Gate Control Theory of Pain
Original Editor - Kapil Narale
Top Contributors - Kapil Narale
Introduction[edit | edit source]
The Gate Control Theory of Pain is a mechanism, in the spinal cord, in which pain signals can be sent up to the brain to be processed to accentuate the possible perceived pain, or attenuate it at the spinal cord itself. [1]
The 'gate' is the mechanism where pain signals can be let through or restricted. One of two things can happen, the gate can be 'open' or the gate can be 'closed': [1]
- If the gate is open, pain signals can pass through and will be sent to the brain to perceive the pain. [1]
- If the gate is closed, pain signals will be restricted from travelling up to the brain, and the sensation of pain won't be perceived. [1]
If someone experiences a painful (noxious) stimulus, the application of a non-noxious (soothing or light rubbing) stimulus can help activate the gate control mechanism, and reduce the pain. [2]
There are also other factors which can help facilitate the pain gate mechanism in reducing the perceived pain. These will be further outlined below.
Physiology[edit | edit source]
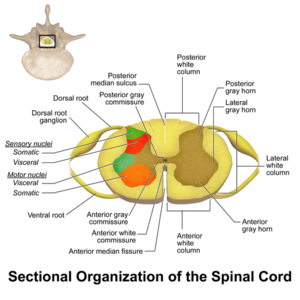
The pain gate mechanism is located in the dorsal horn of the spinal cord, specifically in the Substantia gelatinosa. The interneurons within the Substantia gelatinosa are what synapse to the primary afferent neurons, and are where the gate mechanism occurs. [1] Thus, the substantia gelatinosa modulates the sensory information that is coming in from the primary afferent neurons. [3]
Primary neurons come in three different types:
- A-β fibers, large diameter fibers, have a quick transmission of impulses, due to their myelination [1] - these type of fibers are activated by non-noxious stimuli, such as light touch, pressure, and hair movement. [4]
- A-δ fibers, a smaller diameter fiber [1] - they are thinly myelinated, and are stimulated by noxious stimuli, such as pain and temperature, specifically sharp, intense, tingling sensations. [4]
- C fibers, similar to A-δ fibers, have the slowest transmission of impulse since they are not myelinated [1] - these type of fibers are activated by pain and temperature, namely prolonged burning sensations. [4]
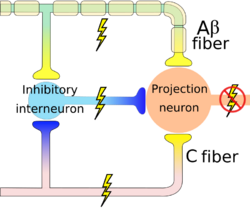
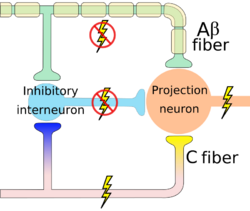
If the interneurons in the substantia gelatinosa are stimulated by the non-noxious large diameter A-β fibers, an inhibitory response is produced and there are no pain signals sent to the brain, and in this instance the 'pain gate' is closed. [1][3]
When the interneurons are stimulated by the smaller diameter A-δ or C fibers, an excitatory response is produced. In this case, pain signals are sent to the brain, these can be modulated, sent back down through descending modulation, and perceived as varying amounts of pain. [1][3]
The activation of the large diameter A-β fibers also can help reduce and inhibit the transmission of the small diameter A-δ and C fibers. [2]
At the Spinal Cord[edit | edit source]
The primary afferent neurons come from the periphery and synapse with the second order neurons in the dorsal horn in the spinal cord, and release respective neurotransmitters or neuropeptides.
Possible neurotransmitters or neuropeptides that can be released are:
- Glutamate, which is excitatory - the activation of NMDA receptors by glutamate increases receptive field size, decreases activation threshold, and extends depolarization, which leads to activation of the dorsal horn neurons. [4]
- Glycine and gamma-amino-butyric-acid (GABA), which are inhibitory - glycine can bind onto NMDA, while GABA has its own specific receptors. [4]
- Substance P is an excitatory neuropeptide - these are found in C-fibers in the periphery, and respond to tissue damage by causing vasodilation, inflammation, and/or pain. [4]
- Endorphins and serotonin are released in the descending pathway to also help with gate control and the modulation of pain. [2]
There are two types of second order neurons: wide dynamic range (WDR) neurons, and nociceptive specific (NS) range neurons. The WDR neurons synapse to A-β, A-δ, and C fibers, and therefore are activated by noxious and non-noxious stimuli. The NS neurons, on the other hand, only synapse to A-δ and C fibers, thus are activated by noxious stimuli. [4]
Third-order neurons, which are located in the brainstem and diencephalon, transmit the pain signal to the cerebral cortex, where the pain signal, from the A-δ and C fibers, can be further modulated. [4]
Here is a video explaining the gate control theory, in a brief and simple manner.
Useful Applications[edit | edit source]
The painful sensation that is perceived and experienced isn't only driven by the sensory event, but also the pain signals sent from the brain (through the descending modulation) due to thoughts, attitudes, emotions, and feelings that surround the painful experience.
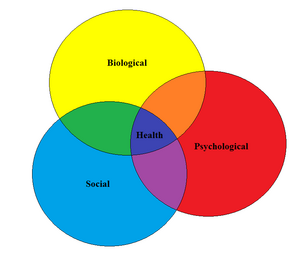
This relates to the biopsychosocial model, and can help increase or decrease the pain perceived. If someone has worrisome or anxious thoughts, negative emotions or memories, poor past experiences, or receives negative social feedback, pain signals will be sent down from the brain passing through an 'open gate', and the pain perceived will be greater. However, positive thoughts, emotions, and memories about the painful experience, relaxation, or positive social feedback, will cause the gate to close, and the person will essentially experience less pain. [1]
Transcutaneous Electrical Nerve Stimulation (TENS)[edit | edit source]
The usage of TENS activates the pain gate mechanism to inhibit pain signals going up to the brain, and thus reduces the sensation of pain. Similar to as described above, the TENS activates non-noxious afferent fibers, which in turn activates the 'pain-inhibiting' interneurons in the spinal cord, and thus minimizes/reduces perceived pain as an output. This is because TENS can activate A-β fibers, which helps facilitate the gate control mechanism. [2] The activation of the A-β fibers will inhibit the input from the noxious A-δ and C fibers. [4]
The Interferential Current (IFC) modality, also commonly used in Physiotherapy practices, inhibits pain through the gate control mechanism, and other neural mechanisms. [2]
Exercise Induced Pain[edit | edit source]
It was found that both TENS and IFC can greatly reduce exercise induced pain during single limb exercise, while only TENS had a positive effect on endurance of the whole body. A such intervention to reduce pain helps to increase exercise endurance performance. [2]
Low Back Pain[edit | edit source]
In regards to low back pain, it was found that the use of TENS, as an intervention on its own, was very effective in reducing pain. Using TENS in addition to other Physiotherapy modalities, such as manual mobilization, massage, stretching, or exercise, further helped to improve painful symptoms and quality of life. [6]
Rubbing and Massage[edit | edit source]
When you have an injury, especially a small injury, such as hitting your thumb with a hammer, burning your hand on your coffee cup, or getting your hand stuck in a door, and experience nociceptive type of pain, the common response is to chase away the pain by rubbing it. This helps sooth and reduce the pain due to the reasons explained above. The non-noxious A-β fibers are activated and inhibit the A-δ and/or C fibers causing the pain.[4] [2]
Massage therapy also makes use of the gate control theory to reduce and inhibit pain, with the same reasoning of activating large diameter A-β nerve fibers. This can be beneficial to many types of patients, and help with improving high blood pressure, sleep, relaxation, depression, stiffness, emotional well-being, recovery time, and many other conditions. Cardiac patients may benefit from massage to various painful body parts, which would help them minimize or eliminate the use of pharmaceuticals, and from experiencing possible side effects. [7]
Other modalities which utilize the pain control theory:
- Acupuncture and acupressure (also modulate the descending pathway) [4]
- Vibration (similar to TENS) [4]
Here is a more in-depth video that dives deep into explaining ascending tracts, pain modulation, and the gate control theory.
Related Resources[edit | edit source]
This page briefly outlines the gate control theory, and talks about aspects of pain modulation, both at the spinal cord level, and at the brain stem and higher brain centers.
This described various Theories of Pain, including the Pain Gate Theory and the Biopsychosocial Model
Discusses ascending and Descending Pathways, and Neurotransmitters
- Dorsal Column Medial Lemniscal Pathway - Physiopedia
This nicely explains DCML pathways, and the different types of neurons that are found within the pathway (1st, 2nd, 3rd order neurons)
This is a good overview of the concept of pain, and discusses some case studies
This outlines the different types of pain that can experienced from Nociceptive, neuropathic, referred, and others.
References[edit | edit source]
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 Campbell TS, Johnson JA, Zernicke KA. Gate Control Theory of Pain. In: Encyclopedia of Behavioral Medicine. Cham: Springer International Publishing; 2020. p. 914–916.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 Astokorki Ahy, Mauger AR. Transcutaneous electrical nerve stimulation reduces exercise-induced perceived pain and improves endurance exercise performance. European journal of applied physiology. 2017;117(3):483–492.
- ↑ 3.0 3.1 3.2 Moayedi M, Davis KD. Theories of pain: from specificity to gate control. Journal of neurophysiology. 2013;109(1):5–12.
- ↑ 4.00 4.01 4.02 4.03 4.04 4.05 4.06 4.07 4.08 4.09 4.10 4.11 Khelemsky Y, Malhotra A, Gritsenko K. Academic Pain Medicine A Practical Guide to Rotations, Fellowship, and Beyond. 1st ed. 2019. Cham: Springer International Publishing; 2019.
- ↑ Alila Medical Media. Gate Control Theory of Pain, Animation. Available from: https://www.youtube.com/watch?v=M-rL8XdHo6Q&ab_channel=AlilaMedicalMedia (accessed 22 April 2022)
- ↑ Safdar F, Sangrasi SA, Waseem MH, Shaikh AG. Low Back Pain: Effectiveness of TENS With or Without Standard Physiotherapy Treatment. The professional medical journal. 2017;24(6):818–23.
- ↑ Adams R, White B, Beckett C. The effects of massage therapy on pain management in the acute care setting. International journal of therapeutic massage & bodywork. 2010;3(1):4–11.
- ↑ Ninja Nerd. Ascending Tracts| Pain Modulation: Gate Control Theory. Available from: https://www.youtube.com/watch?v=8IhN6T3mT04 (accessed 22 April 2022)