Anterior Cruciate Ligament (ACL)
Original Editor - Rachael Lowe
Top Contributors - Laura Ritchie, Admin, Kim Jackson, Rujuta Naik, Evan Thomas, Bruno Serra, Joao Costa, 127.0.0.1, Scott Buxton, George Prudden, WikiSysop, Vidya Acharya, Rucha Gadgil and Ewa Jaraczewska Tarang Jai
Introduction[edit | edit source]
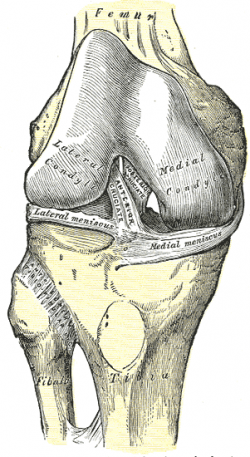
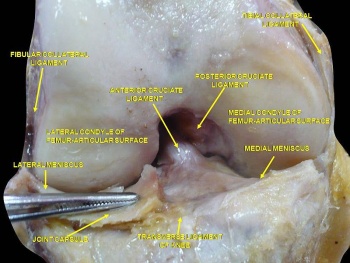
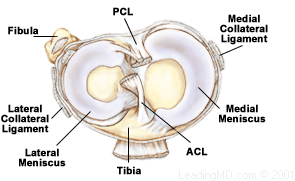
The anterior cruciate ligament (ACL) is a band of dense connective tissue which courses from the femur to the tibia. It consists of type I (90%) and type III collagen[1]. The length of ACL ranges from 27 to 38 mm and the width from 10 to 12 mm. The cross-section area measures approximately 44 mm sq[1]. It represents an hourglass or bowtie shape. The ACL is a key structure in the knee joint, as it resists anterior tibial translation and internal rotational loads as well as valgus angulation.
|
|
Attachments[edit | edit source]
Origin[edit | edit source]
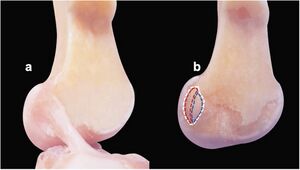
Originates from the tibial plateau between and anterior to the intercondylar eminences.[2]. This femoral attachment of ACL is on posterior part of medial surface of the lateral condyle well posterior to the longitudinal axis of the femoral shaft. The attachment is actually an interdigitation of collagen fibres & rigid bone through the transitional zone of fibrocartilage and mineralized fibrocartilage[3].
Orientation[edit | edit source]
It runs inferiorly, medially and anteriorly.
Insertion[edit | edit source]
It inserts on the lateral intercondylar ridge (also known as the resident's ridge) and the lateral bifurcate ridge (also known as the cruciate ridge) on the lateral femoral condyle.[4] Both the medial and lateral intercondylar tubercles of the tibia serve as the attachment points for the two anteromedial and posterolateral bundles of the ACL.[2].
For more detail on the anatomy of the ACL, please see this page: Anterior Cruciate Ligament (ACL) - Structure and Biomechanical Properties
Nerve Supply[edit | edit source]
The ACL receives nerve fibres from the posterior articular branches of the tibial nerve. [5] These fibres penetrate the posterior joint capsule and run along with the synovial and periligamentous vessels surrounding the ligament to reach as far anterior to the infrapatellar fat pad.[5] Most of the fibres are associated with the endoligamentous vasculature and have a vasomotor function. The receptors of the nerve fibres mentioned are as follows:
- Ruffini receptors are sensitive to stretching and are located at the surface of the ligament, predominantly on the femoral portion where the deformations are the greatest. [6]
- Vater–Pacini receptors are sensitive to rapid movements and are located at the femoral and tibial ends of the ACL. [6]
- Golgi-like tension receptors are located near the attachments of the ACL as well as at its surface, beneath the synovial membrane. [5]
- Free-nerve endings function as nociceptors, but they may also serve as local effectors by releasing neuropeptides with vasoactive function. Thus, they may have a modulatory effect in normal tissue homeostasis or in the late remodelling of grafts. [6][7]
The mechanoreceptors cited above (Ruffini, Pacini, and Golgi-like receptors) have a proprioceptive function and provide the afferent arc for signalling knee postural changes. Deformations within the ligament influence the output of muscle spindles through the fusimotor system. [7] Hence, activation of afferent nerve fibres in the proximal part of the ACL influences motor activity in the muscles around the knee; a phenomenon called the ‘‘ACL reflex.’’ These muscular responses are elicited by stimulation of group II or III fibres (i.e. mechanoreceptors). The ACL reflex is an essential part of normal knee function and is involved in the updating of muscle programs.[8] This becomes even more obvious in patients with a ruptured ACL, where the loss of feedback from mechanoreceptors in the ACL leads to quadriceps femoris weakness.[8] Indeed, this afferent feedback from the ACL has a major influence on the maximal voluntary contraction exertion of the quadriceps femoris. [9]
Vascular Supply[edit | edit source]
| [10] |
The major blood supply of the cruciate ligaments arises from the middle genicular artery. Additionally, the inferior genicular arteries and diffusion through the synovial sheath of the ACL also contribute to the overall process.[2] [11] The AMB and PLB are separated by a connective tissue septum that contains vascular stem cells. This membrane has periligamentous vessels that penetrate the ligament horizontally and connect with a longitudinal network of endoligamentous vessels that supply blood to the ACL.[12] The density of blood vessels within the ligaments is not homogeneous.[13] In the ACL, an avascular zone is located within the fibrocartilage of the anterior part where the ligament faces the anterior rim of the intercondylar fossa.[13] The coincidence of poor vascularity and the presence of fibrocartilage is also seen in gliding tendons in areas that are subjected to compressive loads, and the coincidence of these two factors undoubtedly plays a role in the poor healing potential of the ACL. [14]
Bundles[edit | edit source]
| [15] |
For a longer period of time, only two bundles of ACL were identified. However, recent studies suggest that there are three components of the ACL, the smaller anteromedial bundle (AMB), the intermediate bundle and the larger posterolateral bundle (PLB) [16]. The AMB and the PMB are distinguished by a tissue sheath in between them and their differing insertion sites.[2]
The anteromedial bundle is tight in flexion whereas the posterolateral bundle is stretched in extension. In extension both bundles are parallel. In flexion, the femoral insertion site of the posterolateral bundle moves anteriorly, both bundles are crossed, the anteromedial bundle tightens and the posterolateral bundle loosens.
With the knee extended, resistance to anterior translation of the tibia, Lachmans Test, is by the bulky posterolateral bundle. With the knee flexed, resistance to anterior translation of the tibia, the Anterior Drawer Test, is by the anterior medial bundle.
Rupture of the posterolateral bundle causes an increase in hyperextension, anterior translation (extended knee), increase in external and internal rotation (knee extended), and increases in external rotation with the knee in mid-flexion; Rupture of the anteromedial bundle causes anterolateral instability with an increase in anterior translation in flexion, minimal increase in hyperextension, and minimal rotational instability.
For more detail on the ACL bundles, please see this page: Anterior Cruciate Ligament (ACL) - Structure and Biomechanical Properties
Function[edit | edit source]
The ACL provides approximately 85% of the total restraining force of anterior translation. It also prevents excessive tibial medial and lateral rotation, as well as varus and valgus stresses. To a lesser degree, the ACL checks extension and hyperextension. Together with the posterior cruciate ligament (PCL), the ACL guides the instantaneous center of rotation of the knee, therefore controlling joint kinematics. While the anteromedial bundle is the primary restraint against anterior tibial translation, the posterolateral bundle tends to stabilize the knee near full extension, particularly against rotatory loads[17].
Video[edit | edit source]
Presentations[edit | edit source]
 |
Anterior Cruciate Ligament Injury
This presentation, created by Terdsak Rojsurakitti, Doctor at Managed Care, discusses anatomy, mechanism of injury, surgical options and rehabilitation of ACL tears. Anterior Cruciate Ligament Injury/ View the presentation |
References[edit | edit source]
- ↑ 1.0 1.1 Avalos RM, Torres-González EM, Padilla-Medina JR, Monllau JC. ACL ANATOMY: IS THERE STILL SOMETHING TO LEARN?. Revista Española de Cirugía Ortopédica y Traumatología. 2023 Feb 12.
- ↑ 2.0 2.1 2.2 2.3 Hassebrock JD, Gulbrandsen MT, Asprey WL, Makovicka JL, Chhabra A. Knee ligament anatomy and biomechanics. Sports medicine and arthroscopy review. 2020 Sep 1;28(3):80-6.
- ↑ Wheeless, C,R. Wheeless' Textbook of Orthopaedics. http://www.wheelessonline.com/ortho/anatomy_of_acl Accessed 8/1/12.
- ↑ Schillhammer CK, Reid III JB, Rister J, Jani SS, Marvil SC, Chen AW, Anderson CG, D'Agostino S, Lubowitz JH. Arthroscopy up to date: anterior cruciate ligament anatomy. Arthroscopy: The Journal of Arthroscopic & Related Surgery. 2016 Jan 1;32(1):209-12.
- ↑ 5.0 5.1 5.2 Kennedy JC, Alexander IJ, Hayes KC. Nerve supply of the human knee and its functional importance. Am J Sports Med. 1982 Nov-Dec;10(6):329-35.
- ↑ 6.0 6.1 6.2 Haus J, Halata Z. Innervation of the anterior cruciate ligament. Int Orthop. 1990;14(3):293-6.
- ↑ 7.0 7.1 Hogervorst T, Brand RA. Mechanoreceptors in joint function. J Bone Joint Surg Am. 1998 Sep;80(9):1365-78.
- ↑ 8.0 8.1 Konishi Y, Fukubayashi T, Takeshita D. Possible mechanism of quadriceps femoris weakness in patients with ruptured anterior cruciate ligament. Med Sci Sports Exerc. 2002 Sep;34(9):1414-8.
- ↑ Konishi Y, Suzuki Y, Hirose N, Fukubayashi T. Effects of lidocaine into knee on QF strength and EMG in patients with ACL lesion. Med Sci Sports Exerc. 2003 Nov;35(11):1805-8.
- ↑ Dr. Bertram Zarins, MD. Knee Ligament Anatomy Animation. Available from: http://www.youtube.com/watch?v=RTV5Yo3E7VQ[last accessed 04/10/14]
- ↑ Markatos K, Kaseta MK, Lallos SN, Korres DS, Efstathopoulos N. The anatomy of the ACL and its importance in ACL reconstruction. European Journal of Orthopaedic Surgery & Traumatology. 2013 Oct;23:747-52.
- ↑ Irarrázaval S, Albers M, Chao T, Fu FH. Gross, arthroscopic, and radiographic anatomies of the anterior cruciate ligament: foundations for anterior cruciate ligament surgery. Clinics in sports medicine. 2017 Jan 1;36(1):9-23.
- ↑ 13.0 13.1 Petersen W, Tillmann B. Structure and vascularization of the cruciate ligaments of the human knee joint. Anat Embryol (Berl). 1999 Sep;200(3):325-34.
- ↑ Giori NJ, Beaupré GS, Carter DR. Cellular shape and pressure may mediate mechanical control of tissue composition in tendons. J Orthop Res. 1993 Jul;11(4):581-91.
- ↑ Non-Contact ACL Injury, Treatment and Rehabilitation Animation. The Normal Function of the Anterior Cruciate Ligament. Available from: http://www.youtube.com/watch?v=RwwxtD-xT4Y[last accessed 04/10/14]
- ↑ MacKay JW, Whitehead H, Toms AP. Radiological evidence for the triple bundle anterior cruciate ligament. Clinical Anatomy. 2014 Oct;27(7):1097-102.
- ↑ Petersen W, Zantop T. Anatomy of the anterior cruciate ligament with regard to its two bundles. Clin Orthop Relat Res. 2007 Jan;454:35-47