An Introduction to Red Flags in Serious Pathology
Introduction[edit | edit source]
Only around 1% of all musculoskeletal presentations in primary care will be due to serious pathology.[1][2] Such pathologies include spinal infection, cauda equina, fracture, and malignancy.[3] Vertebral fracture is the most common serious spinal pathology, followed by metastatic bone disease.[4]
Yet despite the low incidence rates, these conditions should be considered as differential diagnoses when individuals present with back pain - particularly if the patient is not responding in an expected way or is starting to worsen.[1] Identifying serious pathology early on is very important for a number of reasons:
- Prognosis improves with early diagnosis
- Patients tolerate treatment better
- Outcomes are better
- Quality of life is better maintained[1]
However, it can be challenging identifying serious pathologies as they often masquerade as musculoskeletal conditions, particularly in the early stages of disease. As a disease progresses, it becomes easier to identify as patients become systemically unwell.[1]
"Our job as health professionals is to try and identify [serious pathologies] early." -- Laura Finucane
What are Red Flags?[edit | edit source]
"Red Flags (RFs) are signs and symptoms related to the screening of serious underlying pathologies mimicking a musculoskeletal pain."[5]
Red flags are specific attributes derived from a patient's medical history and the clinical examination that are usually linked with a high risk of having a serious disorder like an infection, cancer, or a fracture.[6]
- Red flags are not diagnostic tests and they don't necessarily predict diagnosis or prognosis but are rather clinical prediction guides.
- Their main function is to raise the therapist's suspicion when they are combined[6]
The flag system describes clinical and psychological flags and is comprised of red, orange, yellow, blue and black. To find out more about different types of flags, please see: The Flag System. To learn more about an unofficial type of flags proposed by Louis Gifford, please see: Pink Flags and Tendons.
- Clinical flags are common to many areas of health – for example, red flags are indicators of possible serious pathology such as inflammatory or neurological conditions, structural musculoskeletal damage or disorders, circulatory problems, suspected infections, tumours or systemic disease.
- If suspected, these require urgent further investigation and often surgical referral.
Red flag screening questions were developed to help detect serious spinal pathology.[1]
- Specific red flag questions are not used consistently across guidelines and there is little evidence to support their use[7][8][9]
- There are 163 different items that could be considered to be red flags, all of which are subject to interpretation.[10] This includes:[10]
- 119 items in the patient history
- 44 items in the physical assessment
- Because of these factors, the benefit of using red flags has been questioned.[10] Yet a clinician still needs to determine if a patient’s presenting condition is suitable for conservative management or if a referral is necessary.
"Therefore in spite of no consensus in either guidelines or research, red flags are still seen as the most reliable clinical indicator for potential serious pathology and remain fundamental to the assessment process."[10]
Common Red Flags[edit | edit source]
- Age over 50 years
- Progressive symptoms
- Thoracic pain
- Past history of cancer
- Weight loss
- Drug abuse
- Night pain
- Systemically unwell (fever)
- Night sweats[1]
Evidence for Red Flags[edit | edit source]
"So, we know that red flags are clinical indicators of possible serious spinal pathology. They are physical manifestations of underlying significant medical pathology. And we've used these historically for many years [...] But there are a list of items that we need to interpret. And my interpretation of those red flags may be very different to your interpretation and someone else's interpretation." -- Laura Finucane[1]
Certain red flags have been shown to have good accuracy. These include:
- recent trauma and age more than 50 years are associated with vertebral fracture[7]
- similarly, a “history of cancer” and “strong clinical suspicion” have empirical evidence of high diagnostic accuracy for malignancy[11]
On the whole, it is argued that red flag screening for low back pain has not been used successfully:[8]
- red flags generally have poor diagnostic accuracy[7]
- there is a lack of consensus in guidelines as to which red flags should be used[12] or when clinicians should act[1]
According to Cook et al.,[8] there are four key reasons why red flag screening has not been successful:
- Red flag symptoms do not rule out serious spinal pathology, but they do not identify it either. The clinical tests for red flags do not have low negative likelihood ratios, which means they cannot "rule out" a red flag even when the test is negative.[8]
- There is great variability in how red flags are defined, which limits research and clinical progress.[8]
- Most guidelines recommend screening for red flags and then encourage anyone who presents with red flags to undergo extensive diagnostic testing,[8] even if only one symptom is present. However, at least 80% of patients will have at least one red flag.[1] Moreover, it is important to remember that "true screening" really only can occur in a pre-clinical phase when there are no outward symptoms of a disease (ie before a physiotherapist would see a patient). Thus, our red flag "screening" is actually a management strategy that does not involve any screening in the medical sense.[8]
- Clinicians are not screening for red flags, but rather are managing the conditions that they see. And as Cook et al. note, red flag findings are more related to prognosis than to serious pathology (ie fracture, cancer).[8]
Alternative Approach for Clinical Practice[edit | edit source]
It is still recommended that health professionals use red flags to identify potential serious pathology.[10]
- Recent research focused on creating an alternative approach to red flag screening.
- A key aspect of this framework is a greater focus on the context of the red flag.
- A patient's entire history must be considered and clinicians must ask for enough detail to understand the context behind answers to red flag screening questions.[1]
For example:
- History of Cancer: it is important to enquire where the original cancer was. Certain types of cancer would heighten the index of suspicion of metastases in the spine.[1] The five types of cancer that are most likely to spread to the spine are:
- Weight Loss: unexplained weight loss is a cause for concern (weight loss would be expected if a patient has been on a diet, exercising more, or if they are taking new medications or have pain as these factors can suppress a patient’s appetite).[1]
- Night Pain: many patients with back pain will complain of night pain. It is important to find out more about the quality of this pain. A patient who is able to get back to sleep will not generate the same level of suspicion as a patient who cannot get back to sleep or has to get up to sit in a chair to get back to sleep.[1]
The Framework[edit | edit source]
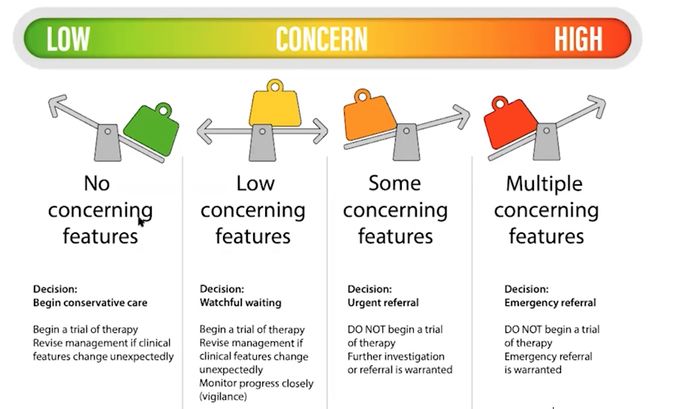
Level of Concern[edit | edit source]
The level of concern is considered (please see Figure 2). The framework encourages clinicians to not simply rely on one red flag, but rather to consider the context of the patient and the context of the red flag/s, including symptom progression and co-morbidities.[13]
Decision[edit | edit source]
The clinician needs to decide if there is a level of concern. If there is none, management can begin. If there is some concern, the clinician could consider a trial treatment but will need to monitor the patient over time and revise the management if necessary. Red flags should be regularly considered and re-evaluated. It is not enough to simply consider red flags at the initial assessment.[13]
If there are more concerning features, the clinician needs to consider their urgency. Is it a medical emergency (eg cauda equina) that requires immediate action or potential metastases, which could wait a few days, but still requires urgent referral?[13]
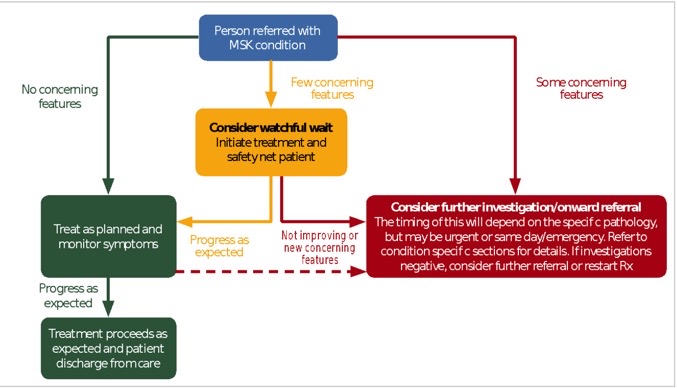
Pathway[edit | edit source]
The pathway helps clinicians understand what they should do with patients who present with concerning features. This pathway is moveable and flexible - a patient can move between pathways.[13]
Summary[edit | edit source]
- Identifying serious pathology early is vital:
- patients tolerate treatment better
- outcomes are better
- quality of life is improved
- It can be challenging to identify serious pathologies as they may masquerade as musculoskeletal conditions, particularly in the early stages
- We must, therefore, consider serious pathology as a differential diagnosis. We need to consider how a red flag presents for a particular patient. Context is essential.
- Red flags should be re-evaluated at every session.
- It is important to identify which pathway a patient should be on, to ensure that they receive the correct care in a timely fashion.
References[edit | edit source]
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 Finucane L. An Introduction to Red Flags in Serious Pathology Course. Plus, 2020.
- ↑ Melman A, Maher CG, Needs C, Machado GC. Many people admitted to hospital with a provisional diagnosis of nonserious back pain are subsequently found to have serious pathology as the underlying cause. Clin Rheumatol. 2022 Jun;41(6):1867-71.
- ↑ Chu EC, Trager RJ. Prevalence of serious pathology among adults with low back pain presenting for chiropractic care: a retrospective chart review of integrated clinics in Hong Kong. Med Sci Monit. 2022 Sep 27;28:e938042.
- ↑ Finucane L, Greenhalgh S, Selfe J. Which red flags aid the early detection of metastatic bone disease in back pain? Physiotherapy Practice and Research. 2017;38(2): 73-77.
- ↑ Maselli F, Palladino M, Barbari V, Storari L, Rossettini G, Testa M. The diagnostic value of Red Flags in thoracolumbar pain: a systematic review. Disabil Rehabil. 2022 Apr;44(8):1190-1206.
- ↑ 6.0 6.1 Finucane LM, Downie A, Mercer C, Greenhalgh SM, Boissonnault WG, Pool-Goudzwaard AL et al. International Framework for Red Flags for Potential Serious Spinal Pathologies. J Orthop Sports Phys Ther. 2020;50(7):350-372.
- ↑ 7.0 7.1 7.2 Premkumar A, Godfrey W, Gottschalk MB, Boden SD. Red Flags for Low Back Pain Are Not Always Really Red. J Bone Jt Surg. 2018;100(5):368–74.
- ↑ 8.0 8.1 8.2 8.3 8.4 8.5 8.6 8.7 Cook CE, George S Z, Reiman M P. Red flag screening for low back pain: nothing to see here, move along: a narrative review. British Journal of Sports Medicine. 2018;52: 493–496.
- ↑ Budtz CR, Rønn-Smidt H, Thomsen JNL, Hansen RP, Christiansen DH. Primary care physical therapists' experiences when screening for serious pathologies among their patients: a qualitative study. Phys Ther. 2022 May 5;102(5):pzac026.
- ↑ 10.0 10.1 10.2 10.3 10.4 Yusuf M, Finucane L, Selfe J. Red flags for the early detection of spinal infection in low back pain. BMC Musculoskeletal Disorders. 2019; 20(606).
- ↑ Verhagen AP, Downie A, Maher CG, Koes BW. Most red flags for malignancy in low back pain guidelines lack empirical support: a systematic review. Pain. 2017;158(10):1860-8.
- ↑ Verhagen AP, Downie A, Popal N, Maher C, Koes BW. Red flags presented in current low back pain guidelines: a review. European Spine Journal. 2016 Sep 1;25(9):2788-802.
- ↑ 13.0 13.1 13.2 13.3 Finucane L, Selfe J, Mercer C, Greenhalgh S, Downie A, Pool A et al. An evidence informed clinical reasoning framework for clinicians in the face of serious pathology in the spine course slide. Plus2020.