Celiac Disease (Coeliac Disease)
Original Editors - Brandon Fowler from Bellarmine University's Pathophysiology of Complex Patient Problems project.
Top Contributors - Brandon Fowler, Zeina Grifoni, Admin, Kim Jackson, Laura Ritchie, Lucinda hampton, Dave Pariser, Vidya Acharya, 127.0.0.1, Elaine Lonnemann, Wendy Walker, WikiSysop and Rishika Babburu
Introduction[edit | edit source]
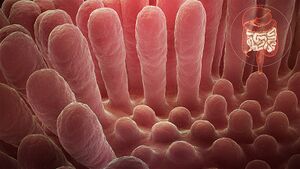
Celiac disease, or alternativly gluten-sensitive enteropathy, is an autoimmune disease of the small intestine. In this condition the bodies immune system responds inappropriately to gluten causing small intestinal inflammation and damage. This results in impairment of the mucosal surface of the small intestine and, consequently, poor absorption of nutrients.[1] [2]Celiac disease is set-off when a genetically susceptible person is exposured to gluten in their food. It is a chronic condition with treatment being permanent exclusion of gluten from the diet.
Epidemiolgy[edit | edit source]
Coeliac disease in the White population is fairly common, 1 in 200, however it is extremely rare in the Asian and Black population.[3] The incidence among people with autoimmune disorders for example type 1 diabetes is higher. The risk is much greater also in people with a first-degree relatives of people affected by celiac disease ( risk 1 in 10).[4] Environmental factors may increase the risk and prevalence of the disease such as increased gluten exposure at a young age, increased presence of gluten in processed foods, and exposure to antibiotics or other factors that have the potential to change the overall gut biome.[5]
Characteristics/Clinical Presentation[edit | edit source]
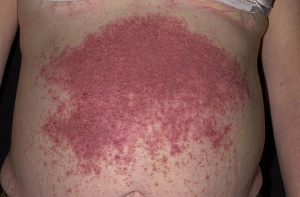
Primary symptoms often include abdominal bloating (with significant distention often noted in children), diarrhea, chronic diarrhea, abdominal cramping, bloating, indigestion, weight loss, gastric ulceration, and reduced fertility for both men and women.[2][6] Secondary symptoms, due to malnutrition, include fatigue, depression, nausea, muscle atrophy, changes in bone mineral density, and joint pain. If the problem persists long enough without treatment, excessive nocturnal reabsorption of intestinal fluids can occur, causing nocturia (excessive night time urination). In addition to nocturia, if the condition is severe enough, a gluten-related skin disorder may also be present (dermatitis herpetiformis)[7]. Celiac Disease is commonly found in adjunct with Diabetes, Down Syndrome, Turner Syndrome, William Syndrome, Sjogren Syndrome, autoimmune thyroid disorder, autoimmune hepatitis, congenital heart defects, and Addison Disease.[2][8]
Associated Co-morbidities[edit | edit source]
Co-morbidities for Celiac Disease include dermatitis herpetiformis, diabetes mellitus, pernicious anemia, dehydration, hypotension, lymphoma, bowel cancer, microscopic colitis, systemic lupus erythematosus, scleroderma, autoimmune hepatitis, primary biliary cirrhosis, and osteopenia/osteoporosis.[2][7]
Medications[edit | edit source]
There is currently no treatment for Celiac Disease except the avoidance of gluten in the diet. This proves to be increasingly difficult as gluten is found in many commercially produced foods and there is high risk of cross contamination in production and packaging facilities, restaurants, and homes. In addition, substitution of foods not containing gluten for familiar gluten containing foods, such as gluten free breads, crackers, pastries, lack the vitamins and minerals that are naturally found in their gluten containing counterparts, predisposing those with Celiac disease for nutritional deficiency.[9] Over-the-counter supplements may be prescribed in order to meet personal daily nutritional needs. Hematinics may also be prescribed to stimulate red blood cell volume and to increase hemoglobin availability in order to address blood volume deficiencies. If primary means of treatment prove to be ineffective, corticosteroids can be utilized in order to reduce the inflammatory processes present in the small intestine. [2]
Diagnosis[edit | edit source]
The gluten free diet is a huge undertaking involving lifestyle changes and having to read and interpret food labels. Therefor a diagnosis of coeliac disease must be properly medically established. The tests for coeliac disease are listed below.
- Gluten challenge: The ‘gluten challenge’ involves consuming a minimum of four slices of wheat based bread (or equivalent) each day (for adults) (two slices of wheat based bread each day for children). A doctor guides the client during the challenge period.
- Blood tests (coeliac serology) are used to screen for coeliac disease. Measures antibody levels in the blood, elevated in people with untreated coeliac disease, as a consequence of the body’s reaction to gluten. A positive blood test must be followed by a small bowel biopsy for confirmation of the diagnosis. Other blood tests are also used eg complete blood count (CBC), Vitamin B12 testing, complete metabolic profile (BMP) .
- Biopsy (several tiny biopsies of the small bowel are obtained). Examined under a microscope, looking for the presence of villous atrophy.[10]
- Other tests include: Barium Xray test to detect the presence of malabsorption along the gastrointestinal tract; Direct stool sample analysis of fat content can also be implemented to detect the presence of steatorrhea (abnormally high-fat content contained within expelled fecal matter). Fecal fat greater than 7 grams per day is considered abnormal.[2][11]
Causes/Mechanism[edit | edit source]
Although there is no direct known cause for Celiac disease and no consistent trigger for the immune response in affected individuals, researchers believe changes in genes, primarily but not limited to the HLA-DQ2 and DQ8, predispose a person to Celiac Disease.[6] In people with the genetic propensity for a gluten reaction, estimated to be between 10 and 15% in those with a first degree relative with Celiac Disease, [12]the ingestion of foods containing gluten stimulates gluten sensitive T-cells in the small intestine. The T-cells trigger an inflammatory process in the small intestine which changes the histological makeup of the cells that line the lumen of the small intestine and it causes the villi (hair like projections within the lumen of the small intestine involved in nutrient absorption) to atrophy and eventually to be destroyed.[7]
Systemic Involvement[edit | edit source]
The small intestine is the primary organ targeted for systemic involvement of Celiac Disease. Abdominal distention, abdominal cramping, nausea, and indigestion are all direct results of systemic involvement of Celiac Disease affecting the small intestine.[7] Malabsorption of ingested nutrients and changes in dietary habits however, can manifest dysfunction throughout the entire systemic system.[7] Changes in bowel and bladder habits are commonly associated with the presence of Celiac Disease. Explosive acute diarrhea, chronic diarrhea, steatorrhea (increased fraction of fecal fat), and nocturia (increased urination at night) are among the symptoms that can occur pertaining to changes in bowel and bladder function related to Celiac Disease.[7] Changes in blood volume can result from malabsorption problems of the small intestine. Hypotension and anemia can often manifest from pathologic changes of blood volume related to malabsorption problems.[7] Fatigue (both central command and peripheral) and an inability to focus conscious attention can result from the brain and entire body not receiving daily nutritional requirements from blocked absorption at the small intestine. In some cases of Celiac Disease, hypertension has also been reported[13].The issues related to blood volume can vary from person to person, depending on family history, dietary habits, and lifestyle choices of the indvidual. An associated reaction of the epidermis may also be involved. A skin rash known as Dermatitis Herpetiformis can form commonly at the buttocks, knees, or elbows as a direct consequence of Celiac Disease.[7] Other systemic conditions such as polyneuropathy, dilatative cardiomyopathy, psoriasis, and vasculitis may also result from malabsorption.[7]
Management[edit | edit source]
The primary treatment for Celiac Disease is maintaining a life long regimen of a gluten free diet.[2]and should be managed by a registered dietitian nutritionist and physician with expertise in the management of Celiac Disease.[8] [12]Nutritional supplements are also commonly used in adjunct to maintaining a gluten free diet.[2][8] This is done in order to make up for nutritional deficiencies that are often present when following a gluten free dietary regimen. The nutritional insufficiencies may vary depending on the dietary habits of the individual. Corticosteroid treatments may also be utilized if the traditional means of treating Celiac Disease are unsuccessful.[2]
Physical Therapy Management[edit | edit source]
Although Celiac Disease is derived solely from pathology involving the enteric system, physical therapy can be beneficial in order to minimize and treat secondary conditions that may accompany Celiac Disease.
Such conditions include:
- Joint pain
- Edema
- Muscle atrophy and weakness
- Osteoporosis/osteopenia.[14]
- Peripheral axonal neuropathy
- Energy management
- Overall physical fitness and weight management
- Patient education and resources for dietary recommendations, lifestyle choices, appropriate rest intervals, and community resources
Differential Diagnosis[edit | edit source]
- Bacterial gastroenteritis
- Crohn disease
- Giardia
- Irritable Bowel syndrome
- Malabsorption
- Viral gastroenteritis[4]
Case Reports[edit | edit source]
- Celiac Disease Symptoms in a Female Collegiate Tennis Player: A Case Report[13][13][13][13][12][12][9][9][9][9][9][9]
Resources[edit | edit source]
1. Link to comprehensive list of foods containing gluten [24][24][24][24][23][19][19][17][16][16][15][15][15][15][15][15][15][15][14][14][14][14][14][14][14][13][13]
2.Celiac Sprue Association Sponsored Gluten-free recipes and tips for cooking gluten free: http://www.csaceliacs.org/recipes.php[25][25][25][25][24][20][20][18][17][17][16][16][16][16][16][16][16][16][15][15][15][15][15][15][15][14][14]
3.Link to Nationwide contacts for Celiac Disease support groups by state[16][16][16][16][15][15]
5. Gluten Sensitivity: a disease of the brain: Professor Marios Hadjivassiliou 2021, Sheffield Gastroentereology. A lecture on the effects of gluten exposure on the brain.
References[edit | edit source]
- ↑ Parzanese I, Qehajaj D, Patrinicola F, Aralica M, Chiriva-Internati M, Stifter S, Elli L, Grizzi F. Celiac disease: From pathophysiology to treatment. World journal of gastrointestinal pathophysiology. 2017 May 15;8(2):27.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 2.8 Ruiz,Atenodoro R. Jr. Celiac Sprue.Merck Manual for Healthcare Professionals. http://www.merck.com/mmpe/sec02/ch017/ch017d.html?qt=celiac%20disease&alt=sh. (Accessed 1 March 2010).
- ↑ Radiopedia Celiac Disease Available:https://radiopaedia.org/articles/coeliac-disease-1 (28.1.2023)
- ↑ 4.0 4.1 Posner EB, Haseeb M. Celiac disease.Available: https://www.ncbi.nlm.nih.gov/books/NBK441900/(accessed 28.1.2023)
- ↑ Makharia, GK, Chauhan, A, Singh, P, Ahuja, V. Epidemiology of coeliac disease. Aliment Pharmacol Ther. 2022; 56(Suppl. 1): 3- 17.
- ↑ 6.0 6.1 Mayo Clinic. Celiac Disease. http://www.mayoclinic.com/health/celiac-disease/DS00319 (Accessed 1 March 2010).
- ↑ 7.0 7.1 7.2 7.3 7.4 7.5 7.6 7.7 7.8 Goodman Catherine C., Fuller Kenda S. Pathology: Implications for the Physical Therapist. 3rd ed. St. Louis: Saunders Elsevier, 2009. p848-851.
- ↑ 8.0 8.1 8.2 Fasano Alessio,Catassi Carlo. Current Approaches to Diagnosis and Treatment of Celiac Disease: An Evolving Spectrum. Gastroenterology 2001;120:636–651. http://medschool.umaryland.edu/celiac/documents/celiacgastro.pdf (Accessed 1 March 2010).
- ↑ Makharia GK. Current and emerging therapy for celiac disease. Front Med (Lausanne). 2014 Mar 24;1:6. doi: 10.3389/fmed.2014.00006. PMID: 25705619; PMCID: PMC4335393.
- ↑ Coeliac Disease Diagnosis Available:https://www.coeliac.org.au/s/coeliac-disease/diagnosis (accessed 28.1.2023)
- ↑ Johnson, Larry E. Vitamin B12. Merck Manual for Healthcare Professionals. http://www.merck.com/mmpe/sec01/ch004/ch004i.html#sec01-ch004-ch004j-395 (Accessed 2 March 2010).
- ↑ 12.0 12.1 Rubin JE, Crowe SE. Celiac Disease. Ann Intern Med. 2020 Jan 7;172(1):ITC1-ITC16. doi: 10.7326/AITC202001070. PMID: 31905394; PMCID: PMC7707153.
- ↑ Zamani Farhad, Et al. Celiac disease as a potential cause of idopathic portal hypertension: a case report. Journal of Medical Case Reports 2009; 3:68. http://jmedicalcasereports.com/content/3/1/68 (Accessed 3 March 2010)
- ↑ Fuchs, V., Kurppa, K., Huhtala, H., Collin, P., Mäki, M., & Kaukinen, K. (2014). Factors associated with long diagnostic delay in celiac disease. Scandinavian Journal of Gastroenterology, 1–7.
- ↑ Silvester JA, Therrien A, Kelly CP. Celiac Disease: Fallacies and Facts. Am J Gastroenterol. 2021 Jun 1;116(6):1148-1155. doi: 10.14309/ajg.0000000000001218. PMID: 33767109; PMCID: PMC8462980.