Clavicular Fracture
Original Editor - Sofie Van Cutsem
Top Contributors - Elvira Muhic, Sofie Van Cutsem, Manisha Shrestha, Lucinda hampton, Kim Jackson, Nupur Smit Shah, WikiSysop, Claire Knott, Tony Lowe, Naomi O'Reilly and Karen Wilson
Clinical Anatomy[edit | edit source]
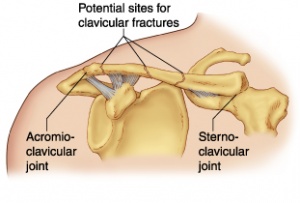
The clavicle is located subcutaneously between the sternum and the scapula, and it connects the arm to the body.[1]
The clavicle is the first bone in the human body to begin intramembranous ossification directly from mesenchyme during the fifth week of fetal life. Similar to all long bones, the clavicle has both a medial and lateral epiphysis but it lacks a well-defined medullary cavity. The growth plates of the medial and lateral clavicular epiphyses do not fuse until the age of 25 years. Peculiar among long bones is the clavicle’s S-shaped double curve, which is convex medially and concave laterally. This contouring allows the clavicle to serve as a strut for the upper extremity, while also protecting and allowing the passage of the axillary vessels and brachial plexus medially.[2]
Clavicle Fracture[edit | edit source]
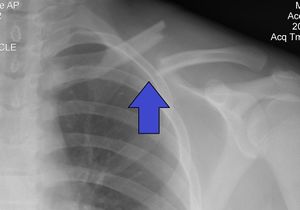
A clavicle fracture is also known as a broken collarbone. Clavicle fractures are very common injuries in adults (2–5%) and children (10–15%) and represent the 44–66% of all shoulder fractures. It is the most common fracture of childhood. A fall onto the lateral shoulder most frequently causes a clavicle fracture. Radiographs confirm the diagnosis and aid in further evaluation and treatment. While most clavicle fractures are treated conservatively, severely displaced or comminuted fractures may require surgical fixation[1].
Etiology[edit | edit source]
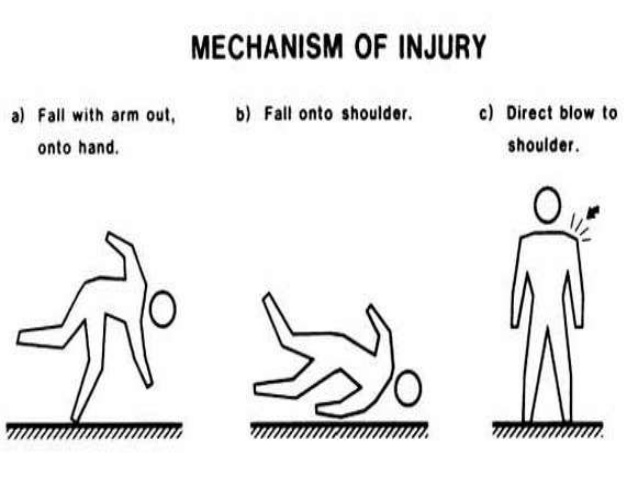
Younger individuals often sustain these injuries by way of moderate to high-energy mechanisms such as motor vehicle accidents or sports injuries, whereas elderly individuals are more likely to sustain injuries because of the sequela of a low-energy fall.
Although a fall onto an outstretched hand was traditionally considered the common mechanism, it has been found that the clavicle most often fails in direct compression from a force applied directly to the shoulder.[2] About 87% of reported cases, a clavicle fracture results from a fall directly onto the lateral shoulder.[1]
Epidemiology[edit | edit source]
Clavicle fractures represent 2% to 10% of all fractures. Clavicle fractures[1]
- Affect 1 in 1000 people per year
- Are the most common fractures during childhood
- Approximately two-thirds of all clavicle fractures occurring in males.
- There is a bimodal distribution of clavicle fractures, with the 2 peaks being men younger than 25 (sports injuries) and patients older than 55 years of age (falls).
- The middle third of the clavicle is fractured in 69% of cases following the distal third in 28% of cases, and the proximal third in 3% of cases.[1]
- Comprise up to 10% of all sport-related fractures and have the third-longest return time to sport with as many as 20% of athletes with such injuries failing to return to sport.[3]
The clavicle is the only osseous link between the upper extremity and the trunk. Due to its superficial subcutaneous location and the numerous ligamentous and muscular forces applied to it, the clavicle is easily fractured. Because the midshaft of the clavicle is the thinnest segment and does not contain ligamentous attachments, it is the most easily fractured location.[1]
Classification[edit | edit source]
Fractures of the clavicle is typically described using the Allman classification system, dividing the clavicle into 3 groups based on location which was later revised by Neer(in which Group II was further classified into 3 types).[1]
Group I: Fractures of the middle third or midshaft fractures (the most common site),
Group II: Fractures of the distal or lateral third. A common site for non-union.
Group III: Fractures of the proximal or medial third.
Robinson’s classification was more specific for different fracture patterns in the middle third, while Craig’s classification was more specific for fractures of the lateral third.[4]
History and Physical Examination[edit | edit source]
The patient may appear with the following signs and symptoms:
- A patient may cradle the injured extremity with the uninjured arm.
- A patient may report a snapping or cracking sound when the injury occurs.
- The shoulder may appear shortened relative to the opposite side and may droop.
- Swelling, ecchymosis, and tenderness may be noted over the clavicle.
- Abrasion over the clavicle may be noted, suggesting that the fracture was from a direct mechanism.
- Crepitus from the fracture ends rubbing against each other may be noted with gentle manipulation.
- Difficulty breathing or diminished breath sounds on the affected side may indicate a pulmonary injury, such as a pneumothorax.
- Palpation of the scapula and ribs may reveal a concomitant injury.
- Tenting and blanching of the skin at the fracture site may indicate an impending open fracture, which most often requires surgical stabilization.
- Nonuse of the arm on the affected side is a neonatal presentation.
- Associated distal nerve dysfunction indicates a brachial plexus injury.
- Decreased pulses may indicate a subclavian artery injury.
- Venous stasis, discoloration, and swelling indicate a subclavian venous injury.[5]
Diagnostic Procedures and Differential Diagnosis[edit | edit source]
A diagnosis can often be made by a client's history and physical examination.[6]
The differential diagnosis of a clavicle fracture includes acromioclavicular joint injury, rib fracture, scapular fracture, shoulder dislocation, rotator cuff injury, and sternoclavicular joint injury.
Possible complications of clavicle fractures must also be fully evaluated, including pneumothorax, brachial plexus injury, and subclavian vessel injury.[1]
Laboratory studies are ordered in clavicle fractures according to the severity of trauma. With a suspected vascular injury, obtain a complete blood count (CBC) to check the hemoglobin and hematocrit values. If a pulmonary injury is suspected or identified, perform an arterial blood gas (ABG) test and obtain an expiration posteroanterior (PA) chest film. Other imaging studies that can be used in the assessment of a clavicle fracture include the following:
- Radiography of the clavicle and shoulder
- Computed tomography (CT) scanning with 3-dimensional (3-D) reconstruction
- Arteriography
- Ultrasonography[5]
Management[edit | edit source]
Clavicle fracture is managed either surgically or conservatively based upon various factors including the location (mid-shaft, distal, proximal), nature (displaced, undisplaced, comminuted) of the fracture, open VS closed injury, age, and neurovascular compromises.[3]
Traditionally, the management of clavicle fractures has been through conservative management with sling immobilization and subsequent rehabilitation. This continues to provide satisfactory results for undisplaced fractures but conservative management of displaced mid-shaft clavicle fractures results in increased rates of re-injury, increased return times to sport and suboptimal shoulder function, secondary to clavicular mal-union and shortening, with resultant thoracoscapular dyskinesia. Similarly, conservative management of displaced lateral fractures in the athletic patient has been shown to result in high rates of non-union and subsequent impairment of shoulder function.
So for the athletic individual, operative intervention is routinely performed for displaced lateral fractures and is recommended for mid-shaft fractures that are completely displaced, shortened >2 cm or comminuted.[3]
Surgical Treatment[edit | edit source]
The chief goal of this treatment is to achieve a healed clavicular strut in a normal anatomical position as possible.
Indications for operative treatment of clavicular fractures are;[7]
- Severe displacement caused by comminution with resultant angulation and tenting of the skin severe enough to threaten its integrity and that fails to respond to closed reduction.
- Symptomatic non-union like shoulder girdle dysfunction neurovascular compromise.
- Neurovascular injury or compromise that is progressive or that fails to revere after the closed reduction of the fracture.
- Open fracture.
- Type II distal clavicular fracture (displaced).
- Multiple traumas, when mobility of the patients is desirable and closed methods of immobilization are impractical or possible.
- Floating shoulder.
- Inability to tolerate closed immobilization such as neurological problems of Parkinsonism, seizure disorders.
- Cosmetic reasons.
- Relative indications include shortening of more than 15 to 20mm and displacement more than the width of the clavicle.
Surgical procedure includes:[8]
- Internal fixation with plates and screws. ( most common)
- Intramedullary (IM) fixation.
The routine removal of metalwork was recommended for IM Nail but not for plate fixation in midshaft displaced fractures. Whereas, in displaced lateral clavicle fracture routine removal of metalwork was performed for ‘hook’ plate fixation, screw fixation, cerclage wire fixation, and tension band wire fixation but not for ‘non-ACJ-spanning’ plate fixation and suture fixation. These fixation methods are necessary for lateral clavicle fracture as it involves acromioclavicular joint and various ligaments that may become injured during fracture.[3]
Physical Therapy/Rehabilitation[3][9][10][11][edit | edit source]
The primary goal of rehabilitation is to improve and restore the function of the shoulder for activities of daily living, vocational, and sports activities. Rehabilitation protocol may vary slightly in first few weeks based upon the primary treatment approach i.e. conservative vs surgical.
Rehabilitation for Conservative Management[edit | edit source]
Fracture healing may take more time in nonoperative treatment. Conservatively treated fractures of the clavicular midshaft usually unite between 18 and 28 weeks after the injury. So regular follow- up needs to be done to check whether the fracture site is properly unioned or not. So rehabilitation protocol may also vary based upon individual co-morbidities.
In first few weeks ( 2-4 weeks), POLICE principle can be used in acute undisplaced clavicle fracture which is further explained below in context of clavicle fracture.
Protection:[edit | edit source]
Patient's shoulder is immobilized in a sling or figure-of-eight brace until the clinical union is achieved. A figure-of-eight brace is often thought to prevent or reduce secondary fracture shortening during the time of fracture healing. But it is associated with more discomfort and pain including nerve compression with temporary brachial plexus palsies and restriction of venous blood return.[9] And studies concluded that there are no differences between these two techniques regarding healing time and the rate of nonunion for treating clavicle fractures. So a sling is usually used and immobilization in internal rotation is usually recommended for 2-4 weeks.[9] [1] Wear the sling during the day, except for exercises and personal hygiene.Patient's choice to wear at night or not but they need to be cautious. [9]
During forceful coughing, sneezing also patients need to take caution (as respiratory excursions may cause clavicle movement) by avoiding it as much as possible and also learning active-assisted coughing techniques if necessary.
Optimal loading[edit | edit source]
It is essential to know the stage of bone healing in order to proceed with optimal loading.
Bone healing during day of injury to one week:
Stability at the site of fracture: None
Stage of Bone healing: Inflammatory phase and there is no callus seen on the radiograph.[12]
Bone healing during the second week :
Stability at the fracture site : minimal amount
Stage of bone healing : early reparative stage and some amount of callus formation is seen in the radiograph.[12]
Therapy/Advice for 1-2 weeks Post injury:
- Use of arm sling as mentioned above ( need to use most of the time).
- Self-mobilisation of the elbow and wrist out of the sling is required several times a day to avoid stiffening of the elbow and wrist.
- Do not lift your elbow above shoulder height as this may be painful.
- The range of motion of the shoulder should usually be limited to pendulum exercises for the first 1-2 weeks.
- Correct postural habits and neck ROM are taught.
Bone healing from 3 to 6 weeks post injury :
- Stability: Callus formation is started and the fracture site becomes stable.
- Stage of bone healing : Reparative stage and fracture line appears less prominent in the radiograph.[12]
Therapy/Advice for 3-6 weeks Post -injury:
- Decrease the use of arm sling (use during non-dependent position).
- Begin normal light daily activities with the arm and shoulder.
- Shoulder active-assisted to active range of motion in a single plane with no more above than 90 degrees is recommended within the first 6 weeks.
- Scapular mobilization exercises are addressed.
- Isometric exercises of the Shoulder with tolerable resistance is started within 4-6 weeks.
- Avoid heavy lifting for the full 6 weeks.
- Gradual progression of cardiovascular endurance training can be started using brisk walking and static bicycle.
Bone healing from 6 to 8 weeks post injury :
Fracture becomes stable by this time
The stage of fracture healing is reparative stage and bridging callus is seen clearly.
After 8 weeks the remodelling phase begins and the fracture line is less distinct.
Therapy/Advice for 6-12 weeks Post-injury:
- Free active and active assisted range of motion of shoulder in all planes is usually allowed after 6 weeks with passive ROM as tolerable.
- Progressive resistive exercises (isotonic) for scapular stabilizers, biceps, triceps and rotator cuff are prescribed after 6 weeks.
- Weight-bearing should be avoided until clinical fracture.
- Sporting activities and work, demanding weight-bearing and the use of the arm, are usually suspended until the patient is free of pain with radiographic signs of progressing fracture consolidation, usually after 6-12 weeks.
Therapy/Advice for 12 weeks and beyond:
Start a more aggressive strengthening program, cardiovascular endurance training as tolerated, and progressive sports-specific training are addressed.
- Return to specific sports is determined by the physical therapist through functional testing specific to the patient’s demands according to which progressive sport-specific training is planned.[13]
- Advance activities including muscle endurance activities (upper body ergometer) and cardiovascular endurance exercises (treadmill, cycling) can be prescribed.
- Contact sports should be avoided for 3-4 months. Return to full contact sports requires the athlete should demonstrate radiographic evidence of bony healing, no tenderness to palpation, a full range of motion, and normal shoulder strength.[9][1]
Rehabilitation After Postoperative Treatment[edit | edit source]
- Primary open reduction and internal fixation with plate ( locking compression plate) and screws of middle third clavicle fractures provides a more rigid fixation and allow immediate post-surgical mobilzation.[7] Surgical management help bone healing faster than that of conservative treatment. So the duration of immobilization is shorter compare to conservative treatment and mobilization and strengthening exercises can be prescribed in earlier than that of conservative management. A similar progression of exercise can be prescribed as of conservative treatment but progression can be made earlier.
This 13-minute video is good viewing
Return to Sports[edit | edit source]
According to the Systematic review done by Robertson and Wood, 2016, most patients with an acute clavicle fracture will return to sports activity, with around four-fifths of all patients able to return to their pre-injury level of sports activity.[3]
The studies have reported that return to sports is between 6 to 12 weeks post-operatively and 3-4 months to those who are managed conservatively.[3][1]
Displaced mid-shaft fractures treated conservatively demonstrated decreased return rates and increased return times to sports than those managed surgically. Displaced mid-shaft fractures treated with conservative management can lead to refracture (over half of the cases) and delayed surgical intervention ( over quarter of the cases). Regarding the preferred surgical technique for mid-shaft fractures, both plate fixation and IM nail demonstrated near complete return rates and similar return times.[3]
In displaced lateral clavicle fracture, surgical management is standardized and has shown increased return rates and decreased return time. Non-ACJ-spanning plate fixation and open suture fixation appear to offer better sporting outcomes than other fixation which is likely due to the preservation of ACJ function. Lateral clavicle fracture is more complicated than mid-shaft clavicle fracture so the outcome of mid-shaft fracture is better than that of lateral clavicle fracture.[3]
Conclusion[edit | edit source]
- Patients with clavicular fractures are best managed by an interprofessional team that includes an orthopedic surgeon, emergency department physician, primary care provider, nurse practitioner, and a physical therapist.
- Immediate orthopedic consultation should be obtained for patients with neurovascular compromise, open fractures, tenting of the skin, or any break in the skin near the fracture.
- Non-surgical management forms the first-line treatment for undisplaced fracture.
- Whereas in the athlete, surgical management is the routine treatment for displaced lateral fractures and the recommended treatment for displaced mid-shaft fractures, offering improved return rates and return times over conservative management.[3]
- The healing of the fracture may take 8-12 weeks and most patients have a good outcome. However, a few patients may have chronic pain and limited range of motion of the shoulder.[1]
- An early mobilization rehab protocol can be safely recommended for both acute and non-union post-operative cases.[11]
Resources[edit | edit source]
- CLAVICLE FRACTURE REHABILITATION PROTOCOL: Jordon Young Institute
- Broken collarbone rehab protocol-CLAVICLE FRACTURE STABILIZATION Post –Operative Rehabilitation
Related pages[edit | edit source]
References[edit | edit source]
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 Bentley TP, Journey JD. Clavicle Fractures. InStatPearls [Internet] 2020 May 6. StatPearls Publishing. Available from: https://www.ncbi.nlm.nih.gov/books/NBK507892/ (last accessed 22.12.2019)
- ↑ 2.0 2.1 Paladini, P et al. “Treatment of Clavicle Fractures.” Translational Medicine @ UniSa 2 (2012)
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 3.7 3.8 3.9 Robertson GA, Wood AM. Return to sport following clavicle fractures: a systematic review. British medical bulletin. 2016 Sep 1;119(1).
- ↑ O’Neill BJ, Hirpara KM, O’Briain D, McGarr C, Kaar TK. Clavicle fractures: a comparison of five classification systems and their relationship to treatment outcomes. International orthopaedics. 2011 Jun 1;35(6):909-14.
- ↑ 5.0 5.1 Medscape. Kleinhenz BP, Young CC, Clavicle Fractures. www.emedicine.medscape.com/article/92429-overview#showall
- ↑ M. Pecci, J. Kreher, MD, Boston university, Clavicle fractures, jan. 2008. Level of evidence: 1 Grade of recommendation: B
- ↑ 7.0 7.1 Reddy YT, Reddy SS, Reddy V, Vadlamani KV, Suresh M. Operative treatment of clavicular fractures: a prospective study. JOURNAL OF EVOLUTION OF MEDICAL AND DENTAL SCIENCES-JEMDS. 2015 Sep 24;4(77):13394-410.
- ↑ Fanter NJ, Kenny RM, Baker III CL, Baker Jr CL. Surgical treatment of clavicle fractures in the adolescent athlete. Sports health. 2015 Mar;7(2):137-41.
- ↑ 9.0 9.1 9.2 9.3 9.4 Waldmann S, Benninger E, Meier C. Nonoperative Treatment of Midshaft Clavicle Fractures in Adults. The open orthopaedics journal. 2018;12:1.
- ↑ Rabe SB, Oliver GD. Clavicular fracture in a collegiate football player: a case report of rapid return to play. Journal of athletic training. 2011 Jan;46(1):107-11.
- ↑ 11.0 11.1 Lädermann A, Abrassart S, Denard PJ, Tirefort J, Nowak A, Schwitzguebel AJ. Functional recovery following early mobilization after middle third clavicle osteosynthesis for acute fractures or nonunion: a case-control study. Orthopaedics & Traumatology: Surgery & Research. 2017 Oct 1;103(6):885-9.
- ↑ 12.0 12.1 12.2 Hoppenfeld. Treatment and rehabilitation of fractures.Philadelphia.Lippincott Williams & Wilkins.2019.
- ↑ Stone clinic Broken collar bone Available from: https://www.stoneclinic.com/broken-collarbone-rehab-protocol (last accessed 22.12.2019)
- ↑ Bob and Brad Clavicle fracture Available from: https://www.youtube.com/watch?v=8uUT2Ozin5o&feature=youtu.be (last accessed 22.12.2019)