, Health and Medicine Division, Board on Global Health, Forum on Public-Private Partnerships for Global Health and Safety. Using Technology to Advance Global Health: Proceedings of a Workshop. Washington (DC): National Academies Press (US); 2017 Nov 17. Available from: https://www.ncbi.nlm.nih.gov/books/NBK538094/ [accessed 6/1/2023]
- ↑ WHO Draft global strategy on digital health 2020- 2025. Available from: https://www.who.int/docs/default-source/documents/gs4dhdaa2a9f352b0445bafbc79ca799dce4d.pdf [accessed 13/4/2023]
- ↑ FDA.What is Digital Health? 2020 Available online: https://www.fda.gov/medical-devices/digital-health-center-excellence/what-digital-health [accessed 4/1/2023]
- ↑ TechTarget Health IT (health information technology). Available online: https://www.techtarget.com/searchhealthit/definition/Health-IT-information-technology [accessed 4-1-2023]
- ↑ Jen M., Kerndt C., Korvek S. Health Information Technology. 2022 Jun 23. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan–.
- ↑ Snoswell C., Chelberg G., De Guzman K., Haydon H., Thomas E., Caffery L., Smith A. The clinical effectiveness of telehealth: A systematic review of meta-analyses from 2010 to 2019. J Telemed Telecare. 2021 Jun 29:1357633X211022907.
- ↑ 11.0 11.1 11.2 Connect2HealthFCC. Telehealth, Telemedicine, and Telecare: What's What? Available online: https://www.fcc.gov/general/telehealth-telemedicine-and-telecare-whats-what [accessed 9/1/2023]
- ↑ Knitza J., Simon D., Lambrecht A., Raab C., Tascilar K., Hagen M., Kleyer A., Bayat S., Derungs A., Amft O., Schett G., Hueber A. Mobile Health Usage, Preferences, Barriers, and eHealth Literacy in Rheumatology: Patient Survey Study. JMIR Mhealth Uhealth. 2020 Aug 12;8(8):e19661.
- ↑ 13.0 13.1 13.2 Agnew J., Hanratty C., McVeigh J., Nugent C., Kerr D. An Investigation Into the Use of mHealth in Musculoskeletal Physiotherapy: Scoping Review. JMIR Rehabil Assist Technol. 2022 Jan-Mar; 9(1): e33609.
- ↑ MacKinnon G., Brittain E. Mobile Health Technologies in Cardiopulmonary Disease. Chest. 2020 Mar; 157(3): 654–664.
- ↑ Haghi M., Thurow K., Stoll R. Wearable devices in medical internet of things: scientific research and commercially available devices. Healthc Inform Res 2017; 23: 4–15.]
- ↑ Rodgers M., Alon G., Pai V., Conroy R. Wearable technologies for active living and rehabilitation: Current research challenges and future opportunities. J Rehabil Assist Technol Eng. 2019 Jan-Dec; 6: 2055668319839607.
- ↑ 17.0 17.1 Sigman M. Introduction: Personalized medicine: what is it and what are the challenges? Fertil Steril. 2018 Jun;109(6):944-945.
- ↑ Classification of Digital Health Interventions. Geneva: World Health Organization, 2018. WHO/RHR/18.06. License: CC BY-NC-SA 3.0 IGO.
- ↑ 19.0 19.1 Pronovost P., Urwin J., Beck E., Coran J., Sundaramoorthy A., Schario M., Muisyo J., Sague J., Shea S., Runnels P. Making a dent in the trillion-dollar problem: toward zero defects. NEJM Catal Innovations Care Delivery 2021;2.
- ↑ Bird M., Li L., Ouellette C., Hopkins K., McGillion M., Carter N. Use of Synchronous Digital Health Technologies for the Care of Children With Special Health Care Needs and Their Families: Scoping Review. JMIR Pediatr Parent. 2019 Jul-Dec; 2(2): e15106.
- ↑ Jhala M., Menon R. Examining the impact of an asynchronous communication platform versus existing communication methods: an observational study. BMJ Innov. 2021 Jan;7(1):68-74.
- ↑ Davenport T., Kalakota R. The potential for artificial intelligence in healthcare. Future Healthc J. 2019 Jun; 6(2): 94–98.
- ↑ Marwaha J., Landman A., Brat G., Dunn T., Gordon W. Deploying digital health tools within large, complex health systems: key considerations for adoption and implementation. NPJ Digit Med. 2022; 5: 13.
- ↑ Vaish A., Ahmed S., Shetty A. Remote physiotherapy monitoring using the novel D+R Therapy iPhone application. J Clin Orthop Trauma. 2017 Jan-Mar; 8(1): 21–24.
- ↑ Estel K., Scherer J., Dahl H., Wolber E., Forsat N., Back D. Potential of digitalization within physiotherapy: a comparative survey. BMC Health Services Research 2022; 22:496.
- ↑ Wallcook S., Morris K. Supporting Digital Health and Digital Inclusion: An Occupational Therapy Perspective. Journal of Corporate Citizenship 2017;(68):82-94.
- ↑ Dahl-popolizio S., Carpenter H., Coronado M., Popolizio N.,Swanson C. Telehealth for the Provision of Occupational Therapy: Reflections on Experiences During the COVID-19 Pandemic. Int J Telerehabil. 2020; 12(2): 77–92.
- ↑ Lamplot J., Pinnamaneni S., Swensen-Buza S., Lawton C., Dines J., Nawabi D., Young W., Rodeo S., Taylor S. The virtual shoulder and knee physical examination. Orthop J Sports Med. 2020;8(10):2325967120962869.
- ↑ Bossen D., Veenhof C., Van Beek K., Spreeuwenberg P., Dekker J., De Bakker D. Effectiveness of a web-based physical activity intervention in patients with knee and/or hip osteoarthritis: randomized controlled trial. J Med Internet Res. 2013;15(11):e257.
- ↑ Grona S., Bath B., Busch A., Rotter T., Trask C., Harrison E. Use of videoconferencing for physical therapy in people with musculoskeletal conditions: a systematic review. J Telemed Telecare. 2018;24(5):341–55.
- ↑ Digital Europe. A digital health decade: driving innovation in Europe. Available online: https://digital-europe-website-v1.s3.fr-par.scw.cloud/uploads/2022/04/DIGITALEUROPE_A-DIGITAL-HEALTH-DECADE_DRIVING-INNOVATION-IN-EUROPE.pdf [accessed 19-12-2022]
- ↑ Arias A, Wright A. White Paper. Switching on the lights. Benchmarking digital health systems across EMEA. Available from: https://www.iqvia.com/-/media/iqvia/pdfs/emea/benchmarking-digital-health-systems-iqvia-emea.pdf [accessed 19/7/2023]