Introduction to Human Biomechanics - Internal Forces
Original Editor - Tolulope Adeniji Top Contributors - Pierre Roscher, Tarina van der Stockt, Tolulope Adeniji, Lucinda hampton, Kim Jackson and Jess Bell
Introduction[edit | edit source]
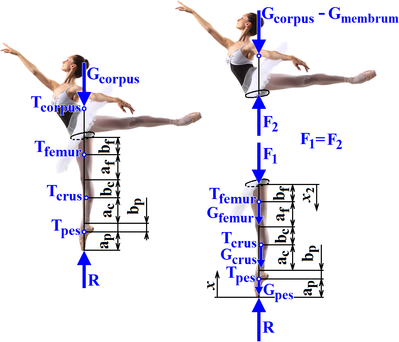
When external forces act on a body segment to produce posture and movement, the internal structures of the specific body segment responds by generating specific forces to counter the external forces, thereby producing a specific desired posture or movement.
Image 1: Ballerina standing on tiptoe (En pointe). Biomechanics - application of the imaginary incision method and simplified force analysis in the lower limb.
Understanding the mechanical properties of these internal structures will enable physiotherapists to evaluate causes of injury that are movement-related, and more importantly, how to prevent it.
When external forces act on a body segment for movement and posture, the body tissue also responds by generating forces to interact for the desired posture and movement[1].
- Stress: The internal resistance, or counter force, of a material to the distorting effects of an external force or load. The total resistance developed is equal to the external load.
- Strain: The relative change or deformation in the shape of the structure that accompanies the stress[2]. Dense connective tissue may display a wavy configuration under a microscope referred to as the crimp, or the crimp properties of connective tissue[2].
Viscoelastic Properties[edit | edit source]
Definition - Dense connective tissue: Relative abundance of the collagen fibers, contains fewer cells and less ground substance in comparison with the other type, loose connective tissue. A property of dense connective tissue is its viscoelastic properties. This property allows a dense connective tissue fibre to temporarily elongate in length and once the stress is removed, to return to its original length.
- Compliance: The temporary elongation of dense connective tissue is referred to as compliance.
- Elasticity: The ability of the tissue to return to its original length after the stress is removed is referred to as elasticity.
These activities occur at the physiological limit and the crimp property of a related collagen fibre is removed when dense connective tissues are elongated[2][3]. Thus, it is important to consider this physiological limit when stretching a dense connective tissue, as well as the stress-strain curve that will give us some indication of its physiologic limit[2].
Please see tendon biomechanics on Physiopedia for more information on the viscoelastic properties of dense connective tissue.
Stress-Strain Curve[edit | edit source]
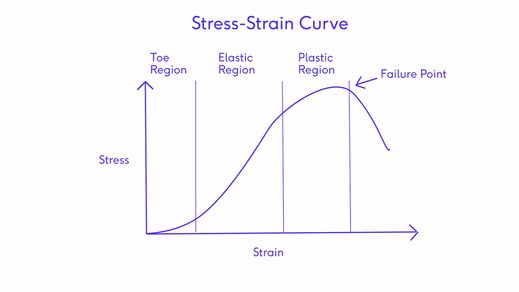
The stress-strain curve is a graph that shows the change in stress as strain increases when connective tissue undergoes tension( also known as the load-deformation curve).
Based on the force applied to a specific tissue, the stress-strain curve can be explained using four specific regions or phases on a graph namely: 1. the toe, 2. elastic, 3. plastic and 4. the ultimate failure point[2].
- At the toe region of the curve, the crimp straightens when collagen fibres begin to stretch as phase 2 begins (elastic phase).
- The force application to collagen in the elastic phase causes a residual change in the tissue structure.
- If this force persists, the tissue may rupture at its ultimate failure point [2].
The stress-strain curve is applicable in manual therapy eg
- Early rehabilitation of a joint should focus on joint proprioception. This would be achieved by mobilising the joint tissue within the toe region of the stress-strain curve.[4][5] In this phase, the tissue crimp can be removed without any trauma and it is at this phase that type 1 to 111 mechanoreceptors are most active. Any further stress on the connective tissue to the point of eliciting type iv receptors (that is a nociceptive pain) suggests that the tissue mobilisation is no longer at a normal physiologic limit[4].
- The concept of the stress-strain curve is also essential in understanding the interaction between dense connective tissue constituents and the physical mechanisms when stretching and nerve sliding, as these govern material behaviour at and between tissue length scales[5][6].
It is essential to understand details of the concept of load transfer and damage, from the molecular to the tissue level, in order to deliver an effective intervention and practice safely.
Human Skeletal System[edit | edit source]
The skeletal system is a biomechanics system of rigid links that are connected to each other at joints, to allow specific movements. The human skeletal system comprises of bones, tendons, ligaments and connective tissue. Muscles are attached to bones to provide forces and to generate movement. It is important to understand the biomechanical properties of skeletal system elements to understand human motion. More importantly, the nature of musculoskeletal interconnection enhances human stability, voluntary movement, and robustness to injury[7].
Biomechanical Properties of Bone[edit | edit source]
Bone is a highly specialised connective tissue, and a biological composite. It is composed of two types of bony tissues
- Cortical bone ( also known as compact bone): forms the walls of the bone and it is dense (5%–30% porous) and stiff,[8]
- Cancellous bone ( also known as spongy bone): occupies the central space within the bone, which is less dense (90% porous), but considerably more malleable[8][9].
Bone has great compressive, tensile, viscoelastic and shear strength and this biomechanical property of bone makes the human skeleton very well suited for its function to support body load and to move body segments.
Biomechanical Properties of Human Joints[edit | edit source]
A joint can be defined as the area where two or more bones meet.
- A joint's primary function is to allow motion and force transferal. These two functions led to interesting structural designs of joints.
- Human joint materials include bones, bursae, capsules, cartilage, ligament, tendon and other associated materials.
The materials comprising human joints are composed of living tissue, which makes human joints unique. This uniqueness includes the ability of the tissue to respond to environmental changes or functional demands[2].
Joint Classification[edit | edit source]
Anatomists have categorised joints in several ways. Some of these classifications are based on joint complexity, the number of axes present, joint geometry, or joint movement capabilities. Human biomechanics is more concerned with kinesiologic motion that occurs in a joint. The focus of the joint classification system is based on joint motion capabilities.
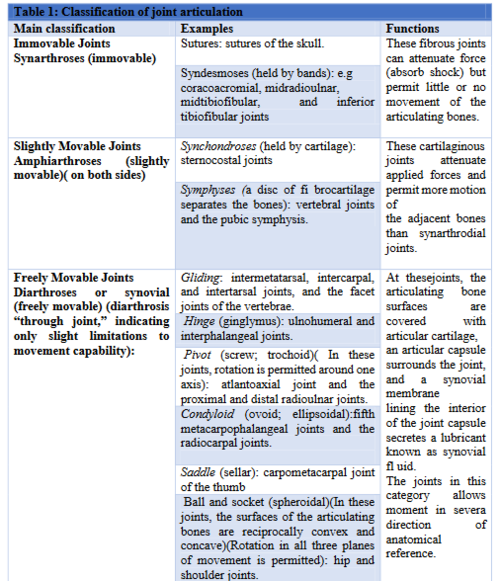
See Table R: Classification of Joints
There are three major categories of joint classifications 1. synarthroses e.g. suture joints in the skull2. amphiarthroses e.g. pubic symphysis 3. diarthrosis e.g. hinge joint and ball and socket joint .
Joint Surfaces[edit | edit source]
The nature of movement at any joint is largely determined by the joint structure, especially the shapes of the joint surfaces. The traditional classification of synovial joints by structure includes the categories of spheroid, trochoid, condyloid, ginglymoid and ellipsoid joint[4].
Limitations in the Anatomical Joint Description[edit | edit source]
The anatomical classification of joints is deficient in explaining the finer details of mechanical properties of a joint structure, and those details may be useful to clinicians who are considered movement specialist eg physiotherapist[4].
- Joint surfaces are neither truly spheres, ovals, nor ellipses.
- Any joint surface can be thought of as being part of an ovoid surface, that is, resembling the surface of an egg.
- An example: a hinge joint under diarthrosis, such as the humeroulnar joint, does not allow a true hinge motion of flexion and extension, but rather a helical movement involving considerable rotation.
Traditional classification of joint movements such as sliding, angular, rotation and circumduction ignore movement occurring between joint surfaces, meaning that when movement is defined, what happens at that joint surface is often ignored[4]. Therefore, it is essential to classify joints into specifics of joint movement occurring between bones and between respective joint surfaces. This leads us to the concept of osteokinematic and arthrokinematic movement.
Osteokinematic and Arthrokinematic[edit | edit source]
Kinematic motion is described by the terms osteokinematic and arthrokinematic motion[10].
- Osteokinematics deals with the angular/rotary movement occurring between two bones at synovial joints. This movement is described in terms of its direction, plane, and axis of motion. [10] This movement can be measured by a goniometer, flexion / extension, abduction / adduction and internal rotation / external rotation. These movements occur about a joint mechanical axis. The mechanical axis refers to a line that passes through the moving bone, touching the centre of the relatively stationary joint surface and lying perpendicular to it.
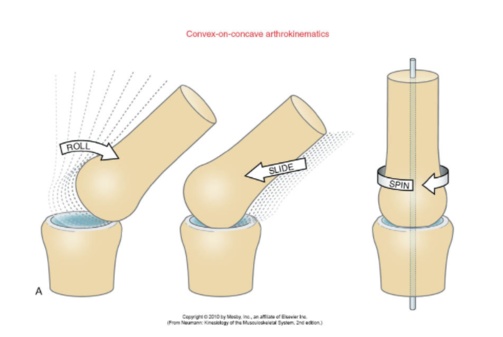
- Arthrokinematic movements are also called accessory movements. This is the relative movement of joint surfaces in relation to each other when osteokinematic movement occurs. Arthrokinematic movement includes rolling, gliding and spinning[10].
- Rolling is when a joint surface moves in relation to the other surface during angular motion. The roll happens in the direction of the osteokinematic movement. New points on the rolling surface will contact new points on the other surface as rolling occurs.
- Gliding/sliding is the translation movement of one joint surface on another joint surface. This means that one point of the moving joint surface will contact multiple points on the other joint surface.
- Spinning is a pure rotation movement. During spinning, multiple points of the moving joint surface will contact one point on the stationary joint surface. [10]
For joint integrity a combination of rolling and gliding will normally occur.[10] If joint surface “A” rolls on the opposing joint surface “B”, the joint surface “A” will move at different points of contact on the corresponding opposing joint surface “B” at the same intervals. For example, the tyre of a car needs to roll on different points on the ground before the motion takes place. If, however, only one point on the moving joint surface contacts various points on the opposing surface, slide is said to have taken place. This analogy could be made to a car tyre that is skidding on ice. The tyre is not turning but is moving relative to the road surface.
One clinical implication of this is that a joint movement that occurs in the absence of normal arthrokinematics will cause either impingement or dislocation[4]. More so, principles of osteokinematic and arthrokinematic are essential in relieving adhesive joints. Recent findings note that when a patient with shoulder adhesive capsulitis was managed with angular joint mobilization, a form of osteokinematic approach, there was an improvement in shoulder pain, ROM, and disability[11]. Another paper showed that consideration of osteokinematic in a lateral ankle sprain is essential to improve its ROM[12].
Concave-Convex Rule[edit | edit source]
An important concept from arthrokinematics is the concave-convex rule. The concave-convex rule states that if a concave surface moves on a convex surface, roll and slide must occur in the same direction, and if a convex surface moves on a concave surface, roll and slide occurs in opposite directions. Clinicians like physiotherapists may need to apply this concept to the restoration of restricted joint motion, by considering roll and slide motion alongside the traditional anatomical motion of the joint that is involved[4]. For example, if flexion of the humerus is restricted, in addition to active or passive motion into flexion to increase this movement, one must also consider inferior glide of the head of the humerus on the glenoid cavity, as it may be restricted as well. Thus, by knowing the concave-convex rule, the therapist knows in which direction to apply joint slide mobilisations to increase any restricted swing of a bone[4].
Closed and Open/Loose-Packed Position[edit | edit source]
Joint stability is the ability of the joint to resist the displacement of the articulating bones. Although most joints have asymmetrical surfaces, there is typically one position where the area of contact is at its maximum. This is known as the closed-packed position, and it is in this position that joint stability and congruency is the greatest. In this position, the capsules and ligaments are maximally tight and there is limited accessory movement
Any movement of the bones at the joint away from the closed-packed position results in a loose-packed position, with a reduction of stability and less area of contact[13]. The loose-packed position is also called the open packed-position. A joint's loose-packed position is the position with the least amount of congruency where the capsule and ligaments are lax and joint play (accessory movement) is optimised[14].
Application of Close and Loose-Packed Position Concept[edit | edit source]
This concept is applied to joint distraction and compression. A distraction occurs when there is a separation of joint surfaces while approximation of opposing surfaces is compression. The principle here is that a movement toward the close-packed position has an element of compression, whereas movement out of this position involves distraction. Hertling et al[4] noted that the concept of close and loose-packed position of a joint will help clinicians like physiotherapists understand joint stability and to know when to apply joint distraction and compression when exercising a joint.
As an example, the loose-packed position of the knee is at 25 degrees flexion in a non-weight-bearing position. This means the knee is 'unlocked' and easy to perform the knee ligament stress tests or assess tibial IR/ER.[14] The close-packed position for the knee is in full extension[14].
Joint Flexibility[edit | edit source]
It is important for clinicians to know that joint flexibility is primarily a function of the relative tightness of the muscles and ligaments that span the joint. If these tissues are not stretched, they tend to shorten. Approaches for increasing flexibility include active versus passive stretching, static versus dynamic stretching and proprioceptive neuromuscular facilitation (PNF). Amongst these approaches, PNF is one of the most effective procedure for stretching muscles and ligaments. This is because all PNF patterns involve some pattern of alternating contraction and relaxation of agonist and antagonist muscles for effective stretching.
Muscular System[edit | edit source]
Muscles exert forces on the bone to produce movement, and if the force exerted is aimed at maintaining a constant length, this is called an isometric action. The force exerted to contract the muscle for shortening is called concentric action, and the action to lengthen it is called an eccentric contraction. In concentric muscle action, there is positive mechanical work that is being done while in isometric muscle action, there is no mechanical work being done by isometric muscle action. Negative mechanical work is done by eccentric muscle action.
Skeletal Muscle Fibre Type[edit | edit source]
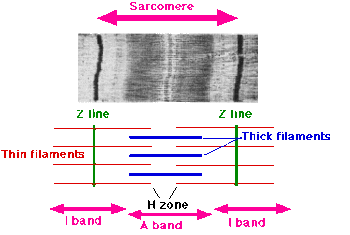
In a skeletal muscle fibre, the sarcomere is the fundamental structure and within it, the muscle generates active tension by cross-bridges of myosin filaments to actin filaments[15]. The rate of tension generated depends on the type of muscle fibre and skeletal muscle fibres differ in terms of their fatigue resistance, and rate of tension development. The muscle fibres are classified into three types according to these differences: type I, or slow-twitch oxidative (SO); type IIA, or fast-twitch oxidative-glycolytic (FOG), and type IIB, or fast-twitch glycolytic (FG).
Mechanical Characteristics of Muscle[edit | edit source]
There are three mechanical characteristics of muscle that are based on the variations in muscle force because of differences in velocity, length, and time relative to activation. The Force–Velocity relationship explains how the force of fully activated muscle varies with velocity. In the force-velocity relationship of a muscle that is shortening i.e concentric action, the force the muscle can create decreases with increasing velocity and vice versa for eccentric actions. Force–Time relationship describes a temporal delay in the development of tension. This temporal delay can be partly caused by a delay in the rise of muscle stimulation (active state or excitation dynamics ). Repeated firing of muscle fibres can cause a temporal delay in the time to develop tension. However. length of time to develop tension depends strongly on the cognitive effort of the subject, training, kind of muscle action, and the activation history of the muscle group.
Neuromuscular Control of Motion[edit | edit source]
The mechanical response of muscles also strongly depends on how the muscles are activated. The basic functional unit of neuromuscular control includes the motor unit, recruitment and firing rate. A motor unit is one motor neuron and all the muscle fibres it innervates. While recruitment is the activation of different motor units within a muscle and firing rate is the repeated stimulation of a particular motor unit over time. A tetanic muscle contraction occurs when there is a sustained muscle contraction induced when the motor nerve innervates a skeletal muscle produces action potential at a very high rate.
Neuromuscular control of motion is one of the concepts in designing neuromuscular exercise for neuromuscular impairments. A recent study had shown that patients who have anterior shoulder dislocations with shoulder mechanical loss and proprioceptive impairment improve with shoulder instability neuromuscular exercise[16]. Another recent paper also noted that neuromuscular control exercises are essential in pivoting related injuries and that they improve lower limb functions among patients with pivoting related movement disorders such as cerebral palsy, stroke, and incomplete spinal cord injury[17].
Proprioception of Muscle Action and Movement[edit | edit source]
What is proprioception? Charles Sherrington first used the term proprioception and described it as “the perception of joint and body movement as well as the position of the body, or body segments, in space”[18]. In a muscle, muscle spindles are proprioceptive stretching receptors, and they are responsible for the stretch reflex or myotatic reflex. Static reflex is a muscle contraction in response to stretching within the muscle. The muscle spindle is sensitive to slow stretching of the muscle, but provides the largest response to rapid stretches[18]. Physiotherapists can assist with restoring balance control and postural dysfunctional corrections in patients with neurological and or musculoskeletal impairments such as hemiparesis due to stroke, nerve impairments and soft tissue injuries. One way of achieving a significant functional improvement is through the use of PNF, as it uses proprioception for activating muscle action and movement. A recent paper has shown that PNF with transcutaneous electrical nerve stimulation improves pain, ROM and balance in patients with ankle sprains[19]. PNF techniques have also proven to be effective in stroke rehabilitation[20].
Reciprocal Inhibition[edit | edit source]
In reciprocal inhibition, the muscle spindles act in such a way to inhibit an opposing muscle action when the muscle of interest is shortening. This relaxation of an opposing muscle when the muscle of interest is shortening, contributes to the efficient movement of the muscle that is shortening. For e.g. when you contract your biceps, your triceps are inhibited to allow efficient elbow flexion.
Active and Passive Insufficiency[edit | edit source]
Another important concept of motion is active and passive insufficiency. Active insufficiency is the decreased tension of a multiarticular muscle when it is shortened across one or more of its joints. This concept implies that muscle shortening leads to low tension. In passive insufficiency, there is a limitation of joint motion when multiarticular muscles are stretched across multiple joints[21]. This concept is important in generating tension in muscle or to explain the limitation of a joint range of motion when multiarticular muscles like hamstrings and quadriceps are to be exercised.
Conclusion[edit | edit source]
Internal biomechanics knowledge is important, particularly to evaluate causes and prevention of movement-related injuries.
References[edit | edit source]
- ↑ McGinnis PM. Biomechanics of sport and exercise. 3rd. Human Kinetics; 2013.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 Levangie PK, Norkin CC. Joint Structure and function: a comprehensive analysis. 4th. Philadelphia: FA. Davis Company. 2005.
- ↑ Barrett JM, Callaghan JP. A one-dimensional collagen-based biomechanical model of passive soft tissue with viscoelasticity and failure. Journal of Theoretical Biology. 2020 Sep 12;509:110488.
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 4.6 4.7 4.8 Hertling D, Kessler RM. Management of common musculoskeletal disorders: physical therapy principles and methods. Lippincott Williams & Wilkins; 2006.
- ↑ 5.0 5.1 Zitnay JL, Weiss JA. Load transfer, damage, and failure in ligaments and tendons. Journal of Orthopaedic Research®. 2018 Dec;36(12):3093-104.
- ↑ Freedman BR, Rodriguez AB, Leiphart RJ, Newton JB, Ban E, Sarver JJ, Mauck RL, Shenoy VB, Soslowsky LJ. Dynamic loading and tendon healing affect multiscale tendon properties and ECM stress transmission. Scientific reports. 2018 Jul 18;8(1):1-3.
- ↑ Murphy AC, Muldoon SF, Baker D, Lastowka A, Bennett B, Yang M, Bassett DS. Structure, function, and control of the human musculoskeletal network. PLoS biology. 2018 Jan 18;16(1):e2002811.
- ↑ 8.0 8.1 Malik SS, Malik SS. Orthopaedic biomechanics made easy. Cambridge University Press; 2015 May 28.
- ↑ Walker J. Skeletal system 1: the anatomy and physiology of bones. Nursing Times. 2020 Feb;116(2):38-42.
- ↑ 10.0 10.1 10.2 10.3 10.4 Eric Shamus, Arie J. van Duijn. Manual Therapy of the Extremities [Internet]. Burlington, MA: Jones & Bartlett Learning; 2017
- ↑ Kim Y, Lee G. Immediate Effects of Angular Joint Mobilization (a New Concept of Joint Mobilization) on Pain, Range of Motion, and Disability in a Patient with Shoulder Adhesive Capsulitis: A Case Report. The American journal of case reports. 2017;18:148.
- ↑ Medina McKeon JM, Hoch MC. The ankle-joint complex: a kinesiologic approach to lateral ankle sprains. Journal of Athletic Training. 2019 Jun;54(6):589-602.
- ↑ Hall S. Basic biomechanics. 4th. McGraw-Hill Higher Education; 2014 Feb 7.
- ↑ 14.0 14.1 14.2 Importance of Open & Closed packed Positions. TSPT. 2015. Last Accessed 1 March 2021
- ↑ Zatsiorsky VM, Prilutsky BI. Biomechanics of skeletal muscles. Human Kinetics; 2012 Apr 10
- ↑ Eshoj HR, Rasmussen S, Frich LH, Hvass I, Christensen R, Boyle E, Jensen SL, Søndergaard J, Søgaard K, Juul-Kristensen B. Neuromuscular Exercises Improve Shoulder Function More Than Standard Care Exercises in Patients With a Traumatic Anterior Shoulder Dislocation: A Randomized Controlled Trial. Orthopaedic Journal of Sports Medicine. 2020 Jan 30;8(1):2325967119896102.
- ↑ Lee SJ, Zhang LQ. Learning Patterns of Pivoting Neuromuscular Control Training–Toward a Learning Model for Therapy Scheduling. IEEE Transactions on Biomedical Engineering. 2018 May 30;66(2):383-90.
- ↑ 18.0 18.1 Han J, Waddington G, Adams R, Anson J, Liu Y. Assessing proprioception: a critical review of methods. Journal of Sport and Health Science. 2016 Mar 1;5(1):80-90.
- ↑ ALAHMARI KA, Samuel PS, Ahmad I, Reddy RS, Tedla JS, Kakaraparthi VN, Rengaramanujam K. Effectiveness of Low-Frequency Stimulation in Proprioceptive Neuromuscular Facilitation Techniques for Post-Ankle-Sprain Balance and Proprioception in Adults-a Randomized controlled trial.
- ↑ Chaturvedi A. Effect of proprioceptive neuromuscular facilitation in functional recovery of patients with stroke–a review. J Neurol Neurosci. 2017;8(5):220.
- ↑ Knudson D. Fundamentals of biomechanics. Springer Science & Business Media; 2007 May 28.