Sjogren's Syndrome
Top Contributors - Cassie Shay, Kim Jackson, Admin, Lucinda hampton, Elaine Lonnemann, 127.0.0.1, Wendy Walker, WikiSysop and Sehriban Ozmen
Introduction[edit | edit source]
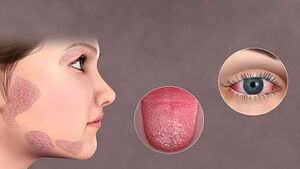
Sjögren's syndrome (SS) is a chronic systemic autoimmune disease characterized by lymphocytic infiltration of exocrine glands. It is a relatively common condition that mainly affects the eyes and salivary glands, but can affect different parts of the body.[1][2].
There is no cure, but the condition can be managed with medications and products such as artificial tears and saliva as well as mouth washes and lozenges.[3]
Epidemiology[edit | edit source]
SS is the second most prevalent autoimmune rheumatic disease. In 2008, it was estimated that 1.3 million Americans were affected[2][4] It can present as an entity by itself, primary Sjögren's syndrome (pSS), or in addition to another autoimmune disease, secondary Sjögren's syndrome (sSS). pSS has a strong female propensity and is more prevalent in Caucasian women, with the mean age of onset usually in the 4th to 5th decade.[1]
Etiology[edit | edit source]
It is not known what causes SS. Genes may play a role, combined with an outside trigger eg bacteria or virus.It’s also more likely to affect people who have conditions such as rheumatoid arthritis, scleroderma and lupus[3].
Clinical Presentation[edit | edit source]
This 90 second video takes a look at this syndrome.
The more common symptoms of Sjogren’s syndrome include:
- dry eyes (irritation, feeling gritty or itchy, burning)
- dry mouth (or difficulty chewing or swallowing).
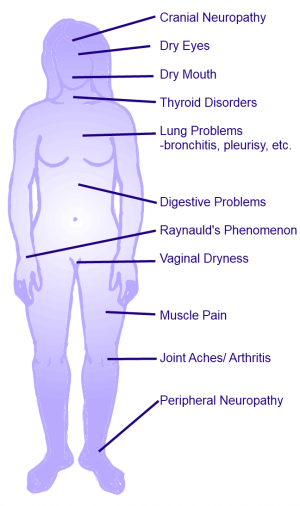
Sjogren’s syndrome is a systemic condition, which means it can affect the entire body, other symptoms can include:
- swelling and tenderness of the glands around your face, neck, armpits and groin
- tiredness (fatigue)
- dry skin or rashes
- joint pain and general achiness
- dryness of the nose, ear and throat
- vaginal dryness
- bowel irritation.
Complications can include:
- increased risk of dental decay
- increased risk of developing thrush infections in the mouth
- vision problems
- inflammation of internal organs (such as the kidneys, lungs or liver)
- problems with the circulatory and nervous system.[3]
Associated Co-morbidities[edit | edit source]
Secondary Sjogren's is a form of the syndrome which develops after the presentation of a primary disease, usually another autoimmune connective tissue disease[2]. Common primary diseases associated with Sjogren's Syndrome include: Polymyositis; Rheumatoid Arthritis; Scleroderma; Systemic Lupus Erythematosus; Lymphoma.[5]
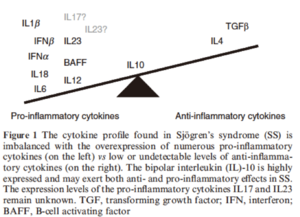
Image R: The cytokine profile found in Sjogren’s syndrome (SS) is imbalanced with the overexpression of numerous pro-inflammatory cytokines (on the left) vs low or undetectable levels of anti-inflammatory cytokines (on the right in image).
Treatment[edit | edit source]
There is no cure for Sjogren's syndrome, therefore its symptoms are managed through medications, both prescription and over the counter. A variety of medications may be used to treat each of the associated symptoms. Treatment may include:
- artificial tears and lubricating ointments for the eyes
- artificial saliva
- mouth rinses and lozenges
- nasal sprays
- vaginal lubricants
- moisturising lotion for the skin
- non-steroidal anti-inflammatory drugs (NSAIDs) – these medications (for example naproxen and ibuprofen) help control inflammation and provide temporary pain relief
- corticosteroid medications – may be used as a temporary treatment for joint pain
- immunosuppressive medications (for example hydroxychloroquine and methotrexate) – may be used to help control your overactive immune system[3].
Diagnostic Tests[edit | edit source]
Diagnosis of this disease is based on medical history, a physical exam, and results from some clinical and laboratory tests[5][2][4]. Due to the nature of the disease in that the symptoms are similar to other diseases and they appear gradually over time, it may take years for Sjogren's to be properly diagnosed[2]. Nonetheless, diagnostic testing may include the following:
- Schirmer’s test – special blotting paper held to the eye is used to assess the degree of tear production
- eye examination – including the use of special dyes
- biopsy – a small piece of salivary gland tissue is removed (usually from the lip) and examined under a microscope
- blood tests – may be used to check the levels of particular immune system cells in the blood, and to check for any problems with your kidneys or liver[3].
Physical Therapy Management[edit | edit source]
Individuals with Sjogren's syndrome have reduced physical capacity and tend to fatigue very easily. While research on the effects of exercise on individuals diagnosed with Sjogren's is limited, the available studies suggest these patients benefit from moderate to high-intensity levels of exercise[4]. This type of activity has a positive influence on aerobic capacity, fatigue, physical function, and mood.
Further research is required to understand the effects exercise may have on individuals with varying severities of this disease, and to determine the long-term effects exercise may have on their symptoms[4]. However, some of the musculoskeletal presentations of SS are muscle and joint pain, along with arthritis. Thererfore, a patient may be treated by a physical therapist to relieve these symptoms[6].
Lifestyle Changes[edit | edit source]
There are also several things a patient can do at home in order to manage his or her symptoms. These may include[2]:
- Over the counter eye drops
- Chewing gum or sucking on hard candy to increase oral secretions
- Drinking water to relieve a dry mouth
- Using lip balm to moisten the lips
- Practice thorough oral hygiene to avoid oral infection
- Heavy moisturizing creams or ointment for dry skin
- Humidifier to hydrate the skin and moisten the air for breathing[3]
References[edit | edit source]
- ↑ 1.0 1.1 Patel R, Shahane A. The epidemiology of Sjögren's syndrome. Clin Epidemiol. 2014 Jul 30;6:247-55. doi: 10.2147/CLEP.S47399. PMID: 25114590; PMCID: PMC4122257.Available: https://pubmed.ncbi.nlm.nih.gov/25114590/(accessed 6/3/2022)
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 National Institute of Arthritis and Musculoskeletal and Skin Diseases. Sjogren's Syndrome. http://ww.niams.niih.gov/Health_Info/Sjogrens_Syndrome/default.asp (accessed 17 March 2011).
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 Better Health Sjogren's Syndrome Available: https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/sjogrens-syndrome#self-management-of-sjogren%E2%80%99s-syndrome(accessed 6.3.2022)
- ↑ 4.0 4.1 4.2 4.3 Goodman C, Fuller K. Pathology: Implications for the Physical Therapist. 3rd ed. Denver, CO: Saunders, 2009.
- ↑ 5.0 5.1 American College of Rheumatology. Sjogren's Syndrome. http://www.rheumatology.org/practice/clinical/patients/diseases_and_conditions/sjogrens.asp (accessed 17 March 2011).
- ↑ Medline Plus. Sjogren Syndrome. http://www.nlm.nih.gov/medlineplus/ency/article/000456.htm (accessed 6 April 2011)