Mechanical Loading of Bone
Introduction[edit | edit source]
Bone mass is regulated by both mechanical and biochemical stimuli. Like muscles, bones add mass when they are loaded (physical activity) and will lose mass if they are not (immobilisation or time spent at low or zero gravity) [1]
Smart Material: Bone is a remarkable living material that comes in two forms with different porosities and different macrostructure, but with the same highly organised microstructure and nanostructure. As bone accumulates damage, it is removed and replaced. When the mechanical demands on bone increase the bone mass increases, while reductions in the loading leads to the removal of bone, thus bone can be considered a ‘smart material’.
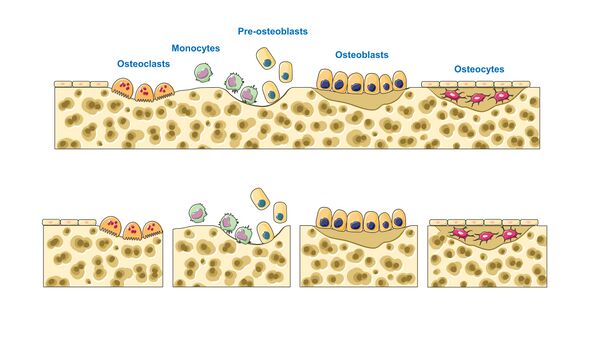
Remodelling: The ongoing replacement of old bone tissue by new bone tissue is called remodelling. Bone formation, repair and remodelling is controlled and produced by four types of cell, namely osteoblasts, osteoclasts, osteocytes and bone lining cells. Bone remodelling is regulated by signals to these cells generated by mechanical loading. Exactly how loads are transferred into bone, how the bone cells sense these loads and how the signals are translated into bone formation or removal is unknown[2].
Detecting Mechanical Load[edit | edit source]
The main sensor of mechanical forces is the osteocytes network, which transmits orders to effector cells ie osteoclasts, and osteoblasts, by the secretion of several cytokines which modulate the concentration of the bone microenvironment.
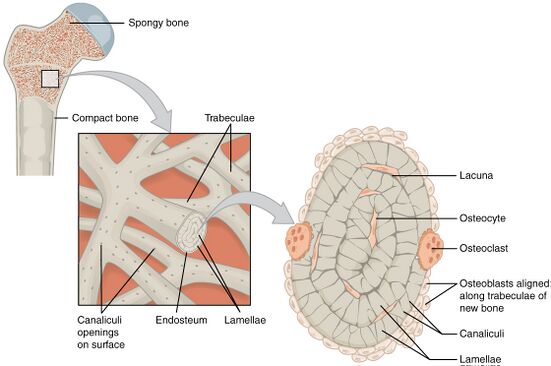
Osteocytes:
- The most abundant cells found in bone (90-95% of all bone cells) with long dendritic processes to communicate with surrounding cells.
- Detect the change of deformation by load and send signals to the osteoblasts and osteoclasts to repair and strengthen the bone.
- The biochemical reaction triggered by these mechanosensitive osteocytes leads to osteogenesis (new bone formation).
Key molecules in sensing and transducing:
- Calcium channels (an ion channel which shows selective permeability to calcium ions)
- MAP kinases (involved in cellular responses to various stimuli and regulate cell growth, cycling, differentiation, mitosis and apoptosis).
The response of bone to mechanical appeals will depend on the quality of these appeals, both in terms of intensity and of frequency. Because of desensitization of the system with continuous loading, intermittent activity is expected and has been shown to be more efficient. The response will also depend on the sensitivity of the sensor, which decreases with age and is modulated by the hormonal environment, particularly estrogens.[3]A study in 2002 by Robling et. al. found that participants gained more bone mass by breaking up loading sessions into multiple smaller sessions separated by recovery periods compared with those completing all loading in single uninterrupted sessions [4].
Osteogenic Loading[edit | edit source]
When just standing upright, the simple act of resisting gravity puts a load on bone, but our body is well adapted to this load. To build stronger bones, a much higher load — that is, greater compression and bending — is needed to encourage our bodies to spend the necessary energy and resources.
The load put on bone can be measured in terms of multiples of body weight. The higher the load, the better able the activity is to stimulate bone growth.Most physical activity loads bone to a degree, but for strong osteogenic stimulation, the load needs to reach around 4 times body weight. Calculations of multiples of body weight look like this for common physical activities:
- Swimming: 0 (Your load is actually lessened in water.)
- Standing: 1
- Brisk walking : 1–2
- Running/jogging: 3–4
- Power jumping: 4+
- Resistance, strength training: 4 to 10 (Depending on impact.)[5]
What Does This Mean for the Physiotherapist?[edit | edit source]
Most physical activity loads bone to a degree, but for strong osteogenic stimulation, the load needs to reach around 4 times body weight.- At these higher multiples of body weight, however, safety becomes an issue. Any bone will succumb to fracture under loads that exceed its capacity. When training with high multiples of body weight, professional guidance is mandatory.
- Many safe impact training programs have been shown to build bone
- Besides the effect of physical activity on bone, it also affects muscle mass and force, an effect which will contribute to fall and fracture prevention.[3][5]
References[edit | edit source]
- ↑ Gusmão CVB de, Belangero WD. HOW DO BONE CELLS SENSE MECHANICAL LOADING? Revista Brasileira de Ortopedia. 2009;44(4):299-305. doi:10.1016/S2255-4971(15)30157-9.
- ↑ Mellon SJ, Tanner KE. Bone and its adaptation to mechanical loading: a review. International Materials Reviews. 2012 Sep 1;57(5):235-55.Available: https://www.tandfonline.com/doi/full/10.1179/1743280412Y.0000000008(accessed 17.6.2021)
- ↑ 3.0 3.1 Bergmann P, Body JJ, Boonen S, Boutsen Y, Devogelaer JP, Goemaere S, Kaufman J, Reginster JY, Rozenberg S. Loading and skeletal development and maintenance. Journal of osteoporosis. 2011 Jan 1;2011.Available: https://www.hindawi.com/journals/jos/2011/786752/#summary-and-conclusion(accessed 17.6.2021)
- ↑ Klein-Nulend J, Bacabec RG, Bakker AD. Mechanical loading and how it affects bone cells:the role of the osteocyte cytoskeleton in maintaining our skeleton. Eur Cell Mater. 2012;24(24):278-91
- ↑ 5.0 5.1 Better bones OL Available : https://www.betterbones.com/exercise/osteogenic-loading/ (accessed 17.6.2021)