Humerus
Description[edit | edit source]
The humerus is a long bone which consists of a shaft (diaphysis) and two extremities (epiphysis). It is the longest bone of the upper extremity.
Introduction[edit | edit source]
Welcome to the fascinating world of humerus anatomy—a cornerstone in the realm of physiotherapy. Understanding the intricacies of the humerus, the long bone that forms the upper arm, is paramount for physiotherapists seeking to optimize patient care and rehabilitation.
The humerus, with its unique structure comprising a head, anatomical neck, surgical neck, tuberosities, and body, plays a pivotal role in the intricate dance of the upper limb's movements. As a physiotherapist with a keen focus on patient well-being, delving into the nuances of humerus anatomy opens up a myriad of possibilities for effective intervention and support.
Practical Applications[edit | edit source]
In the dynamic field of physiotherapy, an in-depth understanding of humerus anatomy is instrumental in tailoring interventions for optimal patient outcomes[1] . Physiotherapists dealing with humerus-related conditions can apply this knowledge in various practical ways:
1. Tailor Rehabilitation Programs: - A nuanced understanding of the humerus allows physiotherapists to tailor rehabilitation programs to the specific needs of patients recovering from humerus-related injuries, such as fractures or dislocations[2] .
2. Enhance Range of Motion:- Knowledge of the humerus' articulations and muscle attachments empowers physiotherapists to design exercises that effectively enhance range of motion in the upper limb, crucial for rehabilitation post-humerus surgery or trauma[3] .
3. Address Functional Impairments:- Physiotherapists can leverage their understanding of humerus anatomy to address functional impairments resulting from humerus-related conditions. This includes developing targeted interventions to improve activities of daily living affected by these impairments[4] .
4. Prevent Secondary Complications:- Proactive physiotherapy, grounded in sound anatomical knowledge of the humerus, aids in the prevention of secondary complications. Physiotherapists can implement strategies to mitigate issues such as muscle imbalances or joint stiffness, enhancing overall patient well-being[5] .
5. Facilitate Informed Patient Education:- Physiotherapists, armed with a profound understanding of humerus anatomy, can play a crucial role in patient education. By explaining the relevance of humerus anatomy in a patient-friendly manner, they foster collaboration and empower patients in their recovery journey[6] .
These practical applications underscore the pivotal role of humerus anatomy in guiding effective physiotherapeutic interventions, promoting holistic patient care.
Structure[edit | edit source]
Upper Extremity Features[edit | edit source]
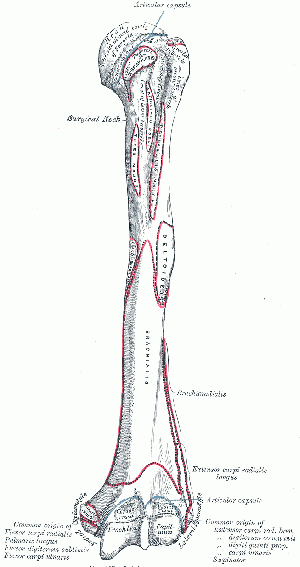
The head of the humerus is the proximal articular surface of the upper extremity, which is an irregular hemisphere. It articulates with the glenoid fossa of the scapula.
The anatomical neck is the part between the head and the tuberosities.
The surgical neck is the part between the tuberosities and the shaft.
The greater tuberosity it is located lateral to the head at the proximal end.
The lesser tuberosity is located inferior to the head, on the anterior part of the humerus, Its very prominent and palpable.
Bicipital (intertubercular) groove is located between the two tuberosities. The long head of the biceps tendon is placed here.
Body Features[edit | edit source]
The body of the humerus has three borders and three surfaces.
Borders[edit | edit source]
- Anterior
- Lateral
- Medial
Surfaces[edit | edit source]
- Antero-lateral
- Antero-medial
- Posterior
Function[edit | edit source]
The humerus serves as an attachment to 13 muscles which contribute to the movements of the hand and elbow, and therefore the function of the upper limb.
The humerus, as the longest bone in the upper extremity, serves several crucial functions within the musculoskeletal system. These functions are integral to the overall movement and stability of the upper limb [8]
1. Articulation at the Glenohumeral Joint:- The head of the humerus forms the proximal articular surface, articulating with the glenoid fossa of the scapula, facilitating the wide range of movements at the glenohumeral joint .[9]
2. Muscle Attachments and Movement Coordination:- The humerus serves as an attachment point for various muscles, including the supraspinatus, infraspinatus, and teres minor, contributing to the coordinated actions of the upper limb [10]
3. Transmission of Forces:- Acting as a bridge between the shoulder and the forearm, the humerus plays a crucial role in transmitting forces generated by the muscles, allowing for effective and controlled movements[11]
4. Support for Soft Tissues:- The anatomical neck, surgical neck, and tuberosities of the humerus provide support for various soft tissues, including tendons and ligaments, contributing to the stability of the shoulder joint [12]
5. Facilitation of Muscle Functionality:- Muscle attachments along the humerus, such as the greater and lesser tuberosities, play a key role in facilitating the functionality of muscles like the supraspinatus, infraspinatus, and teres minor .[13]
6. Facilitation of Forearm Movements:- The humerus, through its articulation with the radius and ulna at the elbow joint, enables flexion and extension movements of the forearm, contributing to the overall dexterity of the upper limb .[14]
Video[15][edit | edit source]
Articulations[edit | edit source]
Muscle Attachments[edit | edit source]
| Muscle | Attachment |
|---|---|
| Supraspinatus | Greater Tubercle |
| Infraspinatus | Greater Tubercle |
| Teres Minor | Greater Tubercle
Upper Part of the Lateral Border |
| Subscapularis | Lesser Tubercle |
| Pectoralis Major | Upper Part of the Anterior Border |
| Triceps Brachii | Lower Part of the Lateral Border
Lateral Supracondylar Ridge |
| Brachioradialis | Lateral Supracondylar Ridge |
| Extensor Carpi Radialis Longus | Lateral Supracondylar Ridge |
| Teres Major | Crest of the Lesser Tubercle |
| Coracobrachialis | Crest of the Lesser Tubercle |
| Brachialis | Medial Supracondylar Ridge |
| Pronator Teres | Medial Supracondylar Ridge |
| Latissimus Dorsi | Bicipital Groove |
Clinical Relevance[edit | edit source]
Proximal end or Head-Surgical Neck Fracture[16]
- It is caused by a direct blow on the area or fall on an outstretched hand.
- It can result in damage to the Axillary nerve and Posterior circumflex artery.
- Axillary nerve damage results in paralysis of deltoid and teres minor muscles.
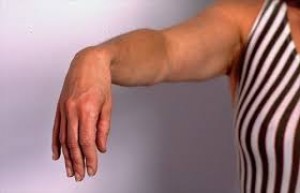
Shaft-Mid-shaft fracture[16]
- This fracture causes damage to radial nerve and Profunda brachii artery.
- Sensory loss can be seen over the dorsal surface of the hand, proximal parts of lateral 3 and a half fingers dorsally.
- Radial nerve palsy results in wrist drop.
Distal end-Supracondylar fracture[16]
- It is a fracture of the distal humerus just above the elbow joint.
- It results in damage to the brachial artery and anterior interosseous nerve, the resulting ischemia causes Volkmann's ischaemic contracture.
Other conditions
- Humerus Varus can be caused due to haematologic, infectious, genetic and neurological disorders.[17]
- Charcot arthropathy is a rare disorder characterised by debilitating joint destruction.[17]
References[edit | edit source]
- ↑ Moore KL, Dalley AF, Agur AM.Clinically Oriented Anatomy.7th ed. (Edition) Philadelphia, PA: Lippincott Williams & Wilkins; 2014.
- ↑ Magee DJ.Orthopedic Physical Assessment.6th ed. St. Louis, MO: Saunders; 2014.
- ↑ Neumann DA.Kinesiology of the Musculoskeletal System: Foundations for Rehabilitation. 3rd ed.St. Louis, MO: Mosby; 2016.
- ↑ Kendall FP, McCreary EK, Provance PG, Rodgers MM, Romani WA.Muscles: Testing and Function, with Posture and Pain.5th ed. Baltimore, MD: Lippincott Williams & Wilkins; 2005.
- ↑ Levangie PK, Norkin CC.Joint Structure and Function: A Comprehensive Analysis. 5th ed. Philadelphia, PA: F.A. Davis Company; 2016.
- ↑ Kisner C, Colby LA. *Therapeutic Exercise: Foundations and Techniques*. 6th ed. Philadelphia, PA: F.A. Davis Company; 2012.
- ↑ Gray H. Anatomy of the human body [Internet]. 20th ed. Lewis WH, editor. Philadelphia: Lea & Febiger; 1918. Accessed 26 March 2020.
- ↑ Moore KL, Dalley AF, Agur AMR. *Clinically Oriented Anatomy.* 7th ed. Lippincott Williams & Wilkins; 2014.
- ↑ Standring S, Borley NR, Collins P, et al. *Gray's Anatomy: The Anatomical Basis of Clinical Practice.* 40th ed. Churchill Livingstone; 2008
- ↑ Drake RL, Vogl AW, Mitchell AWM. *Gray's Anatomy for Students.* 2nd ed. Churchill Livingstone; 2009.
- ↑ Palastanga N, Field D, Soames R. *Anatomy and Human Movement: Structure and Function.* 6th ed. Butterworth-Heinemann; 2002.
- ↑ Netter FH. *Atlas of Human Anatomy.* 7th ed. Saunders; 2018.
- ↑ Tortora GJ, Nielsen M. *Principles of Human Anatomy.* 15th ed. Wiley; 2017.
- ↑ Saladin KS. *Anatomy & Physiology: The Unity of Form and Function.* 8th ed. McGraw-Hill; 2018.
- ↑ Kenhub - Learn Human Anatomy. Humerus Bone - Anatomy, Definition & Function - Human Anatomy Kenhub. Available from: https://www.youtube.com/watch?v=GBg3aQ7B1QE [last accessed 25/06/2022]
- ↑ 16.0 16.1 16.2 Jones O. The Humerus (Updated 16 June 2019). Teach Me Anatomy. Accessed 24 March 2020
- ↑ 17.0 17.1 Mostafa E, Varacallo M. Anatomy, Shoulder and Upper Limb, Humerus. InStatPearls [Internet] 2018 Dec 3. Accessed 26 March 2020