Assessment and Treatment of the Thoracic Spine
Top Contributors - Jess Bell, Kim Jackson, Kirenga Bamurange Liliane, Tarina van der Stockt, Lucinda hampton, Olajumoke Ogunleye, Aminat Abolade and Merinda Rodseth
Subjective Assessment[edit | edit source]
Further information about the assessment of the thoracic spine is available here, but specific questions to consider in the subjective assessment include:[1]
- How did the problem begin? How long has it been a problem?
- How has the pain progressed over time?
- Is there a history of overload or trauma?
- Does the patient have pain with breathing? And if so, during which part of the breath does this occur?
- What effect does coughing and / or sneezing have?
- Can the patient lie on the affected side at night?
- How is the pain behaving and what is the level of irritability?
- Is there stiffness for a prolonged period in the morning?
- Is there also a history of enthesopathies?
- This history could indicate that the patient has a seronegative spondyloarthropathy[1][3]
- What are the patient's functional impairments?
- Consider sport and activities of daily living
- What is the patient’s medical history?
- It is essential to have a detailed understanding of this history as there are a number of conditions that can masquerade as musculoskeletal thoracic pain
- Are there any psychosocial factors contributing to the pain?
- Are there any red flags?[4]
Subjective information can give quite specific clues about the potential cause of pain (i.e. inflammatory, mechanical or non-mechanical):[1]
- Nerve root or facet pain may be described as lancinating / nauseating. It may radiate and follow the angulation of the rib
- Costochondritis tends to be described as a deep, boring, aching pain in the chest wall that may radiate (often posteriorly or to the neck)
- Rib fracture or intercostal strain is typically described as a sudden, sharp / piercing pain, which is then aggravated by laughing, sneezing, coughing, deep breaths or any type of straining manoeuvre
- Constant, burning pain can be a sign of inflammation
- This could be from an auto-immune disorder, a severely effected joint, or referred from another structure (e.g. a duodenal ulcer might cause a constant burning pain in the thoracic region)
- When patients have immobility, they tend to report stiffness, restricted movement, or a sense of feeling ‘stuck’
Objective Assessment[edit | edit source]
The objective examination is guided by findings in the subjective interview. Remember:[1]
- It is essential to understand which structures are loaded during each test
- Keep tests to a minimum
- “Less is more” to avoid flaring up the patient
- Consider combinations of tests
- The best ‘special test’ is the one the patient demonstrates to you
- Consider the diaphragm
Objective Testing[edit | edit source]
The following tests should be included in an objective examination of the thoracic spine:[1]
- Static and dynamic postural assessment:
- Watch how the patient moves / drifts / hinges
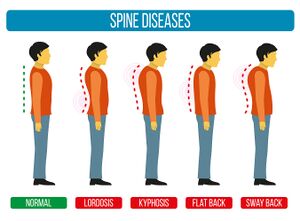
- Consider different types of postural dysfunctions[5] (see Figure 1)
- Is the postural change a primary or secondary problem (e.g. lumbopelvic dysfunction)
- Breathing mechanics
ROM tests from neutral
- Look for intersegmental restrictions
- Assess from behind
- Inter-ring and articular palpation during motion
- Motor control and strength tests
- Sitting
- Puppy lie (i.e. prone extension propped on forearms)
- 4 point
- Neurodynamic tests
- Upper limb tension test for thoracic outlet syndrome (TOS) (see videos below)[6][7] - NB this test may not always be positive in TOS patients, but it needs to be assessed in detail[1]
- Neurological
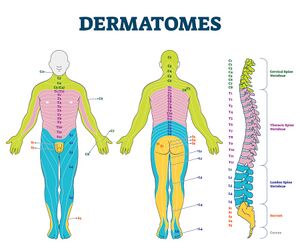
- Thoracic dermatome testing (see Figure 2)
- Palpation, including the clavicle and first rib
Active Thoracic Movement Tests[edit | edit source]
During the active movement tests:[1]
- Assess the patient in sitting in order to isolate the thoracic spine (this position blocks the lumbar spine)
- Assess for asymmetry of movement and any segmental restriction
- Remember that motor control is also important in the thoracic region, not just stiffness
Thoracic Flexion and Extension[edit | edit source]
- Flexion: feel for anterior tilt of the ribs
- Extension: feel for posterior tilt of the ribs
- NB extension is the most limited movement in the thoracic spine[10]
Thoracic Rotation[edit | edit source]
Rotation is one of the most useful tests for the thoracic spine. During rotation movements, it is possible to identify:[1]
- Stiffness
- Sequencing issues
Thoracic Side Bend / Lateral Shift[edit | edit source]
Assess the patient from behind - it is only necessary to assess the patient from the front if you wish to specifically examine the ribs from this position. During thoracic side bend there is:[1]
- Ipsilateral approximation of the ribs
- Contralateral separation of the ribs
- Contralateral rib translation
Treatment[edit | edit source]
Sleep[edit | edit source]
Sleep is the most powerful antioxidant.[1] It is recognised that there is a bi-directional relationship between pain and sleep.[11]
Thoracic Manipulation[edit | edit source]
It is still not known if / why thoracic manipulation works, but it has been found that thoracic manipulation can decrease pain, improve mobility and enhance a patient’s feeling of health.[12]
- There is, however, no evidence that one manipulation is better than another
- There is no evidence that thoracic manipulation has a long-term effect, so if it is used, it should be used in combination with specific rehabilitation exercises
- Joint position, direction, velocity and force are all variables that should be considered[1]
Postural Correction and Motor Control[edit | edit source]
Correcting a patient’s posture can also have a positive impact on a patient’s pain.[1]
- Consider the centre of gravity
- Look for areas of muscle spasm or hyperactivity (e.g. of iliocostalis)
Iliocostalis Release[edit | edit source]
Iliocostalis is the most lateral of the erector spinae.[13] Patients with significant thoracic kyphosis and lumbar lordosis may have increased activity of iliocostalis. This muscle can be released under the 10th and 11th ribs.[1]
Posterior-Anterior Glides[edit | edit source]
Patients with inverted thoracic spines, rotated spines and / or increased kyphosis will likely find posterior-anterior (PA) glides of the spinous processes uncomfortable as they are highly nociceptive.[1]
Instead, it can be beneficial to perform a PA glide on the rib angle (which results in a mobilisation of 13 articulations for each thoracic ring). For individuals with inverted spines, this will create an anterior-posterior (AP) movement on the spinous process.[1] For patients with increased kyphosis, a PA glide on the rib angle while performing an AP glide on the anterior shoulder / coracoid can be effective. A rotatory technique for patients with kyphosis can be effective.[1]
Exercise Therapy[edit | edit source]
A survey of thoracic spine management trends in the United Kingdom found that exercise is used widely as a treatment modality despite limited supporting evidence.[14] Speed, starting positions, dosage and load progression have not been investigated, but exercises which aim to stretch, mobilise and stabilise the thoracic spine can be beneficial in clinical practice.[1]
Types of Exercises[edit | edit source]
Stretches for the thoracic spine are shown in Figure 3. Figure 4 shows stretches that can specifically address an inverted thoracic spine.
Figures 5 and 6 show exercises to mobilise the thoracic spine, while Figure 7 focuses specifically on exercises that rotate the thoracic spine.
Exercises to stabilise the thoracic spine are shown in figures 8, 9 and 10. Initially it is beneficial to use closed kinetic chain exercises (Figures 8 and 9) before aiming to increase strength through range (Figure 10).
A Lot is Unknown[edit | edit source]
- Most ‘research’ is anecdotal, or found on social media / YouTube
- Information from other regions of the spine has been ‘transferred’ to the thoracic spine
- The unique features of the thoracic spine are often not recognised
- There are many deep thoracic muscles whose contribution to motor control in the thorax is unknown, such as semispinalis thoracic and rotatores
- It is also not known what role the thoracic spine has in proprioception
Summary[edit | edit source]
Assessment:[1]
- It is beneficial to use anatomical knowledge and biomechanical insights to look at poor motion habits
- Do not focus on tiny faults
Management:[1]
- It can be helpful to use specific manual techniques to mobilise restricted areas, but this will not result in macro changes
- Postural adjustments can, however, be used to change systems and make macro changes
- Thoracic rotation is essential for movement, sports and performance
- Utilise exercises that promote rotation, stability (motor control) and strength
- Exercise therapy should be used in conjunction with manual therapy to achieve an optimal outcome
- Management should not just focus on thoracic stiffness - it is perhaps more important to address thoracic motor control and segmental stability
References[edit | edit source]
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 1.16 1.17 1.18 Bell-Jenje T. Assessment and Treatment of the Thoracic Spine Course. Plus , 2021.
- ↑ Alvarez A, Tiu TK. Enthesopathies. [Updated 2021 Jul 18]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK559030/
- ↑ Martey C. Co-morbidities within Spondyloarthritis Course. Plus , 2020.
- ↑ Finucane LM, Downie A, Mercer C, Greenhalgh SM, Boissonnault WG, Pool-Goudzwaard AL et al. International framework for red flags for potential serious spinal pathologies. J Orthop Sports Phys Ther. 2020;50(7):350-72.
- ↑ Czaprowski D, Stoliński Ł, Tyrakowski M, Kozinoga M, Kotwicki T. Non-structural misalignments of body posture in the sagittal plane. Scoliosis Spinal Disord. 2018;13:6.
- ↑ Jones MR, Prabhakar A, Viswanath O, Urits I, Green JB, Kendrick JB et al. Thoracic outlet syndrome: a comprehensive review of pathophysiology, diagnosis, and treatment. Pain Ther. 2019;8(1):5-18.
- ↑ Li N, Dierks G, Vervaeke HE, Jumonville A, Kaye AD, Myrcik D et al. Thoracic outlet syndrome: a narrative review. J Clin Med. 2021;10(5):962.
- ↑ John Gibbons. Upper Limb Tension Test (ULTT) for the Median Nerve (C5-T1 Brachial plexus). Available from: https://www.youtube.com/watch?v=fhsrNKWVh0s [last accessed 4/9/2021]
- ↑ John Gibbons. Upper Limb Tension Test - Radial Nerve (C5-T1 Brachial Plexus). Available from: https://www.youtube.com/watch?v=VngRTMhAlGE [last accessed 4/9/2021]
- ↑ Wilke HJ, Herkommer A, Werner K, Liebsch C. In vitro analysis of the segmental flexibility of the thoracic spine. PLoS One. 2017;12(5):e0177823.
- ↑ Haack M, Simpson N, Sethna N, Kaur S, Mullington J. Sleep deficiency and chronic pain: potential underlying mechanisms and clinical implications. Neuropsychopharmacology. 2020;45(1):205-16.
- ↑ Takatalo J, Leinonen T, Rytkönen M, Häkkinen A, Ylinen J. The effect of thoracic spine manipulation on thoracic spine pain and mobility – Preliminary results of RCT. Manual Therapy. 2016;25:e161.
- ↑ Henson B, Kadiyala B, Edens MA. Anatomy, Back, Muscles. [Updated 2021 Aug 10]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK537074/
- ↑ Heneghan NR, Gormley S, Hallam C, Rushton A. Management of thoracic spine pain and dysfunction: A survey of clinical practice in the UK. Musculoskelet Sci Pract. 2019;39:58-66.