Treatment of Plantar Heel Pain - A Literature Review
Original Editor - Merinda Rodseth based on the course by
Bernice Saban
Top Contributors - Merinda Rodseth, Kim Jackson, Jess Bell and Tarina van der Stockt
Introduction[edit | edit source]
Plantar heel pain (PHP) is regarded as a multifactorial condition with a number of proposed associated factors.[1][2] It is generally viewed as a self-limiting condition and for the majority of individuals with PHP, the symptoms resolve within one year without any therapeutic intervention.[1][3][4] Twenty percent of individuals, however, continue to experience PHP beyond a year.[1][3]
Because the aetiology of PHP is generally not well understood, there is uncertainty about its management.[1][2] There is a lack of high quality evidence regarding optimal treatment. This leaves clinicians with a variety of treatment options, but no clear guidance on what works best and no firm, evidence-based advice about the optimal management of PHP.[3][4][5][6][7][8]
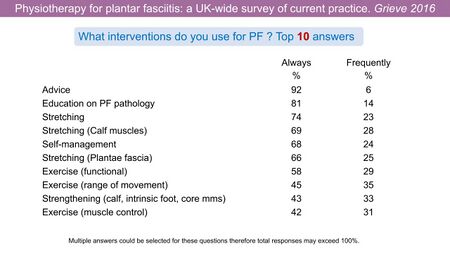
This lack of guidance prompted Grieve et al[9] to conduct a survey asking UK-based physiotherapists to identify which interventions they used to treat PHP (Figure 1).
Figure 1. Interventions used by physiotherapists in the UK for PHP [9][10]
The results of this survey highlighted the need to search the available research in order to establish which treatment options are available and effective in the management of plantar heel pain syndrome (PHPS).[10]
When considering the research, it is important to keep in mind that the term “significant difference” is a statistical value and not always reflective of a difference / change that would be meaningful for the patient. It is, therefore, also important to consider the “minimal important difference” (minimal clinically important difference / change) or the “smallest change in the treatment outcome that an individual patient would identify as important, and which would mandate a change in the patient’s management”.[10][11]
Which treatments should then be used for patients with PHPS? The physiotherapy and medical treatments shown in Figure 2 will be discussed in this review, with the aim of identifying treatment options supported by high-quality research studies.
Figure 2. Treatment options proposed for PHPS [10]
Physiotherapy Treatments[edit | edit source]
A large variety of physiotherapy treatment options for PHPS have been discussed in the literature and will be reviewed in the following section (Figure 3).
Figure 3. Physiotherapy treatment options proposed for PHPS [10]
Ultrasound[edit | edit source]
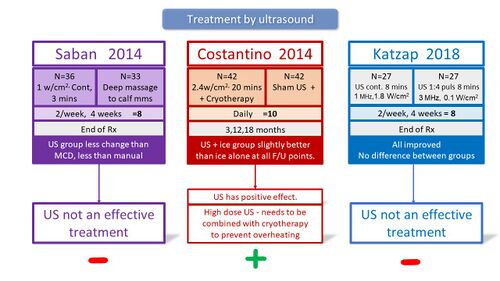
Therapeutic ultrasound is one of the electrical devices most widely used by physiotherapists despite the fact that there is not sufficient high-quality evidence to support its use in musculoskeletal conditions.[12] Many studies investigated the use of ultrasound and found therapeutic ultrasound to be ineffective for the treatment of PHP. Its use is, therefore, not recommended for individuals with PHPS (Figure 4). [12][13][14][15][16]
Figure 4. Studies investigating the treatment of PHP by ultrasound
Stretching[edit | edit source]
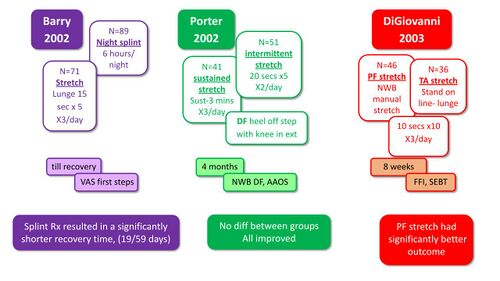
Stretching of the triceps surae muscles has been proposed in many studies as an essential part of the management of plantar fasciitis.[12] The aim of stretching is to release tension in the Achilles tendon and plantar fascia, both of which attach to the calcaneus.[12] Many studies have investigated the use of stretching for the treatment of PHPS, often with conflicting results. Several studies compared the use of various stretches for PHPS and generally found that all groups improved. Barry et al[17] also reported a shorter recovery time with the use of night splinting (Figure 5).[17][18][19]
Figure 5. Research studies comparing various stretching regimes [10][17][18][19]
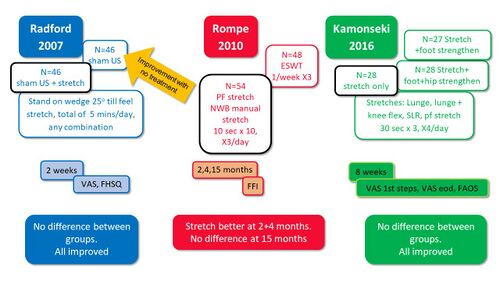
Some studies compared stretching to various other treatment interventions (sham US, ESWT, strengthening) and generally found no differences between groups, and that all groups improved. Stretching was therefore not found to be superior to other forms of treatment (Figure 6). [20][21][22]
Figure 6. Stretching compared to other forms of treatment [10][20][21][22]
In a systematic review analysing the effectiveness of manual stretching for PHPS, Sweeting et al[23] reported:
- Conflicting results
- One study showed placebo to be equally effective to stretching
- Another study showed stretch to be more effective than EWST
- Intermittent or sustained methods of stretching were equally effective
- A non-weight bearing stretch of the plantar fascia could be more effective than a weight bearing dorsiflexion stretch
Strengthening[edit | edit source]
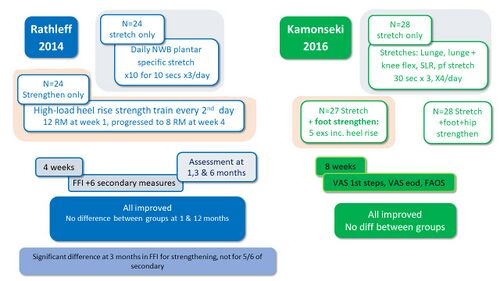
Weakness of the intrinsic foot muscles, as well as the ankle plantar flexors have been proposed as risk factors for the development of PHPS and prompted the use of strengthening as a treatment for PHPS.[8] Several studies investigated the effect of strengthening on PHPS and reported improvement in all groups with no advantage to strengthening in the management of PHPS, except after 3 months of plantar-specific strengthening (Figure 6).[22][24]
Figure 6. Effect of strengthening on PHPS [10][22][24]
Manual Therapy[edit | edit source]
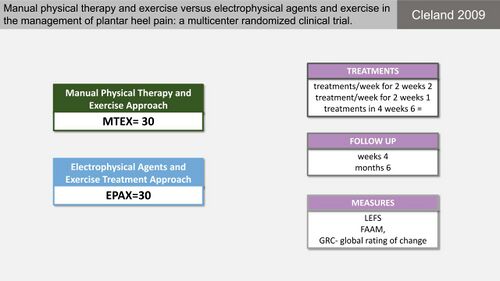
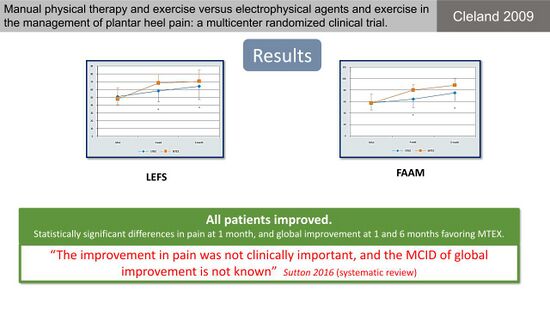
Physiotherapists often use manual therapy to improve joint mobility, mobilise soft tissue and reduce pain.[25][26] Current literature on the use of manual therapy for patients with PHP is, however, sparse and often of lesser quality.[25] Cleland et al[27] conducted a study on the efficacy of manual therapy and exercise (MTEX) compared to electro-physical agents and exercise (EPAX) in the management of PHPS (Figure 7). Both treatment groups, however, received multiple different interventions - this is problematic when attempting to interpret which intervention made the difference (Figure 8). The authors concluded that all patients improved with statistically significant differences between groups regarding pain and global improvement favouring MTEX (Figure 9).[27] There is, however, not enough information about the clinical effects of the treatment.
Figure 7. Manual therapy and exercise compared to electro-physical agents and exercise for PHPS [10][27]
Figure 8. Treatment details of the groups in the study by Cleland et al [27][10]
Figure 9. Results of the comparison between manual therapy and electro-physical agents for PHPS [10][27]
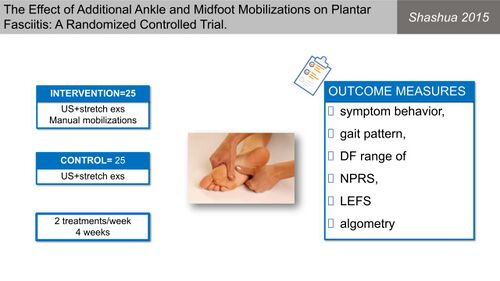
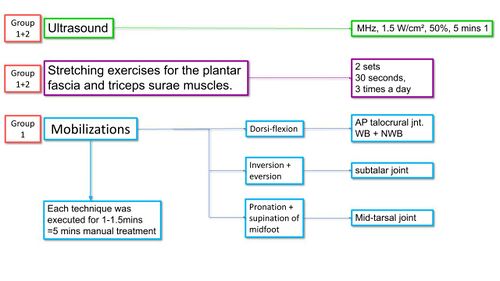
Shashua et al[28] also investigated the effect of manual therapy on plantar fasciitis (Figure 10) with the treatment group receiving manual therapy, ultrasound and stretch exercises and the control group only ultrasound and stretch exercises (Figure 11). They reported an improvement in both groups with no difference between groups, indicating no additional advantage to manual therapy for PHPS (Figure 12)[28].
Figure 10. Manual therapy for Plantar fasciitis [10][28]
Figure 11. Treatment details for both groups in the study by Shashua et al [28][10]
Figure 12. Results on the effect of manual therapy for plantar fasciitis [10][28]
Taping[edit | edit source]
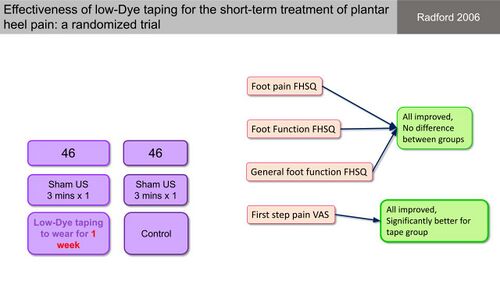
Taping is proposed to be associated with pain reduction, increased circulation and improved proprioception, all of which would be beneficial for the management of PHPS.[29] Radford et al[30] applied standardised Leukotape to the plantar skin of patients and kept it in situ for 7 days. This group was compared to a control group. Both groups improved and there was no significant reduction in heel pain intensity in the taping group compared to the controls.[3][30] First step pain, however, was significantly better in the taping group compared to the controls (Figure 13).[30]
Figure 13. Effectiveness of low-dye taping for the treatment of PHPS [10][30]
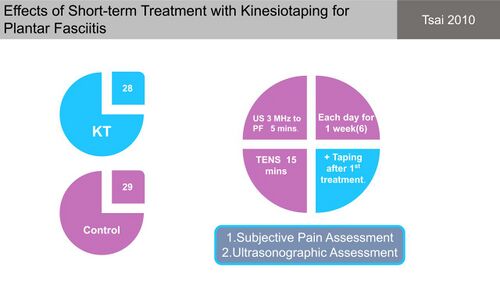
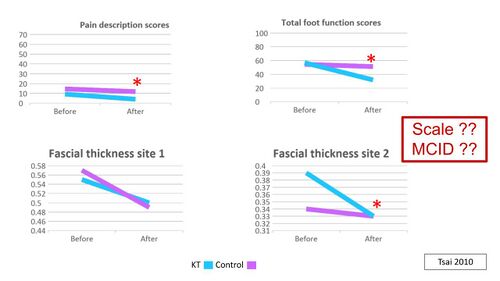
Tsai et al[29] compared the use of Kinesio tape for plantar fasciitis, applied over the gastrocnemius and plantar fascia and kept in situ for one week, to a control group (Figure 14). Both groups reported a significant reduction in pain and there was a significant difference in pain reduction between the groups, but this was also reported before the intervention. No differences in plantar fascia thickness were found between groups.[29] This study, however, had insufficient information to accurately interpret its measurements and come to a final conclusion about the treatment effects (Figure 15).[10]
Figure 14. Kinesiotaping versus control group [10][29]
Figure 15. Results of the study by Tsai et al [29][10]
Dry Needling[edit | edit source]
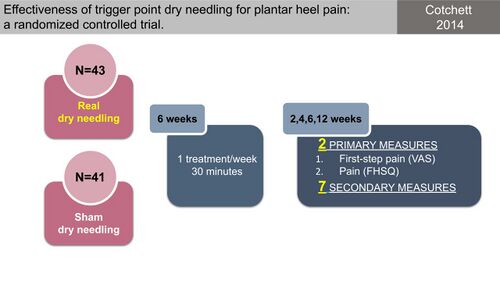
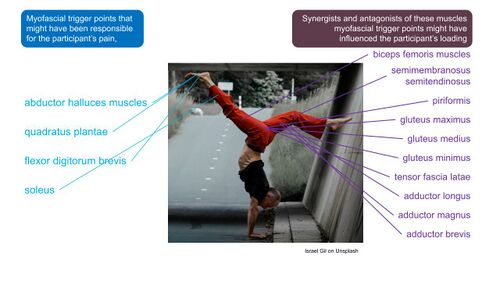
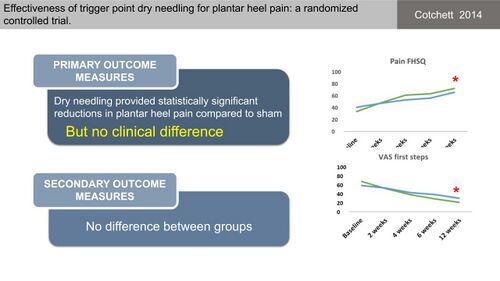
The presence of myofascial trigger points within the musculature of the plantar foot, as well as the muscles proximal to the foot, has been proposed to play a role in PHPS.[31] Dry Needling of these myofascial trigger points has, therefore, been proposed for the management of plantar fasciitis.[31][32][33] Limited evidence for the effectiveness of dry needling was, however, reported in a systematic review on dry needling for PHPS and the poor quality of the studies mean it is not possible to make definite conclusions.[33] Following this, Cotchett et al[31] conducted a study to determine the efficacy of trigger point dry needling for PHPS (Figure 16) and compared “real dry needling” into the myofascial trigger points of a variety of muscles (Figure 17) to sham dry needling. They found that even though real dry needling provided statistically significant reductions in PHP compared to sham dry needling, the size of the effect was not clinically meaningful (Figure 18).[31]
Figure 16. Effectiveness of trigger point dry needling for PHPS [10][31]
Figure 17. Different muscles in which trigger points were dry needled [10][31]
Figure 18. Outcome of real vs sham dry needling [10][31]
Cryotherapy[edit | edit source]
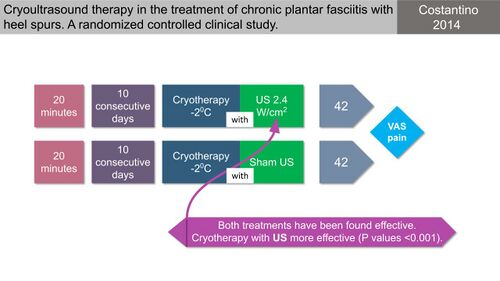
Ice/cryotherapy is generally considered as a basic component in the management of any injury due to its proposed effectiveness in reducing swelling and relieving short-term pain.[15] Thus, as for many other musculoskeletal conditions, it has also been proposed as a treatment option for PHP.[15][26] Costantino et al [15] conducted a study comparing cryoultrasound to only cryotherapy and found that all patients improved, but the ultrasound group showed a larger improvement (Figure 19).
Figure 19. Cryoultrasound vs cryotherapy for chronic plantar fasciitis [10][15]
Medical Treatments[edit | edit source]
While it varies between countries and depends on the scope of practice, many of the following treatments are often not performed by physiotherapists, but rather by medical doctors. They are mostly used after the failure of conservative management (Figure 20).
Figure 20. Proposed medical treatments for the management of PHPS [10]
Orthotics[edit | edit source]
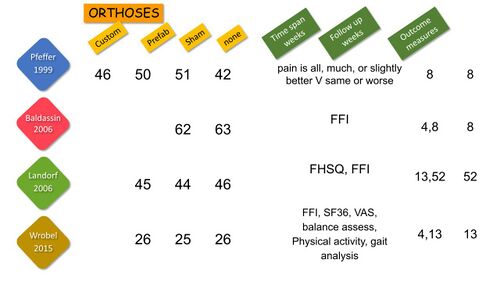
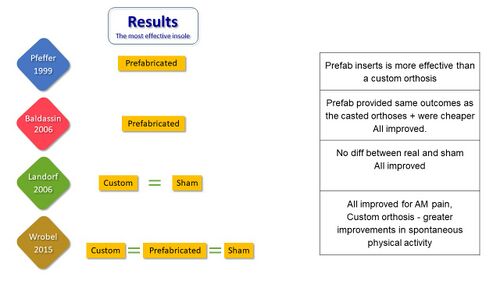
Four high-quality studies investigating the effect of a variety of foot orthoses / insoles in PHPS were identified (Figure 21 and Figure 22).[10] They provided varied and somewhat conflicting results on the efficacy of various insoles for PHPS and generally reported improvement in all groups with no consistent benefit to anyone orthosis (Figure 23).[6][34][35][36][37]
Figure 21. Good quality studies on the use of orthoses/insoles for PHPS [10]
Figure 22. Study details of the four studies on orthoses for PHPS [10][34][35][36][37]
Figure 23. Results on the most effective insole for PHPS [10]
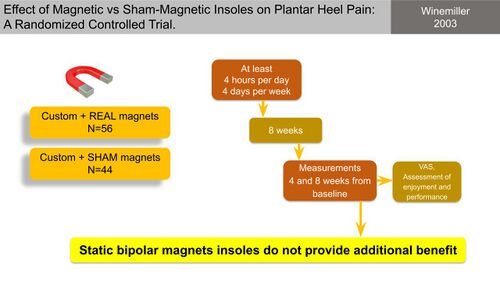
Winemiller et al [38] compared the effect of magnetic versus sham-magnetic insoles on PHP and found no benefit to magnetic insoles compared to sham-magnetic inserts (Figure 24).
Figure 24. Magnetic insoles vs sham-magnetic insoles for PHP [10][38]
Extracorporeal Shock Wave Therapy[edit | edit source]
Extracorporeal shock wave therapy (ESWT) has been used since 1976 to disintegrate kidney and gallstones (lithotripsy) and for several decades as a non-invasive pain-relief treatment option for failed conservative management of plantar fasciitis before surgical intervention.[26][39] ESWT involves an electromagnetic system where a magnetic field in a surrounding fluid medium is used to produce shock waves.[26] Abrupt, high-amplitude pulses of mechanical energy (similar to sound waves) are generated by an electromagnetic coil or a spark in water.[10] The shock waves are proposed to stimulate angiogenesis (new blood vessels) and neurogenesis (new nerve cells).[10] Its mechanism of action is still not well understood, but proposed to be through the destruction of unmyelinated nerve fibres with simultaneous stimulation of neovascularisation and collagen synthesis.[26] The cells, therefore, appear to undergo microtrauma which promotes the inflammatory and catabolic processes associated with the removal of damaged matrix waste and stimulation of wound healing mechanisms.[10] In short, ESWT should:[10]
- Increase blood supply
- Improve collagen remodelling
- Enhance waste elimination
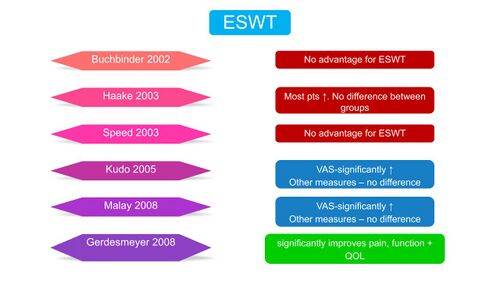
Several studies, many of poor methodological quality, explored the effect of ESWT on PHPS with conflicting results (Figure 25).
Figure 25. Evidence for the use of ESWT in PHPS [10][39][40][41][42][43][44]
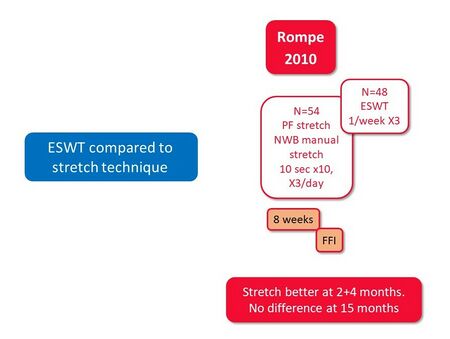
Of the studies reviewed, only Gerdesmeyer et al[40] reported a significant improvement in pain, function and quality of life with ESWT whereas others had conflicting results. Rompe et al[21] compared ESWT to stretching techniques and found stretching to be more advantageous than ESWT at 2 and 4 months (Figure 26).
Figure 26. ESWT compared to a stretching regime for PHPS [10][21]
Following the results of their systematic review, Yu et al [45] reported inconsistent evidence on the effectiveness of ESWT for PHPS and stated that the current evidence does not support the use of ESWT for PHPS.
Steroid Injections[edit | edit source]
Corticosteroid injections are used in multiple musculoskeletal conditions, including PHP, as a way of relieving pain.[26][46] In a Cochrane review, David et al [46] reported low quality evidence that local steroid injections may slightly reduce PHP for up to one month, compared to placebo or no treatment (Figure 27).
Figure 27. Cochrane review of injected corticosteroids for the treatment of PHP [10][46]
Surgery[edit | edit source]
Surgical interventions are generally not considered for plantar fasciitis until conservative treatment has been thoroughly pursued and symptoms have been present for more than 6 months.[47] Plantar fasciotomy will only be considered if conservative therapies have been ineffective and significant symptoms continue to persist.[47] Plantar fasciotomy involves:[47]
- an open procedure
- either a partial release of the medial one-third of the plantar fascia
- or a complete release of the fascia
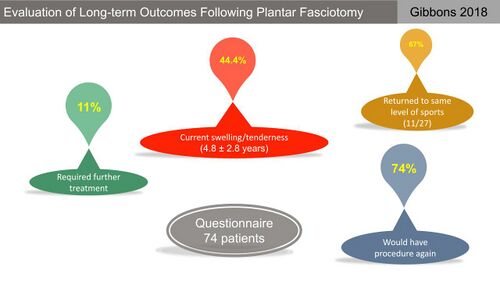
The outcomes following plantar fasciotomy vary but it generally shows good early pain relief and return to function in the short term.[47] However, many individuals experience ongoing pain and functional limitations and a retrospective study by Gibbons et al[47] demonstrated that even though 72 percent of patients reported long-term satisfaction with the surgery, 44 percent continued to experience ongoing pain, swelling and tenderness (Figure 28).
Figure 28. Long-term outcomes following plantar fasciotomy [10][47]
Conclusion[edit | edit source]
From the literature explored, it seems that stretches could possibly help for PHPS and strengthening may be beneficial, but the available evidence does not support any of the commonly used treatments for PHP as significantly better than any other.[4][13] At the moment, there is limited evidence upon which to base clinical practice,[48] which poses a professional spur for clinicians as it relates to the risk factors, assessment and management of PHPS.
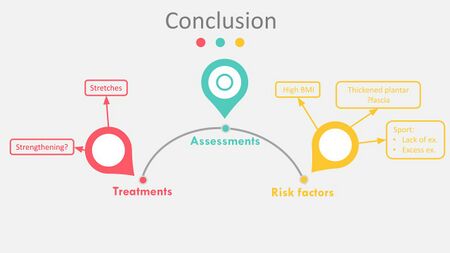
From the literature reviews on these topics in PHPS, it has been shown that there is some information on the risk factors associated with PHPS, no evidence for the assessment of PHPS and very little information on the management of PHP (Figure 29). This prompts us to the next course in this series, the pursuing of a new protocol for PHPS.[10]
Figure 29. Known variables from the literature reviews on risk factors, assessment and treatment of PHPS [10]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 Sullivan J, Pappas E, Burns J. Role of mechanical factors in the clinical presentation of plantar heel pain: implications for management. The Foot. 2020 Mar 1;42:101636. DOI:10.1016/j.foot.2019.08.007
- ↑ 2.0 2.1 Thomas MJ, Whittle R, Menz HB, Rathod-Mistry T, Marshall M, Roddy E. Plantar heel pain in middle-aged and older adults: population prevalence, associations with health status and lifestyle factors, and frequency of healthcare use. BMC musculoskeletal disorders. 2019 Dec;20(1):1-8.
- ↑ 3.0 3.1 3.2 3.3 Salvioli S, Guidi M, Marcotulli G. The effectiveness of conservative, non-pharmacological treatment, of plantar heel pain: a systematic review with meta-analysis. The Foot. 2017 Dec 1;33:57-67.
- ↑ 4.0 4.1 4.2 Babatunde OO, Legha A, Littlewood C, Chesterton LS, Thomas MJ, Menz HB, van der Windt D, Roddy E. Comparative effectiveness of treatment options for plantar heel pain: a systematic review with network meta-analysis. British journal of sports medicine. 2019 Feb 1;53(3):182-94.
- ↑ Morrissey D, Cotchett M, J'Bari AS, Prior T, Griffiths IB, Rathleff MS, Gulle H, Vicenzino B, Barton CJ. Management of plantar heel pain: a best practice guide informed by a systematic review, expert clinical reasoning and patient values. British Journal of Sports Medicine. 2021 Mar 30.
- ↑ 6.0 6.1 Rasenberg N, Bierma-Zeinstra SM, Bindels PJ, van der Lei J, van Middelkoop M. Incidence, prevalence, and management of plantar heel pain: a retrospective cohort study in Dutch primary care. British Journal of General Practice. 2019 Nov 1;69(688):e801-8.
- ↑ Whittaker GA, Landorf KB, Munteanu SE, Menz HB. Predictors of response to foot orthoses and corticosteroid injection for plantar heel pain. Journal of Foot and Ankle Research. 2020 Dec;13(1):1-9.
- ↑ 8.0 8.1 Franettovich Smith MM, Collins NJ, Mellor R, Grimaldi A, Elliott J, Hoggarth M, Weber Ii KA, Vicenzino B. Foot exercise plus education versus wait and see for the treatment of plantar heel pain (FEET trial): a protocol for a feasibility study. Journal of foot and ankle research. 2020 Dec;13:1-4. DOI: 10.1186/s13047-020-00384-1
- ↑ 9.0 9.1 Grieve R, Palmer S. Physiotherapy for plantar fasciitis: a UK-wide survey of current practice. Physiotherapy. 2017 Jun 1;103(2):193-200.
- ↑ 10.00 10.01 10.02 10.03 10.04 10.05 10.06 10.07 10.08 10.09 10.10 10.11 10.12 10.13 10.14 10.15 10.16 10.17 10.18 10.19 10.20 10.21 10.22 10.23 10.24 10.25 10.26 10.27 10.28 10.29 10.30 10.31 10.32 10.33 10.34 10.35 10.36 10.37 Saban B.Treatment of Plantar Heel Pain - A Literature Review Course. Plus. 2021.
- ↑ Cotchett M, Rathleff MS, Dilnot M, Landorf KB, Morrissey D, Barton C. Lived experience and attitudes of people with plantar heel pain: a qualitative exploration. Journal of foot and ankle research. 2020 Dec;13(1):1-9.
- ↑ 12.0 12.1 12.2 12.3 Katzap Y, Haidukov M, Berland OM, Itzhak RB, Kalichman L. Additive effect of therapeutic ultrasound in the treatment of plantar fasciitis: a randomized controlled trial. Journal of Orthopaedic & Sports Physical Therapy. 2018 Nov;48(11):847-55.
- ↑ 13.0 13.1 Martin RL, Davenport TE, Reischl SF, McPoil TG, Matheson JW, Wukich DK, McDonough CM, Altman RD, Beattie P, Cornwall M, Davis I. Heel pain—plantar fasciitis: revision 2014. Journal of Orthopaedic & Sports Physical Therapy. 2014 Nov;44(11):A1-33.
- ↑ Saban B, Deutscher D, Ziv T. Deep massage to posterior calf muscles in combination with neural mobilization exercises as a treatment for heel pain: a pilot randomized clinical trial. Manual therapy. 2014 Apr 1;19(2):102-8.
- ↑ 15.0 15.1 15.2 15.3 15.4 Costantino C, Vulpiani MC, Romiti D, Vetrano M, Saraceni VM. Cryoultrasound therapy in the treatment of chronic plantar fasciitis with heel spurs. A randomized controlled clinical study. Eur J Phys Rehabil Med. 2014 Feb 1;50(1):39-47.
- ↑ Shanks P, Curran M, Fletcher P, Thompson R. The effectiveness of therapeutic ultrasound for musculoskeletal conditions of the lower limb: A literature review. The Foot. 2010 Dec 1;20(4):133-9.
- ↑ 17.0 17.1 17.2 Barry LD, Barry AN, Chen Y. A retrospective study of standing gastrocnemius-soleus stretching versus night splinting in the treatment of plantar fasciitis. The Journal of foot and ankle surgery. 2002 Jul 1;41(4):221-7.
- ↑ 18.0 18.1 DiGiovanni BF, Nawoczenski DA, Malay DP, Graci PA, Williams TT, Wilding GE, Baumhauer JF. Plantar fascia-specific stretching exercise improves outcomes in patients with chronic plantar fasciitis: a prospective clinical trial with two-year follow-up. JBJS. 2006 Aug 1;88(8):1775-81.
- ↑ 19.0 19.1 Porter D, Barrill E, Oneacre K, May BD. The effects of duration and frequency of Achilles tendon stretching on dorsiflexion and outcome in painful heel syndrome: a randomized, blinded, control study. Foot & ankle international. 2002 Jul;23(7):619-24.
- ↑ 20.0 20.1 Radford JA, Landorf KB, Buchbinder R, Cook C. Effectiveness of calf muscle stretching for the short-term treatment of plantar heel pain: a randomised trial. BMC musculoskeletal disorders. 2007 Dec;8(1):1-8.
- ↑ 21.0 21.1 21.2 21.3 Rompe JD, Cacchio A, Weil Jr L, Furia JP, Haist J, Reiners V, Schmitz C, Maffulli N. Plantar fascia-specific stretching versus radial shock-wave therapy as initial treatment of plantar fasciopathy. JBJS. 2010 Nov 3;92(15):2514-22.
- ↑ 22.0 22.1 22.2 22.3 Kamonseki DH, Gonçalves GA, Liu CY, Júnior IL. Effect of stretching with and without muscle strengthening exercises for the foot and hip in patients with plantar fasciitis: a randomized controlled single-blind clinical trial. Manual therapy. 2016 Jun 1;23:76-82.
- ↑ Sweeting D, Parish B, Hooper L, Chester R. The effectiveness of manual stretching in the treatment of plantar heel pain: a systematic review. Journal of foot and ankle research. 2011 Dec;4(1):1-3.
- ↑ 24.0 24.1 Rathleff MS, Mølgaard CM, Fredberg U, Kaalund S, Andersen KB, Jensen TT, Aaskov S, Olesen JL. High‐load strength training improves outcome in patients with plantar fasciitis: A randomized controlled trial with 12‐month follow‐up. Scandinavian journal of medicine & science in sports. 2015 Jun;25(3):e292-300.
- ↑ 25.0 25.1 Mischke JJ, Jayaseelan DJ, Sault JD, Emerson Kavchak AJ. The symptomatic and functional effects of manual physical therapy on plantar heel pain: a systematic review. Journal of Manual & Manipulative Therapy. 2017 Jan 1;25(1):3-10.
- ↑ 26.0 26.1 26.2 26.3 26.4 26.5 Hasegawa M, Urits I, Orhurhu V, Orhurhu MS, Brinkman J, Giacomazzi S, Foster L, Manchikanti L, Kaye AD, Kaye RJ, Viswanath O. Current concepts of minimally invasive treatment options for plantar fasciitis: A comprehensive review. Current Pain and Headache Reports. 2020 Sep;24(9):1-1.
- ↑ 27.0 27.1 27.2 27.3 27.4 Cleland JA, Abbott JH, Kidd MO, Stockwell S, Cheney S, Gerrard DF, Flynn TW. Manual physical therapy and exercise versus electrophysical agents and exercise in the management of plantar heel pain: a multicenter randomized clinical trial. journal of orthopaedic & sports physical therapy. 2009 Aug;39(8):573-85.
- ↑ 28.0 28.1 28.2 28.3 28.4 Shashua A, Flechter S, Avidan L, Ofir D, Melayev A, Kalichman L. The effect of additional ankle and midfoot mobilizations on plantar fasciitis: a randomized controlled trial. Journal of Orthopaedic & Sports Physical Therapy. 2015 Apr;45(4):265-72.
- ↑ 29.0 29.1 29.2 29.3 29.4 Tsai CT, Chang WD, Lee JP. Effects of short-term treatment with Kinesio taping for plantar fasciitis. Journal of Musculoskeletal Pain. 2010 Jan 1;18(1):71-80.
- ↑ 30.0 30.1 30.2 30.3 Radford JA, Landorf KB, Buchbinder R, Cook C. Effectiveness of low-Dye taping for the short-term treatment of plantar heel pain: a randomised trial. BMC musculoskeletal disorders. 2006 Dec;7(1):1-7.
- ↑ 31.0 31.1 31.2 31.3 31.4 31.5 31.6 Cotchett MP, Munteanu SE, Landorf KB. Effectiveness of trigger point dry needling for plantar heel pain: a randomized controlled trial. Physical therapy. 2014 Aug 1;94(8):1083-94.
- ↑ Llurda-Almuzara L, Labata-Lezaun N, Meca-Rivera T, Navarro-Santana MJ, Cleland JA, Fernández-de-Las-Peñas C, Pérez-Bellmunt A. Is Dry Needling Effective for the Management of Plantar Heel Pain or Plantar Fasciitis? An Updated Systematic Review and Meta-analysis. Pain Medicine. 2021 Mar 24.
- ↑ 33.0 33.1 Cotchett MP, Landorf KB, Munteanu SE. Effectiveness of dry needling and injections of myofascial trigger points associated with plantar heel pain: a systematic review. Journal of foot and ankle research. 2010 Dec;3(1):1-9.
- ↑ 34.0 34.1 Pfeffer G, Bacchetti P, Deland J, Lewis AI, Anderson R, Davis W, Alvarez R, Brodsky J, Cooper P, Frey C, Herhck R. Comparison of custom and prefabricated orthoses in the initial treatment of proximal plantar fasciitis. Foot & Ankle International. 1999 Apr;20(4):214-21.
- ↑ 35.0 35.1 Landorf KB, Keenan AM, Herbert RD. Effectiveness of foot orthoses to treat plantar fasciitis: a randomized trial. Archives of internal medicine. 2006 Jun 26;166(12):1305-10.
- ↑ 36.0 36.1 Baldassin V, Gomes CR, Beraldo PS. Effectiveness of prefabricated and customized foot orthoses made from low-cost foam for non-complicated plantar fasciitis: a randomized controlled trial. Archives of physical medicine and rehabilitation. 2009 Apr 1;90(4):701-6.
- ↑ 37.0 37.1 Wrobel JS, Fleischer AE, Crews RT, Jarrett B, Najafi B. A randomized controlled trial of custom foot orthoses for the treatment of plantar heel pain. Journal of the American Podiatric Medical Association. 2015 Jul;105(4):281-94.
- ↑ 38.0 38.1 Winemiller MH, Billow RG, Laskowski ER, Harmsen WS. Effect of magnetic vs sham-magnetic insoles on plantar heel pain: a randomized controlled trial. Jama. 2003 Sep 17;290(11):1474-8.
- ↑ 39.0 39.1 Buchbinder R, Ptasznik R, Gordon J, Buchanan J, Prabaharan V, Forbes A. Ultrasound-guided extracorporeal shock wave therapy for plantar fasciitis: a randomized controlled trial. Jama. 2002 Sep 18;288(11):1364-72.
- ↑ 40.0 40.1 Gerdesmeyer L, Frey C, Vester J, Maier M, Lowell Jr W, Weil Sr L, Russlies M, Stienstra J, Scurran B, Fedder K, Diehl P. Radial extracorporeal shock wave therapy is safe and effective in the treatment of chronic recalcitrant plantar fasciitis: results of a confirmatory randomized placebo-controlled multicenter study. The American journal of sports medicine. 2008 Nov;36(11):2100-9.
- ↑ Haake M, Buch M, Schoellner C, Goebel F, Vogel M, Mueller I, Hausdorf J, Zamzow K, Schade-Brittinger C, Mueller HH. Extracorporeal shock wave therapy for plantar fasciitis: randomised controlled multicentre trial. Bmj. 2003 Jul 10;327(7406):75.
- ↑ Kudo P, Dainty K, Clarfield M, Coughlin L, Lavoie P, Lebrun C. Randomized, placebo‐controlled, double‐blind clinical trial evaluating the treatment of plantar fasciitis with an extracoporeal shockwave therapy (ESWT) device: A North American confirmatory study. Journal of orthopaedic research. 2006 Feb;24(2):115-23.
- ↑ Malay DS, Pressman MM, Assili A, Kline JT, York S, Buren B, Heyman ER, Borowsky P, LeMay C. Extracorporeal shockwave therapy versus placebo for the treatment of chronic proximal plantar fasciitis: results of a randomized, placebo-controlled, double-blinded, multicenter intervention trial. The Journal of foot and ankle surgery. 2006 Jul 1;45(4):196-210.
- ↑ Speed CA, Nichols D, Wies J, Humphreys H, Richards C, Burnet S, Hazleman BL. Extracorporeal shock wave therapy for plantar fasciitis. A double-blind randomised controlled trial. Journal of Orthopaedic Research. 2003 Sep;21(5):937-40.
- ↑ Yu H, Randhawa K, Côté P, Optima Collaboration. The effectiveness of physical agents for lower-limb soft tissue injuries: A systematic review. Journal of Orthopaedic & Sports Physical Therapy. 2016 Jul;46(7):523-54.
- ↑ 46.0 46.1 46.2 David JA, Sankarapandian V, Christopher PR, Chatterjee A, Macaden AS. Injected corticosteroids for treating plantar heel pain in adults. Cochrane Database of Systematic Reviews. 2017(6). CD009348.
- ↑ 47.0 47.1 47.2 47.3 47.4 47.5 Gibbons R, Mackie KE, Beveridge T, Hince D, Ammon P. Evaluation of long-term outcomes following plantar fasciotomy. Foot & ankle international. 2018 Nov;39(11):1312-9.
- ↑ Crawford F, Thomson CE. Interventions for treating plantar heel pain. Cochrane Database of Systematic Reviews. 2003(3).