Case Study: Traumatic Brain Injury in an Elderly Woman
Top Contributors - Emily Villeneuve, Emily Hogan, Tianzi Zhao, Kim Jackson, Shaimaa Eldib, Lucinda hampton and Aminat Abolade
Abstract[edit | edit source]
The following fictional case study discusses possible interventions for restoring physical and cognitive function during an in-patient rehabilitation program of a 65-year old woman who presented with a traumatic brain injury (TBI). She underwent surgical procedure to correct a subdural haematoma in the frontal lobe, resulting from a TBI. She entered the in-patient rehabilitation program two weeks after a craniotomy, with stable vitals. The initial examination findings included impaired memory, balance issues, limited ambulation and increased tone in the left upper and lower extremities as well as right upper extremities. Physiotherapy interventions consisted of balance training, task-specific exercises, strength training, flexibility exercises, gait training and postural education. Outcome measures were then used to reassess the patient's progress at week 4 of in-patient rehabilitation, including: the Berg balance scale, Ranchos Los Amigos scale, Modified Ashworth Scale, gait speed and distance measurements. The Functional Independence Measure (FIM) score improved from 68 upon rehabilitation to 106 when she was discharged to a home-rehabilitation program.
Introduction[edit | edit source]
Traumatic brain injury(TBI)s a major health condition[1], and one of the common causes is falls[2] [3]. More specifically, subdural haematomas have been identified as one of the most prevalent injuries in patients who presented to the emergency department due to a TBI[3]. Few studies have looked at the role of rehabilitation and its effects on the improvement of functional outcomes in patients who have undergone surgery for subdural haematomas[4]. The purpose of this fictional case study is to explore the rehabilitation of an elderly woman with an acute TBI, post-surgical intervention.
Client Characteristics[edit | edit source]
A 65-year-old woman was getting groceries with her friend when she slipped on ice, hit her head and lost consciousness. An ambulance was called, and she was rushed to the hospital. The patient lost consciousness for one hour and remained in an altered state of consciousness for 24 hours. Diagnostic imaging confirmed right-sided focal subdural haematoma. Her Glasgow Coma Score (GCS) score upon arrival was 9 (E5; M2; V2) and she presented as a level III on the Ranchos Los Amigos Scale. The severity of her TBI was classified as ‘moderate’.
The patient underwent a craniotomy the following afternoon. After 2 weeks in the ICU, the patient’s Functional Independent Measure (FIM) score improved from 57 to 68 and was deemed appropriate for the in-patient rehabilitation unit. The patient presented with 7 days of retrograde amnesia, and no signs of anterograde amnesia. Her pre-existing conditions included hypertension and osteoporosis, and the medications she was taking for these conditions included Perindopril (Coversyl) and Alendronate (Fosamax), respectively. She had limited range of motion and required assistance with ambulation. Due to her FIM score, hospital protocol dictated that she was to enter an in-patient rehabilitation which includes daily physiotherapy.
Examination Findings[edit | edit source]
2 Weeks Post-Op: In-Patient Rehabilitation Program[edit | edit source]
Subjective[edit | edit source]
During the examination, information was collected from the patient’s chart, from members within the multidisciplinary team, the patient and her husband. As mentioned, diagnostic imaging confirmed right-sided focal subdural haematoma, affecting the frontal lobe. When speaking with the patient, she had complaints of dizziness and a headache earlier that morning. Prior to her fall, she was living with her husband in a bungalow and was independent in all activities of daily living. She is a retired teacher, and her husband is a healthy 68-year-old retired farmer. Her husband reported that she was active and independent and did not use any walking aids prior to her fall. She enjoyed activities such as pickleball, camping, hiking, baking and playing with her grandchildren. Her husband also stated that they had 4 steps to get into their house, with a railing on the right side. Her main goal was to return home and resume her regular activities. Upon gathering a subjective interview, her husband also explained that he was very concerned about his wife and that he was having difficulties coping with her changes in behaviour.
Objective[edit | edit source]
After the patient was admitted to in-patient rehabilitation, the patient’s screening results showed stable vital signs with a heart rate of 76bmp, blood pressure of 115/76, SpO2 of 97% and intact integuments. The physiotherapist proceeded to choose various outcome measures to obtain the patient’s mental status at baseline and monitor any changes over time.
The Galvestron Orientation and Amnesia Test (GOAT) was used to evaluate the patient’s orientation and ability to recall events before and after the incident [5]. Her GOAT score was 60/100, which was below the cut-off of 66, suggesting impaired memory[5]. Specifically, the patient had in-depth current memory and remembered most events after she gained consciousness in the ICU; however, she showed signs of retrograde amnesia from events that happened within 7 days prior to the incident[5].
The Ranchos Los Amigos scale is a useful tool to rate the patient’s cognitive level after the patient regains consciousness from a TBI[6]. During initial assessment, she presented with level VI (Confused-appropriate) on the Ranchos Los Amigos scale[6]. As such, the patient was ready for rehabilitation since she was able to consistently follow simple directions (i.e., one step commands), showed carry over for relearned familiar tasks (e.g., self-care), and could attend to highly familiar tasks for a certain period of time[6]. However, the physiotherapist kept in mind that the patient required maximal assistance in learning new tasks due to the lack of carryover from previous sessions[6]. Additionally, the physiotherapist ensured to take proper safety measures (i.e., maximal supervision) since the patient was unaware of her impairments and was inconsistently oriented to person, time, and space[6].
The Moss Attention Rating Scale (MARS) measures the effects of impaired attention on cognitive and motor performance specific to patients with TBI in acute rehabilitation[7]. Considering that patients at Rachos level VI mostly benefit from learning tasks in a non-distracting environment, the physiotherapist used MARS, an observational rating scale, to assess the patient’s daily attentional state and used the results to provide appropriate cueing to help the patient focus[7].
Total Raw Score: 62/110
- Average MARS Item Score: 2.82
- Factor 1 (Restlessness/ Distractibility) Score: 3.80
- Factor 2 (Initiation) Score: 2.67
- Factor 3 (Sustained/ Consistent Attention) Score: 2.33

The Agitated Behavior Scale (ABS) was chosen to objectively measure the extent of agitation including levels of: disinhibition, aggression and liability, and is specific to the acute phase of acquired brain injury[9]. The patient scored 20/56 upon initial assessment, which is considered borderline normal[9]. Although patients at Ranchos level VI tend to have decreased agitated behaviour, the ABS was administered to monitor the extent of decrease over time[9].
The Neurobehavioral Functioning Inventory Depression Scale (NFI) is used to measure post-injury depressive symptoms such as frustration, restlessness, loneliness, etc [10]. Research shows that the NFI Depression Scale is highly reliable and valid, and is sufficient at identifying minimal, borderline and clinical depression in patients with a TBI[10]. The patient scored 26/65 on the NFI Depression Scale. This score classified her as 'minimally depressed', which means that the patient rarely experiences depressive symptoms, therefore immediate intervention was not required, however signs of depressive symptoms were monitored throughout treatment[10].
- Sensory integrity
- Proprioception, light touch, and sharp/dull discrimination were intact on the right and left extremities.
- Assistive and adaptive device
- Patient was using a standard wheelchair when she arrived to in-patient rehabilitation.
- Gait, locomotion and balance:
- Ambulation: Able to ambulate with a four wheeled walker with heavy assistance of one person for 50m using a 3 point step-to gait pattern.
- Decreased gait speed: measured as 0.50m/s
- Observational gait assessment with four wheeled walker:
- ataxia
- difficulty clearing left foot at initial swing due to decreased dorsiflexion
- left hip hike to clear left foot from ground during swing phase
- circumduction of left leg
- hyperextension of right knee during terminal stance
- Sitting balance: able to sit on the edge of the bed and in wheelchair – required supervision
- Berg balance scale: 40/56 – increased risk of fall [11]
- Motor function:Muscle tone graded on the Modified Ashworth Scale (MAS)[12]
- Left Lower Extremity
- Increased tone in the following muscle groups:
- left hip and knee extensors and ankle dorsiflexors
- Grade 2 on the MAS
- Increased tone in the following muscle groups:
- Right Lower Extremity
- No increase in muscle tone was detected
- Grade 0 on MAS
- Left Upper Extremity
- Increased tone in the following muscle groups:
- Left elbow, wrist and finger flexors
- Grade 2 on MAS.
- Increased tone in the following muscle groups:
- Right Upper Extremity
- Slight increase in tone in the follow muscle groups:
- Right shoulder, elbow, wrist and finger flexors
- Grade 1 on MAS
- Slight increase in tone in the follow muscle groups:
- Patient was unable to isolate movement in the left upper and lower extremities but was able to isolate movement in the right upper and lower extremities.
- Patient presented with active (AROM) dorsiflexion, knee flexion as well as finger, elbow and wrist extension on both right and left sides.
- Left Lower Extremity
- Range of Motion {| class="wikitable" | colspan="3" |Goniometry: Range of Motion Measurement (in Degrees) |- | |Left |Right |- |Shoulder flexion |176 |179 |- |Elbow flexion |140 |145 |- |Wrist flexion |80 |80 |- |Finger flexion |MCP: 90 PIP: 100 DIP: 90 |MCP: 90 PIP: 100 DIP:90 |- |Shoulder extension |45 |55 |- |Elbow extension |+10 degrees of flexion contracture |+5 degrees of flexion contracture |- |Wrist extension |50 |65 |- |Finger extension |MCP: 35 PIP: + 5 degrees of flexion contracture DIP: + 5 degrees of flexion contracture |MCP: 40 PIP: +5 degrees of flexion contracture DIP: +5 degrees of flexion contracture |- |Hip Flexion |100 |120 |- |Knee flexion |120 |135 |- |Hip Extension |20 |20 |- |Knee Extension |0 |0 |- |Dorsiflexion |5 degrees of plantar flexion contracture |20 |- |Plantarflexion |45 |45 |}
- Muscle Strength (MMT)
- Left side: Grade 3 across both lower and upper extremities
- Right side: Grade 5 across whole lower extremity, Grade 4 across whole upper extremity
- Reflex Integrity
- Intact UMN and LMN reflexes
- Total FIM score= 68, suggesting minimal assistance to accomplish tasks [13]
Clinical Impression[edit | edit source]
Physiotherapy Diagnosis[edit | edit source]
Patient presented with a moderate TBI with imaging confirming an acute subdural haematoma affecting the frontal lobe of the brain. The patient demonstrated signs of increased tone, limited ROM, general weakness, and cognitive and behavioural deficits, such as, memory problems and mild agitation. Activities, such as walking, sitting, ascending/descending stairs, and moving limbs in isolation were affected. The patient was unable to resume regular activities such as pickleball, camping, hiking, baking, and playing with her grandchildren. However, she hoped to restore as much function as possible during rehabilitation so she could go back to doing things she enjoys. Patient was determined to be a good candidate for physiotherapy to help regain balance control, improve joint range of motion, reduce spasticity and overall restore physical function.
Problem List[edit | edit source]
- Reduced Level of Cognition
- Ranchos Los Amigos Level VI (confused–appropriate) - difficulties retaining new information, memory problems, unaware of safety concerns
- ABS scale = 29/56 - mild agitation
- FIM score = 68
- Signs of Post-Injury Depression
- NFI score = 26/65 - minimal depression
- Impaired Gait and Balance
- Left side hip hike & decreased dorsiflexion during swing phase
- Supervision to sit in wheelchair and on edge of bed
- Berg balance scale = 40/56 - increased risk of falls[11]
- Reduced ROM
- Contractures in the left side elbow, wrist, and finger flexors, as well as ankle plantarflexors
- Contractures in the right side elbow and finger flexors
- Reduced wrist extension and flexion
- Environmental impacts
- Four steps to get into house
- Social Impacts
- Unable to resume regular activities – e.g. playing with grandchildren, hiking, camping, pickle ball
- Husband is concerned for her health and is having difficulties coping with his wife's changes in behaviour
Intervention[edit | edit source]
The patient was at Ranchos level VI (confused-appropriate), and was not cognitively aware of her condition, therefore the focus of her in-patient rehabilitation was to create a program based on not only the patient's goals, but also the facility's protocol on TBI rehabilitation. The treatment included restoring function and progressing the patient to a point where she was safe to return home with her husband. The treatment followed evidence-based clinical practice guidelines for TBI, specifically Understanding Traumatic Brain Injury by Ontario Neurotrauma Foundation and Rehabilitation Following Acquired Brain Injury by the British Society of Rehabilitation Medicine (BSRM). Thus, in-patient rehabilitation involved components of task-specific training, balance re-training, gait re-education, strength training and aerobic fitness training, all in the context of functional tasks where possible[14].
To maximize outcomes of treatment, the in-patient rehabilitation program was adapted to use appropriate learning strategies based on the patient’s cognitive abilities. Treatment began by having a structured routine[15], using distributed practice, explicit feedback[16], closed environments, and clear and concise instructions. As the patient improved in cognitive and physical function, treatment progressed to using random practice schedule[17], open environments, implicit feedback[16] and more complex cognitive tasks. To avoid fatigue, the patient’s energy levels were monitored and treatment was adapted as needed. Adaptations included: lowering frequency, intensity, and/or amount of exercises during treatment sessions. The adaptation chosen depended on her needs at the time. Upper extremity ROM and strengthening was incorporated into dynamic sitting exercises to reduce the number of exercises provided and to avoid redundancy. Finally, segments of education for both the patient and her husband were included in treatment. Education sessions included the physical, cognitive, behavioural and emotional impacts of TBI, as well as the prognosis and symptoms of TBI[14]. It was important to educate her husband on areas of treatment he could help with, and how he could support his wife throughout her prognosis[14].
*NOTE: Treatment occurred daily, for 1-hr sessions. All of the exercises are listed below, however, not all were performed in a single treatment session. Each day of the week, treatment involved a selection of these exercises, and parameters varied, depending on the patient's tolerance. In addition, it was recommended that the patient work on these exercises outside of rehab as well, either with her husband or other staff [14].
Patient Oriented Goals[edit | edit source]
- Be able to ambulate 225m with a quad cane and minimal supervision, within 4 weeks,
- Be able to enter and exit home (e.g. ascend/descend 4 stairs), with the help of her husband within 4 weeks.
- Be able to sit comfortably and maintain proper seating posture for the duration of a meal (30 minutes) within 4 weeks.
- Be able to grab a cup from a cupboard above head height and bring to a counter 3 times in a row within 4 weeks.
Balance and Mobility[edit | edit source]
Treatment started with basic static sitting and standing postures. Treatment progressed to dynamic exercises after the patient tolerated static postures. These exercises were included in the program to help the patient gain balance prior to introducing more dynamic, functional and complex movements, such as walking and/or ascending and descending stairs[14][18].
| Static sitting: with close supervision | ||
| Exercise | Description | FITT Principle |
| Educate on seating posture in chair | Trunk upright, arms on the armrests, wide base of support with feet (I.e. feet shoulder width apart), back against chair, head & neck erect | N/A |
| Educate on seating posture on edge of bed | Trunk upright, arms placed on the bed beside her body, wide base of support with feet (I.e. feet shoulder width apart), head & neck erect | N/A |
| Hold posture sitting in chair or on edge of bed | Patient practiced seating posture in seated position
She was also encouraged to sit during meals |
F – 3-4 days/week
I – quiet sitting, no movement T – 3 sets holding for 1-minute, with 1-minute break in between sets T – static sitting exercise |
| Dynamic sitting: with close supervision, while maintaining proper seating posture | ||
| Exercise | Description | FITT Principle |
| Functional tasks involving shoulder flexion and abduction | Reaching for a cup on a table, alternating the location of the cup throughout sets
|
F – 3-4 days/week
I – minimal intensity, to patient’s comfort T – 3 sets, 6 reps (1 rep = 1 reach for cup) with 1-minute break in between sets T – dynamic sitting exercise |
| Knee extension | Kicked towards a target | F – 3-4 days/week
I – minimal intensity, to patient’s comfort T – 3 sets, 6 reps (alternating cup location) with 1-minute break in between sets T – dynamic sitting exercise |
| Static standing: one assist in parallel bars | |
| Exercise | FITT principle |
| Standing, eyes open | F – 3-4 days/week
I – quiet standing, no movement, to patient’s comfort T – 3 sets holding for 30 seconds, with 1-minute break in between T – static standing exercise |
| Standing, eyes closed | F – 3-4 days/week
I – quiet standing, no movement, to patient’s comfort T –3 sets holding for 30 seconds, with 1-minute break in between sets T – static standing exercise |
| Dynamic standing: one assist in parallel bars | |
| Exercise | FITT principle |
| Weight shifting left to right | F – 3-4 days/week
I – minimal intensity, to patient’s comfort T – 3 sets, 6 reps (e.g. 6 weight shifts) on each leg, 1-minute break in between sets T – dynamic standing exercise |
| Standing, turning head to look at sticker on wall | F – 3-4 days/week
I – minimal intensity, to patient’s comfort T – 3 sets, 10 reps (alternating location of sticker), 1 –minute break in between sets T – dynamic standing exercise |
| Taking a step forward, backwards and to the side | F – 3-4 days/week
I – moderate intensity, to patient’s comfort T – 3 sets, 3 reps (1 rep = step forward, backwards and to the side), with 1-minute break in between sets T – dynamic standing exercise |
| Marching on the spot | F – 3-4 days/week
I – moderate intensity, to patient’s comfort T – 3 sets, 3 reps on each leg (1 rep = lifting of one leg), with 1-minute break in between sets T – dynamic standing exercise |
Strength Training[edit | edit source]
Core strengthening and strengthening of the lower extremities helped improve coordination and efficiency of walking[18][19].
| Core Strengthening | ||
| Exercise | Description/progression | FITT principle |
| Knee Rolling | Patient lays on back, with knees bent, feet flat on bed and hands resting at her side. Patient rolls her hips so that her knees drop to the left, back to centre, and then to the right. Repeat. | F - 2-3 days/week
I - with gravity, to patient's comfort level T – 3 sets, 6 reps each leg, with 1-minute break in between sets T – strengthening/resistance exercise |
| Single Leg Drop-Outs | Patient lays on back, knees bent, feet flat with hands at her side. Patient rolls her left hip so her left knee goes out to the side, then brings it back to the centre. Repeat with right leg. | F - 2-3 days/week
I - against gravity, to patient's comfort level T – 3 sets, 6 reps each leg, with 1-minute break in between sets T – strengthening/resistance exercise |
| Lower Extremity Strengthening | ||
| Exercise | Description/progression | FITT principle |
| Hip abduction |
|
F - 2-3 days/week
I - with gravity, to patient's comfort level T – 3 sets, 6 reps each leg, with 1-minute break in between sets T – strengthening/resistance exercise |
| Knee extension |
|
F - 2-3 days/week
I - against gravity, to patient's comfort level T – 3 sets, 6 reps each leg, with 1-minute break in between sets T – strengthening/resistance exercise |
| Knee flexion |
|
F - 2-3 days/week
I - against gravity, to patient's comfort level T – 3 sets, 6 reps each leg, with 1-minute break in between sets T – strengthening/resistance exercise |
| Ankle dorsiflexion |
|
F - 2-3 days/week
I - against gravity, to patient's comfort level T – 3 sets, 6 reps each leg, with 1-minute break in between sets T – strengthening/resistance exercise |
Flexibility/Range of Motion Training[edit | edit source]
Therapy focused on stretching muscle groups that have developed contractures or have tightened throughout hospital stay.
| Flexibility/ROM | ||
| Exercise | Description/progression | FITT principle |
| Plantar Flexor Stretch |
|
F - 3-4 days/week
I - comfortable stretch, no pain should be felt T - 3 sets, 3 reps (hold each rep for 20 seconds) T - static stretching |
| Finger & Wrist Flexor Stretch |
|
F - 3-4 days per week
I - comfortable stretch, no pain should be felt T - 3 sets, 3 reps (hold each rep for 20 seconds) T - static stretching |
| Hip Extensor Stretch |
|
F - 3-4 days per week
I - comfortable stretch, no pain should be felt T - 3 sets, 3 reps (hold each rep for 20 seconds) T - static stretching |
Task-Specific Training[20][edit | edit source]
- Supine-to-Sit Transfers
- Sit-to-Stand Transfers
*Practicing with staff or PT whenever she needed/wanted to get out of bed was encouraged. Her husband was educated on how to assist her with transfers.
Gait Training[edit | edit source]
Ambulation is a common goal of many TBI patients, making gait training an important aspect of rehabilitation [14][18]. However, the type of gait training varies depending on the severity of the TBI [18]. The most common forms include range of motion activities, weight shifting, and lower extremity and core strengthening, which were addressed earlier in treatment [18][20]. However, higher level exercises such as dual-task techniques can be introduced to make treatment more engaging and functional for the patient [18].
- Conventional gait training in parallel bars (with assistance)
- Patient walked with support of parallel bars
- Therapist cued patient to move joints appropriately throughout gait cycle
- Worked on reciprocal gait pattern & proper weight shifting
- Virtual reality - Computer-generated virtual environment adds patient engagement, enhances motor learning, and makes gait training more task-oriented [21][22]
- Example: Simulation of walking through grocery store, patient pretended she was pushing cart through isles while grabbing food off shelves (see video below).
| [23] | [24] |
- Dual-task training
- Patient walked slowly on treadmill with assistance or body weight support, and was asked to turn head to look at something on the wall
- Progressed treatment by increasing speed
Aerobic Exercise Training[edit | edit source]
Exercise can improve cardiorespiratory fitness as well as cognitive function among patients with TBI [25].
- Arm cycling
- Progressed to leg cycling and eventually treadmill walking
Use the FITT principle
- F - 3-4 days/week
- I - 60-90% of age predicted max HR (~93-140bpm)
- T - 20-40 min per session
- T - aerobic exercise
Outcome[edit | edit source]
4 Weeks in In-Patient Rehabilitation (Re-Assessment)[edit | edit source]
The ROM and flexibility exercises helped normalize the patient's muscle tone, especially in the left side of the body, The left upper extremities and lower extremities showed a slight increase in extensor and flexor muscle tones, respectively, classified as Grade 1 on the Modified Ashworth Scale.
With the decrease in contracture, she was able to isolate movements on the left side of the body, which facilitated her ability to perform ADL's such as self-care. Additionally, the therapist observed her Ranchos level to be VII (automatic-appropriate), suggesting that the patient required minimal assistance in daily living skills. Similarly, her FIM score of 106 suggested that she no longer required assistance to accomplish tasks, but might require supervision to ensure safety[13].
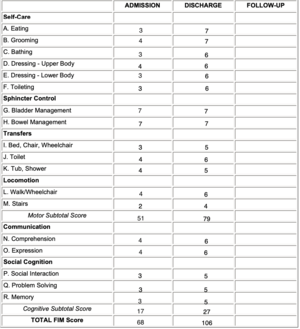
Additionally, gait training combined with static and dynamic balance resulted in improvement of her gait:
- Berg Balance score= 49/56 (above the cut-off score of 45 for increased risk of falls in older adults)[11]
- Gait speed= 0.73m/s, which is clinically significant (i.e., MCID= 0.16m/s) [27]
- The patient independently ambulated 250m with a quad cane, and ascended and descended 4 steps of stairs with minimal assistance.
Discharge Planning[edit | edit source]
The patient was considered appropriate for discharge based on the following information:
- The patient achieved a FIM score of 106
- The patient was able to safely ambulate 250m with a quad cane and go up and down 4 steps with the help of her husband. Based on her performance, she should be able to enter and exit her home, a bungalow with 4 steps, and ambulate within the home as needed, with the help of her spouse.
- Berg score 49/56
- Ranchos los amigos level VII (automatic-appropriate)
Prior to discharge, the physiotherapist and occupational therapist had an education session with the patient and her spouse focusing on safe community ambulation and performing ADLs within the home. The patient also received a document with the same information to refer to when needed.
- Her spouse was made aware of the fact that patients at Ranchos Level VII can overestimate their abilities and be unaware of the consequences of a decision[6]. As such, her husband was encouraged to talk about safety and emergency measures with the patient[28]. Furthermore, it was encouraged to do activities together, such as laundry and groceries, even though the patient does not need close supervision in performing a task[28]. The patient can be distracted, so it was encouraged to write a list of daily to do lists[28][6]. It was possible that the patient was unaware of people’s feelings and could potentially act uncooperatively in social situations[28]. In that case, it was recommended to use a calm tone to offer feedback on such behaviour[28].
The patient has been referred to a home-based rehabilitation program where she will be followed by a physiotherapist and an occupational therapist.
Discussion[edit | edit source]
The fictional case study followed a 65-year of woman attending physiotherapy in an in-patient rehabilitation unit following a craniotomy for a subdural haematoma. The initial examination findings, 2 weeks after surgery, included impaired memory, balance issues, limited ambulation and increased tone in the left and right upper extremities and left lower extremities. Physiotherapy interventions consisted of balance training, task-specific exercises, strength training, flexibility exercises, gait training and postural education. Upon reassessment of outcome measures, 4 weeks after in-patient rehabilitation, the patient showed improvement in her FIM score, Berg Balance Scale, lower muscle tone (i.e., Modified Ashworth Scale), faster gait speed and endurance.
This case study included traditional physiotherapy to improve her strength, range of motion, performance of functional tasks, transfers, and posture. In addition to traditional methods, virtual reality was used to improve her gait. Based on her outcomes, the use of virtual reality to improve gait showed promise. Although there are many studies that demonstrate the benefits of the use of virtual reality and gait training, few physiotherapists use virtual reality in practice[18]. This raises the question of whether this is due to lack of knowledge of the benefits, lack of funding or both. Future inquiry should address the barriers to implementing the use of virtual reality in physiotherapy practice and beneficial technologies regarding the rehabilitation of patients with TBIs.
Furthermore, it is important to take the patient’s cognitive status into consideration during treatment and in discharge planning. Physiotherapists in this case study tailored rehabilitation to the patient’s cognitive abilities to maximize treatment outcomes by using implicit learning early in rehabilitation, and explicit learning later in treatment. Implicit learning strategies were used early in rehabilitation because the treatment focused on functional tasks, and implicit learning ensures acquisition and retention of a given skill [16]. In contrast, explicit learning allows the patient to transfer learning to different tasks, which had higher importance after the patient mastered the skill[16]. This being said, research on motor learning strategies used in TBI patients is not clear [16]. Some studies show that implicit feedback is less impaired following a TBI, therefore it is argued that explicit feedback should be the focus in treatment [16]. Other research argues that implicit learning should be the focus[16]. Therefore, it is unclear as to which approach is better, and what sequence the learning styles should be provided during TBI rehabilitation [16].
In summary, although the patient in this case study showed general improvements in functional ability, there are some evidence gaps regarding the effectiveness of certain rehabilitation interventions following a TBI. In particular, further research must be done on the effectiveness of implicit and explicit learning strategies, as well as the effectiveness and prevalence of virtual reality use in rehabilitation following a TBI.
References[edit | edit source]
- ↑ Bell C, Hackett J, Hall B, Pülhorn H, McMahon C, Bavikatte G. Symptomatology Following Traumatic Brain Injury in a Multidisciplinary Clinic: Experiences from a Tertiary Centre. Br. J. Neurosurg. 2018;32(5):495–500. DOI: 10.1080/02688697.2018.1490945.
- ↑ Brazinova A, Rehorcikova V, Taylor MS, Buckova V, Majdan M, Psota M, et al. Epidemiology of Traumatic Brain Injury in Europe: A Living Systematic Review. J. Neurotrauma. 2018; 33:1-30. DOI: 10.1089/neu.2015.4126
- ↑ 3.0 3.1 Heydari F, Golban M, Majidinejad S. Traumatic Brain Injury in Older Adults Presenting to the Emergency Department: Epidemiology, Outcomes and Risk Factors Predicting the Prognosis. Emerg Med J 2019;4,2e19. DOI:10.22114/ajem.v0i0.170
- ↑ Carlisi E, Feltroni L, Tinelli C, Verlotta M, Gaetani P, Toffola ED. Postoperative rehabilitation for chronic subdural hematoma in the elderly. An observational study focusing on balance, ambulation and discharge destination. Eur J Phys Rehabil Med 2017;53(1):91-97. DOI: 10.23736/S1973-9087.16.04163-0
- ↑ 5.0 5.1 5.2 Levin HS, O'Donnell VM, Grossman RG. The Galveston Orientation and Amnesia Test. A Practical Scale to Assess Cognition After Head Injury. J Nerv Ment Dis 1979;167:675-84. DOI:10.1097/00005053-197911000-00004
- ↑ 6.0 6.1 6.2 6.3 6.4 6.5 6.6 Rancho Los Amigos - Revised [Internet]. Rancho Los Amigos Revised. [cited 2020May19]. Available from: https://www.neuroskills.com/education-and-resources/rancho-los-amigos-revised/
- ↑ 7.0 7.1 Whyte J, Hart T, Bode RK, Malec J. The Moss Attention Rating Scale for Traumatic Brain Initial Psychometric Assessment. Arch Phys Med Rehabil Vol 2003;84268-276. DOI:10.1053/apmr.2003.50108
- ↑ Moss Attention Rating Scale (MARS) [Internet]. Moss Rehabilitation Research Institute (MRRI). [cited 2020May21]. Available from: https://mrri.org/moss-attention-rating-scale-mars/
- ↑ 9.0 9.1 9.2 Agitated Behavior Scale [Internet]. Shirley Ryan AbilityLab. [cited 2020May19]. Available from: https://www.sralab.org/rehabilitation-measures/agitated-behavior-scale
- ↑ 10.0 10.1 10.2 Steel RT, Kreutzer JS. Depression Assessment After Traumatic Brain Injury: An Empirically Based Classification Method. Arch Phys Med Rehab 2003;84:621-1628. DOI:10.1053/S0003-9993(03)00270-3
- ↑ 11.0 11.1 11.2 Santos GM, Souza ACS, Virtuoso JF, Tavares GMS, Mazo GZ. Predictive values at risk of falling in physically active and no active elderly with Berg Balance Scale. Revista Brasileira de Fisioterapia. 2011;15(2):95–101.DOI:0.1590/s1413-35552011000200003
- ↑ In Depth Review of the Modified Ashworth Scale [Internet]. Stroke Engine. [cited 2020May21]. Available from: https://www.strokengine.ca/en/indepth/mashs_indepth/
- ↑ 13.0 13.1 Serfontein L, Visser M, Schalkwyk MV, Rooyen CV. The perceived burden of care among caregivers of survivors of cerebrovascular accident following discharge from a private rehabilitation unit. South African Journal of Occupational Therapy. 2019;49(2):24–32. DOI:org/10.17159/2310-3833/2019/vol49n2a5
- ↑ 14.0 14.1 14.2 14.3 14.4 14.5 Ontario Neurotrauma Foundation. Understanding Traumatic Brain Injury: A Handbook for The Rehabilitation of Adults with Moderate to Severe Traumatic Brain Injury. Toronto, ON: Ontario Neurotrauma Foundation. 2020.
- ↑ Miczak, K. Exercise After Traumatic Brain Injury. Alexandria, VA: American Physical Therapy Association Neurology Section. Accessed from: http://www.neuropt.org/docs/default-source/bi-sig/exercise_after_tbi.pdf?sfvrsn=171a4843_2
- ↑ 16.0 16.1 16.2 16.3 16.4 16.5 16.6 16.7 Skidmore ER. Training to Optimize Learning after Traumatic Brain Injury. Curr Phys Med Rehabil Rep. 2015;3(2):99-105. DOI: 10.1007/s40141-015-0081-6.
- ↑ Giuffrida CG, Demery JA, Reyes LR, Lebowitz BK, Hanlon RE. Functional Skill Learning in Men With Traumatic Brain Injury. Am J Occup Ther. 2009;63:398-407. DOI: 10.5014/ajot.63.4.398
- ↑ 18.0 18.1 18.2 18.3 18.4 18.5 18.6 Wilson T, Martins O, Efrosman M, DiSabatino V, Benbrahim MB, Patterson KK. Physiotherapy practice patterns in gait rehabilitation for adults with acquired brain injury, Brain Injury. 2018; 33:3, 333-348, DOI: 10.1080/02699052.2018.1553067
- ↑ Killington MJ, Mackintosh SFH, Ayres M. An isokinetic muscle strengthening program for adults with an acquired brain injury leads to meaningful improvements in physical function. Brain Injury. 2010;24(7-8):970–7. DOI:10.3109/02699052.2010.489792
- ↑ 20.0 20.1 Scottish Intercollegiate Guidelines Network (SIGN). Brain Injury Rehabilitation in Adults: a national clinical guideline. Edinburgh: SIGN. 2013;130.
- ↑ Cano Porras D, Slemonsma P, Inzelberg R, Zeilig G, Plotnik M. Advantages of virtual reality in the rehabilitation of balance and gait: Systematic Review. Neurology 2018;90:1017-1025. DOI:10.1212/WNL.0000000000005603
- ↑ Tefertiller C, Hays K, Natale A, O'Dell D, Ketchum J, Sevigny M, et al. Results From a Randomized Controlled Trial to Address Balance Deficits After Traumatic Brain Injury. Arch Phys Med Rehab 2019;100:1409-1416. DOI:10.1016/j.apmr.2019.03.015
- ↑ VR4REHAB. TBI Patient Treated with SeeMe Virtual Reality System. Available from: https://www.youtube.com/watch?v=S7KHh530drM&t=3s
- ↑ Cleveland Clinic. CAREN Virtual Reality Treadmill: Take a Video Tour. Available from: https://www.youtube.com/watch?v=TntXjlTUhII&feature=emb_title
- ↑ Mossberg K, Amonette WE, Masel BE. Endurance training and cardiorespiratory conditioning after traumatic brain injury. Journal Head Trauma Rehabil 2010;25(3):173-183. DOI: 10.1097/HTR.0b013e3181dc98ff
- ↑ Functional Independence Measure [Internet]. Shirley Ryan AbilityLab. [cited 2020May19]. Available from: https://www.sralab.org/rehabilitation-measures/fimr-instrument-fim-fimr-trademark-uniform-data-system-fro-medical
- ↑ Bohannon RW, Glenney SS. Minimal clinically important difference for change in comfortable gait speed of adults with pathology: a systematic review. Journal of Evaluation in Clinical Practice. 2014;20(4):295–300. DOI:10.1111/jep.12158
- ↑ 28.0 28.1 28.2 28.3 28.4 Rancho Scale - Level 7 [Internet]. Rancho Scale - Level 7 - Sunnybrook Hospital. [cited 2020May22]. Available from: https://sunnybrook.ca/content/?page=rancho-scale-brain-injury-level-7






