Introduction to Cervicogenic Headaches
Introduction[edit | edit source]
Headaches are highly prevalent and are associated with significant disease burden for the individual and the wider community. Headache disorders are ranked as the third most disabling condition in people aged under 50 years old in the Global Burden of Disease Study.[1]
A global prevalence of active headache disorder in high-income countries is 52.0%.[2] Between 1.7 and 4 percent of the world’s adult population report having a headache on 15 or more days each month.[3] While there are regional variations, headaches affect people from all ages, ethnicities, socio-economic backgrounds and geographical areas.[3] The highest rates for headache are found in North America with 85 to 90 percent of people reporting that they have experienced a headache at some point in time.[4]
There are many different types of headache, which are discussed in more detail here.
Headaches are grouped into three main areas:[5]
- Primary headaches (e.g. migraine, tension-type headaches, and trigeminal autonomic cephalalgias (including cluster headaches))
- Secondary headaches (e.g. cervicogenic headache)
- Neuropathies, facial pain and other headaches
Tension-Type Headaches[edit | edit source]
Tension-type headaches (TTH) is the most common neurological disorder, but its pathophysiology is not well understood.[6] It is characterised by recurrent bilateral headaches of mild to moderate intensity, which does not change with routine physical activity. [7] Lifetime prevalence in the general population ranges from 30 and 78 percent.[5]
- The cause of TTH is not known, but peripheral pain mechanisms are believed to play a role in episodic TTH, whereas central pain mechanisms are implicated in chronic TTH.[5]
- Steel et al. note that individuals with TTH "tend to have muscles that are harder, more tender to palpation, and may have more frequent trigger points of tenderness than patients without headache. However, cause and effect of these muscular findings are unclear."[6]
- The ICHD-3 notes that "pericranial tenderness is easily detected and recorded by manual palpation".
Further information on TTH is available here.
Migraine[edit | edit source]
Migraine also has a high prevalence, affecting over 1 billion people throughout the world,[8] as well as socio-economic and personal burden.[5]
There are two major types of migraine:
- Migraine with aura: "primarily characterized by the transient focal neurological symptoms that usually precede or sometimes accompany the headache"[5]
- recurrent attacks, which last minutes
- "unilateral fully reversible visual, sensory or other central nervous system symptoms that usually develop gradually and are usually followed by headache and associated migraine symptoms."[5]
- Migraine without aura: "a clinical syndrome characterized by headache with specific features and associated symptoms"[5]
- recurrent headache disorder
- attacks tend to last 4–72 hours
- unilateral, pulsating quality, moderate to severe intensity, aggravated by routine physical activity, associated with nausea and / or phonophobia and photophobia[5]
Further information on migraine is found here.
Other more serious causes of headache include:[9][edit | edit source]
- Concussion
- Brain tumour
- Aneurysm
- Substance abuse
- Withdrawal
- Infection
- Inflammatory disease
Primary headaches and serious causes of headaches are explained in the following video.
Cervicogenic Headache[edit | edit source]
Cervicogenic headache (CGH) is a chronic secondary headache that originates in the cervical spine.[11] It affects 2.5 to 4.1 percent of the general population.[4] However, this figure rises to 15 to 20 percent of people who report headaches.[11][12] There is evidence to suggest that it has a similar impact on the quality of life as migraine and episodic tension-type headache.[11]
CGH is described by the ICHD-3 as "Headache caused by a disorder of the cervical spine and its component bony, disc and/or soft tissue elements, usually but not invariably accompanied by neck pain."[5] Their full diagnostic criteria are available here.
It is important to note that while various "clinical criteria have been promoted for the diagnosis of cervicogenic headache, [...] none have been fully validated. On clinical grounds alone, a diagnosis might, at best, be rendered of “possible” cervicogenic headache or “probable” cervicogenic headache."[13]
However, CGH has the following features. It begins in the neck or occipital region and can refer to the face and head. The specific sources of CGH are any structures innervated by the C1 to C3 nerve roots, including:[14]
- the upper cervical joints
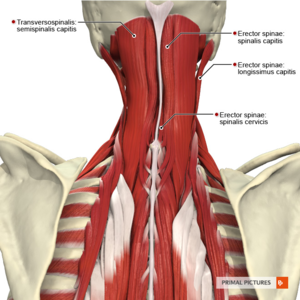
- the upper cervical muscles (see figure 1)
- suboccipital muscles
- sternocleidomastoid
- trapezius (especially the upper fibres)[9]
- the C2-3 disc
- the vertebral and internal carotid arteries
- the dura mater of the upper spinal cord and posterior cranial fossa
This referral of pain to the head from the neck can be explained by the convergence (overlap) of the trigeminal afferents and cervical afferents from the upper three cervical spinal nerves.[11][14][15].
- The trigeminal nucleus caudalis descends down to C3 or C4. This nucleus borders the grey matter of the spinal dorsal horn (i.e. the trigeminocervical nucleus)
- The interneurons in the trigeminocervical nucleus enable sensory information to be exchanged between the upper cervical spinal nerves and the trigeminal nerve
- Through this exchange, nociceptive signals from the upper cervical spine can be referred to the areas supplied by the trigeminal nerve in the head and face[14]
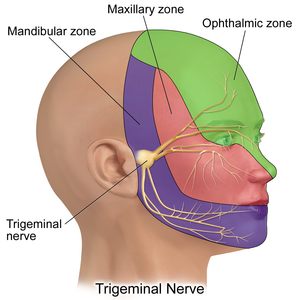
Most of this nociceptive information is exchanged through the ophthalmic division of the trigeminal nerve (cranial nerve V) (see figure 2). Thus, pain generated in the cervical spine will most likely refer to the temple, orbit and forehead.[14]
There is also some exchange of sensory information with the maxillary division of cranial nerve V, so pain generated in the upper cervical spine can also be referred to the face.
Neck muscles can also refer pain to the head and face.[14]
This optional video describes in detail the neurophysiology of cervicogenic headaches.
Distinguishing Headache Types[edit | edit source]
Despite clear criteria to classify cervicogenic headache, it remains difficult to diagnose this condition.[11]
"The diagnosis of cervicogenic headache (CGH) remains a challenge for clinicians as the diagnostic value of detailed history and clinical findings remains unclear."[17]
The following points can be helpful when trying to distinguish between migraine, tension-type headache and CGH.[9]
Location[edit | edit source]
- CGHs are usually unilateral. Pain occurs more frequently in the suboccipital region,[18] although they can also refer to the orbital and frontal regions.[9]
- Migraines also tend to be unilateral,[19] but they can shift from side to side.[9] Pain is more frequently in the frontal and temporal regions,[18] although they can also be orbital.[9] This means that there is some overlap with CGH.
- Tension-type headaches tend to be more diffuse and people often describe it as a sense of pressure like a headband. They originate in the temporal region.[9][20][21]
Type of Pain[edit | edit source]
- CGHs tend to be non-throbbing and often start in the neck.[9]
- Tension-type headaches are described as a pressing or tightening pain, of mild to moderate intensity.[21]
- Migraines are described as a pulsating headache.[19]
Triggers[edit | edit source]
CGHs are triggered by neck postures or movements.[22] There are multiple courses for tension headaches and migraines, but they are not typically related to neck movements.[9]
Additional Symptoms[edit | edit source]
Patients with CGH will more likely present with limited neck range of motion.[9]A 2021 systematic review and meta-analysis by Anarte-Lazo et al.[23] found that individuals with cervicogenic headache had reduced range of rotation during the flexion rotation test compared to individuals with migraine.
Tension headache and migraines might present with sensitivity to light and sound (i.e. photophobia and phonophobia).[21] Migraines may also have additional symptoms of nausea and vomiting, as well as visual changes (aura) and can be aggravated by activity.[5]
The following table provides a summary of these points.[9]
| Cervicogenic Headache | Tension-Type Headache | Migraine | |
|---|---|---|---|
| Location | Unilateral
Occipital, orbital or frontal |
Diffuse
Can feel like a headband |
Unilateral, but can shift sides
Frontal, orbital, temporal |
| Pain type | Non-throbbing, usually starts in the neck | Dull or tightening, pressure | Throbbing, pulsating |
| Triggers | Neck movements | Multiple | Multiple |
| Additional Symptoms | Reduced neck range of motion | Photophobia, phonophobia | Nausea, vomiting. visual changes (aura), photophobia, phonophobia |
Diagnostic Difficulties[edit | edit source]
While there are clear classification systems for headaches, it has been suggested that an incorrect headache diagnosis may occur in as much as 50 percent of cases.[9][24]
In some instances, patients may be diagnosed with one type of headache (e.g. migraine or tension-type), but also have features of CGH. Thus, headaches are not always exclusive.[9] Tension-type headaches can occasionally have some cervical components.[9] And both migraine and tension-type headaches are often associated with neck pain (due to the convergence of the cervical and trigeminal nociceptive afferents in the trigeminocervical complex as discussed above).[15]
Diagnosis of cervicogenic headaches is discussed in more detail here.
Red Flags[edit | edit source]
Certain red flag conditions can be associated with headache, including:[9]
- Cranial artery dysfunction (i.e. cervical or carotid)
- Please see International Framework for Examination of the Cervical Region for more information
- Intracranial issues
- Upper cervical ligamentous laxity (i.e. transverse or alar ligaments)
Other red flags include:[25]
- Sudden onset of a new, severe headache
- A worsening pattern of a pre-existing headache that occurs without any obvious predisposing factors
- Headache that is associated with fever, neck stiffness, skin rash, and with a history of cancer, HIV, or other systemic illness
- Headache associated with focal neurologic signs other than a typical aura
- A moderate or severe headache that is caused by cough, exertion, or bending down
- New onset of a headache either during or after pregnancy
Red flags in relation to headaches and dizziness are discussed in more detail here.
Where red flags are present, a medical review is required. Please watch the following video if you want to learn more about red flags associated with headache.
Summary[edit | edit source]
- Headache disorders are highly prevalent and cause significant disability
- There are many different types of headaches. Some may respond to physiotherapy management, particularly those referring from the cervical spine
- Classifying and diagnosing headaches can be difficult despite the existence of classification systems
- Red flag conditions must be considered and ruled out prior to treatment
Further information on assessing and treating CGH can be found here.
Further information on headaches can be found here and here.
References[edit | edit source]
- ↑ Stovner LJ, Nichols E, Steiner T, Abd-Allah F, Abdelalim A, Al-Raddadi R et al. Global, regional, and national burden of migraine and tension-type headache, 1990–2016: a systematic analysis for the Global Burden of Disease Study 2016. The Lancet Neurology. 2018; 17(11): 954-76.
- ↑ Stovner LJ, Hagen K, Linde M, Steiner TJ. The global prevalence of headache: an update, with analysis of the influences of methodological factors on prevalence estimates. J Headache Pain. 2022 Apr 12;23(1):34.
- ↑ 3.0 3.1 World Health Organisation. Headache disorders. Available from: https://www.who.int/news-room/fact-sheets/detail/headache-disorders (accessed 1/12/2020).
- ↑ 4.0 4.1 Stovner Lj, Hagen K, Jensen R, Katsarava Z, Lipton R, Scher A et al. The global burden of headache: a documentation of headache prevalence and disability worldwide. Cephalalgia. 2007; 27(3):193-210.
- ↑ 5.0 5.1 5.2 5.3 5.4 5.5 5.6 5.7 5.8 5.9 Headache Classification Committee of the International Headache Society (IHS) The International Classification of Headache Disorders, 3rd edition. Cephalalgia. 2018; 38(1): 1-211.
- ↑ 6.0 6.1 Steel SJ, Robertson CE, Whealy MA. Current Understanding of the Pathophysiology and Approach to Tension-Type Headache. Curr Neurol Neurosci Rep. 2021 Oct 2;21(10):56.
- ↑ Ashina S, Mitsikostas DD, Lee MJ, Yamani N, Wang SJ, Messina R, Ashina H, Buse DC, Pozo-Rosich P, Jensen RH, Diener HC, Lipton RB. Tension-type headache. Nat Rev Dis Primers. 2021 Mar 25;7(1):24.
- ↑ Ashina M, Katsarava Z, Do TP, Buse DC, Pozo-Rosich P, Özge A, et al. Migraine: epidemiology and systems of care. Lancet. 2021 Apr 17;397(10283):1485-95.
- ↑ 9.00 9.01 9.02 9.03 9.04 9.05 9.06 9.07 9.08 9.09 9.10 9.11 9.12 9.13 9.14 9.15 Kaplan A. Introduction to Cervicogenic Headache Course. Plus , 2020.
- ↑ Armando Hasudungan. Headache - Overview (types, signs and symptoms, treatment). Available from https://www.youtube.com/watch?v=JMfmDAJo3qc [last accessed 2/12/2020]
- ↑ 11.0 11.1 11.2 11.3 11.4 Fernandez M, Moore C, Tan J, Lian D, Nguyen J, Bacon A et al. Spinal manipulation for the management of cervicogenic headache: A systematic review and meta‐analysis. Eur J Pain. 2020; 24(9): 1687-702.
- ↑ Page P. Cervicogenic headaches: an evidence-led approach to clinical management. Int J Sports Phys Ther. 2011;6(3):254-266.
- ↑ 13.0 13.1 13.2 Govind J, Bogduk N. Sources of cervicogenic headache among the upper cervical synovial joints. Pain Med. 2022 May 30;23(6):1059-65.
- ↑ 14.0 14.1 14.2 14.3 14.4 Biondi DM. Cervicogenic headache: mechanisms, evaluation, and treatment strategies. J Am Osteopath Assoc. 2000;100(9 Suppl): S7-14.
- ↑ 15.0 15.1 Castien R, De Hertogh W. A Neuroscience Perspective of Physical Treatment of Headache and Neck Pain. Front Neurol. 2019;10: 276.
- ↑ Physio Classroom. Cervicogenic Headache: Neurophysiology and Diagnosis. Available from: https://www.youtube.com/watch?v=eEey2CYFOaQ [last accessed 2/12/2020]
- ↑ Demont A, Lafrance S, Benaissa L, Mawet J. Cervicogenic headache, an easy diagnosis? A systematic review and meta-analysis of diagnostic studies. Musculoskelet Sci Pract. 2022 Dec;62:102640.
- ↑ 18.0 18.1 Uthaikhup S, Barbero M, Falla D, Sremakaew M, Tanrprawate S, Nudsasarn A. Profiling the Extent and Location of Pain in Migraine and Cervicogenic Headache: A Cross-sectional Single-Site Observational Study. Pain Med. 2020 Sep 11:pnaa282.
- ↑ 19.0 19.1 Burstein R, Noseda R, Borsook D. Migraine: multiple processes, complex pathophysiology. J Neurosci. 2015;35(17):6619-6629.
- ↑ Dent D. Headaches and Dizziness Course. Plus. 2020.
- ↑ 21.0 21.1 21.2 Chowdhury D. Tension type headache. Ann Indian Acad Neurol. 2012;15(Suppl 1):S83-S88.
- ↑ Jull G, Stanton W. Predictors of responsiveness to physiotherapy management of cervicogenic headache. Cephalalgia. 2005;25:101-108.
- ↑ Anarte-Lazo E, Carvalho GF, Schwarz A, Luedtke K, Falla D. Differentiating migraine, cervicogenic headache and asymptomatic individuals based on physical examination findings: a systematic review and meta-analysis. BMC Musculoskelet Disord. 2021 Sep 3;22(1):755.
- ↑ Pfaffenrath V, Kaube H. Diagnostics of cervicogenic headache. Funct Neurol. 1990; 5(2): 159-64.
- ↑ Hall T, Briffa K, Hopper D. Clinical evaluation of cervicogenic headache: a clinical perspective. J Man Manip Ther. 2008; 16(2): 73-80.
- ↑ Best Doctors. When To Consult A Doctor About Headaches. Available from: https://www.youtube.com/watch?v=GbMXq0TwrdM [last accessed 2/12/2020]