Ketoacidosis
Original Editor - Lucinda hampton
Top Contributors - Lucinda hampton
Introduction[edit | edit source]
Ketoacidosis is a metabolic state associated with pathologically high serum and urine concentrations of ketone bodies[1]. Ketoacidosis is an acute, life-threatening condition[2].[3]
Clinically relevant forms of ketoacidoses include:
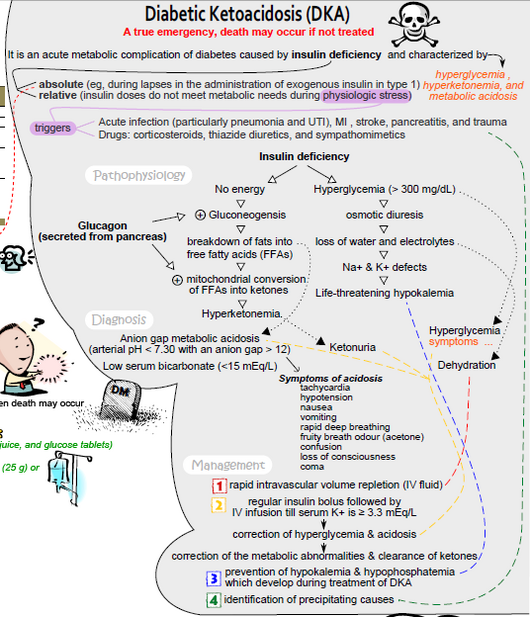
- Diabetic ketoacidosis(DKA) is a potentially life-threatening complication of uncontrolled diabetes.
- Alcoholic ketoacidosis (AKA) occurs in patients with chronic alcohol abuse, liver disease, and acute alcohol ingestion.
- Starvation ketoacidosis occurs after the body is deprived of glucose as its primary source of energy for a prolonged time, causing fatty acids to replace glucose as the major metabolic fuel.[1]
Etiology[edit | edit source]
- DKA can occur in patients with diabetes mellitus, most frequently associated with relative insulin deficiency. This may be caused by precipitating physiologic stress or, in some cases, maybe the initial clinical presentation in patients with previously undiagnosed diabetes. Some of the more common risk factors that can precipitate the development of extreme hyperglycemia and subsequent ketoacidosis are infection, non-adherence to insulin therapy, acute major illnesses like myocardial infarction, sepsis, pancreatitis, stress, trauma, and the use of certain medications eg glucocorticoids or atypical antipsychotic agents, which have the potential to affect carbohydrate metabolism.[1]
- AKA occurs in patients with chronic alcohol abuse. Patients can have a long-standing history of alcohol use and may also present following binges. Acetic acid is a product of the metabolism of alcohol and also a substrate for ketogenesis. The conversion to acetyl CoA and subsequent entry into various pathways or cycles, one of which is the ketogenesis pathway is determined by the availability of insulin in proportion to the counter-regulatory hormones.
- Under normal conditions, cells rely on free blood glucose as the primary energy source, which is regulated with insulin, glucagon, and somatostatin. As the name implies, starvation ketoacidosis (eg eating disorders) is a bodily response to prolonged fasting hypoglycemia, which decreases insulin secretion, shunting the biochemistry towards lipolysis and the oxidation of the by-product fatty acids to ensure a fuel source for the body[1].
Epidemiology[edit | edit source]
- DKA is usually associated with type 1 diabetes mellitus but is not uncommon in some patients with type 2 diabetes mellitus. Approximately 30% of children and adolescents with a new diagnosis of type 1 diabetes present with diabetic ketoacidosis at their first presentation[2]
- For AKA, the prevalence correlates with the incidence of alcohol abuse without racial or gender differences in incidence. It can occur at any age and mainly in chronic alcoholics but rarely in binge drinkers.
- For starvation ketosis, mild ketosis generally develops after a 12- to 14-hour fast. If there is no food source, as in the case of extreme socio-economic deprivation or eating disorders, this will cause the body’s biochemistry to transform from ketosis to ketoacidosis progressively. It can be seen in cachexia due to underlying malignancy, patients with postoperative or post-radiation dysphagia, and prolonged poor oral intake.[1]
Presentation[edit | edit source]
On physical exam, most of the patients with ketoacidoses present with features of hypovolemia from gastrointestinal or renal fluid and electrolyte losses. In severe cases, patients may be hypotensive and in frank shock. They may have a rapid and deep respiratory effort as a compensatory mechanism, known as Kussmaul breathing. They may have a distinct fruity odor to their breath, mainly because of acetone production.[1]
- DKA: Without enough insulin, the body’s cells cannot use glucose for energy. To make up for this, the body begins to burn fat for energy instead. This leads to accumulation of dangerous chemical substances in the blood called ketones, which also appear in the urine. High blood glucose levels and moderate to heavy ketones in the urine with:
- Rapid breathing
- Flushed cheeks
- Abdominal pain
- Sweet acetone (similar to paint thinner or nail polish remover) smell on the breath
- Vomiting
- Dehydration[3].
- In a small number of children, DKA is complicated by injury of the central nervous system. These children have a significant mortality and high long-term neurological morbidity. Cerebral edema is the most common neuroimaging finding in children with DKA and may cause brain herniation..[4]
2. AKA patients may have signs of withdrawal like hypertension and tachycardia.
3. There are signs of muscle wasting in patients with starvation ketoacidosis like poor muscle mass, minimal body fat, obvious bony prominences, temporal wasting, tooth decay, sparse, thin, dry hair and low blood pressure, pulse, and temperature[1].
Treatment[edit | edit source]
- DKA is a medical emergency and institutions will often have set protocols regarding urgent management. However, the principles of treatment should be the same:
- Correction of volume depletion with the administration of intravenous fluids
- Correction of hyperglycaemia with a short-acting insulin infusion
- Potassium replacement and correction of other electrolytes
- Search for the underlying cause
The overall mortality rate for diabetic ketoacidosis is 2.5-5% in developed countries.[2]
2. AKA typically responds to treatment with intravenous saline and intravenous glucose, with rapid clearance of the associated ketones due to a reduction in counter-regulatory hormones and the induction of endogenous insulin. Thiamine replacement is important in alcohol-related presentations. Electrolyte replacement is critical.[1]
3, The treatment of starvation ketoacidosis is similar to AKA. Patients need to be monitored for refeeding syndrome, which is associated with electrolyte abnormalities seen when aggressive feeding is started in an individual starved for a prolonged time. The resultant insulin secreted causes significant transcellular shifts, and hence similar to AKA, monitoring and replacing potassium, phosphate, and magnesium is very important.[1]
Physiotherapy[edit | edit source]
The treatment of ketoacidosis is dictated by the specific pathophysiology of the diagnosis. Regardless of the specific etiology, it is imp0rtant for a physical therapist to be aware of the condition.
DKA relevance:
- Educate clients about DKA.
- Maintaining proper glucose levels can prevent DKA.
- Physical therapists are in a unique position because of the amount of time we spend with patients, and it is imperative that we play a role in monitoring their well-being and are aware of the signs of DKA
Ketogenic Diet[edit | edit source]
The ketogenic diet is made possible by forcing the body into a state of ketosis. This occurs due to eating a very low amount of carbohydrates and eating a very high amount of fat-rich foods. Instead of using glucose from the carbohydrates, the body will now move to using the high amount of fat stored in the body for energy. This diet is often used by people to help them lose weight.
There have been cases of ketoacidosis induced by keto dieting and consumption of ketone supplements. Although some studies have shown significant weight reduction with the implementation of a ketogenic diet, the adverse consequences of such dieting must be highlighted. In at-risk patient populations such as those with diabetes and/or CKD, the use of exogenous ketone supplements, not often regulated to the same extent as Food and Drug Administration-approved medications, must be cautioned. Clients should be counseled on the dangers of taking these weight loss supplements that are unregulated[5].
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 1.7 1.8 Ghimire P, Dhamoon AS, Doerr C. Ketoacidosis (Nursing).2021 Available:https://www.ncbi.nlm.nih.gov/books/NBK534848/ (accessed 24.9.2021)
- ↑ 2.0 2.1 2.2 Radiopedia DKA Available: https://radiopaedia.org/articles/diabetic-ketoacidosis(accessed 24.9.2021)
- ↑ 3.0 3.1 Diabetes Australia Ketoacidosis Available: https://www.diabetesaustralia.com.au/living-with-diabetes/managing-your-diabetes/ketoacidosis/ (accessed 24.9.2021)
- ↑ Barrot A, Huisman TA, Poretti A. Neuroimaging findings in acute pediatric diabetic ketoacidosis. The neuroradiology journal. 2016 Oct;29(5):317-22.Available:https://journals.sagepub.com/doi/10.1177/1971400916665389 (accessed 24.9.2021)
- ↑ Malhi MS, Duerson F, Salabei JK, Okonoboh P. Starvation Ketoacidosis Induced by Ketogenic Diet and Consumption of Ketone Supplement. Cureus. 2021 Jun 20;13(6).Available:https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8291511/ (accessed 24.9.2021)