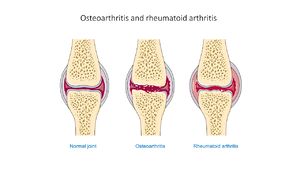
Arthritis
Overview[edit | edit source]
Arthritis is a broad and complex topic with many types, subtypes, and variations. It is defined as an acute or chronic joint inflammation that often co-exists with pain and structural damage. Arthritis affected both the Neanderthals and ancient Egyptians, Arthritis describes a set of symptoms that includes pain, stiffness, and joint deformities after an inflammatory process. The destructive process can occur through multiple pathways. Knowing the type of arthritis a person has means that informed decisions can be made.
Anyone can get arthritis, including children and young people. It can affect people from all backgrounds, ages, and lifestyles.[1]
Etiology[edit | edit source]
The cause of arthritis can differ depending on the type. Osteoarthritis is mainly caused by factors such as aging, being female, joint injuries, and being overweight. There are also some genetic factors that have been identified, such as mutations in genes that encode for types II, IV, V, and VI collagens.[2]
Arthritis can refer to over 150 different conditions that affect the muscles, bones, and joints. These include:
- Degenerative disease (osteoarthritis)
- Post-traumatic arthritis
- Spondyloarthritis (including Psoriatic Arthritis, Ankylosing Spondylitis (Axial Spondyloarthritis), Reactive Arthritis, and Enteropathic Arthritis)
- Auto-immune or auto-inflammatory processes (rheumatoid arthritis and ankylosing spondylitis)
- Crystal deposition (gout and pseudogout)
- Infection (septic arthritis)
- Idiopathic (juvenile idiopathic arthritis).
Many diseases can result in arthritis. Examples include systemic lupus erythematosus, psoriasis, Lyme disease, reactive arthritis, and celiac disease among numerous others.[3]
Other conditions that have similar symptoms to arthritis
- Lupus
- Fibromyalgia
- Polymyalgia rheumatica
- Mechanical low back pain/mechanical neck pain
- Tendinopathy
Healthcare Team Management[edit | edit source]
Arthritis may be a disease of the joint but it also has systemic repercussions. The management of arthritis is ideally done by an interprofessional team that includes a nurse, dietitian, rheumatologist, physical therapist, orthopedic surgeon, pain specialist, pharmacist, and a Physician.
Almost all patients may benefit from physical therapy. Ample evidence indicates that water-based exercise can diminish pain and improve joint function. Further, loss of weight also decreases the stress on the joint.
Polypharmacy is a major concern in these patients because of the need to resolve the pain, hence the pharmacist should closely monitor the medications to prevent serious drug interactions and if narcotics are required, monitor for overuse[4].
Clinical Presentation[edit | edit source]
Arthritis affects people in different ways and each condition will have specific symptoms. However, common symptoms are:
- Pain
- Swelling, redness, and warmth in a joint
- Joint swelling that lasts for more than three days
- Joint swelling that occurs more than three times a month
- Difficulty moving a joint
- Stiffness or reduced movement of a joint
- In the morning (how long does it last?)
- The following exercise
- After you’ve been sitting for a while
- After exercising
- Certain types of arthritis can have symptoms not directly related to your joints.
- Fatigue
- Scaly, itchy skin
- Changes to finger and toenails
- Rashes
- Fever
- Weight loss
- Hair loss in spots or around the hairline [5]
Diagnostic Procedures[edit | edit source]
Numerous exams and tests are needed to diagnose which arthritis is present. Including
- Medical history – finding out about symptoms, family history, and other health problems in the past.
- Physical examination – look for redness and swelling in and around the joint, and check out the range of movement of your joints. Depending on the type of arthritis also look for rashes, check your eyes and throat, and measure your temperature.
- Scans and other tests – again, depending on the type of arthritis test may include: blood tests to check for levels of inflammation in blood or specific genetic markers; X-rays; Ultrasonography; CT (computed tomography) or MRI (magnetic resonance imaging)[6].
- Referral to a specialist – if appropriate your doctor will refer you to a specialist, often a rheumatologist, for diagnosis and specialized management of your condition.[7]
Management / Interventions[edit | edit source]
Living with arthritis can be different from person to person, and symptoms can vary from day to day. Treatment and management options vary with the type of arthritis, its severity, and the parts of the body affected.
There is no cure for arthritis. Management options can include medical treatment and medication, physiotherapy, exercise, and self-management techniques.
A range of health professionals in the management of arthritis, including:
- General practitioner (GP) – central to your care and will help you manage day-to-day, as well as help access other health professionals and services
- Rheumatologist
- Physiotherapist
- Dietitian
- Occupational therapist
- Exercise physiologist
- Podiatrist
- Pharmacist
- Psychologist[7]
Medication[edit | edit source]
Non-inflammatory types of arthritis, such as osteoarthritis, are often treated with pain-reducing medications, physical activity, weight loss if the person is overweight, and self-management education.
These treatments are also applied to inflammatory types of arthritis, such as Rheumatoid Arthritis (RA), along with anti-inflammatory medications such as corticosteroids and non-steroidal anti-inflammatory drugs (NSAIDs), disease-modifying anti-rheumatic drugs (DMARDs), and a relatively new class of drugs known as biologics.
Medications will depend on the type of arthritis. Commonly used drugs include:
- Analgesics: these reduce pain, but do not affect inflammation. Examples include acetaminophen (Tylenol), tramadol (Ultram), and narcotics containing oxycodone (Percocet, Oxycontin) or hydrocodone (Vicodin, Lortab). Tylenol is available to purchase online.
- Non-steroidal anti-inflammatory drugs (NSAIDs): these reduce both pain and inflammation. NSAIDs are available to purchase over-the-counter or online, including ibuprofen (Advil, Motrin IB) and naproxen sodium (Aleve). Some NSAIDs are available as creams, gels, or patches which can be applied to specific joints.
- Counterirritants: some creams and ointments contain menthol or capsaicin, the ingredient that makes hot peppers spicy. Rubbing these on the skin over a painful joint can modulate pain signals from the joint and lessen pain. Various creams are available to purchase online.
- Disease-modifying antirheumatic drugs (DMARDs): used to treat RA, DMARDs slow or stop the immune system from attacking the joints. Examples include methotrexate (Trexall) and hydroxychloroquine (Plaquenil)[4].
- Biologics: used with DMARDs, biologic response modifiers are genetically engineered drugs that target various protein molecules involved in the immune response. Examples include etanercept (Enbrel) and infliximab (Remicade).
- Corticosteroids: prednisone and cortisone reduce inflammation and suppress the immune system.[8][9]
Self-Management[edit | edit source]
Key strategies include:
- staying physically active
- achieving and maintaining a healthy weight
- getting regular check-ups with the doctor
- protecting joints from unnecessary stress
- Adding exercises to the daily routine under the supervision of a physiotherapist.
Seven habits that can help a person with arthritis to manage their condition are:
- Being organized: keep track of symptoms, pain levels, medications, and possible side effects for consultations with your doctor.
- Managing pain and fatigue: a medication regimen can be combined with non-medical pain management. Learning to manage fatigue is key to living comfortably with arthritis.
- Staying active: exercise is beneficial for managing arthritis and overall health.
- Balancing activity with rest: in addition to remaining active, rest is equally important when your disease is active.
- Eating a healthful diet: a balanced diet can help you achieve a healthy weight and control inflammation. Avoid refined, processed foods and pro-inflammatory animal-derived foods, and choose whole plant foods that are high in antioxidants and that have anti-inflammatory properties.
- Improving sleep: poor sleep can aggravate arthritis pain and fatigue. Take steps to improve sleep hygiene so you find it easier to fall asleep and stay asleep. Avoid caffeine and strenuous exercise in the evenings and restrict screen time just before sleeping.
- Caring for joints: tips for protecting joints include using the stronger, larger joints as levers when opening doors, using several joints to spread the weight of an object such as using a backpack, and gripping as loosely as possible by using padded handles.
Do not sit in the same position for long periods. Take regular breaks to keep mobile.[9]
The Role of Exercise in Management[edit | edit source]
This brief video explains the role of exercise.
Recommended Exercises[edit | edit source]
- Exercises will differ as per the type of arthritis and the joint involved.
- Osteoarthritis of the knee is the most common form of arthritis and exercises like quadriceps strengthening, SLR, VMO strengthening, and weight-bearing exercises are prescribed.
Conclusion and Physiotherapist Role in Management[edit | edit source]
Arthritis is a broad and complex topic that encompasses many types, subtypes, and variations. The above paragraph provides a brief overview of this extensive subject and includes links to specific pages for more information. Physical therapists are well-trained and licensed in rehabilitation techniques and can help restore function and prevent disability for individuals affected by arthritis. They can also develop exercise programs that can help alleviate pain and improve the functioning of the joint and musculoskeletal areas impacted by arthritis. Physical therapists can educate patients about the disease and explain the lifestyle modifications necessary for managing the condition in the long term. Arthritis requires long-term changes to manage the disease effectively.
References[edit | edit source]
- ↑ Ma L, Cranney A, Holroyd-Leduc JM. Acute monoarthritis: what is the cause of my patient's painful swollen joint? CMAJ. 2009 Jan 6;180(1):59-65.
- ↑ Shayan Senthelal, Thomas MA. Arthritis [Internet]. Nih.gov. StatPearls Publishing; 2018. Available from: https://www.ncbi.nlm.nih.gov/books/NBK518992/
- ↑ Senthelal S, Thomas MA. Arthritis. InStatPearls [Internet] 2019 Aug 22. StatPearls Publishing.
- ↑ 4.0 4.1 Singh JA, Furst DE, Bharat A, Curtis JR, Kavanaugh AF, Kremer JM, Moreland LW, O'Dell J, Winthrop KL, Beukelman T, Bridges SL Jr, Chatham WW, Paulus HE, Suarez-Almazor M, Bombardier C, Dougados M, Khanna D, King CM, Leong AL, Matteson EL, Schousboe JT, Moynihan E, Kolba KS, Jain A, Volkmann ER, Agrawal H, Bae S, Mudano AS, Patkar NM, Saag KG. 2012 update of the 2008 American College of Rheumatology recommendations for the use of disease-modifying antirheumatic drugs and biologic agents in the treatment of rheumatoid arthritis. Arthritis Care Res (Hoboken). 2012 May;64(5):625-39.
- ↑ Recognizing the Symptoms of Arthritis [Internet]. www.arthritis.org. Available from: https://www.arthritis.org/health-wellness/about-arthritis/understanding-arthritis/recognizing-the-symptoms-of-arthritis
- ↑ Hayashi D, Roemer FW, Guermazi A. Imaging for osteoarthritis. Ann Phys Rehabil Med. 2016 Jun;59(3):161-169.
- ↑ 7.0 7.1 Arthritis [Internet]. Vic.gov.au. 2012. Available from: https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/arthritis
- ↑ McAlindon TE, Bannuru RR, Sullivan MC, Arden NK, Berenbaum F, Bierma-Zeinstra SM, Hawker GA, Henrotin Y, Hunter DJ, Kawaguchi H, Kwoh K, Lohmander S, Rannou F, Roos EM, Underwood M. OARSI guidelines for the non-surgical management of knee osteoarthritis. Osteoarthritis Cartilage. 2014 Mar;22(3):363-88.
- ↑ 9.0 9.1 Arthritis: Causes, types, and treatments [Internet]. www.medicalnewstoday.com. 2017. Available from: https://www.medicalnewstoday.com/articles/7621#treatment
- ↑ Available from:Arthritis Pain Management Help.https://youtu.be/3RnkZ6ohiuo. Arthritis and Exrcise-Best Exercises to help Arthritis(last accessed 28 April 2020)