International Framework for Examination of the Cervical Region
Background[edit | edit source]
This page is based on the following:
Rushton A, Carlesso L, Flynn T, Hing W, Rubinstein S ,Vogel S, Kerry R. International Framework for Examination of the Cervical Region for Potential of Vascular Pathologies of the Neck Prior to Musculoskeletal Intervention: International IFOMPT Cervical Framework. International Federation of Orthopaedic Manipulative Physical Therapists (IFOMPT). 2023[1][2]
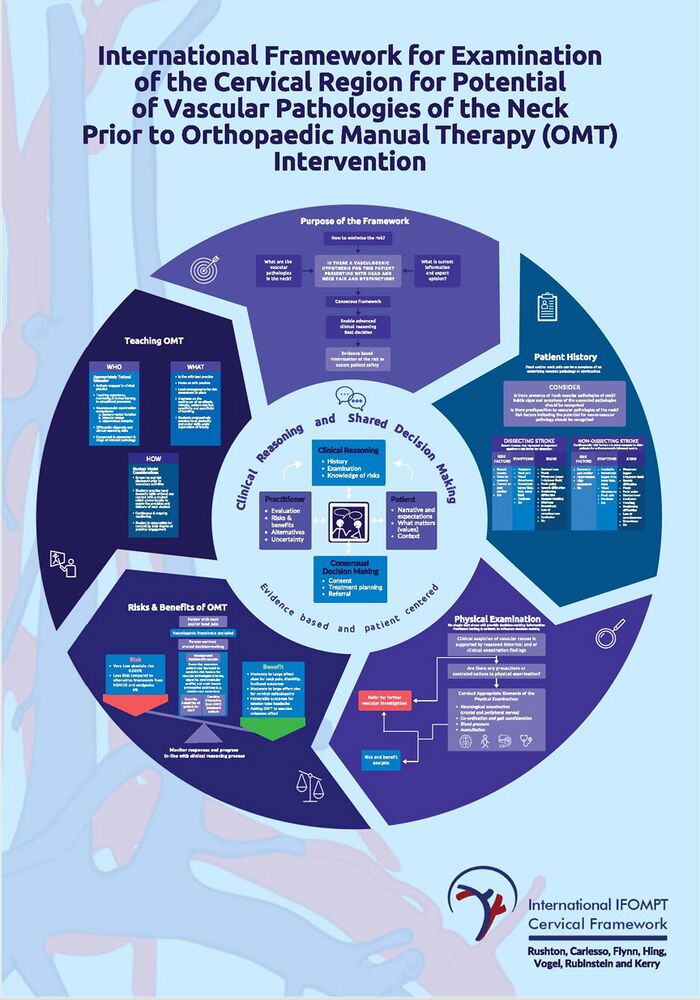
Based on the International IFOMPT (International Federation of Orthopaedic Manipulative Physical Therapists) Cervical Framework, this position statement was developed to assist clinicians during their clinical reasoning process when considering presentations involving the head and neck. It has moved from the IFOMPT language of “OMT” (orthopaedic manual therapy) to musculoskeletal intervention. This change ensured clarity for all clinicians and that the revised framework completes a planned update of the original (2012) framework to ensure access to contemporary evidence for clinical reasoning. The International IFOMPT Cervical Framework, developed through rigorous consensus methods, guides the assessment of the cervical spine region for potential vascular pathologies of the neck before planned interventions. However, using the Framework does not guarantee the identification of vascular pathologies. [3]
Events and manifestations of vascular pathologies of the neck are uncommon within the cervical spine, but they must be considered as part of the patient examination. Vascular pathologies may be detectable if the appropriate questions are asked during the patient history-taking process if the interpretation of elicited data allows recognition of this potential, and if the physical examination can be adapted to evaluate any potential vasculogenic hypothesis.[1] The document was published in 2012 as a resource for clinicians. It was scheduled for revision in 2017, and the final revision was published in September 2020. The revised 2020 framework is free on the IFOMPT website. As a consensus document, the Framework was developed through rigorous methods and pivots around clinical reasoning and evidence-based practice.
IFOMPT[edit | edit source]
Please visit www.ifompt.org for all information.
The vision statement of IFOMPT is as follows:
"World-wide promotion of excellence and unity in clinical and academic standards for manual/musculoskeletal physiotherapists."
The vision statement summarises the mission of IFOMPT that, as an organisation, it aims to:
- Promote and maintain high standards of specialist education and clinical practice in manual/musculoskeletal physiotherapists.
- Promote and facilitate evidence-based practice and research amongst its members.
- Communicate the purpose and level of the specialisation of manual/musculoskeletal physiotherapists amongst physiotherapists widely, other healthcare disciplines and the general public.
- Work towards international unity/conformity of educational standards of practice amongst manual/musculoskeletal physiotherapists.
- Communicate and collaborate effectively with individuals within and with other organisations.
The Standards Committee of IFOMPT is a sub-committee of the Executive Committee and is responsible for advising the Executive on educational issues and maintaining standards. The Standards Document is the guideline document that IFOMPT provides for groups of Manual Therapists who wish to seek membership in IFOMPT by creating postgraduate educational programmes in Orthopaedic Manual Therapy (OMT). Part A of the Standards Document[4]details the educational standards.
Consensus Methodology[edit | edit source]
The framework was developed through rigorous methods and is not intended to be a set of systematic reviews to answer specific questions. The consensus process looked at the breadth and complexity of the evidence and clinical reasoning and facilitated recommendations with a lack of published material and significant uncertainty.
Precisely defined substantive areas were identified for each section of the framework, and relevant electronic databases, reference lists, key journals, existing networks, and relevant organizations and conferences were searched. Within each section, study selection and data and information charting were carried out in accordance with its focus. There were four stages to developing the framework:
- Stage 1:
A survey to evaluate the previous 2012 cervical framework was distributed to all member organizations and registered interest groups of IFOMPT in 2016.
- Stage 2:
The key issues identified in the survey were initially explored at the IFOMPT Conference in 2016 in Glasgow. Findings from the evaluation survey were presented to facilitate discussion and debate through platform presentations, confirming the need for an updated version of the framework.
- Stage 3:
Drafts of the framework were developed through an iterative consultative process and distributed for review and feedback to IFOMPT member organizations. They registered interest groups, international experts/authors, nominated experts within IFOMPT countries, and professional organizations across physical therapy, osteopathy, and chiropractic.
- Stage 4:
The framework was voted on and accepted unanimously at the IFOMPT General Meeting in November 2020 by 22 member organizations (countries) as an international position statement for musculoskeletal clinicians.
Reason for the Development of the Framework[edit | edit source]
Although vascular pathologies of the neck and head are uncommon, they are an important consideration for clinicians treating patients with neck and/or head pain. Identifying vascular pathologies in this region is challenging. The arterial system, which supplies blood to the brain, can have a variety of vascular pathologies and dysfunctions. They are important for physiotherapists/physical therapists who treat musculoskeletal conditions in two ways:
- Neurovascular incidents have been associated with therapeutic interventions.
- There exist multiple arterial pathologies (vascular masqueraders) which could present as musculoskeletal pain and dysfunction of the neck, like neck pain and headache.
The International IFOMPT Cervical Framework aims to increase the physiotherapists' understanding of risk and pathology to promote patient safety and can help healthcare professionals working with cervical musculoskeletal conditions by promoting early detection of vascular pathologies, resulting in the best possible outcome for patients. It is based on the most recent evidence and expert opinion to help all clinicians with their clinical reasoning.
Aim of the framework[edit | edit source]
- The framework is designed to guide the assessment of the cervical spine region for the potential of vascular pathologies in the neck before planned OMT interventions. The IFOMPT definition of Orthopaedic Manual Therapy (OMT), voted in at the General Meeting in Cape Town in March 2004, is:
OMT is a specialised area of physiotherapy/physical therapy for the management of neuro-musculo-skeletal conditions, based on clinical reasoning, using highly specific treatment approaches including manual techniques and therapeutic exercises.
OMT also encompasses, and is driven by, the available scientific and clinical evidence and the biopsychosocial framework of each individual patient.
- OMT interventions for the cervical spine addressed through this framework include manipulation, mobilisation and exercise. Attention is focused on techniques in end-range positions of the cervical spine during mobilisation, manipulation and exercise interventions.
- The framework is based on the best available evidence at the time of writing. It is designed to be used with the IFOMPT Standards[4] that define international postgraduate best practices in OMT. Central to this framework are sound clinical reasoning and evidence-based practice.
- Within the cervical spine, events and presentations of vascular pathologies of the neck are rare but are an essential consideration as part of an OMT assessment. Arterial dissection (a tear in the lining of an artery) and other vascular presentations are somewhat recognisable if the appropriate questions are asked during the patient history if the interpretation of elicited data enables the recognition of this potential, and if the physical examination can be adapted to explore any potential vasculogenic hypothesis further. Therefore, the framework reflects best practices and aims to place risk in an appropriate context informed by the evidence. In this context, the framework considers ischaemic and non-ischaemic presentations to identify risk before overt symptoms in a patient presenting for cervical management.
- An important underlying principle of the framework is that physical therapists cannot rely on the results of only one test to conclude. Therefore, understanding the patient’s presentation following an informed, planned, and individualised assessment is essential. Multiple sources of information are available from the patient assessment process to improve confidence in estimating the probability of vascular pathologies of the neck. Data available to inform clinical reasoning will improve and change with ongoing research. This framework, therefore, encourages physical therapists to critically read the current literature to enable support for their clinical decisions rather than provide specific data prescriptive guidance, as the evidence base for this is not available.
- The framework is intended to be informative and not prescriptive and aims to enhance the physical therapist’s clinical reasoning as part of the patient assessment and treatment process. The framework is intended as simple and flexible. The physical therapist should be able to apply it to their patients, facilitating patient-centred practice.
IFOMPT Cervical Framework[edit | edit source]
The framework is divided into different sections and designed to be used with crucial literature sources identified in the context section.
[edit | edit source]
The current framework builds on the previous 2012 (first version) framework and addresses concerns raised by the consensus methodology and empirical work. To enable effective, efficient, and safe assessment and management of the cervical spine region, sound clinical reasoning is required.
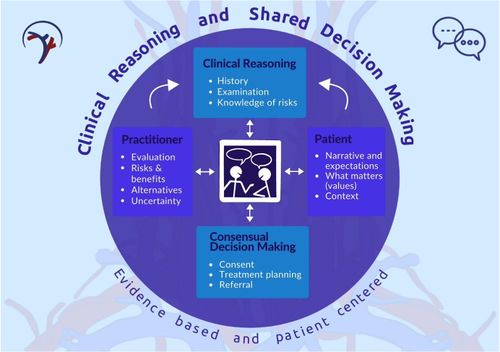
Shared decision-making is an effective means for reaching an agreement on the best treatment strategy. It fosters patient-centred “care that is respectful of and responsive to individual patient preferences, needs, and values” and ensures “that patient values guide all clinical decisions.”
The Informed Medical Decision-Making Foundation describes shared decision-making as a dynamic two-way process:
- The clinician communicates personalized information about the options, outcomes, probabilities, and scientific uncertainties of available treatment options to the patient.
- The patient communicates their values and the relative importance they place on benefits and harms.
The framework adopts the Agency for Healthcare Research and Quality’s 5-step SHARE approach:
- Seek your patient’s participation.
- Help your patient to explore and compare treatment options.
- 'Assess your patient’s values and preferences.
- Reach a decision with your Patient.
- Evaluate your patient’s decision to achieve patient-centred practice.
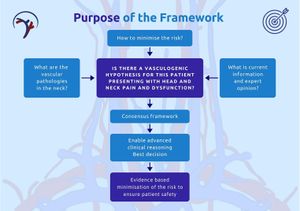
Section 2: Purpose of the Framework[edit | edit source]
- In advance of planned interventions such as mobilisation, manipulation, and exercise, the IFOMPT cervical framework guides assessment of the cervical spine region for potential vascular pathologies of the neck.
- Events and manifestations of vascular pathologies of the neck are uncommon within the cervical spine, but they must be considered as part of the patient examination.
- Vascular pathologies may be detectable if:
- the appropriate questions are asked during the patient history-taking process.
- the interpretation of elicited data allows recognition of this potential.
- the physical examination can be adapted to investigate any potential vasculogenic hypothesis.
- The framework is based on best practices and aims to place risk in a context informed by evidence. The framework considers ischaemic and non-ischaemic presentations in this context to identify risk in a patient presenting for cervical examination and management.
- One of the IFOMPT cervical framework's goals is to ensure that clinicians understand risk in both epidemiological and individual contexts, as clinicians cannot draw conclusions based on the results of a single test. Understanding the patient's presentation after an informed, planned, and individualised evaluation is critical.
Epidemiologically, the risk of a vascular incident related to therapeutic interventions is extremely low. Regardless, clinicians must do everything possible to mitigate and limit that risk.
Individually, patients differ in terms of risk, hazard, profile, or the presence of vascular pathology.
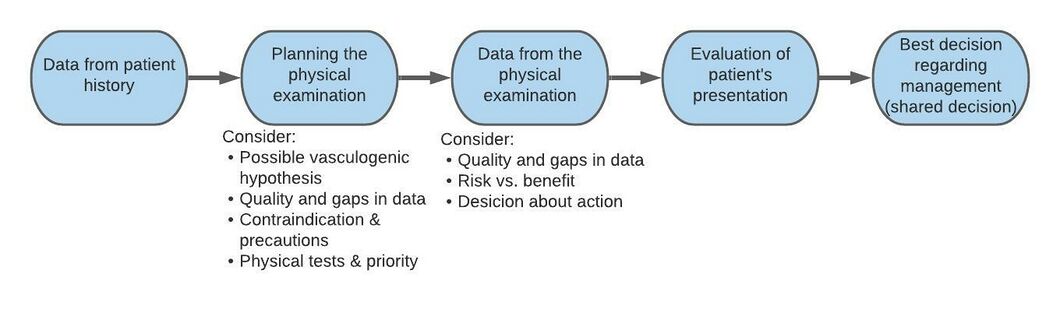
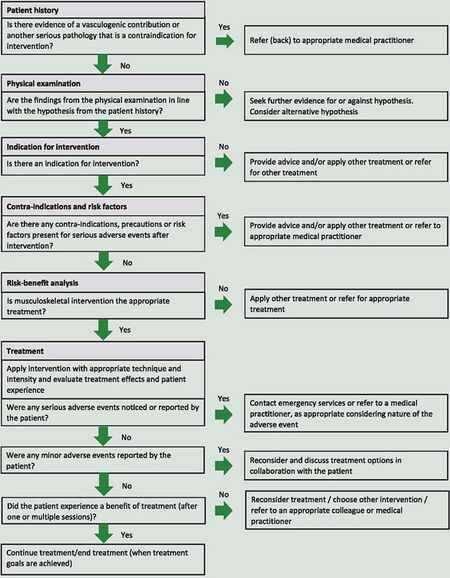
Section 3: Stages of the clinical reasoning process[edit | edit source]
- Stage 1: Taking a patient’s history.
- Stage 2: Planning the physical examination.
- Stage 3: Conducting the physical examination.
- Stage 4: Planning the intervention.
- Stage 5: Evaluating the intervention.
Case A :[edit | edit source]
History:
A 50-year-old male bricklayer complains of a headache. His headache is similar but different to previous migraine headaches that he intermittently experiences. This is different because he also feels lethargic and “run down.” With this in mind, he decides to go to bed sure that he will feel better in the morning as he does feel fatigued and “sleepy.” Upon waking, his headache is still present. He thinks he needs to exercise and “get out for some fresh air” (similar to previous headaches), so he walks to the shops for essentials. The checkout operator says that she cannot understand what he is saying and that his speech is slurred. He is confused as he knows what he is saying and feels this is due to his “overdoing it.” He reflects and cannot understand why he is still lethargic and cannot concentrate on things. Upon his wife's arrival home from work, she also comments that he is difficult to understand and needs to concentrate on their conversation as “he is not listening to her.” She calls a physical therapist friend to seek advice.
Synopsis:
A headache described as “unusual” with progressive signs of likely central ischemia (slurred speech, lethargy, fatigue, confusion) is sufficient information for the therapist to recommend emergency medical attention.
Section 4: Patient history[edit | edit source]
The patient history is used to develop and test hypotheses about the risk of vascular pathologies in the neck or the presence of frank vascular pathologies. Physical examination tests have very limited diagnostic utility data. As a result, the clinician's goal is to use the patient history to make the best judgement on the possibility of treatment contraindications or serious pathology. Subtle signs and symptoms of suspected pathologies should be identified during the patient history-taking. It is also critical to recognise risk factors that indicate the possibility of neurovascular pathology.
Considering Risk Factors[edit | edit source]
Vascular pathology of the neck event has a complex and multifactorial aetiology. Several factors have been linked to an increased risk of arterial pathologies involving the internal carotid or vertebrobasilar vessels. These should be thoroughly considered while taking a patient's history.
Check tables 2 and 3 on page 11 for detailed risk factors for dissection and non-dissection vascular events.
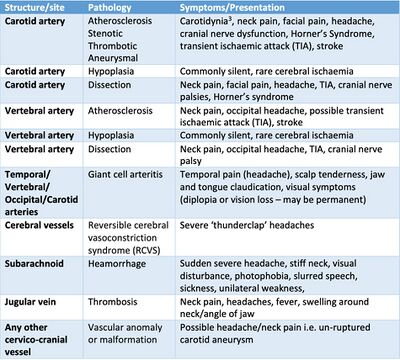
Presenting Features of Vascular Pathologies of the Neck[edit | edit source]
Recognising clinical pattern elements that may support or disprove a vascular hypothesis is critical. A definite clinical pattern cannot be identified due to the extremely low prevalence, a wide range of pathologies, and high variation of the presenting features of vascular pathologies of the neck. However, certain consistent features of clinical presentation emerge from historical case reports, which are supported by observations from systematic reviews. Check tables 4 through 8 on page 11 and 12 for clinical features for dissection and non-dissection events (combining vertebrobasilar artery [VBA], and internal carotid artery [ICA] pathologies).
Importance of Observation Throughout History[edit | edit source]
While the clinician is taking the patient's history, signs and symptoms of serious pathology and contraindications/precautions to treatment may manifest. This is a chance to observe and identify potential red flags indicators early in the clinical encounter such as:[5]
- Gait disturbances.
- Subtle signs of disequilibrium.
- Upper motor neuron signs.
- Cranial nerve dysfunction.
- Behavior suggestive of upper cervical instability (e.g., anxiety, supporting head/neck.)
Case B:[edit | edit source]
History:
A 46-year-old female supermarket worker presents for physical therapy with left-sided head (occipital) and neck pain described as “unusual.” She reports a 10-day history of the symptoms following a road traffic accident. The symptoms are progressively worsening. The pain is eased by rest. The patient reports an onset of new symptoms after about seven days, including “feels like might be sick,” “throaty,” and “feels faint”—especially after performing the gentle exercise. Two days after this, she reports a stronger feeling of nausea, loss of balance, swallowing difficulties, speech difficulties, and acute memory loss. She reports a history of previous road traffic accidents. Past medical history included hypertension, headaches, high cholesterol, and a maternal family history of heart disease and stroke.
Synopsis:
Progressive “unusual” headache with emerging hindbrain/central neurology with a history of trauma indicates additional testing to support a medical referral.
Section 5: Planning the physical examination[edit | edit source]
Necessity for planning[edit | edit source]
Interpreting the data from the patient history and defining the main hypotheses is essential to an effective physical examination[6][7]. Hypothesis generation from the history and refining, re-ranking and rejecting of these hypotheses in the physical examination is necessary to facilitate optimal clinical reasoning in OMT[8]. Therefore careful planning of the physical examination is required. In particular, for this framework, the possible vasculogenic (cervical arterial) contribution to the patient’s presentation needs to be evaluated from the patient history data.
Are any further patient history data required?[edit | edit source]
An important planning component is identifying any further patient history data that may be required. That is, are there any gaps in the information obtained? Is the quality of the information obtained sufficient?
Decision-making regarding the physical examination[edit | edit source]
Based upon the evaluation and interpretation of the data from the patient history, the physical therapist needs to decide the following:
- Are there any precautions for OMT?
- Are there any contraindications to OMT?
- What physical tests must be included or excluded in the physical examination?
- What is the priority for these physical tests for this specific patient? This informs decisions regarding the testing order and determines which tests should be completed at the first visit.
- Do the physical tests need to be adapted for this specific patient?
Case C:[edit | edit source]
History:
A 42-year-old accountant presents to physical therapy with a 5-day history of unilateral (left-sided) neck and jaw pain and temporal headache following decorating the ceiling (sustained head/neck extension). The following day, the patient’s pain worsened, and he developed left-sided ptosis. The patient had underlying risk factors for arterial disease, and the historical presentation was typical of ICA dissection, with a key differentiator being the ptosis.
Synopsis:
Neck pain and temporal headache related to sustained neck extension in a male with a cardiovascular profile. Physical examination findings support a vascular hypothesis and indicate urgent medical referral.
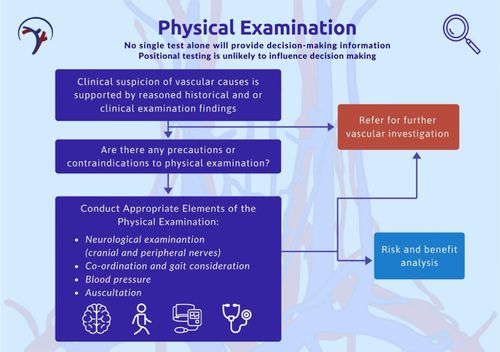
Section 6: Physical examination[edit | edit source]
Data obtained during the physical examination serves the following purposes:
- to support or refute the existing hypotheses
- to reevaluate the level of support for a vasculogenic hypothesis
- to determine whether a medical referral for further vascular workup is warranted
- to determine if the clinician can proceed with physical intervention
Current research data support the use of conventional vascular examination, including blood pressure, neurological examination, and carotid artery examination. However there is a lack of evidence to support functional positional tests to identify vertebral artery pathology (Vertebral Artery Test, VBI).
Blood pressure[edit | edit source]
- Examination of blood pressure informs clinical reasoning in 2 ways:
- Assess the risk for stroke, particularly from carotid origin.
- Assess for acute arterial trauma in situ. An increase in blood pressure may be related to acute arterial trauma, including ICA and vertebral artery (VA).
- Hypertension strongly predicts cardiovascular disease[9], but it should be interpreted in the context of other findings with sound clinical reasoning.
- There is a positive correlation between increased systolic and diastolic pressure and risk of stroke: the higher the pressure, the greater the risk.
Neurological examination[edit | edit source]
Neurological examination for musculoskeletal clinicians is a key element for safe clinical practice. It identifies upper and/or lower limb and upper motor neuron pathology. [10] Examination of the peripheral nerves and cranial nerves in assessing for an upper motor neuron lesion will assist in evaluating the potential for neurovascular conditions. Follow this link to learn more about testing. An increasing body of literature details clinical cases of arterial pathology with cranial nerve involvement to inform pattern recognition. The absence of findings does not rule out underlying pathology. Read the guide to cranial nerve testing for musculoskeletal clinicians here.
Examination of the carotid artery[edit | edit source]
The physiotherapist should aim to understand and experience both normal and pathological pulse quality. Auscultation is advised as palpation of the internal carotid artery may induce vagal reactions (especially when palpating bilaterally). In most cases, the sensitivity or specificity of pulse examination is unknown. Still, it may offer important evidence in the correct clinical context leading to specific diagnoses and treatments[11].
- An internal carotid artery pulse alteration has been identified as a feature of internal carotid disease. [12]
- Asymmetry between left and right vessels is considered significant.
- A pulsatile, expandable mass indicates an arterial aneurysm.[13]
- A bruit on auscultation (controlling for normal turbulence) indicates a significant finding and should be considered in the context of other clinical findings.
- It is possible for dissections and steno-occlusive disease of the carotid arteries to exist without aneurysm formation.
'Differentiation during the physical examination[edit | edit source]
Differentiating a patient’s symptoms from a vasculogenic cause with complete certainty is not currently possible from the physical examination. Thus, it is important for the physical therapist to understand that headache/neck pain may be the early presentation of an underlying vascular pathology. [14][15] The task for the therapist is to differentiate the symptoms by:
- Having a high index of suspicion
- Testing the vascular hypothesis.
This differentiation process should occur early in the assessment process, i.e. early in the patient history. The symptomology and history of a patient experiencing vascular pathology may alert the physical therapist to such an underlying problem[14][15]. A high index of suspicion of cervical vascular involvement is required in cases of acute onset neck/head pain described as “unlike any other”[15]. Physical therapists may be exposed to patients presenting with the early signs of stroke (for example, neck pain/headache) and need both knowledge and awareness of the mechanisms involved. A basic understanding of vascular anatomy, haemodynamics and the pathogenesis of arterial dysfunction may help the physical therapist differentiate vascular head and neck pain from a musculoskeletal cause[14][15] through interpretation of the patient history data and tests in the physical examination.
Refer to for further investigation[edit | edit source]
- There exist no clinical guidelines for medical diagnostic work-up regarding vascular pathology.
- The physiotherapist should follow local policy in referring for further investigation. Immediate referral for medical investigation should occur with clinical suspicion of vascular pathology.
- Conventionally, duplex ultrasound, magnetic resonance imaging/arteriography, and computed tomography are used in the workup.
Case D:[edit | edit source]
History:
A 45-year-old male is referred with a 6-month history of gradual onset unilateral neck pain and, more recently, headaches. The pain is manageable and not worsening, but the patient is worried that the pain has not resolved. Focused questioning for vascular pathology and dysfunction does not indicate a vascular hypothesis: no trauma, history of migraine, or significant cardiovascular factors. The pain is consistent with typical musculoskeletal dysfunction; no signs and symptoms are associated with vascular pathology or dysfunction.
Synopsis:
A history of headaches indicates focused questioning that fails to support a vascular hypothesis. Further findings are consistent with a musculoskeletal disorder.
Case E:[edit | edit source]
History:
A 72-year-old female is referred for episodic neck pain and headache. She has responded very well to manual therapy in the past. This episode is described as severe and irritable, like previous episodes. She has a cardiovascular history of hypertension, high cholesterol levels, and two previous strokes (the last one was three years ago).
Synopsis:
Patient history and physical examination findings support a vascular hypothesis, but an alternative, more likely explanation for the presenting complaint is also supported. There are insufficient data to support medical referral. Safety netting is indicated.
Section 7: Planning Intervention[edit | edit source]
This section relates to those patients NOT presenting with a discrete vascular pathology but with neuromusculoskeletal craniocervical dysfunction suitable for OMT mobilisation, manipulation and exercise intervention. This assessment of risk and benefit relates to the risk associated with treatment, not misdiagnosis.
Framework for evaluating risk[edit | edit source]
Compared to other noninvasive treatments, the risks of a serious adverse event from musculoskeletal intervention (manual and/or exercise interventions) are extremely low and vary depending on the patient's clinical presentation and known risk factors.
In the context of this Framework, there are two substantive but related risks:
- The risk of misdiagnosis of an existing vascular pathology
- The risk of serious adverse events following OMT
The current hypothesis for Misdiagnosis is either:
- Patients presenting with neck pain and headache who go on to develop a serious adverse event, such as a dissection.
- Patients have underlying pathology that is subsequently aggravated by the treatment.
- Patients present with a clinical condition that appears musculoskeletal related but is a different pathology.
Risk[edit | edit source]
- The absolute risk of physical treatments is much lower than that of comparable therapies (e.g., pharmacotherapy ) due to the very low baseline prevalence of vascular pathologies of the neck.
- Biomechanical studies in healthy individuals suggest that physical treatment alone, particularly when performed in a combination of midrange neck positions, cannot generate enough vessel stress or hemodynamic changes to explain the onset of a dissection event.
Benefit[edit | edit source]
- The benefits of OMT are reported in high-quality systematic reviews and meta-analyses by different authors[16][17][18][19]. OMT and exercise interventions are also included in the most recent Clinical Practice Guidelines linked to the International Classification of Functioning, Disability and Health[20]. The combination of OMT and exercise for neck pain and associated disorders like headache and radiculopathy have been proven effective[21][22].
Mobilization and Manipulation[edit | edit source]
- Mobilization and manipulation for neck pain have moderate to large clinically beneficial effects on pain and functional outcomes compared to inactive or active interventions. These advantages were independent of the length of the follow-up (short, intermediate, or long-term) and the duration of the neck pain (acute, subacute, or chronic).
- Mobilization and manipulation produce better results for tension-type headaches.
- Cervical manipulation had an immediate effect with moderate to large effects on cervical radiculopathy compared to no treatment, placebo, or traction interventions.
- This conclusion is supported by the updated Bone and Joint Decade Task Force on neck pain and associated disorders.
Adding Exercise to Mobilization and Manipulation[edit | edit source]
- For people with subacute and chronic nonspecific neck pain, there is moderate to strong evidence that various forms of mobilization and/or manipulation combined with exercise results in better outcomes than exercise alone:
- Pain relief
- Improvement in physical functioning
- Greater patient satisfaction
- Quality of life
- At short and medium-term follow-ups, approximately half of the included trials demonstrated moderate to large clinically beneficial effects when mobilization and/or manipulation were added to the treatment.
- Another review found moderate-quality evidence that adding mobilisation and/or manipulation to exercise therapy did not provide additional benefits for pain, disability, or quality of life in adults with low-grade neck pain.
- As a result, the evidence is conflicting.
Person-centred decision-making[edit | edit source]
- Individually, the epidemiological data must be contextualised to the specific patient encounter, as illustrated by the cases, based on the background literature, highlighting various risk factors for specific pathologies in specific people. There is a lack of accurate data to inform precise levels of risk at an individual level, making it impossible to develop valid clinical prediction rules for risk or benefit.
- The clinician cannot make an absolute risk judgement.
- The clinician must accept that clinical decisions are made without certainty and that the goal of the analysis is to make a decision based on a balance of probabilities.
- When in doubt about intervention, the clinician should consider not intervening and assess the chance of natural recovery of pain and function (assuming a musculoskeletal dysfunction).
- Shared decision-making is an effective method for agreeing on the best treatment strategy. The SHARE framework walks you through the process of having these conversations step by step.
Case F:[edit | edit source]
History:
A 33-year-old male presents with right-sided suboccipital neck pain/headache. Worse is in the mornings and aggravated by the left rotation of the neck. Symptoms began two weeks ago (he recalls “cricking” his neck in a football tackle)—they are gradually worsening. No previous similar episode of this type of pain, but some lower neck pains several years ago. Good health; history of migraine. The patient had manual therapy five days ago (soft tissue massage to his bilateral neck and shoulder; dry needling/acupuncture to his right trapezius; mobilization of the upper cervical spine [C0-C2]). Immediate increased pain in the left cervical spine and an episode of feeling very unsteady/dizzy. The therapist attempted to continue with soft-tissue massage when the dizziness settled, but the patient became unwell and vomited.
Synopsis:
A young patient with a history of migraine and recent trauma present with “unusual” headaches. The onset of vascular signs and symptoms during care should alert the therapist to test a vascular hypothesis in line with best practice guidance and refer appropriately.
Section 8: Evaluating An Intervention[edit | edit source]
- Clinical reasoning should enable effective, efficient, and safe management of the cervical spine.
- Using the principles described in the IFOMPT cervical framework to aid patient-centred clinical reasoning through intervention, evaluation, and progression is important.
Section 9: Summary[edit | edit source]
References[edit | edit source]
- ↑ 1.0 1.1 Rushton A, Carlesso LC, Flynn T, Hing WA, Rubinstein SM, Vogel S, Kerry R. International Framework for Examination of the Cervical Region for Potential of Vascular Pathologies of the Neck Prior to Musculoskeletal Intervention: International IFOMPT Cervical Framework. J Orthop Sports Phys Ther. 2023 Jan;53(1):7-22.
- ↑ Rushton A, Carlesso LC, Flynn T, Hing WA, Kerry R, Rubinstein SM, Vogel S. International Framework for Examination of the Cervical Region for potential of vascular pathologies of the neck prior to Orthopaedic Manual Therapy (OMT) Intervention: International IFOMPT Cervical Framework, 2020. Available from https://www.ifompt.org/site/ifompt/IFOMPT [last access 21.03.2023]
- ↑ Hutting N, Wilbrink W, Taylor A, Kerry R. Identifying vascular pathologies or flow limitations: Important aspects in the clinical reasoning process. Musculoskelet Sci Pract. 2021 Jun;53:102343.
- ↑ 4.0 4.1 INTERNATIONAL FEDERATION OF ORTHOPAEDIC MANIPULATIVE PHYSICAL THERAPISTS (IFOMPT) INC. Educational Standards In Orthopaedic Manipulative Therapy. PART A: EDUCATIONAL STANDARDS 2016 Available at: https://www.ifompt.org/site/ifompt/IFOMPT [last access 20.03.2023]
- ↑ Russek LN, Block NP, Byrne E, Chalela S, Chan C, Comerford M, Frost N, Hennessey S, McCarthy A, Nicholson LL, Parry J, Simmonds J, Stott PJ, Thomas L, Treleaven J, Wagner W, Hakim A. Presentation and physical therapy management of upper cervical instability in patients with symptomatic generalized joint hypermobility: International expert consensus recommendations. Front Med (Lausanne). 2023 Jan 18;9:1072764.
- ↑ Maitland G, Hengeveld E, Banks K, English K, editors. Maitland's Vertebral Manipulation, 7th Edition, Elsevier Butterworth Heinemann, Edinburgh, 2005.
- ↑ Petty NJ. Neuromusculoskeletal Examination and Assessment: A Handbook for Therapists (Physiotherapy Essentials), 4th edition, Churchill Livingstone, Elsevier, Edinburgh, 2011.
- ↑ Jones MA, Rivett DA. Introduction to clinical reasoning. In Jones MA and Rivett DA editors. Clinical Reasoning for Manual Therapists. Butterworth-Heinemann: Edinburgh, 2004. p3-24.
- ↑ Saiz LC, Gorricho J, Garjón J, Celaya MC, Erviti J, Leache L. Blood pressure targets for the treatment of people with hypertension and cardiovascular disease. Cochrane Database Syst Rev. 2020 Sep 9;9(9):CD010315.
- ↑ Taylor A, Mourad F, Kerry R, Hutting N. A guide to cranial nerve testing for musculoskeletal clinicians. J Man Manip Ther. 2021 Dec;29(6):376-389.
- ↑ Pickett CA, Jackson JL, Hemann BA, Atwood JE. Carotid artery examination is an important tool in patient evaluation. South Med J. 2011 Jul;104(7):526-32.
- ↑ Patel RR, Adam R, Maldjian C, Lincoln CM, Yuen A, Arneja A. Cervical carotid artery dissection: current review of diagnosis and treatment. Cardiol Rev. 2012 May-Jun;20(3):145-52.
- ↑ Elder A, Japp A, Verghese A. How valuable is a physical examination of the cardiovascular system? BMJ. 2016 Jul 27;354:i3309.
- ↑ 14.0 14.1 14.2 Rivett DA. Adverse effects of cervical manipulative therapy. In Boyling JD and Jull GA editors, Grieve’s Modern Manual Therapy of the Vertebral Column (3rd ed). Churchill Livingstone: Edinburgh, 2004, p533-549.
- ↑ 15.0 15.1 15.2 15.3 Taylor AJ, Kerry R. A ‘system based’ approach to risk assessment of the cervical spine before manual therapy. International Journal of Osteopathic Medicine 2010; 13(3): 85-93.
- ↑ Gross A, Langevin P, Burnie SJ, Bédard-Brochu MS, Empey B, Dugas E, Faber-Dobrescu M, Andres C, Graham N, Goldsmith CH, Brønfort G, Hoving JL, LeBlanc F. Manipulation and mobilisation for neck pain contrasted against an inactive control or another active treatment. Cochrane Database Syst Rev. 2015 Sep 23;(9):CD004249.
- ↑ Lozano López C, Mesa Jiménez J, de la Hoz Aizpurúa JL, Pareja Grande J, Fernández de Las Peñas C. Efficacy of manual therapy in the treatment of tension-type headache. A systematic review from 2000-2013. Neurologia. 2016 Jul-Aug;31(6):357-69. English, Spanish
- ↑ Zhu L, Wei X, Wang S. Does cervical spine manipulation reduce pain in people with degenerative cervical radiculopathy? A systematic review of the evidence and a meta-analysis. Clin Rehabil. 2016 Feb;30(2):145-55.
- ↑ Varatharajan S, Ferguson B, Chrobak K, Shergill Y, Côté P, Wong JJ, Yu H, Shearer HM, Southerst D, Sutton D, Randhawa K, Jacobs C, Abdulla S, Woitzik E, Marchand AA, van der Velde G, Carroll LJ, Nordin M, Ammendolia C, Mior S, Ameis A, Stupar M, Taylor-Vaisey A. Are non-invasive interventions effective for the management of headaches associated with neck pain? An update of the Bone and Joint Decade Task Force on Neck Pain and Its Associated Disorders by the Ontario Protocol for Traffic Injury Management (OPTIMa) Collaboration. Eur Spine J. 2016 Jul;25(7):1971-99.
- ↑ Blanpied PR, Gross AR, Elliott JM, Devaney LL, Clewley D, Walton DM, Sparks C, Robertson EK. Neck Pain: Revision 2017. J Orthop Sports Phys Ther. 2017 Jul;47(7):A1-A83.
- ↑ Hidalgo B, Hall T, Bossert J, Dugeny A, Cagnie B, Pitance L. The efficacy of manual therapy and exercise for treating non-specific neck pain: A systematic review. J Back Musculoskelet Rehabil. 2017 Nov 6;30(6):1149-1169.
- ↑ Fredin K, Lorås H. Manual therapy, exercise therapy or combined treatment in managing adult neck pain - A systematic review and meta-analysis. Musculoskelet Sci Pract. 2017 Oct;31:62-71.