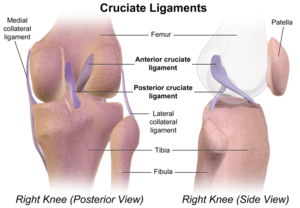
Posterior Cruciate Ligament
Description[edit | edit source]
The posterior cruciate ligament (PCL) is the strongest and largest intra-articular ligament in human knee and the primary posterior stabilizer of the knee. It comprises of 2 functional bundles: the larger anterolateral bundle (ALB) and the smaller posteromedial bundle (PMB). The size of the femoral attachment of the ALB is nearly twice the size of its tibial attachment[1].
Attachments[edit | edit source]
Origin[edit | edit source]
The PCL originates from the anterolateral aspect of the medial femoral condyle within the notch[1].
Insertion[edit | edit source]
The PCL inserts along the posterior aspect of the tibial plateau, approximately 1 cm distal to the joint line[1]. The average surface area of the PCL attachments to the femur and tibia was studied by Voos et al. It was found the area of the femoral footprint to be 209 mm2 and tibial footprint to be 243 mm2[2]. Thus, the PCL insertion sites are roughly three times larger than its mid-substance.
Vascular Supply[edit | edit source]
The middle geniculate artery perforates the posterior capsule running parallel to the superior edge of the synovial septum. It has branches to the synovium around the PCL forming a plexus of vessels supplying the PCL. There is also a potential supply from a branch of the inferior geniculate artery[3].
Nerve Supply[edit | edit source]
The tibial and obturator nerve has posterior articular branches to the posterior capsule. These branches perforate the posterior capsule to reach the PCL[3].
Function[edit | edit source]
The PCL functions as one of the main stabilizers of the knee joint and serves primarily to resist excessive posterior translation of the tibia relative to the femur. The PCL also acts as a secondary stabilizer of the knee preventing excessive rotation specifically between 90° and 120° of knee flexion[4]. The two bundles of PCL, ALB and PMB function synergistically[5].
Clinical Relevance[edit | edit source]
Posterior cruciate ligament (PCL) tears comprise 3% of outpatient knee injuries and 38% of acute traumatic knee hemarthroses. These injuries rarely occur in isolation, and up to 95% of PCL tears occur in combination with other ligament tears.PCL tears are increasingly being recognized as source of morbidity and reduced function because of persistent instability, pain, impaired function and development of degenerative joint disease[2].
PCL tears are typically produced by external trauma such as the classic “dashboard injury” resulting from a posteriorly directed force on the anterior aspect of the proximal tibia with the knee flexed. In athletics, the typical mechanism of isolated PCL tears is a direct blow to the anterior tibia or a fall onto the knee with the foot in a plantar flexed position. Football, soccer, rugby and skiing are among the sports with highest incidence of PCL tears[2].
Symptoms depend upon the injury mechanism (high vs low-energy) as well as chronicity. Stiffness, swelling and pain on the posterior aspect of the knee are typical symptoms, while anterior knee pain and instability when descending stairs are more often associated with chronic isolated tears[2].
Assessment[edit | edit source]
A careful vascular examination of the lower extremities is essential because a PCL injury can be accompanied by a popliteal artery injury. If the pulses are weak or the ankle-brachial index is ≤0.8, an intimal tear should be suspected and arteriography should be performed. Acute PCL injuries present with joint swelling and about 10° to 20° of restriction in further flexion due to pain. Chronic PCL injuries may present with limited activity such as having difficulty in climbing slopes due to lethargy and pain in the anterior and medial areas of the knee rather than instability[6].
Special Test[edit | edit source]
The posterior drawer test is the most accurate test for PCL injuries. At 90° of knee flexion, posterior sagging of the tibia is observed on the affected side. If the tibia is pulled forward or the quadriceps is contracted with the knee flexed to 90° (quadriceps active test), anteroposterior instability of the knee is noted[6].
Physiotherapy Management[edit | edit source]
Nonsurgical treatment has been advocated for patients with isolated grade I or II PCL injuries or those with grade III injuries but have mild symptoms or only participate in low-demand activities. The rehabilitation program consists of phases with generalized time frames, and the patient’s progress depends on severity of injury and patient presentation.[8]
Phase I (Protective Phase) Week 1-6[edit | edit source]
During the first few weeks, the goals of treatment should focus on effusion control, knee range of motion within prescribed limits, normalization of gait, and reactivation of the quadriceps musculature. Hyperextension of the knee and posterior tibial translation should be avoided during this initial phase.
Immediately after injury, it is common to have swelling, generalized knee pain, and loss of motion. Joint effusion has been shown to inhibit the quadriceps, resulting in loss of musculature and subsequent “knee buckling”. Treatment strategies to address effusion consist of cryotherapy, elevation, joint compression, transcutaneous electrical stimulation, and manual therapy techniques. Once the effusion is controlled and the patient can perform a straight leg raise without a quadriceps lag, they can begin to progress off of crutches. Weight bearing may be limited the first 2 weeks to partial weight bearing (PWB) or weight bearing as tolerated (WBAT) depending on the grade of injury.
Phase II (Transitional Phase) Week 6-12[edit | edit source]
The goals of phase II are to enhance proprioception and strengthen the lower extremities in order to perform light low-impact activities pain free and without effusion. Patients are full weight bearing and should achieve full knee ROM. Knee hyperextension and posterior tibial translation should continue to be avoided.
Strengthening with closed kinetic chain exercises (squats and leg press) are performed and limited to 0 to 70° of flexion. With squats, the patient and therapist must ensure that compensatory movements are not performed, such as shifting away from the injured limb (leg dominance) and genu valgus. Leg dominance relates to side-to-side symmetry, balance, and muscular strength, which may place both limbs at risk. This will cause the weaker limb to be compromised in its ability to dissipate forces while the stronger limb is subjected to high forces secondary to increased dependence and excessive loading. Proprioceptive exercises are advanced from double to single limb, and on varying unstable surfaces.
Phase III (Functional Phase) Week 12-16[edit | edit source]
In phase III, any bracing should be discontinued and the goal is to return to light activities such as a jogging program. Closed-chain exercises may advance past 70° and can progress to single-limb pending strength and quality of movement. Isolated hamstring exercises can be performed and advanced as tolerated. Core strengthening, proprioception, and neuromuscular control are advanced to restore dynamic stabilization of the knee joint. In order to advance to running, the patient must demonstrate sufficient strength and stability on one limb, as well as be pain free and without effusion with functional activities. Agility work may begin with a focus on quality of movement and coordination that is specific to the patient’s goals or sport.
Return to Play Phase: Week 16-24[edit | edit source]
Further phases are dedicated to establishing a full-strength base for advanced movements and functional exercises, endurance, sports-specific agility, neuromuscular control, and ensure quality of movement to avoid re-injury. Compensatory movements should be assessed and addressed to avoid re-injury as well as future injury. Dynamic stabilization drills and plyometrics are advanced from double limb to single limb. Plyometric exercises are explosive and meant to build power, strength, and speed. These activities involve jumping, landing, and cutting maneuvers in varying planes of motion at varying intensity levels.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 Logterman SL, Wydra FB, Frank RM. Posterior cruciate ligament: anatomy and biomechanics. Current reviews in musculoskeletal medicine. 2018 Sep 1;11(3):510-4.
- ↑ 2.0 2.1 2.2 2.3 Voos JE, Mauro CS, Wente T, Warren RF, Wickiewicz TL. Posterior cruciate ligament: anatomy, biomechanics, and outcomes. The American journal of sports medicine. 2012 Jan;40(1):222-31.
- ↑ 3.0 3.1 Marais JJ. Anatomy of the posterior cruciate ligament. SA Orthopaedic Journal. 2009 Jan;8(4):23-9.
- ↑ Papannagari R, DeFrate LE, Nha KW, Moses JM, Moussa M, Gill TJ, Guoan L. Function of posterior cruciate ligament bundles during in vivo knee flexion. The American journal of sports medicine. 2007 Sep;35(9):1507-12.
- ↑ Ahmad CS, Cohen ZA, Levine WN, Gardner TR, Ateshian GA, Mow VC. Codominance of the individual posterior cruciate ligament bundles: an analysis of bundle lengths and orientation. The American journal of sports medicine. 2003 Mar;31(2):221-5.
- ↑ 6.0 6.1 Lee BK, Nam SW. Rupture of posterior cruciate ligament: diagnosis and treatment principles. Knee surgery & related research. 2011 Sep;23(3):135.
- ↑ Physiotutors. Posterior Drawer Test⎟Posterior Cruciate Ligament. Available from: https://www.youtube.com/watch?v=wDIGll5wzZs [last accessed 21/10/2019]
- ↑ Wang D, Graziano J, Williams RJ, Jones KJ. Nonoperative Treatment of PCL Injuries: Goals of Rehabilitation and the Natural History of Conservative Care. Current reviews in musculoskeletal medicine. 2018 Jun 1;11(2):290-7.