Myofascial Pain Evaluation and Treatment
Top Contributors - Carin Hunter, Jess Bell, Kim Jackson, Merinda Rodseth and Tarina van der Stockt
Myofascial Pain Symptoms[edit | edit source]
The following symptoms are typically associated with myofascial pain:[1]
- Sore spots that are sensitive to pressure - there are primarily located in muscles
- Dull, aching, and nagging pain
- Deep muscle pain rather than joint pain
- Limbs may feel slightly weak, heavy, and stiff
- Pain is mostly in a specific area and it has a clear epicentre
- Patients often want a massage, but find that it only relieves symptoms temporarily
- Patients tend to find hot showers and baths relieving (at least for a short time)
- Patients usually find activity and exercise helps reduce symptoms
- Pain is not strongly associated with movement
- There is no clear mechanism of injury, however symptoms are often aggravated by extreme positions, exercise, or temperature
- Pain is mostly episodic, but each episode might last a long period of time (i.e. weeks / months)
- Pain can shift around, even to the contralateral side of the body - this is a less common symptom of trigger points
Myofascial Treatment Techniques[edit | edit source]
- Instrument assisted soft tissue mobilization (IASTM)
- Trigger point release
- Selective functional movement assessment (SMFA)
- Kinesiotaping
- Dry needling
- Foam Rolling
- Exercises
1. Instrument Assisted Soft Tissue Mobilization (IASTM)[edit | edit source]
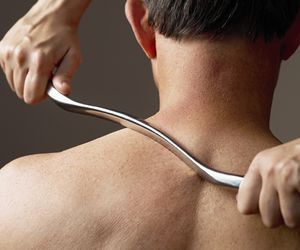
Instrument assisted soft tissue mobilization (IASTM) is a widely known and acknowledged treatment for myofascial restriction. It makes use of specially designed instruments in order to mobilise scar tissue and myofascial adhesions.[2] One example of IASTM is the Graston® technique (see Figure 1).[2] Other tools/companies include: Técnica Gavilán®, Hawk Grips®, Functional and Kinetic Treatment and Rehab (FAKTR)®, Adhesion Breakers® and Fascial Abrasion Technique™.[2]
These IASTM instruments have a mechanical advantage for the clinician and enable them to penetrate further into the tissue. It is proposed that using instruments to achieve soft tissue mobilisation might increase "vibration sense" for both the therapist and client.[2] This may enhance the therapist's ability to notice changes in tissue property (e.g. tissue adhesions) while also increasing the client's awareness of any changes in sensation in their tissues.[2][3] [4]
As is summarised by Cheatham et al.,[2] it is believed that IASTM is able to:
- Stimulate connective tissue remodelling through the resorption of excessive fibrosis
- Induce repair and regeneration of collagen in response to the recruitment of fibroblasts
This leads to the release and breakdown of:
- Scar tissue
- Adhesions
- Fascial restrictions
Cheatham et al.[2] conducted a systematic review to appraise the evidence for IASTM:
- Seven randomised controlled studies were included in the review
- Five studies compared IASTM with a control or alternative intervention for participants with a musculoskeletal condition
- The studies showed insignificant differences (p>.05) - i.e. both the control and study groups had equal outcomes
- Two studies found that IASTM resulted in significant (p<.05) short-term (i.e. up to 24 hours) joint range of motion gains when compared to a control or alternative intervention[2]
The Graston® technique[edit | edit source]
As is summarised in Cheatham et al.,[2] the Graston® technique's treatment protocol has several components:
- Examination
- Warm-up
- IASTM treatment (e.g. 30–60 seconds per lesion)
- Stretching post-treatment
- Strengthening
- Ice (when subacute inflammation is of concern)
As per the Graston Technique® website:[5]
"Graston Technique® (GT) is a unique, evidence-based form of instrument-assisted soft tissue mobilization that enables clinicians to effectively and efficiently address soft tissue lesions and fascial restrictions resulting in improved patient outcomes. GT uses specially designed stainless steel instruments with unique treatment edges and angles to deliver an effective means of manual therapy. The use of GT instruments, when combined with appropriate therapeutic exercise, leads to the restoration of pain-free movement and function. The instruments also are used diagnostically to assess the kinetic chain, in an efficient manner using the principles of regional interdependence."
Effects of the Graston® technique[edit | edit source]
According to Graston® Technique,[5] there is empirical and anecdotal evidence to suggest that this technique has the following benefits:
- "Separates and breaks down collagen cross-links, and splays and stretches connective tissue and muscle fibers
- Facilitates reflex changes in the chronic muscle holding pattern (inhibition of abnormal tone/guarding leading to pain reduction via improved sensory input)
- Alters/inhibits spinal reflex activity (facilitated segment)
- Increases the rate and amount of blood flow to and from the area (angiogenesis vs. immediate local increases in blood flow)
- Increases cellular activity in the region, including fibroblasts and mast cells
- Increases histamine response secondary to mast cell activity"
Conditions treated with the Graston® technique[edit | edit source]
This list of conditions is provided on the Graston® Technique website:[5]
- Achilles tendinitis/tendinosis
- Carpal tunnel syndrome
- Cervicothoracic sprain/strain
- Fibromyalgia
- Lateral epicondylitis/epicondylosis (tennis elbow)
- Lumbosacral sprain/strain
- Medial epicondylitis/epicondylosis (golfer's elbow)
- Myofascial pain syndromes
- Patellofemoral disorders
- Plantar fasciitis/plantar heel pain
- Post surgery (dependent on the post-surgical protocol)
- Rotator cuff tendinitis/tendinosis
- Scar tissue/post-surgical scars (once closed)
- Patients who have central and/or peripheral sensitisation (light stroking/brushing mode is used to help with desensitisation)
- Shin splints
- Trigger finger
- Women's health issues (e.g. post-mastectomy and Caesarean scarring)
2. Trigger Point Release[edit | edit source]
Primary vs Secondary Trigger Points[edit | edit source]
- Primary or central trigger points: trigger points at the centre of the muscle belly where the motor endplate goes into the muscle.[6] They are caused by an acute or chronic overloading of the involved muscle. They are not activated because of the action of other muscles.[7]
- Secondary or satellite trigger points: A trigger point that arises in response to primary trigger points in surrounding muscles.[7] They usually spontaneously resolve when the central trigger point is healed, but they can form a cluster.
Trigger Point Types[edit | edit source]
- Active trigger points: A point that causes tenderness or referred pain on palpation / direct pressure. Pain is continuous and there is reduced muscle elasticity / weakness.[7] Most central and some satellite trigger points are active. Trigger point irritability determines pain intensity and extension.[7]
- Inactive or latent trigger points: Lumps / nodules that feel like trigger points.[6] They have the same features as active trigger points, but are less severe. The pain is not constant, but rather induced (e.g. on palpation).[7] They are described as a "foci of hyperirritability in a taut band of muscle" and tend to be associated with tenderness, a local twitch response and / or referred pain on palpation.[8] Latent trigger points can be activated and become active trigger points.[8]
- Diffuse Trigger Points: Commonly happen in individuals who have a severe postural deformity and when an entire body quadrant is involved.[6] Secondary trigger points are labelled as "diffuse trigger points" when there are multiple satellite trigger points which develop in response to central trigger points.[6]
- Attachment Trigger Points: Tendo-osseous junctions often become very tender. If not treated these can lead to or hasten degenerative processes of an adjacent joint.[6]
- Ligamentous Trigger Points: Evidence suggests that trigger points can also develop in ligaments. For instance, it has been found that trigger points in the anterior longitudinal ligament of the spine can result in neck instability.[6] Similarly, addressing trigger points in the patella ligament and fibular collateral ligament can be beneficial for knee pain syndromes.[6]
Indications of Trigger Point Therapy[edit | edit source]
- Repetitive / acute micro-trauma
- Vitamin deficiencies
- Poor posture
- Sleep disturbances
- Joint problems
- Chronic stress on muscles fibres or psychological stress
- Chronic infections
- Radiculopathy
- Depression
- Hypothyroidism
- Hyperuricemia
- Hypoglycemia[9]
Contraindications of Trigger Point Therapy[edit | edit source]
- Epilepsy
- Asthma
- Pregnancy
- Hypertension
- Patient pain tolerance
- Anxiety and stress
- Acute stage of healing or open wounds, burns
- Medical conditions such as pneumonia, kidney, liver or respiratory failure
- Diabetes with gangrene
- Haemorrhagic conditions and use of blood thinners
- Severe atherosclerosis
- Unstable hypertension
- Shock
- Contagious diseases[9]
Interventions for Trigger Point Therapy[edit | edit source]
- Modify or eliminate every day micro stressors
- Correction and training of posture, extensive patient education on lifestyle (ergonomics)
- Passive stretching techniques and/or foam roller stretching a few times per day
- Self-massage, a few times per day, especially Deep Stroking Massage, done rhythmically and in only one direction
- Strengthening: initially only isometric and then isotonic exercises
- Taping technique
- Spray and stretch technique by using ethyl chloride spray
- Manual lymphatic drainage (MLD), since the presence of trigger points can act as an obstacle to lymphatic flow
- Other proprioceptive neuromuscular techniques: Reciprocal Inhibition (RI), Post-Isometric Relaxation (PIR), Contract-Relax/Hold-Relax (CRHR), Contract-Relax/Antagonist Contract (CRAC)[9]
3. Selective Functional Movement Assessment (SMFA)[edit | edit source]
The Selective Functional Movement Assessment (SFMA) was developed by Gray Cook and colleagues.[10] They also developed the Functional Movement Systems.[11] The SFMA is a clinical model that aims to identify movement pattern dysfunctions and, thus, aid in the diagnosis and management of musculoskeletal disorders.[12]
The SFMA is a diagnostic system that can only be performed by medical professionals. The SFMA assessment is broken down into seven top tier tests. Each test result is given one of the following scores:[13]
- Functional/Painful (FP): Patient completes the movement, but has pain
- Dysfunctional/ Non-painful (DN): Patient is unable to complete movement, but does not have pain
- Dysfunctional/ Painful (DP): Patient is unable to complete the movement and has pain
- Functional/Non-painful (FN): Patient completes the movement with no pain
SFMA patterns for assessment:[13][14]
- Cervical spine patterns
- Flexion: Touch chin to chest
- Extension: Look up towards the ceiling
- Rotation with flexion: Touch chin to collar bone and repeat each side
- Upper extremity patterns
- Abduction with external rotation: Reach arm around head and attempt to touch the superior angle of the opposite scapula
- Adduction with internal rotation: Reach arm around the back and attempt to touch the inferior angle of the scapula
- Multi-segmental Flexion: Reach down and touch the toes
- Multi-segmental Extension: Reach overhead and extend as far as possible
- Multi-segmental rotation: Rotate body as far as possible to each side, keeping feet flat on the floor
- Single leg stance: Stand on one leg with the other leg held at 90 degrees of hip flexion or more for at least 10 seconds
- Overhead deep squat: Lift hands overhead, place feet approximately shoulder width apart and squat down as far as possible while keeping the feet on the floor
Example: Overhead squat and upper extremity patterns
- Upper extremity patterns - abduction/external rotation and adduction/internal rotation: Can be addressed by treating the front arm and back arm lines[9][15]
- Back arm line (third tract):[14]
- Latissimus dorsi
- Thoracolumbar fascia
- Sacral fascia contralateral to thoracolumbar fascia
- Gluteus maximus contralateral to thoracolumbar fascia
- Vastus lateralis
- Front arm line (third tract):[14]
- Pectoralis major
- External oblique
- Adductor longus contralateral to external oblique
- Gracilis contralateral to external oblique
- Pes anserine contralateral to external oblique
- Tibial periosteum contralateral to external oblique
The SFMA can be used conjunction with palpation and visual observation.[14] It is important to then assess and re-assess the dysfunctional movement.[9] Please click here for more information on the upper extremity myofascial chains.
4. Kinesiotaping[edit | edit source]
Zhang et al.[16] recently conducted a systematic review and meta-analysis to assess the evidence for kinesiotaping as an intervention for myofascial pain syndrome. They included 20 randomised controlled trials with 959 participants. They found that:[16]
- Kinesiotaping was more effective at decreasing pain intensity post-intervention than other treatments
- Compared to other non-invasive techniques, kinesiotaping was superior at reducing pain intensity at follow-up
- There was no identified effect on disability / function
Thus, Zhang et al.[16] concluded that there is statistical evidence to support the use of kinesiotaping to reduce pain intensity and improve range of motion in clients with myofascial pain syndrome during the post-intervention period.
5. Dry Needling[edit | edit source]
Charles et al.[17] conducted a systematic review to evaluate the effect of manual therapy techniques, dry cupping and dry needling on myofascial pain and trigger points. Eight manual therapy studies, 23 dry needling studies, and two dry cupping studies met the inclusion criteria. The authors found that:[17]
- There was a moderate number of randomised controlled trials to support the use of manual therapy
- The evidence for dry needling was very low to moderate when compared to control groups, sham treatments, and other treatments
- There was a lack of data on dry cupping
6. Foam Rolling[edit | edit source]
Kalichman and David[18] conducted a narrative review on the effect of self-myofascial release (SMFR) on myofascial pain, muscle flexibility, and strength. They found that:[18]
- Therapists and fitness professionals have, for the last 10 years, mainly used foam rolling to implement SMFR as a treatment / maintenance tool
- Joint range of motion can increase significantly after SMFR is used
- There is no decrease in muscle force or altered performance post SMFR-treatment
- SMFR is widely used by health professionals to treat myofascial pain
The authors[18] note, however, that there are no clinical trials assessing the effect of SMFR on myofascial pain.
Hughes and Ramer[19] conducted a systematic review to determine how long myofascial rolling should be applied for optimal recovery, and improvements in range of motion and performance. They found:[19]
- The "most evidence-based" benefit of myofascial rolling is decreased muscle soreness
- Seven of eight studies found that there was a short-term reduction in pain / soreness
- A minimum rolling time of 90 seconds per muscle appeared to be beneficial
- Ten of 17 studies looking at range of motion found that there were acute improvements following rolling, but results were not consistent
- There were no significant effects on performance post-rolling
Thus, the authors[19] concluded that in order to achieve short-term reductions in pain/soreness, patients should perform at least 90 seconds of myofascial rolling per muscle group (with no upper time limited found). There is, however, no research to suggest that myofascial rolling is associated with long-term improvements in performance or range of motion and the current data is insufficient to make recommendations for acute changes in range of motion.[19]
7. Exercises[edit | edit source]
The following are some exercises that can help to address myofascial pain in the upper limb:[9]
- Sit on a rolling chair: Face palms down on the table in front of you. Slide hips back until elbows are almost straight. Keep feet on the floor, pull forward using your mid back and the core
- Progression: Rest on the medial side of the palm
- Further progression: Place palms on the tennis balls and pull forwards
- Desk or wall stretch: Place palm down, roll the hip away, keeping the feet flat on the floor, rotate to the opposite direction. Turn the neck in the same direction as the trunk.
- Progression: as above, but face palm up
- Further progression: as above, but add in extension of the wrist and fingers
References[edit | edit source]
- ↑ Ingraham P. The complete guide to trigger points and myofascial pain [Internet]. Pain Science. 2021 [accessed 29 November 2021]. Available from: https://www.painscience.com/tutorials/trigger-points.php
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 2.8 Cheatham SW, Lee M, Cain M, Baker R. The efficacy of instrument assisted soft tissue mobilization: a systematic review. The Journal of the Canadian Chiropractic Association. 2016 Sep;60(3):200.
- ↑ Baker RT, Nasypany A, Seegmiller JG, Baker JG. Instrument-assisted soft tissue mobilization treatment for tissue extensibility dysfunction. International Journal of Athletic Therapy and Training. 2013 Sep 1;18(5):16-21.
- ↑ Lee JJ, Lee JJ, Kim DH, You SJ. Inhibitory effects of instrument-assisted neuromobilization on hyperactive gastrocnemius in a hemiparetic stroke patient. Bio-medical materials and engineering. 2014 Jan 1;24(6):2389-94.
- ↑ 5.0 5.1 5.2 Graston Technique®. What is Graston Technique®? Available from: https://grastontechnique.com/Patients/FAQ/ (accessed 28 November 2021).
- ↑ 6.0 6.1 6.2 6.3 6.4 6.5 6.6 Team NAT. Trigger point therapy - what are the different types of trigger point? [Internet]. NielAsher. 2017 [accessed 29 November 2021]. Available from: https://nielasher.com/blogs/video-blog/71233797-what-are-the-different-types-of-trigger-point
- ↑ 7.0 7.1 7.2 7.3 7.4 Vázquez-Delgado E, Cascos-Romero J, Gay-Escoda C. Myofascial pain syndrome associated with trigger points: a literature review. (I): Epidemiology, clinical treatment and etiopathogeny. Med Oral Patol Oral Cir Bucal. 2009;14(10):e494-8.
- ↑ 8.0 8.1 Ge HY, Arendt-Nielsen L. Latent myofascial trigger points. Curr Pain Headache Rep. 2011;15(5):386-92.
- ↑ 9.0 9.1 9.2 9.3 9.4 9.5 Pandya R. Myofascial Pain Evaluation and Treatment Course. Plus , 2021.
- ↑ Cook G Movement: Functional Movement Systems: Screening, Assessment, and Corrective Strategies. On Target Publications; Santa Cruz, CA: 2010
- ↑ Cook G, Burton L, Hoogenboom BJ, Voight M. Functional movement screening: the use of fundamental movements as an assessment of function - part 1. Int J Sports Phys Ther. 2014;9(3):396-409.
- ↑ Riebel M, Crowell M, Dolbeer J, Szymanek E, Goss D. Correlation of self-reported outcome measures and the selective functional movement assessment (SFMA): an exploration of validity. Int J Sports Phys Ther. 2017; 12(6):931-947.
- ↑ 13.0 13.1 Stanek JM, Smith J, Petrie J. Intra- and inter-rater reliability of the selective functional movement assessment (SFMA) in health participants. Int J Sports Phys Ther. 2019;14(1):107-16.
- ↑ 14.0 14.1 14.2 14.3 Ward P. SFMA and Anatomy Trains: Concepts For Assessment and Treatment [Internet]. Sports Rehab Expert [accessed 29 November 2021]. Available from: https://www.sportsrehabexpert.com/public/472.cfm
- ↑ Wilke J, Krause F, Vogt L, Banzer W. What is evidence-based about myofascial chains: a systematic review. Archives of physical medicine and rehabilitation. 2016 Mar 1;97(3):454-61.
- ↑ 16.0 16.1 16.2 Zhang XF, Liu L, Wang BB, Liu X, Li P. Evidence for kinesio taping in management of myofascial pain syndrome: a systematic review and meta-analysis. Clinical rehabilitation. 2019 May;33(5):865-74.
- ↑ 17.0 17.1 Charles D, Hudgins T, MacNaughton J, Newman E, Tan J, Wigger M. A systematic review of manual therapy techniques, dry cupping and dry needling in the reduction of myofascial pain and myofascial trigger points. Journal of bodywork and movement therapies. 2019 Jul 1;23(3):539-46.
- ↑ 18.0 18.1 18.2 Kalichman L, David CB. Effect of self-myofascial release on myofascial pain, muscle flexibility, and strength: a narrative review. Journal of bodywork and movement therapies. 2017 Apr 1;21(2):446-51.
- ↑ 19.0 19.1 19.2 19.3 Hughes GA, Ramer LM. Duration of myofascial rolling for optimal recovery, range of motion, and performance: a systematic review of the literature. International journal of sports physical therapy. 2019 Dec;14(6):845.