Agnosia
Top Contributors - Manisha Shrestha, Niha Mulla, Rucha Gadgil and Aminat Abolade
Introduction[edit | edit source]
Agnosia (in greek gnosis- "not knowing") is a neurological condition in which a patient is unable to recognize and identify objects, persons, or sounds using one or more of their senses in spite of normally functioning senses.[1] It is a sensory disorder as person is unable to process sensory information.
Less than 1% of all neurological patients have agnosia and pure form of agnosia is rare. Visual agnosia is the most common and better-explained type of agnosia.[2]
Pathophysiology of Agnosia[edit | edit source]
To analysis something by our brain, first of all we need to have sensory stimulus (vision, hearing, taste, touch and smell). These sensory stimulus are then taken to our sensory cortex by our afferent/sensory pathway. As it is processed by higher order centers, meaning is attributed to percepts, and information becomes multi-modal. Perceptual processing is necessary to identify what is being perceived through the various sensory modalities thus allowing access to semantic knowledge and through this understanding of the environment. Semantic memory comprises knowledge of facts, concepts, and language, stored without corresponding information about the initial learning experience.
For example, if standing in the path of an oncoming bus, basic perception will involve visual information, hearing the bus coming, and feeling vibration from the ground. These separate tributes then come together, accessing relevant semantic knowledge and thus allowing the individual to understand what is taking place.[4]
Agnosia was first described by the German neurologist Lissauer in 1980 who hypothesized that object recognition occurred on two consequential levels of analysis. First being the perceptual level, in which the integration of elementary sensory data takes place in the complex forms and in second (associative), there is a comparison between what is perceived and the knowledge stored in memory.[5]But the deficits are not due to memory loss.
Clinically Relevant Anatomy[edit | edit source]
To understand the pathophysiology of agnosia, it is necessary to understand about sensory cortex, sensory relay center, sensory pathways and also memory and attention center.
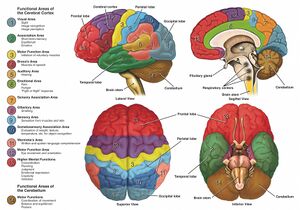
Parietal cortex is mainly responsible for processing and integrating somatosensory inputs. Occipital lobe is for vision and temporal for hearing.
Etiology[edit | edit source]
Agnosia happens when there is brain damage along pathways that connect primary sensory processing areas. These areas typically include the posterior parietal cortex and occipitotemporal regions.[2]
It occurs in various neurological conditions such as strokes, tumors, infections, dementia, hypoxia, toxins such as carbon monoxide poisoning, head injury, developmental disorders, and other neurological disorders.
Types of Agnosia[edit | edit source]
There are 2 forms of agnosia based on causes: apperceptive and associative.
- Apperceptive agnosia: It is a failure in recognition due to deficits in the early stages of perceptual processing.
- Associative agnosia: It is a failure in recognition despite no deficit in perception. Associative agnosia patients can typically draw, match or copy objects but couldn't recognize while apperceptive agnosia patients cannot.
There are 3 main types of agnosia, based on the type of sensation involved.
- Visual (vision)
- Auditory (hearing)
- Tactile (touch)
Visual Agnosia[edit | edit source]
Visual agnosia refers to an impairment in recognizing visually presented objects, despite otherwise normal visual field, acuity, color vision, brightness discrimination, language, and memory. Patients can recognize objects using other sensory modalities.
Visual agnosia is further divided in 2 subtypes: apperceptive visual agnosia and associative visual agnosia.
- Apperceptive visual agnosia: an abnormality in visual perception and discriminative process, despite the absence of elementary visual deficits. These people are unable to recognize objects, draw, or copy a figure. They cannot perceive correct forms of the object, although knowledge of the object is intact. It is typically associated with lesions to the parietal, occipital cortex.
- Associative visual agnosia: difficulty with understanding the meaning of what they are seeing. They can draw or copy but do not know what they have drawn. They correctly perceive the form and know the object when tested with verbal or tactile information, but cannot identify the object. They are unable to link the fully perceived visual stimulus to prior experience to help them recognize the stimulus. It is usually associated with damage to the bilateral inferior occipitotemporal cortex.
Types of Visual Agnosia
- Prosopagnosia is the inability to recognize familiar faces. Patients can often identify other aspects like gender, hair, emotions. Prosopagnosia results from damage to fusiform face area (located in the inferior temporal cortex in fusiform gyrus).
- Simultanagnosia is the inability to recognize and sort out objects when they appear together, but they can recognize them when they appear alone. Patients are unable to perceive the overall meaning of a picture or multiple things together, although they can describe isolated elements. Two forms of simultagnosia have been explained.
- Dorsal simultagnosia: Patients cannot see more than one object at a time. For example, when presented with a picture with a table, chair and flower vase, they may report only one thing at a time. When their attention is diverted to the other thing, they can then identify only that thing; other things disappear to them. They often have difficulty reading as it involves viewing more than one word at a time. They often bump into objects that are close together. Dorsal simultagnosia is typically associated with lesions in the bilateral occipitotemporal cortex.
- Ventral simultagnosia: These individuals also cannot identify more than one object or complex objects at one time, although they can see more than one object at a time. They are unable to perceive the whole picture as one and derive a meaning out of it. For example, in a night sky picture with stars and full moon, they may identify the moon as a ball, unable to derive the meaning of the whole picture. Ventral simultagnosia is associated with lesions in the left inferior occipital area.
3. Color agnosia is the inability to identify and distinguish colors, despite intact basic color vision and brightness discrimination mechanisms. Usually, it occurs following lesion in the left occipitotemporal region of the brain.
4. Topographical agnosia is the inability to orient to surroundings because of the inability to interpret the spatial information. These patients have a good memory of the layout and specifics of the places well known to them, but they are unable to navigate their way through. It is associated with a lesion in the right posterior cingulate area of the brain.
5. Finger agnosia is a difficulty in naming and differentiating among the fingers of either hand as well the hand of others. It does not refer to the inability to identify a finger as a finger. Gerstmann syndrome which includes acalculia, agraphia, finger agnosia, and left-right disorientation.
6. Akinetopsia refers to the inability to perceive motion.
7. Agnostic alexia refers to the inability to recognize words visually. They can still write and talk without difficulty.[1]
Auditory Agnosia[edit | edit source]
It is an inability to recognize sounds despite intact hearing. It is typically associated with right side temporal lesions.
Types of Auditory Agnosia
- Phonagnosia is the inability to recognize familiar voices. They can recognize words spoken by others. It is caused by damage to certain parts of the sound association region.
- Verbal auditory agnosia or pure word deafness is the inability to comprehend spoken words but can read, write, and speak in a relatively normal manner.
- Nonverbal auditory agnosia is the inability to comprehend nonverbal sounds and noises, with sparing of speech comprehension.
- Amusia is the inability to recognize the music. They are unable to comprehend that certain types of sounds represent music and therefore cannot distinguish music from other sounds.[1]
Tactile Agnosia[edit | edit source]
Tactile agnosia refers to the inability to recognize objects by touch. They can name objects visually.
- Asterognosis is the inability to identify the size and shape of objects by touch, for example, a triangle or square. It is also known as "Somatosensory agnosia". Astereognosis may also be defined as the impairment of recognition of the objects by somatosensory discrimination of the size, texture, weight, and shape of the objects, in the absence of any major somatosensory deficit. Manual stereognosis requires the dorsal column-medial lemniscus tract (DCMLT) to receive discriminative touch and proprioceptive information, and the parietal cortex to process the information. So damage in parietal or DCMLT can lead to asterognosis. It can be further divided into primary and secondary recognition deficits.[8]
- Anosognosia is a lack of ability to perceive the realities of one's own condition.[10]
Asomatoagnosia[edit | edit source]
It is characterized as loss of recognition or awareness of part of the body schemes. Most often, only one half of the body (usually the left) is affected which is called as hemiasomatognosia.[12]
How to diagnose agnosia?[edit | edit source]
History is key to diagnose agnosia. A detailed interview with the patient, family members, and caregivers helps to identify etiology and also difficulty in activities of daily living. For instance, Patients with simultagnosia will often have trouble reading and writing and interpreting multiple things at a time.
Neurological assessment should be performed thoroughly as diagnosing agnosia is ruling out alternative explanations. Agnosia can be diagnosed only in the absence of aphasia, generalized dementia, delirium, or any deficit that may impair some or all of the information-processing steps involved in object recognition.[2]
Management[edit | edit source]
Multidisciplinary team is needed to treat patient with agnosia.
For neuropsychological rehabilitation, two approaches can be used.[13]
- The first type, restoration, aims to improve a particular function by training the impaired function and thereby the damaged brain structure directly and repetitively.
- The second type, compensation, refers to using an intact sensory function to compensate for the loss of the other one. Thus, the impaired function itself is not targeted, but functioning on an activity and participation level is rather attempted to be improved.[13]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 Kumar A, Wroten M. Agnosia. 2020 Nov 1. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 Jan–. PMID: 29630208.
- ↑ 2.0 2.1 2.2 Kumar A, Wroten M. Agnosia. 2018
- ↑ Agnosia. Available from: https://www.youtube.com/watch?v=0E6eHKrYs6k last assessed: 29th July 2021
- ↑ Greene JD. Apraxia, agnosias, and higher visual function abnormalities. Journal of Neurology, Neurosurgery & PsychiatryGreene JD. Apraxia, agnosias, and higher visual function abnormalities. Journal of Neurology, Neurosurgery & Psychiatry. 2005 Dec 1;76(suppl 5):v25-34.. 2005 Dec 1;76(suppl 5):v25-34.
- ↑ Perrotta G. Agnosia: Definition, clinical contexts, neurobiological profiles and clinical treatments. Archive of Gerontology and Geriatrics Research. 2020 Jul 17;5(1):031-5.
- ↑ Finger agnosia. Available from: https://www.youtube.com/watch?v=m7RGLEextMY Laasted accessed :29th July 2021
- ↑ Visual Agnosia.Available from: https://www.youtube.com/watch?v=ze8VVtBgK7A lasted accessed: 29th July 2021
- ↑ Unnithan AK, Emmady PD. Astereognosis. StatPearls [Internet]. 2020 Jul 15.
- ↑ What is ASTEREOGNOSIS? What does ASTEREOGNOSIS mean? ASTEREOGNOSIS meaning & explanation. Available from:https://www.youtube.com/watch?v=_pW44HyYOnE Lasted accessed: 29th July 2021
- ↑ Acharya AB, Sánchez-Manso JC. Anosognosia.2018
- ↑ Anosognosia. Available from: https://www.youtube.com/watch?v=i4SSiS-a4js lasted accessed : 29th July 2021
- ↑ Saetta G, Zindel-Geisseler O, Stauffacher F, Serra C, Vannuscorps G, Brugger P. Asomatognosia: Structured Interview and Assessment of Visuomotor Imagery. Frontiers in Psychology. 2020;11.
- ↑ 13.0 13.1 Heutink J, Indorf DL, Cordes C. The neuropsychological rehabilitation of visual agnosia and Balint’s syndrome. Neuropsychological rehabilitation. 2019 Nov 26;29(10):1489-508.