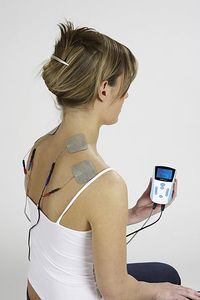
Transcutaneous Electrical Nerve Stimulation (TENS)
Introduction[edit | edit source]
TENS is a method of electrical stimulation which primarily aims to provide a degree of symptomatic pain relief by exciting sensory nerves and thereby stimulating either the pain gate mechanism and/or the opioid system. The different methods of applying TENS relate to these different physiological mechanisms. The effectiveness of TENS varies with the clinical pain being treated, but research would suggest that when used ‘well’ it provides significantly greater pain relief than a placebo intervention. There is an extensive research base for TENS in both the clinical and laboratory settings and whilst this summary does not provide a full review of the literature, the key papers are referenced. It is worth noting that the term TENS could represent the use of ANY electrical stimulation using skin surface electrodes which has the intention of stimulating nerves. In the clinical context, it is most commonly assumed to refer to the use of electrical stimulation with the specific intention of providing symptomatic pain relief. If you do a literature search on the term TENS, do not be surprised if you come across a whole lot of ‘other’ types of stimulation which technically fall into this grouping.
The illustrations shows a 2 channel TENS unit as it has 4 lead wires (Each channel has two lead wires) with electrode pads attached.
Mechanism of Action[edit | edit source]
The type of stimulation delivered by the TENS unit aims to excite (stimulate) the sensory nerves, and by so doing, activate specific natural pain relief mechanisms. For convenience, if one considers that there are two primary pain relief mechanisms which can be activated : the Pain Gate Mechanism and the Endogenous Opioid System, the variation in stimulation parameters used to activate these two systems will be briefly considered.
Pain relief by means of the pain gate mechanism involves activation (excitation) of the A beta (Aβ) sensory fibres, and by doing so, reduces the transmission of the noxious stimulus from the ‘c’ fibres, through the spinal cord and hence on to the higher centres. The Aβ fibres appear to appreciate being stimulated at a relatively high frequency HF (in the order of 90 - 130 Hz or pps). It is difficult to find support for the concept that there is a single frequency that works best for every patient, but this range appears to cover the majority of individuals. Clinically it is important to enable the patient to find their optimal treatment frequency – which will almost certainly vary between individuals. Setting the machine and telling the patient that this is the ‘right’ setting is almost certainly not going to be the maximally effective treatment, though of course, some pain relief may well be achieved.
An alternative approach is to stimulate the A delta (Aδ) fibres which respond preferentially to a much low frequency LF (in the order of 2 - 5 Hz), which will activate the opioid mechanisms, and provide pain relief by causing the release of an endogenous opiate (encephalin) in the spinal cord which will reduce the activation of the noxious sensory pathways. In a similar way to the pain gate physiology, it is unlikely that there is a single (magic) frequency in this range that works best for everybody – patients should be encouraged to explore the options where possible.[1]
A third possibility is to stimulate both nerve types at the same time by employing a burst mode stimulation. In this instance, the higher frequency stimulation output (typically at about 100Hz) is interrupted (or burst) at the rate of about 2 - 3 bursts per second. When the machine is ‘on’, it will deliver pulses at the 100Hz rate, thereby activating the Aβ fibres and the pain gate mechanism, but by virtue of the rate of the burst, each burst will produce excitation in the Aδ fibres, therefore stimulating the opioid mechanisms. For some patients this is by far the most effective approach to pain relief, though as a sensation, numerous patients find it less acceptable than some other forms of TENS as there is more of a ‘grabbing’, ‘clawing’ type sensation and usually more by way of muscle twitching than with the high or low frequency modes.
TENS as a treatment technique is non invasive and has few side effects when compared with drug therapy. The most common complaint is an allergic type skin reaction (about 2-3% of patients) and this is almost always due to the material of the electrodes, the conductive gel or the tape employed to hold the electrodes in place. Most TENS applications are now made using self adhesive, pre gelled electrodes which have several advantages including reduced cross infection risk, ease of application, lower allergy incidence rates and lower overall cost. Digital TENS machines are becoming more widely available and extra features (like automated frequency sweeps and more complex stimulation patterns) are emerging, though there remains little clinical evidence for enhanced efficacy at the present time. Some of these devices do offer pre-programmed and/or automated treatment settings.
Impedence of Current Flow[edit | edit source]
The amount of electrical current flowing through body tissues is influenced by the impedance of the pathway - this is a measure of how readily the body allows the current to pass.. Impedance in biological tissues consists of resistive (ohmic) properties and reactive elements, which can be capacitive or inductive. The inductive elements are negligible in body tissues, meaning they do not significantly affect current flow.[2]
Ohmic resistance refers to the resistance to direct current flow offered by tissues. Tissues that have a high water content, such as blood, muscle, and nerve, present less resistance, i.e., they have a lower ohmic resistance. Conversely, tissues such as bone and fat offer more resistance, and the skin's outer layer, the epidermis, has the highest resistance.[2]
However, in the context of Transcutaneous Electrical Nerve Stimulation (TENS) therapy, which typically involves high-frequency signals between 2 to 200 Hz, another type of resistance called capacitive reactance becomes particularly important.[3] This capacitive reactance pertains to the resistance offered by the capacitance of the tissue to the flow of alternating current. Capacitive reactance refers to the opposition that a capacitor offers to the flow of alternating current in an electric circuit. It impacts how tissues respond to varying frequencies of the electrical signal, particularly at higher frequencies.[2]
Therefore, to determine the effectiveness of TENS therapy, it is necessary to take into account both the resistive (ohmic) and capacitive elements of the skin and underlying tissues' overall impedance.[3]
Types of TENS[edit | edit source]
| Conventtional TENS(High) | Acupuncture-like TENS(Low) | Brief Intense TENS | |
|---|---|---|---|
| Physiological Intervention | To activate large diameter non-notious afferent to elicit segmental analgesia. | To produce muscle twitch to activate small diameter motor affrent to elicit extra segmental analgesia. | To activate small diameter noxious affrents to elicit peripheral nerve blockade and extrasegmental analgesia. |
| Clinical Teqnique | Low intensity \High Frequency at site of pain to produce strong but comfrtable sensation. | High intensity\Low frequency over muscle or Acupuncture points to produce strong but comfortable contraction. | High intensity \High frequency to produce maximum parathesia |
| Duration of stimulation | 30 min | No more than 20 min | no more than 5 min |
Electrode Placement Technique[edit | edit source]
this is determined by the target muscle or muscle group either single or in relation to other muscles
- Unilateral : Unilateral placement causes inflammation of one limb or half of muscle pair.
- Bilateral : It allow the stimulation of both limbs or both halves of a muscle Pair
- Uni-polar : Only one of two essential leads and the electrode connected to it are placed over the target area affected by the stimulation This electrode is called treatment electrode.
- Quadripolar : Involve the use of two sets of electrode each originating from its own channel. It may be considered the concurrent application of two bipolar circuit. This technique could be used with stimulation of agonist and antagonist. Also could be used in crossed pattern or for large flat area as back.
Contraindications[edit | edit source]
- Patients who do not comprehend the physiotherapist’s instructions or who are unable to co-operate
- It has been widely cited that application of the electrodes over the trunk, abdomen or pelvis during pregnancy is contraindicated BUT a recent review suggests that although not an ideal (first line) treatment option, application of TENS around the trunk during pregnancy can be safely applied, and no detrimental effects have been reported in the literature (see www.electrotherapy,org for publication details).TENS during labour for pain relief is both safe and effective.
- Patients with a Pacemaker should not be routinely treated with TENS though under carefully controlled conditions it can be safely applied. It is suggested that routine application of TENS for a patient with a pacemaker or any other implanted electronic device should be considered a contraindication.
- Patients who have an allergic response to the electrodes, gel or tape
- Electrode placement over dermatological lesions e.g. dermatitis, eczema
- Application over the anterior aspect of the neck or carotid sinus[6]
Precautions[edit | edit source]
- If there is abnormal skin sensation, the electrodes should preferably be positioned elsewhere to ensure effective stimulation
- Electrodes should not be placed over the eyes
- Patients who have epilepsy should be treated at the discretion of the therapist in consultation with the appropriate medical practitioner as there have been anecdotal reports of adverse outcomes, most especially (but not exclusively) associated with treatments to the neck and upper thoracic areas
- Avoid active epiphyseal regions in children (though there is no direct evidence of adverse effect)
- The use of abdominal electrodes during labour may interfere with foetal monitoring equipment and is therefore best avoided.
The Evidence for TENS for Pain Control[edit | edit source]
A 2020 review suggests that the use of TENS has positive outcomes in treatment of Primary Dysmenorrhea[7].
A 2014 study set out to provide a critical review of the latest basic science and clinical evidence for TENS. Key findings were:
- Application of TENS at inadequate intensities is one of the primary factors attributed to conflicting reports of TENS efficacy. Using the strongest intensity that remains comfortable produces hypoalgesia in healthy subjects is imperative; lower intensities are ineffective. In addition to activation of greater numbers of sensory afferents, higher pulse amplitudes are proposed to activate deeper tissue afferents allowing for greater analgesia. High intensity TENS decreases post-operative opioid requirements and negative opioid-side effects.
- Both High Frequency(HF) and Low Frequency(LF) TENS been shown to provide analgesia specifically when applied at a strong, non-painful intensity. HF TENS may be more effective for people taking opioids.
- Effective analgesia for chronic pain conditions may be limited by the development of tolerance to TENS if repeated application of either HF or LF TENS at the same frequency, intensity and pulse duration is used daily.
- Application of TENS electrodes at acupoint sites may increases analgesia and targeting the use of TENS during movement or required activity may provide the most benefit.
- Systematic reviews suggest that TENS, when applied at adequate intensities, is effective for postoperative pain, osteoarthritis, painful diabetic neuropathy and some acute pain conditions.
- Emerging evidence suggests TENs may be helpful for peoples with fibromyalgia and spinal cord injury.
- TENS may be effective in restoration of central pain modulation, a measure of central inhibition.[1]
Effectiveness on Chronic Pain[edit | edit source]
There are nine reviews investigating TENS use in people with defined chronic pain or in people with chronic conditions associated with ongoing pain. One review investigating TENS for phantom or stump‐associated pain in people following amputation did not have included studies. For people with chronic pain, this overview offers very low quality evidence and cannot confidently make any statement regarding the effectiveness of TENS for people with chronic pain. The very low quality of all reviewed evidence means we have very limited confidence in any suggested estimate of effect for all outcomes and the true effect is likely to be different from that summarised here and within individual reviews.[8]
Helpful resource[edit | edit source]
TENS for constipation in children (systematic review)
References[edit | edit source]
- ↑ 1.0 1.1 Vance CG, Dailey DL, Rakel BA, Sluka KA. Using TENS for pain control: the state of the evidence. Pain management. 2014 May;4(3):197-209. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4186747/ (last accessed 12.5.2019)
- ↑ 2.0 2.1 2.2 Geddes, L. A., Baker, L. E., & Moore, A. G. (1980). Electrical properties of skin at moderate frequencies. Medical and biological engineering & computing, 18(6), 652-656
- ↑ 3.0 3.1 Gabriel S, Lau RW, Gabriel C. The dielectric properties of biological tissues: II. Measurements in the frequency range 10 Hz to 20 GHz. Physics in medicine & biology. 1996 Nov 1;41(11):2251.
- ↑ Professor Mark Johnson Transcutaneous Electrical Nerve Stimulation: Mechanisms, Clinical Application and Evidence (2007)
- ↑ Ask Dr Jo. TENS. Available from: https://www.youtube.com/watch?v=TrFrcIzGF6E&feature=youtu.be (last accessed 12.5.2019)
- ↑ Enriched health care.Use of TENS machines. Available from: http://www.enrichedhealthcare.com.au/library/resources/tens (last accessed 12.5.2019)
- ↑ Elboim-Gabyzon M, Kalichman L. Transcutaneous Electrical Nerve Stimulation (TENS) for Primary Dysmenorrhea: An Overview. International Journal of Women's Health. 2020;12:1.
- ↑ William Gibson, Benedict M Wand, Catherine Meads, Mark J Catley, Neil E O'Connell.Transcutaneous electrical nerve stimulation for chronic pain.2019