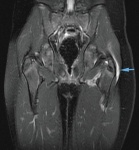
Trochanteric Bursitis
Original Editors - Emy Van Rode as part of the Vrije Universiteit Brussel's Evidence-based Practice project
Top Contributors - Mudra Shah, Emy Van Rode, Lionel Geernaert, Gertjan Van Gijsegem, Lena Vanderaa, Wendy Snyders, Admin, Kim Jackson, Andrea Nees, Rachael Lowe, Uchechukwu Chukwuemeka, Vidya Acharya, Wanda van Niekerk, WikiSysop and Claire Knott
Definition/Description[edit | edit source]
Trochanteric bursitis was first described in 1923 [1][2]and was used to describe lateral hip pain[2][3] thought to be caused by inflammation of the trochanteric bursa.
The continued use of trochanteric bursitis for lateral hip pain is however unsuitable as bursitis implies inflammation yet three of the four cardinal inflammatory signs, namely rubor, tumour and calor[1][2] [4]are rarely present[1][2]. Studies have revealed that trochanteric bursitis is rarely present in isolation [3][5] and that there is a low prevalence of trochanteric bursa inflammation[3][6] in patients with lateral hip pain. More recently it has become clear that gluteal tendon pathology (gluteal tendinopathy or gluteal tendon tears[1][2][3][7][8]or external coxa saltans [9][4] is more likely the primary cause of the lateral hip pain and that associated trochanteric bursitis can be present[1][2][3][7][8]. The gluteal tendon pathology or external coxa saltans with the possible associated trochanteric bursitis is now referred to as greater trochanteric pain syndrome (GTPS)[2][6][7][8]. If there is GTPS and an associated bursitis, the bursitis can occur in the subgluteus maximus (trochanteric bursa), subgluteus medius or subgluteus minimus bursa but it most commonly occurs in the trochanteric bursa[8].
In the rarer cases of isolated trochanteric bursitis, the causes could include:
If inflammatory signs such as redness, swelling and warmth are present, septic arthritis should be suspected[8][10]. Sometimes septic bursitis can be present without these inflammatory signs and then aspiration is needed to confirm the diagnosis[10]. It can be acute, sub-acute or chronic[10].
- Other causes of trochanteric bursitis
Certain auto-immune diseases such as rheumatoid arthritis (RA) can lead to trochanteric bursitis[11] as well as crystal arthropathies such as gout[8]. Direct trauma could potentially also lead to isolated trochanteric bursitis. Isolated trochanteric bursitis due to repetitive rubbing/friction is possible[9] but is very rare[3].
Clinically Relevant Anatomy[edit | edit source]
A bursa is a sac that usually contains a small amount of fluid and functions as a friction-reducing structure between two anatomical structures, e.g. bone and tendon[8][12]. Bursitis is characterised by soft-tissue swelling, localised pain, synovial thickening and increased fluid in the bursa[12].
The trochanteric bursa covers the posterior facet and lies deep into the gluteus maximus muscle. It also lies over the trochanter attachments of gluteus medius, gluteus minimus and vastus lateralis[8]. The sub gluteus medius bursa is situated at the lateral and superolateral facets deep to the gluteus medius tendon insertion while the sub gluteus minimus bursa is located between the anterior facet and gluteus minimus tendon[8].
Epidemiology /Etiology[edit | edit source]
When there is GTPS with associated trochanteric bursitis, the following are possible causes/contributing factors:
- direct trauma
- mechanical overload[4][13]
- overuse[4]
- compression of the tendon (and bursa)[13]
- female gender[8]
- poor pelvic control or weak hip abductors[13]
- external coxa saltans[4][9]
- Gluteus medius [14] and minimus tears (degenerative or traumatic)
- Obesity[15]
GTPS is more common in women in their 4th to 6th decades of life[1][7]. A recent study found that only 2% of women had isolated trochanteric bursitis, while 25% had hip abductor tendon pathology with an associated trochanteric bursitis[3].
Septic bursitis occurs when bacteria is introduced into the bursa[14] and can occur due to:
- Tuberculosis infection (less than 2% of musculoskeletal tuberculosis presents as septic trochanteric bursitis)[4][8][16]
- Direct puncture of the skin[10]
- Micro-trauma[10]
- Cellulitis of the skin that is adjacent to the bursa[10]
Most cases of acute septic bursitis involve Staphylococcus aureus, followed by Streptococcus[10] . Atypical mycobacteria or fungi are associated with chronic septic bursitis[10]. Septic bursitis, in general, is more common in men around the age of 50 years[10]. People who are more susceptible to septic arthritis, in general, include those with inflammatory arthritis (e.g. RA) and those with crystal arthropathies like gout (19).
Characteristics/Clinical Presentation[edit | edit source]
- Lateral hip pain[2][8][17]
- Pain to the lateral thigh and knee[2][8][17]
- Local tenderness over the greater trochanter[2][8][17]
- Pain with side-lying on the affected side[2][8][17] and sometimes when lying on the unaffected side too due to hip adduction on the affected side[17]
- Pain with weight-bearing activities[2][8][17]
- Pain with sitting crossed-legged[17]
- Pain with prolonged sitting[2][8]
Diagnostic Procedures[edit | edit source]
There is no one specific test to confirm GTPS. Please see the GTPS page for a complete list of the tests that can be used. Concerning imaging, ultrasound can be used but is only indicated if conservative management has failed[8][17]; if the diagnosis is unclear[8][17] or if the primary pathology is thought to be a gluteal tear[8]. MRI can be used for differential diagnosis[1][17].
In septic arthritis, antibiotics should only be started after blood cultures and inflammatory marker investigations have been done and should include white blood count, C-reactive protein and erythrocyte sedimentation[10]. Currently, the gold standard for diagnosis is aspiration and analysis of the bursal fluid[10]. Uric acid and rheumatoid factor should be ordered if one of these is suspected[10]. Imaging does not help diagnose septic arthritis and should only be conducted if other pathology, such as septic arthritis, is suspected[10].
Differential Diagnosis[edit | edit source]
Multiple structures can present as lateral hip pain. In the absence of inflammatory signs, differential diagnosis can include:
- GTPS, including external coxa saltans[4][9], gluteal tendinopathy[1][2][3]and gluteal tears[1][2][3].
- Referred pain from the lumbar spine[8][17]
- Hip osteoarthritis[8][17]
- Femoroacetabular impingement[8][17]
- Femoral head stress fracture[8]
- Labral tears[8][17]
- Bony metastasis[17]
- Neck-of-femur fracture[17]
- Rheumatoid arthritis[17]
- Femoral head avascular necrosis[8]
If inflammatory signs are present:
Outcome Measures[edit | edit source]
• VISA-G - GTPS-specific outcome measure[18]
Physiotherapy Management[edit | edit source]
If trochanteric bursitis is associated with GTPS, the primary problem will need to be addressed. Please see the Physiopedia pages GTPS, gluteal tendinopathy and coxa saltans on how to manage the primary problems of the associated trochanteric bursitis. For the management of specifically the associated bursitis, please see the medical and surgical management below. The videos below simplifies Trochantric bursitis and it's physiotherapy management
Medical Management[edit | edit source]
Corticosteroid injections can be used to manage the associated bursitis in GTPS but they only provide short-term relief[6]. Platelet-rich plasma (PRP) has also been found to be a feasible option[21][22], but it is unknown whether corticosteroid injections or PRP are more effective.
Non-steroidal anti-inflammatory drugs (NSAIDs) may provide analgesia in the acute phase of GTPS or primary bursitis. Still, if the GTPS is chronic, NSAIDs are not advised as they may have a detrimental effect on tendon healing[8].
Septic bursitis is managed with antibiotics and if pain management is needed, NSAIDs can be used[10]. If the NSAIDs are insufficient, corticosteroid injection can be used[10]. TB trochanteric bursitis is also managed with antibiotics but treatment continues for much longer, usually 6-18 months[23].
Surgical Management[edit | edit source]
Indications for surgery for septic arthritis include[10] significant swelling, severe cases that aren’t responding to antibiotics alone or chronic or recurrent cases. Operative interventions include:
- Suction irrigation[10]
- Needle aspiration in conjunction with systemic antibiotics[10]
- If aspiration fails, incision and drainage[10]
- Bursectomy[10][16][23]
In GTPS, surgical intervention is only indicated if conservative management has failed[7] or if there is a significant tendon tear[17]. Surgical options for GTPS, without a tendon tear, that are safe and effective include:
- Bursectomy[24] [25](arthroscopic)
- Iliotibial tract (ITT) release[26]
- ITT bursectomy[26]
For gluteal tendon tears, a reconstruction/repair[27] [28]is done. Please see this reference[27] for the rehabilitation protocol after abductor tendon repair.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 1.7 1.8 Hilligsøe M, Rathleff MS, Olesen JL. Ultrasound definitions and findings in greater trochanteric pain syndrome: a systematic review. Ultrasound in Medicine & Biology. 2020 Jul 1;46(7):1584-98.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 2.13 2.14 Board TN, Hughes SJ, Freemont AJ. Trochanteric bursitis: the last great misnomer. Hip international. 2014 Nov;24(6):610-5.
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 3.7 3.8 Lange J, Tvedesøe C, Lund B, Bohn MB. Low prevalence of trochanteric bursitis in patients with refractory lateral hip pain. Danish medical journal. 2022 Jun 15;69(7):A09210714.
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 4.6 Reid D. The management of greater trochanteric pain syndrome: a systematic literature review. Journal of Orthopaedics. 2016 Mar 1;13(1):15-28.
- ↑ Long SS, Surrey DE, Nazarian LN. Sonography of greater trochanteric pain syndrome and the rarity of primary bursitis. American Journal of Roentgenology. 2013 Nov;201(5):1083-6.
- ↑ 6.0 6.1 6.2 Koulischer S, Callewier A, Zorman D. Management of greater trochanteric pain syndrome: a systematic review. Acta Orthop Belg. 2017 Jun 1;83(2):205-14.
- ↑ 7.0 7.1 7.2 7.3 7.4 Speers CJ, Bhogal GS. Greater trochanteric pain syndrome: a review of diagnosis and management in general practice. British Journal of General Practice. 2017 Oct 1;67(663):479-80.
- ↑ 8.00 8.01 8.02 8.03 8.04 8.05 8.06 8.07 8.08 8.09 8.10 8.11 8.12 8.13 8.14 8.15 8.16 8.17 8.18 8.19 8.20 8.21 8.22 8.23 8.24 8.25 8.26 Lin CY, Fredericson M. Greater trochanteric pain syndrome: an update on diagnosis and management. Current Physical Medicine and Rehabilitation Reports. 2015 Mar;3(1):60-6.
- ↑ 9.0 9.1 9.2 9.3 Khoury AN, Brooke K, Helal A, Bishop B, Erickson L, Palmer IJ, et al. Proximal iliotibial band thickness as a cause for recalcitrant greater trochanteric pain syndrome. Journal of Hip Preservation Surgery. 2018 Aug;5(3):296-300.
- ↑ 10.00 10.01 10.02 10.03 10.04 10.05 10.06 10.07 10.08 10.09 10.10 10.11 10.12 10.13 10.14 10.15 10.16 10.17 10.18 10.19 10.20 10.21 10.22 Truong J, Mabrouk A, Ashurst JV. Septic Bursitis. InStatPearls [Internet] 2021 Sep 14. StatPearls Publishing.
- ↑ Suh JY, Park SY, Koh SH, Lee IJ, Lee K. Unusual, but important, peri-and extra-articular manifestations of rheumatoid arthritis: a pictorial essay. Ultrasonography. 2021 Oct;40(4):602.
- ↑ 12.0 12.1 Ivanoski S, Nikodinovska VV. Sonographic assessment of the anatomy and common pathologies of clinically important bursae. Journal of Ultrasonography. 2019 Jan 1;19(78):212-21.
- ↑ 13.0 13.1 13.2 Grimaldi A, Mellor R, Hodges P, Bennell K, Wajswelner H, Vicenzino B. Gluteal tendinopathy: a review of mechanisms, assessment and management. Sports Medicine. 2015 Aug;45(8):1107-19.
- ↑ 14.0 14.1 Pascual-Garrido C, Schwabe MT, Chahla J, Haneda M. Surgical treatment of gluteus medius tears augmented with allograft human dermis. Arthroscopy techniques. 2019 Nov 1;8(11):e1379-87.
- ↑ Bird PA, Oakley SP, Shnier R, Kirkham BW. Prospective evaluation of magnetic resonance imaging and physical examination findings in patients with greater trochanteric pain syndrome. Arthritis & Rheumatism: Official Journal of the American College of Rheumatology. 2001 Sep;44(9):2138-45.
- ↑ 16.0 16.1 Vlaic J, Pavic I, Batos AT, Zmak L, Kruslin B. Neglected tuberculous trochanteric bursitis in an adolescent girl: A case report and literature review. Joint diseases and related surgery. 2021 Aug;32(2):536.
- ↑ 17.00 17.01 17.02 17.03 17.04 17.05 17.06 17.07 17.08 17.09 17.10 17.11 17.12 17.13 17.14 17.15 17.16 17.17 Grimaldi A, Fearon A. Gluteal tendinopathy: integrating pathomechanics and clinical features in its management. journal of orthopaedic & sports physical therapy. 2015 Nov;45(11):910-22.
- ↑ Fearon AM, Ganderton C, Scarvell JM, Smith PN, Neeman T, Nash C, et al. Development and validation of a VISA tendinopathy questionnaire for greater trochanteric pain syndrome, the VISA-G. Manual therapy. 2015 Dec 1;20(6):805-13.
- ↑ Zero To Finals. Understanding Trochanteric Bursitis. Available from: http://www.youtube.com/watch?v=Ue9EL8C4R5Y [last accessed 20/01/2024]
- ↑ HT Physio - Over-Fities- Specialist Physio. 5 Best Exercises to FIX Hip Bursitis (Pain on Outside of Hip). Available from: http://www.youtube.com/watch?v=lRTEnTT4vlY [last accessed 20/01/2024]
- ↑ Jacobson JA, Yablon CM, Henning PT, Kazmers IS, Urquhart A, Hallstrom B, et al. Greater trochanteric pain syndrome: percutaneous tendon fenestration versus platelet‐rich plasma injection for the treatment of gluteal Tendinosis. Journal of Ultrasound in Medicine, 2016; 35(11):2413-2420.
- ↑ Ali M, Oderuth E, Atchia I, Malviya A. The use of platelet-rich plasma in the treatment of greater trochanteric pain syndrome: a systematic literature review. Journal of Hip Preservation Surgery. 2018 Aug;5(3):209-19.
- ↑ 23.0 23.1 Ramos-Pascua LR, Carro-Fernández JA, Santos-Sánchez JA, Ramos PC, Díez-Romero LJ, Izquierdo-García FM. Bursectomy, curettage, and chemotherapy in tuberculous trochanteric bursitis. Clinics in Orthopedic Surgery. 2016 Mar 1;8(1):106-9.
- ↑ Wiese M, Rubenthaler F, Willburger RE, Fennes S, Haaker R. Early results of endoscopic trochanter bursectomy. International orthopaedics. 2004 Aug;28(4):218-21.
- ↑ Fox JL. The role of arthroscopic bursectomy in the treatment of trochanteric bursitis. Arthroscopy: The Journal of Arthroscopic & Related Surgery. 2002;18(7):1-4.
- ↑ 26.0 26.1 Mitchell JJ, Chahla J, Vap AR, Menge TJ, Soares E, Frank JM, et al. Endoscopic trochanteric bursectomy and iliotibial band release for persistent trochanteric bursitis. Arthroscopy Techniques. 2016;5(5):e1185-9.
- ↑ 27.0 27.1 Ebert JR, Bucher TA, Mullan CJ, Janes GC. Clinical and functional outcomes after augmented hip abductor tendon repair. Hip International. 2018 Jan;28(1):74-83.
- ↑ Ebert JR, Brogan K, Janes GC. A prospective 2-year clinical evaluation of augmented hip abductor tendon repair. Orthopaedic Journal of Sports Medicine. 2020 Jan 22;8(1):2325967119897881.