Boutonniere Deformity
Original Editor - Esraa Mohamed Abdullzaher
Top Contributors - Shreya Pavaskar, Wanda van Niekerk, Adu Omotoyosi Johnson, Esraa Mohamed Abdullzaher, Uchechukwu Chukwuemeka and Kim Jackson
Introduction[edit | edit source]
Extensor injuries of the hand are common in young, otherwise healthy males.[1] Various injury mechanisms include hyperflexion, direct blunt trauma and penetrating trauma. When left untreated, disruption of the extensor mechanism over zone III and detachment of the central slip leads to a Boutonniere deformity. This deformity is characterised by flexion of the proximal interphalangeal joint (PIP) and hyperextension of the distal interphalangeal joint (DIP) due to the volar subluxation of the lateral bands.[2]
Definition[edit | edit source]
A Boutonniere deformity is a deformity of the fingers in which the proximal interphalangeal joint (PIP) is flexed and the distal interphalangeal joint (DIP) is hyperextended.[2] It is an extensor tendon injury over zone III. It is also referred to as a "buttonhole deformity."[3]
Clinically relevant anatomy[edit | edit source]
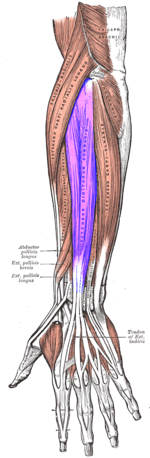
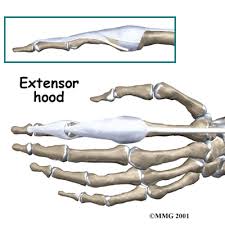
The Extensor Digitorum Communis(EDC) tendon at each finger splits into three bands or slips namely the central tendon/slip, which inserts on the base of the middle phalanx, and two lateral bands/slips, which rejoin as the terminal tendon/slip to insert into the base of the distal phalanx. In order to produce active interphalangeal extension, the EDC muscle requires the assistance of two intrinsic muscle groups, the interossei and the lumbricals, that also have attachments to the extensor hood and the lateral bands/slips. The EDC tendon and all its complicated active and passive interconnections at and distal to the metacarpophalangeal joint are known together as the extensor mechanism. The foundation of the extensor mechanism is formed by the tendons of the EDC muscle (with extensor indicis and extensor digiti minimi) and the extensor hood, the central tendon/slip, and the lateral bands/slips that merge into the terminal tendon/slip. The triangular ligament helps stabilize the bands on the dorsum of the finger. The triangular ligament provides stability to the lateral bands preventing palmar subluxation during flexion of the proximal interphalangeal joint.[5][6][7]
Aetiology[edit | edit source]
A Boutonniere Deformity (BD) may develop secondary to trauma to the extensor mechanism over zone III or zone IV (including a direct laceration to the extensor mechanism), secondary to rheumatoid arthritis (RA), and in the setting of burns. Reports of congenital Boutonniere deformities are also documented.[9]The pathogenesis of a BD varies according to its aetiology.[10]
Patients who suffer a traumatic BD may have been subject to a direct injury to the central slip or a force that placed the central slip on stretch, leading to failure of the extensor mechanism. Direct injuries can occur when lacerations disrupt the central slip. Central slip injuries may also occur in the setting of passively forced flexion of an actively extended PIP joint. In another scenario, a volar PIP joint dislocation can avulse the dorsal lip of the middle phalanx base and create a central slip disruption.[2]
In people with Rheumatoid Arthritis, Boutonniere deformities develop and progress as the soft tissues of the digit are compromised. The extensor mechanism is stretched as a result of synovial proliferation within the proximal interphalangeal joint (PIP). As a result of this, the central slip is compromised and unable to achieve full extension, therefore leading to a subtle extensor lag. With the PIP joint in slight flexion, the lateral bands are subluxated volar and become fixed volar to the axis of rotation. Furthermore, the oblique retinacular ligaments contract, resulting in hyperextension and restricted flexion at the DIP joint. In the early stages of Rheumatoid arthritis, the joints are still passively correctable, but as the disease progress and capsular tissues contract and fibrosis developing around the PIP joint, the deformity becomes fixed.[11][12]
Boutonniere deformities that develop secondary to burns may be due to direct trauma or injury of the central slip or due to infection.[13][14]
Mechanism[edit | edit source]
If the central slip of the digital expansion is ruptured, minimal deformity results as long as the transverse fibers of the expansion remain intact. If they are also torn, a deformity is produced at the PIP joint. In this case, all extensor force will be transmitted to the distal phalanx by intact lateral bands, producing hyperextension of the DIP joint. The PIP joint buckles into flexion and protrudes through the breach in the extensor hood. The two lateral bands will now run on the palmar aspect of the PIP joint and will exaggerate flexion.[15][16]
Signs and Symptoms[edit | edit source]
Signs of the classic boutonnière deformity can develop immediately following an injury to the finger or may occur 10 to 14 days after the initial injury.[18]
- Loss of extension at PIP joint and hyperextension at the DIP joint[18]
- The finger at the middle joint (PIP) cannot be straightened and the fingertip (DIP joint) cannot be bent
- A weak grip and an inability to grasp and manipulate small objects with the tip of the digit
- Swelling and pain occur and continue on the top of the middle joint of the finger[19]
There are 2 special tests that help in identifying injury to the extensor mechanism:
- Elson Test - Fixing PIP Joint at 90° and ask the patient to extend the DIP joint. A lax DIP joint, despite the patient's effort to extend, is a negative or normal finding (if the central slip is intact, the loose lateral bands/slips when the PIP is flexed prevent DIP extension). A positive finding is a rigid DIP joint because of increased unopposed pull through the lateral bands/slips.[18]
- Boyes Test - Extend PIP and ask to flex DIP; positive is unable to flex DIP actively[20]
Boyes test may become positive only in the late stages.
Treatment[edit | edit source]
[edit | edit source]
Treatment options include prolonged splinting or surgery for patients who present for evaluation with a chronic injury such as in patients with Rheumatoid arthritis.
| Stage | PIP Joint | DIP Joint |
|---|---|---|
| 1 - Mild,
Passively correctable, Normal articular surface. |
Splinting Injection and/or synovectomy | Extensor tenotomy |
| 2 - Moderate,
Passively correctable, Normal articular surface. |
Treat as stage 1 ± Extensor reconstruction | Extensor tenotomy |
| 2 - Moderate,
Partially passively correctable, Normal articular surface. |
Treat as stage 1 Convert to correctable Extensor reconstruction | Extensor tenotomy |
| 2 - Moderate to severely fixed,
Normal articular surface. |
Treat as above If correctable → Extensor reconstruction If not correctable →Salvage →Rarely volar release | Extensor tenotomy |
| 3 - Joint destruction | Arthrodesis or arthroplasty | Extensor tenotomy |
Physiotherapy management[edit | edit source]
Treatment for an acute injury is uninterrupted splinting of the PIP in full extension for 6 weeks. An extensor lag greater than 15° is an indication to splint the DIP joint in slight flexion for several weeks to allow healing.[23] After 6 weeks of immobilization, exercises are begun. The exercise involves two sequential maneuvers. The first is active assisted PIP joint extension. This will stretch the tight volar structures, will cause the lateral bands to ride dorsal to the PIP joint axis, and will put longitudinal tension on the lateral bands and oblique retinacular ligaments. The second maneuver is maximal active forced flexion of the DIP joint while the PIP joint is held at 0°or as close to that position as the PIP will allow. This will gradually stretch the lateral bands and oblique retinacular ligaments to their physiologic length. Continue splinting 2 to 4 weeks when not exercising. When full PIP joint extension can be maintained throughout the day, then night splinting only is appropriate. Length of treatment and splinting maybe several weeks.[15]
Surgical management[edit | edit source]
While nonsurgical treatment of boutonnière deformity is preferred, surgery is an option in certain cases, such as when:
- The deformity results from rheumatoid arthritis.
- The tendon is severed.
- A large bone fragment is displaced from its normal position.
- The condition does not improve with splinting.
Surgery can reduce pain and improve functioning, but it may not be able to fully correct the condition and make the finger look normal. If the boutonniere deformity remains untreated for more than 3 weeks, it becomes much more difficult to treat.[19]
Occupational Therapy[edit | edit source]
An Oval-8 Finger Splint which is basically a three point splint It holds PIP in a straight line and allows DIP to move freely. It is easily removable and washable. It is also available in a tube for more comfort and cushioning effect. Splinting is usually required for 6 weeks in conservative treatment.[26] DIP flexion exercises, with the PIP held in extension promotes pull through of the lateral Bands dorsally from the volar subluxed position.
Capener splint is a dynamic extension splint can also be introduced to improve strength and mobility.
References[edit | edit source]
- ↑ de Jong JP, Nguyen JT, Sonnema AJ, Nguyen EC, Amadio PC, Moran SL. The incidence of acute traumatic tendon injuries in the hand and wrist: a 10-year population-based study. Clinics in orthopedic surgery. 2014 Jun 1;6(2):196-202.
- ↑ 2.0 2.1 2.2 Geoghegan L, Wormald JC, Adami RZ, Rodrigues JN. Central slip extensor tendon injuries: a systematic review of treatments. Journal of Hand Surgery (European Volume). 2019 Oct;44(8):825-32.
- ↑ Coons MS, Green SM. Boutonniere deformity. Hand clinics. 1995 Aug;11(3):387-402.
- ↑ Dr Thomas McClellan. What is a Boutonnière Deformity? Available from: http://www.youtube.com/watch?v=5M4wL-n_c3E [last accessed 5/10/2020]
- ↑ Levangie PK, Norkin CC. Joint Structure and function: a comprehensive analysis. 3rd. Philadelphia: FA. Davis Company. 2000.
- ↑ Johnson C, Swanson M, Manolopoulos K. A case report: Treatment of a zone III extensor tendon injury using a single relative motion with dorsal hood orthosis and a modified short arc motion protocol. Journal of Hand Therapy. 2019 May 10.
- ↑ Newton AW, Tonge XN, Hawkes DH, Bhalaik V. Key aspects of anatomy, surgical approaches and clinical examination of the hand. Orthopaedics and Trauma. 2019 Feb 1;33(1):1-3.
- ↑ Digital MEdIC at Stanford University. Anatomy of the Upper Limb: Extensor Expansion. Available from https://www.youtube.com/watch?v=G0v_wX8Ms4Y (last accessed 21 November 2020)
- ↑ Kim JP, Go JH, Hwang CH, Shin WJ. Restoration of the central slip in congenital form of boutonniere deformity: case report. J Hand Surg Am. 2014 Oct. 39 (10):1978-81.
- ↑ Feldon P, Terrono AL, Nalebuff EA, Millender LH. Rheumatoid arthritis and other connective tissue diseases. Wolfe SW, Hotchkiss RN, Pederson WC, Kozin SH, eds. Green’s Operative Hand Surgery. 6th ed. Philadelphia: Elsevier; 2011. 2: 2052-6
- ↑ Dwivedi S, Testa EJ, Modest JM, Ibrahim Z, Gil JA. Surgical Management of Rheumatoid Arthritis of the Hand. Rhode Island Medical Journal. 2020 May 1;103(4):32-6.
- ↑ Muir IFK, Barclay TL. Burns and Their Treatment. London: Lloyd-Luke; 1962. 109
- ↑ Grishkevich VM. Surgical treatment of postburn boutonniere deformity. Plast Reconstr Surg. 1996 Jan. 97 (1):126-32.
- ↑ Tsuge K. Congenital aplasia or hypoplasia of the finger extensors. Hand. 1975 Feb. 7(1):15-21.
- ↑ 15.0 15.1 Hertling D, Kessler RM. Management of common musculoskeletal disorders.4th ed. Philadelphia : Lippincott Williams & Wilkins;1983.
- ↑ Grandizio LC, Klena JC. Sagittal band, boutonniere, and pulley injuries in the athlete. Current reviews in musculoskeletal medicine. 2017 Mar 1;10(1):17-22.
- ↑ Nabil Ebraheim. Boutonniere Deformity Available from:https://www.youtube.com/watch?v=ncGPMKpKTv8 [last accessed 5/10/2020]
- ↑ 18.0 18.1 18.2 Yoon AP, Chung KC. Management of acute extensor tendon injuries. Clinics in plastic surgery. 2019 Jul 1;46(3):383-91.
- ↑ 19.0 19.1 OrthoInfo. Boutonniere deformity. Available from:https://orthoinfo.aaos.org/en/diseases--conditions/boutonniere-deformity/ (accessed 4 October 2020)
- ↑ Boyes JH. Bunnell's Surgery of the Hand. 5th ed. Philadelphia: JB Lippincott; 1971. 393.
- ↑ Dr Vinay Kumar Singh. Elson's Test for Central Slip Injury. Available from: https://www.youtube.com/watch?v=eQbU0mPWtsE[last accessed 5/10/2020]
- ↑ CRTechnologies. Boyes Test (CR). Available from: https://www.youtube.com/watch?v=m71MIeqLzys [last accessed 5/10/2020]
- ↑ 23.0 23.1 Williams K, Terrono AL. Treatment of boutonniere finger deformity in rheumatoid arthritis. The Journal of hand surgery. 2011;36(8):1388-93.
- ↑ OrthoMontana. Wrist & Hand Rehab Techniques Following Sports Injury. Available from: https://www.youtube.com/watch?v=XEcQZ6fISqQ&t=4s [last accessed 5/10/2020]
- ↑ RMCrayne. ROM Therapy Strategies for Fingers. Available from:https://www.youtube.com/watch?v=fgunRLNQMs8&t=1s [last accessed 5/10/2020]
- ↑ Moussallem CD, El-Labaky CY, El-Yahchouchi CA, Hoyek FA, Lahoud JC. Extensor Tendon Injuries. Journal of Hand Surgery. 2011;36(2):368.
- ↑ 3-Point Products. How to Treat Boutonniere Deformity with an Oval-8 Finger Splint . Available from: https://www.youtube.com/watch?v=d_QrmReS--M&t=3s [last accessed 5/10/2020]
- ↑ Orfit Industries. Capener orthosis - Orficast Instructional Movie 3. Available from: https://www.youtube.com/watch?v=j3sscSSHe1E [last accessed 5/10/2020]
.