Central Slip Extensor Tendon Injuries
Original Editor - Wanda van Niekerk
Top Contributors - Wanda van Niekerk, Kim Jackson, Tarina van der Stockt, Jess Bell and Olajumoke Ogunleye
Introduction[edit | edit source]
Extensor injuries of the hand are common in young, otherwise healthy males.[1] Various injury mechanisms include hyperflexion, direct blunt trauma and penetrating trauma. When left untreated, disruption of the extensor mechanism over zone III and detachment of the central slip leads to a Boutonniere deformity. This deformity is characterised by flexion of the proximal interphalangeal joint (PIP) and hyperextension of the distal interphalangeal joint (DIP) due to the volar subluxation of the lateral bands.[2] It is an extensor tendon injury over zone III. It is also referred to as a "buttonhole deformity."[3]
Clinically relevant anatomy[edit | edit source]
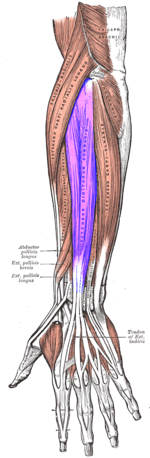
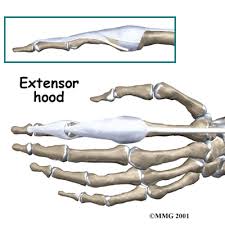
The Extensor Digitorum Communis (EDC) tendon at each finger splits into three bands or slips. These slips are: the central tendon/slip, which inserts on the base of the middle phalanx; and two lateral bands/slips, which rejoin as the terminal tendon/slip to insert into the base of the distal phalanx. In order to produce active interphalangeal extension, the EDC muscle requires the assistance of two intrinsic muscle groups, the interossei and the lumbricals. These muscles also have attachments to the extensor hood and the lateral bands/slips. The EDC tendon and all its complicated active and passive interconnections at, and distal to the metacarpophalangeal joint are known together as the extensor mechanism. The foundation of the extensor mechanism is formed by the tendons of the EDC muscle (with extensor indicis and extensor digiti minimi) and the extensor hood, the central tendon/slip, and the lateral bands/slips that merge into the terminal tendon/slip. The triangular ligament helps stabilize the bands on the dorsum of the finger. The triangular ligament provides stability to the lateral bands preventing palmar subluxation during flexion of the proximal interphalangeal joint.[5][6][7]
Aetiology[edit | edit source]
Central slip injuries in zone III are often the result of the following[2]:
- hyperflexion
- direct blunt trauma
- penetrating trauma
Closed central slip injuries are often caused by hyperflexion and direct blunt trauma, as is commonly seen in athletes.[9]
A Boutonniere Deformity (BD) may develop secondary to trauma to the extensor mechanism over zone III or zone IV (including a direct laceration to the extensor mechanism), secondary to rheumatoid arthritis (RA), and in the setting of burns. Reports of congenital Boutonniere deformities are also documented.[10] The pathogenesis of a BD varies according to its aetiology.[11]
Mechanism[edit | edit source]
If the central slip of the digital expansion is ruptured, there will be minimal deformity as long as the transverse fibers of the expansion remain intact. If they are also torn, a deformity is produced at the PIP joint. In this case, all extensor force will be transmitted to the distal phalanx by intact lateral bands, producing hyperextension of the DIP joint. The PIP joint buckles into flexion and protrudes through the breach in the extensor hood. The two lateral bands will now run on the palmar aspect of the PIP joint and will exaggerate flexion.[12][13]
Signs and Symptoms[edit | edit source]
Signs of the classic boutonnière deformity or central slip disruption can develop immediately after an injury to the finger. Alternatively, they may occur 10 to 14 days after the initial injury[15] as it may take a while for the proximal interphalangeal extensor hood and triangular ligament to disrupt completely.[16] Typical signs are:
- Loss of extension at PIP joint and hyperextension at the DIP joint[15]
- The finger at the middle joint (PIP) cannot be straightened and the fingertip (DIP joint) cannot be bent
- A weak grip and an inability to grasp and manipulate small objects with the tip of the digit
- Swelling and pain occur and continue on the top of the middle joint of the finger (proximal interphalangeal joint)[17]
Special Tests[edit | edit source]
Special tests that help in identifying injury to the extensor mechanism include:
- Elson Test - Fixing PIP Joint at 90° and ask the patient to extend the DIP joint. A lax DIP joint, despite the patient's effort to extend, is a negative or normal finding (if the central slip is intact, the loose lateral bands/slips when the PIP is flexed prevent DIP extension). A positive finding is a rigid DIP joint because of increased unopposed pull through the lateral bands/slips.[15]
- Modified Elson Test - The injured digit and its normal counterpart are placed in full proximal interphalangeal flexion, with the dorsum of each middle phalanx firmly against each other. If the injured digit has visibly better distal interphalangeal extension than the uninjured digit, a central slip injury is likely.[16]
- Boyes Test - Extend PIP and ask to flex DIP; positive is unable to flex DIP actively[18]
Boyes test may become positive only in the late stages.
Management and Rehabilitation of Central Slip Injuries[edit | edit source]
Acute Closed Central Slip Injury - Conservative management[edit | edit source]
Conservative management of an acute closed central slip injury is appropriate when the injury is less than 4 weeks old.[21] The injury is managed by splinting the injured finger with the PIP in extension with the DIP, MCP and wrist joint free for 3 to 6 weeks. This is then followed by 6 weeks of night time splinting.[15] If the lateral bands/slips are not involved, DIP joint flexion exercises may be prescribed. Flexion exercises of the DIP joint with the PIP joint in extension promote the retraction of the lateral bands dorsally from a volarly subluxed position. This allows tightening of the triangular ligament and, therefore, prevents the lateral bands from volar migration. It also prevents the development of a Boutonniere deformity.[15]
The PIP joint needs to be monitored closely for an extensor lag. This sometimes occurs after 6 weeks when the splint is removed.[21] The following exercises can be prescribed if there is no extensor lag present[21]:
- Patient can start weaning out of the splint
- Commence with active range of motion exercises of the the PIP joint
- Light functional use from 6 to 8 weeks
- Theraputty strengthening exercises from 8 weeks if the patient is progressing well with range of motion exercises and pain
If there is an PIP extension lag present, the patient needs to continue with the extension splint for a further two weeks, plus a further two weeks of night splinting in extension, if it is required.[21]
Post-Surgical Rehabilitation of Central Slip Repairs[edit | edit source]
Geoghegan et al (2018)[2] recently conducted a systematic review on treatments of central slip extensor tendon injuries. Different rehabilitation regimes are reported in the literature and these can be broadly classified into[2]:
- PIP joint immobilisation, followed by an isolated PIP flexion-extension exercise
- Controlled early active short arc motion
- PIP joint immobilisation followed by mobilisation with a dynamic spring coil finger splint
Evans et al (1994)[25] reported significantly better functional results in a cohort of early short arc motion compared to a cohort of prolonged immobilisation.
Early Short Arc Motion Regime[edit | edit source]
The basis for the early short arc motion regime is that sufficient tendon excursion is necessary to prevent adhesions. An arc of 30° of flexion at the PIP joint will achieve the desired amount of (3 -5 mm) of tendon excursion. With this protocol patients need to be seen on a weekly basis to monitor progress and monitor for an extensor lag. It is also necessary to remould the exercise splint.[25]
Splinting[edit | edit source]
Patients who have had a surgical repair of a central slip tendon injury will require different splints[25][2]:
- Full finger volar extension splint - worn at all times, except for during exercises
- Exercise splints:
- Volar slab from distal metacarpophalangeal (MCP) joint to the end of the finger - allowing 30° PIP joint flexion and 20° DIP flexion
- Short volar splint with PIP in neutral, but allowing DIP to flex over the top of the splint
Rehabilitation Exercises[edit | edit source]
These exercises are done in the different exercise splints usually made out of thermoplastic. The splints are also remoulded as the flexion angles increase.[21]
- Week 1: 30° PIP and 20° DIP flexion
- Week 2: 40° PIP and DIP flexion (if no extensor lag present)
- Week 3: 50° PIP and DIP flexion
- Week 4: 70° - 80° PIP and DIP flexion
- Week 5: full composite flexion
- Week 6 -8: light functional use allowed
- Week 8: Strengthening with Theraputty
- Perform exercises 3 times a day and 10 repetitions of each exercise
- Scar management is crucial for post-surgical zone III tendon repairs to prevent adhesions.
Red Flags[edit | edit source]
Some red flags to look out for when managing patients with central slip extensor repairs are[21]:
- Signs of infection
- PIP extensor lag
References[edit | edit source]
- ↑ de Jong JP, Nguyen JT, Sonnema AJ, Nguyen EC, Amadio PC, Moran SL. The incidence of acute traumatic tendon injuries in the hand and wrist: a 10-year population-based study. Clinics in orthopedic surgery. 2014 Jun 1;6(2):196-202.
- ↑ 2.0 2.1 2.2 2.3 2.4 Geoghegan L, Wormald JC, Adami RZ, Rodrigues JN. Central slip extensor tendon injuries: a systematic review of treatments. Journal of Hand Surgery (European Volume). 2019 Oct;44(8):825-32.
- ↑ Coons MS, Green SM. Boutonniere deformity. Hand clinics. 1995 Aug;11(3):387-402.
- ↑ Dr Thomas McClellan. What is a Boutonnière Deformity? Available from: http://www.youtube.com/watch?v=5M4wL-n_c3E [last accessed 5/10/2020]
- ↑ Levangie PK, Norkin CC. Joint Structure and function: a comprehensive analysis. 3rd. Philadelphia: FA. Davis Company. 2000.
- ↑ Johnson C, Swanson M, Manolopoulos K. A case report: Treatment of a zone III extensor tendon injury using a single relative motion with dorsal hood orthosis and a modified short arc motion protocol. Journal of Hand Therapy. 2019 May 10.
- ↑ Newton AW, Tonge XN, Hawkes DH, Bhalaik V. Key aspects of anatomy, surgical approaches and clinical examination of the hand. Orthopaedics and Trauma. 2019 Feb 1;33(1):1-3.
- ↑ Digital MEdIC at Stanford University. Anatomy of the Upper Limb: Extensor Expansion. Available from https://www.youtube.com/watch?v=G0v_wX8Ms4Y (last accessed 21 November 2020)
- ↑ Avery DM, Rodner CM, Edgar CM. Sports-related wrist and hand injuries: a review. Journal of orthopaedic surgery and research. 2016 Dec 1;11(1):99.
- ↑ Kim JP, Go JH, Hwang CH, Shin WJ. Restoration of the central slip in congenital form of boutonniere deformity: case report. J Hand Surg Am. 2014 Oct. 39 (10):1978-81.
- ↑ Feldon P, Terrono AL, Nalebuff EA, Millender LH. Rheumatoid arthritis and other connective tissue diseases. Wolfe SW, Hotchkiss RN, Pederson WC, Kozin SH, eds. Green’s Operative Hand Surgery. 6th ed. Philadelphia: Elsevier; 2011. 2: 2052-6
- ↑ Hertling D, Kessler RM. Management of common musculoskeletal disorders.4th ed. Philadelphia : Lippincott Williams & Wilkins;1983.
- ↑ Grandizio LC, Klena JC. Sagittal band, boutonniere, and pulley injuries in the athlete. Current reviews in musculoskeletal medicine. 2017 Mar 1;10(1):17-22.
- ↑ Nabil Ebraheim. Boutonniere Deformity Available from:https://www.youtube.com/watch?v=ncGPMKpKTv8 [last accessed 5/10/2020]
- ↑ 15.0 15.1 15.2 15.3 15.4 Yoon AP, Chung KC. Management of acute extensor tendon injuries. Clinics in plastic surgery. 2019 Jul 1;46(3):383-91.
- ↑ 16.0 16.1 Merritt WH, Wong AL, Lalonde DH. Recent Developments Are Changing Extensor Tendon Management. Plastic and Reconstructive Surgery. 2020 Mar 1;145(3):617e-28e.
- ↑ OrthoInfo. Boutonniere deformity. Available from:https://orthoinfo.aaos.org/en/diseases--conditions/boutonniere-deformity/ (accessed 4 October 2020)
- ↑ Boyes JH. Bunnell's Surgery of the Hand. 5th ed. Philadelphia: JB Lippincott; 1971. 393.
- ↑ Dr Vinay Kumar Singh. Elson's Test for Central Slip Injury. Available from: https://www.youtube.com/watch?v=eQbU0mPWtsE[last accessed 5/10/2020]
- ↑ CRTechnologies. Boyes Test (CR). Available from: https://www.youtube.com/watch?v=m71MIeqLzys [last accessed 5/10/2020]
- ↑ 21.0 21.1 21.2 21.3 21.4 21.5 Kate Thorn. Central Slip and Mallet Finger. Plus Course.2020
- ↑ Rehab my patient. Finger pain exercise. Available from https://www.youtube.com/watch?v=5qRb3ht3zsA. (last accessed 22 November 2020)
- ↑ Rehab my patient. How to get your grip back after injury. Available from https://www.youtube.com/watch?v=4NZ2drULuzc&feature=emb_logo. (last accessed 22 November 2020)
- ↑ Rehab my patient. How to improve finger strength using putty. Available from https://www.youtube.com/watch?v=wtSn4B8lKm4&feature=emb_logo (last accessed 22 November 2020)
- ↑ 25.0 25.1 25.2 Evans RB. Early active short arc motion for the repaired central slip. The Journal of hand surgery. 1994 Nov 1;19(6):991-7.