Biomechanics and Dynamics of the Pelvic Girdle
Original Editor - Wanda van Niekerk
Top Contributors - Wanda van Niekerk, Tarina van der Stockt, Kim Jackson, Lucinda hampton, Vidya Acharya and Olajumoke Ogunleye
Sacral Biomechanics[edit | edit source]
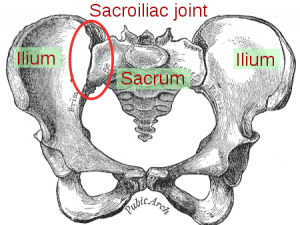
The sacroiliac joint (SIJ) is the largest axial joint in the body. It connects the spine to the pelvis and transfers load between the lumbar spine and the lower extremities. The SIJ does not have much stability against shear loads. Several ligaments across the joint support and limit movement of the SIJ.[1]
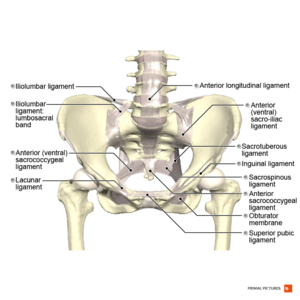
The sacrum tightly wedges between the ilia and the ligaments provide resistance to shear loads.[2] Additional resistance is also provided by grooves and ridges to protect the joint against shearing.[2][3] Although several of the body’s largest and powerful muscles surround the SIJ, no muscle directly affects sacral movements.[1] Muscles that do play a role in providing SIJ stability through increasing compression load across the joint are the transversus abdominis and the pelvic floor muscles (levator ani and coccygeus muscles). Ligaments that play an important role in SIJ stability are the iliolumbar ligament (ventral side), the posterior sacroiliac ligaments, interosseus ligaments, sacrotuberous and sacrospinous ligaments. The pubic ligaments, the anterior sacroiliac ligaments and the dorsal side of the iliolumbar ligaments have the least effect on pelvic stability.[1][2]
The Sacroiliac Joint[edit | edit source]
The Sacroiliac Joint (SIJ) is a synovial joint between the auricular surfaces of the sacrum bone and the two ilium bones [4]. The auricular surfaces are covered in hyaline cartilage and are broader above and narrower below. The SIJ is also a true diarthrodial joint, as it has a joint space, filled with synovial fluid between the matching articulating surface and a fibrous capsule. However, it is different from other diarthrodial joints as it has fibrocartilage and hyaline cartilage on the auricular surfaces.[5] The SIJ main roles' are to provide stability and offset the load of the trunk to the lower limbs.[6] The SIJ has a high level of stability from the self-locking mechanisms of the pelvis, which comes from the anatomy and shape of the bones in the SIJ (Form Closure) and also the muscles supporting the pelvis (Force Closure).[7][8]
Form and Force Closure[edit | edit source]
Form Closure[edit | edit source]
Form closure describes the stability of the joint from the design of the pelvic anatomy. The sacrum and the ilium each have one flat surface[10] and one ridged surface which interlocks together, promoting stability[11]. The symmetrical grooves and ridges allow the highest coefficient of friction of any diarthrodial joint and protect the joint against shearing. The position of the bones in the SIJ creates a “keystone-like” shape which adds to the stability in the pelvic ring. This “keystone” shape is created, as the sacrum has a wider side superiorly, which allows the sacrum to be “wedged” in between the ilium[12].
Force Closure[edit | edit source]
Although form closure provides stability to the SIJ, for mobility to occur, further joint compression and stabilisation is required to withstand a vertical load[11][12]. Force closure is the term used to describe the other forces acting across the joint to create stability[13]. This force is generated by structures with a fibre direction perpendicular to the sacroiliac joint and is adjustable according to the loading situation.[11] Muscles, ligaments and the thoracolumbar facia all contribute to force closure[8][11][12]. Force closure is particularly important during activities such as walking when unilateral loading of the legs creates shear forces.[11][10]
Force closure creates greater friction and therefore increased form closure and what is called “self-bracing” or “self-locking” of the joint [13][14][15][16][7]. According to Willard et al.[12] force closure reduces the joint’s ‘neutral zone’ thereby facilitating stabilisation.
As the ilium and sacrum only meet for approximately a third of the surfaces, the rest of the stability between the bones is provided by the ligaments[6].
Range of Motion[edit | edit source]
The sacrum can move with respect to the ilium in all directions, but the magnitude of motion is minimal at about 6° of freedom. The SIJ range of motion in flexion-extension is about 3°. Axial rotation is about 1.5° and lateral bending is about 0.8°.[1] The two main movements occur when the sacrum moves relative to the iliac bones in the sagittal plane. Nutation describes when the sacrum is rotated forwards relative to the iliac bones and Counternutation describes when the sacrum is rotated backwards relative to the iliac bones.[18][3]
According to Willard et al[12] nutation can be regarded as anticipation for joint loading, as it is a more stable than counternutation. During nutation, the posterior parts of the iliac bones are compressed into the “keystone-like” shape, and the joint is in the locked and close-packed position[11]. This normally occurs during increased load-bearing situations e.g. standing and sitting, to increase stability[3][14].
Ligaments involved in nutation and counternutation[edit | edit source]
Ligaments that tighten with sacral counternutation[21]:- Long dorsal sacroiliac ligament
- The upper band of the iliolumbar ligament
Ligaments that tighten with sacral nutation[21]:
- Sacrotuberous
- Sacrospinous
- The lower band of the iliolumbar ligament
- Interosseus
Sexual Dimorphism[edit | edit source]
The female sacrum is wider, more uneven, less curved and more backward rotated. The male pelvis tends to be relatively long and narrow, with a longer and more conical pelvic cavity compared to the female pelvis. The female pelvis has a wider sciatic notch and the acetabula are wider apart compared to the male pelvis.[1][8]
These sex differences are also seen in the biomechanics of the SIJ with the female SIJ having higher mobility and greater stresses, greater loads and more pelvis ligament strains compared to the male SIJ. Furthermore, the influence of hormones such as relaxin, which increases the mobility of the SIJ by providing ligament laxity for birth, needs to be considered. All these features may contribute to women being more prone to incidences of SIJ and pelvic pain due to high mobility.[1]
[22]Musculoskeletal Dynamics[edit | edit source]
Superficial Anatomical Sling Systems[edit | edit source]
The four muscle slings around the pelvic girdle that contribute to force closure of the pelvis are[23]:
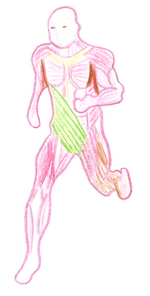
Anterior Oblique Sling (AOS)[edit | edit source]
- External and internal obliques connecting with contralateral adductor muscles via the adductor-abdominal fascia[23]
- Contraction of these group of muscles provides stability, compressing the pelvic girdle, resulting in force closure of the pubic symphysis
- Multidirectional sports such as tennis, soccer, football, basketball rugby and hockey places a great demand on the AOS as it must not only contribute to accelerating the body but also to rotating and decelerating it during the change of direction.
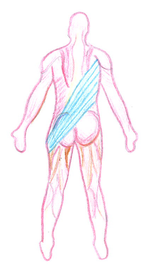
Posterior Oblique Sling (POS)[edit | edit source]
- Latissimus Dorsi, gluteus maximus, biceps femoris and interconnecting thoracolumbar fascia[25]
- Muscles work as synergists to directly stabilise the pelvic girdle
- Force closure increases indirectly due to the anatomical attachments of the gluteus maximus and the thoracolumbar fascia with the sacrotuberous ligament
- POS works with AOS to create balance
Deep Longitudinal Sling[edit | edit source]
- Erector Spinae, multifidus, thoracolumbar fascia, sacrotuberous ligament and biceps femoris[23]
- The sling allows for movement in the sagittal plane while also influencing local stability
- Contraction of the sacral part of multifidus causes sacral nutation thereby increasing tension in the interosseus and short dorsal ligaments and thus creating increased force closure of the SIJ[27]
- The iliac attachments of multifidus together with erector spinae pull the posterior parts of the iliac bones toward each other and therefore limiting further nutation
- Contraction of erector spinae and long head of biceps may increase force closure due to their anatomical attachments with the sacrotuberous ligament.
- Contraction of erector spinae and multifidus has broadening effect (inflation of the fascial cylinder), this will increase tension and assist with force closure.
Lateral Sling[edit | edit source]
- Gluteus medius, gluteus minimus, tensor fascia latae (TFL) and iliotibial band (ITB)[23]
- Sling provides stability in the coronal plane and involved in pelvo-femoral stability in dynamic movements (gait, lunges, stair climbing)
- To understand the relevance of the lateral sling, the actions of the muscles need to be understood
- Hip abduction and medial rotation – gluteus medius and minimus
- Tensor Fascia Latae works in synergy with these muscles to hold pelvis level in single leg movements
- Tensor Fascia Latae also works with gluteus maximus on ITB to stabilise the hip joint by holding the head of the femur in the acetabulum
- Movements involving single-leg stance, such as walking, lateral sling comes into tension to maintain pelvis stable over stance leg and preventing pelvic drop on the opposite side of the pelvis[29]
- Failed control of lateral sling often presents a hip drop/ Trendelenburg sign during the stance phase of gait and single-leg stance
A good understanding of the concept of these anatomical slings and the ways in which they function to influence lumbopelvic stability and function will be helpful in deciding on which treatment strategy to apply in patients with pelvic girdle dysfunction.
[31]For a further in-depth look at anatomy slings see this PP page: Anatomy Slings and their Relationship to Lower Back Pain
Integrated Model of Function[edit | edit source]
The integrated model of function has been derived from anatomical and biomechanical studies of the pelvis as well as clinical experience. This model aims to address why the pelvis is painful and not able to sustain and transfer loads as opposed to a model which only seeks to identify specific pain generating structures. The four components of this model are[32]:
- Form closure (structure)
- Force closure (forces produced by myofascial action)
- Motor control (specific timing of muscle action/inaction during loading)
- Emotions
This model suggests that multiple factors affect joint mechanics. Some of these factors may be intrinsic to the joint itself, whereas other factors are produced by muscle action. These in turn can be influenced by the emotional state. To effectively manage pelvic girdle pain or dysfunction it is necessary to address all four components to guide patients towards a healthier way to live and move.[32]
For more detail on the integrated model of function read this chapter: Principles of the Integrated Model of Function and its Application to the Lumbopelvic-hip Region Chapter 5 in: The Pelvic Girdle
Neurovascular Dynamics[edit | edit source]
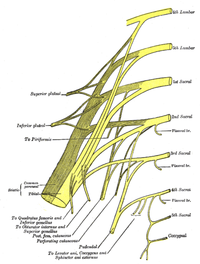
Innervation of the Pelvis[edit | edit source]
Innervation of the pelvis includes the sacral and coccygeal plexuses[3]:
- Sacral plexus:
- derives from L4-S4 nerve roots
- sits on the internal surface of the piriformis muscle
- most of the sacral nerves stemming from the sacral plexus exit through the greater trochanteric notch
- the sciatic nerve forms out of sacral plexus and may be compressed by muscle, causing radicular pain down the leg
- Coccygeal plexus
- derives from the S4 - S5 nerve roots
- lies along the coccygeus muscle on the pelvic surface
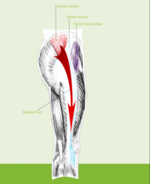
Problematic Nerves in the Pelvic Girdle[edit | edit source]
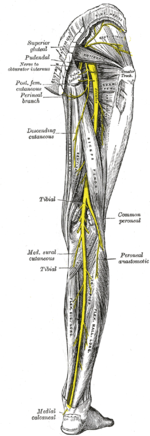
Sciatic nerve[edit | edit source]
- Responsible for low back, buttock, posterior thigh/leg/foot pain and weakness[33]
- Widest and longest nerve
- Branches from L4 to S3
- Innervates[33]:
- Lateral hip rotators (except for piriformis)
- Posterior compartment of the thigh
- Branches into common peroneal and tibial nerve
Obturator Nerve[edit | edit source]
- Difficulty ambulating[34]
- Possible lower extremity instability
- Deep ache in adductors by the pubic bone
- Exercise-related pain or groin pain[34]
- Pain and weakness worsens with exercise[34]
- Impaired jumping ability in athletes
Superior Gluteal Nerve[edit | edit source]
- Arises from the dorsal divisions of L4, L5, S1 nerve roots of the sacral plexus[35]
- Innervates[35]:
- gluteus medius
- gluteus minimus
- Tensor fascia latae
- Piriformis entrapment
- Aching claudication-type buttock pain
- Tenderness to palpation
- A weakness of abduction and a waddling gait[35]
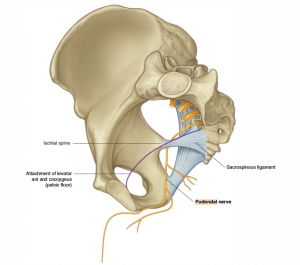
Pudendal Nerve[edit | edit source]
Specific symptoms present with pudendal neuralgia[36]:
- Pelvic pain with sitting except on toilet
- Discomfort with tight clothing
- Bladder/bowel symptoms
- Hesitancy, frequency, urgency, retention, constipation, pain
- Dyspareunia
- Genital pain
- Anal pain
- Condition is often misdiagnosed and mistreated[37]
- Causes may be excessive sitting or cycling
Resources[edit | edit source]
[38]References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 Kiapour A, Joukar A, Elgafy H, Erbulut DU, Agarwal AK, Goel VK. Biomechanics of the sacroiliac joint: anatomy, function, biomechanics, sexual dimorphism, and causes of pain. International journal of spine surgery. 2020 Feb 1;14(s1):S3-13.
- ↑ 2.0 2.1 2.2 Zlomislic V, Garfin SR. Anatomy and Biomechanics of the Sacroiliac Joint. Techniques in Orthopaedics. 2019 Jun 1;34(2):70-5.
- ↑ 3.0 3.1 3.2 3.3 Le Huec JC, Bourret S, Thompson W, Daulouede C, Cloché T. A painful unknown: sacroiliac joint diagnosis and treatment. EFORT Open Reviews. 2020 Oct;5(10):691-8.
- ↑ Palastanga N, Field D and Soames R. Anatomy and Human Movement structure and function. 5th edition. 2006. Elsevier Ltd.
- ↑ Forst S.L, Wheeler M, Fortin J.D and Vilensky J.A. The Sacroiliac Joint: Anatomy, Physiology and Clinical Significance. Pain Physician. 2006;9:61-68
- ↑ 6.0 6.1 Cohen S.P. Sacroiliac Joint Pain: A Comprehensive Review of Anatomy, Diagnosis, and Treatment. Anesthesia & Analgesia 2005: 101:1440-53
- ↑ 7.0 7.1 Arumugam A, Milosavljevic S, Woodley S and Sole G. Effects of external pelvic compression on form closure, force closure, and neuromotor control of the lumbopelvic spine. A systematic review. Manual Therapy 2012; 17: 275-284
- ↑ 8.0 8.1 8.2 Vleeming A, Schuenke MD, Masi AT, Carreiro JE, Danneels L, Willard FH. The sacroiliac joint: an overview of its anatomy, function and potential clinical implications. Journal of anatomy. 2012 Dec;221(6):537-67.
- ↑ SI Bone. SI Joint Anatomy, Biomechanics and Prevalence. Available from: http://www.youtube.com/watch?v=D6NTMgWCSaU [last accessed 19/04/14]
- ↑ 10.0 10.1 Liebenson C. The relationship of the sacroiliac joint, stabilization musculature, and lumbo-pelvic instability. Journal of bodywork and movement therapies 2004:8:43-45.
- ↑ 11.0 11.1 11.2 11.3 11.4 11.5 Pool-Goudzwaard A.L, Vleeming A, Stoeckart R, Snijders C. J & Mens J.M.A. Insufficient lumbopelvic stability: a clinical, anatomical and biomechanical approach to ‘a-specific’ low back pain. Manual Therapy. 1998; 3(1): 12-20
- ↑ 12.0 12.1 12.2 12.3 12.4 Willard F.H, Vleeming A, Schuenke M.D, Danneels L & Schleip R. The thoracolumbar fascia: anatomy, function and clinical considerations. Journal of Anatomy 2012; 221(6): 507-36
- ↑ 13.0 13.1 Takasaki H, Iizawa T, Hall T, Nakamura T, Kaneko S. The influence of increasing sacroiliac joint force closure on the hip and lumbar spine extensor muscle firing pattern. Manual Therapy; 2009:14:5: 484-489.
- ↑ 14.0 14.1 Vleeming A, Stoeckart R, Volkers, ACW, Snijders CJ. Relation between form and function in the sacroiliac joint. Part 1: Clinical anatomical aspects. Spine 1990a; 15(2): 130-132
- ↑ Vleeming A, Volkers ACW, Snijder CJ, Stoeckart R. Relation between form and function in the sacroiliac joint. Part 2: Biomechanical aspects. Spine 1990b; 15(2):133-136
- ↑ Snijder CJ, Vleeming A, Stoeckart R. Transfer of lumbosacral load to iliac bones and legs. Part 1: Biomechanics of selfbracing of the sacroiliac joints and its significance for treatment and exercise. Journal of Clinical Biomechanics 1993a; 8:295-301
- ↑ Catalyst University. The sacroiliac joint (part 2). Factors affecting stabilisation. Available from https://www.youtube.com/watch?v=RtnkNJmdMH4&t=638s. (last accessed 20 December 2020)
- ↑ Toyohara R, Kurosawa D, Hammer N, Werner M, Honda K, Sekiguchi Y, Izumi SI, Murakami E, Ozawa H, Ohashi T. Finite element analysis of load transition on sacroiliac joint during bipedal walking. Scientific reports. 2020 Aug 13;10(1):1-0.
- ↑ Catalyst University. The Sacroiliac joint. Sacral nutation and counternutation. Available from https://www.youtube.com/watch?v=nxvtQt5PL2E. (last accessed 20 December 2020)
- ↑ PT Final Exam. Nutation vs Counternutation. Available from https://www.youtube.com/watch?v=2gr5-oKBT2Q (last accessed 20 December 2020)
- ↑ 21.0 21.1 Cho HJ, Kwak DS. Movement of the sacroiliac joint: Anatomy, systematic review, and biomechanical considerations. Proceedings of the Institution of Mechanical Engineers, Part H: Journal of Engineering in Medicine. 2020 Nov 30:0954411920978021.
- ↑ Judson Laipply. Tixe Schooling. Male pelvis vs Female pelvis. Available from https://www.youtube.com/watch?v=7pYuLtv29m0. (last accessed 20 December 2020)
- ↑ 23.0 23.1 23.2 23.3 Lee, D; Vleeming, A; Jones, M. The Pelvic Girdle: An Integration of Clinical Expertise and Research. Edinburgh: Elsevier/Churchill Livingstone, 2011.
- ↑ Yoga Anatomy. Anterior oblique sling system - Myofascial slings (Vleeming & Lee). Available from https://www.youtube.com/watch?v=-13QIq-5qa8&t=65s. (last accessed 20 December 2020)
- ↑ Lee JK, Lee JH, Kim KS, Lee JH. Effect of abdominal drawing-in maneuver with prone hip extension on muscle activation of posterior oblique sling in normal adults. Journal of Physical Therapy Science. 2020;32(6):401-4.
- ↑ Yoga Anatomy. Posterior Oblique sling system - Myofascial slings - (Vleeming & Lee). Available from https://www.youtube.com/watch?v=YpJbL-IA-wA. (last accessed 20 December 2020)
- ↑ Vleeming, A; Mooney, V; Stoeckart, R. Movement, Stability & Lumbopelvic Pain, Integration of Research and Therapy. UK: Churchill Livingstone, 2007
- ↑ Institute Education. Posterior Longitudinal Sling. Available from https://www.youtube.com/watch?v=VtWQQNSZ6KU. (last accessed 20 December 2020)
- ↑ Drake, R; Vogl, W; Mitchell, A. Gray’s Anatomy for Students, Third Edition. London: Churchill Livingstone, 2015.
- ↑ Institute Education. Lateral Sling. Available from https://www.youtube.com/watch?v=gjxytSr_qoE. (last accessed 20 December 2020).
- ↑ Physiopedia. Slings & Sacroiliac Joint Pain by Ismail Saracoglu, University of Nottingham. Available from https://www.youtube.com/watch?v=pBgZoApSltY. (last accessed 20 December 2020)
- ↑ 32.0 32.1 Lee D, Hodges P. Principles of the integrated model of function and its application to the lumbopelvic-hip region. The Pelvic Girdle, ed. 2004;3:41-54.
- ↑ 33.0 33.1 Davis D, Vasudevan A. Sciatica. InStatPearls [Internet] 2019 Feb 28. StatPearls Publishing.
- ↑ 34.0 34.1 34.2 Koh M, Markovich B. Anatomy, Abdomen and Pelvis, Obturator Nerve. InStatPearls [Internet] 2019 Dec 11. StatPearls Publishing.
- ↑ 35.0 35.1 35.2 Lung K, Lui F. Anatomy, Abdomen and Pelvis, Superior Gluteal Nerve. InStatPearls [Internet] 2018 Dec 9. StatPearls Publishing.
- ↑ Kaur J, Singh P. Pudendal Nerve Entrapment Syndrome. InStatPearls [Internet] 2019 Jun 21. StatPearls Publishing.
- ↑ Filler AG. Diagnosis and treatment of pudendal nerve entrapment syndrome subtypes: imaging, injections, and minimal access surgery. Neurosurgical focus. 2009 Feb 1;26(2):E9.
- ↑ BASEM Education. SIJ Biomechanics. Available from https://www.youtube.com/watch?v=XT4PXg_YoTU. (last accessed 21 December 2020)