Slipping Rib Syndrome
Original Editor - Jeroen Verwichte
Top Contributors - Tessa de Jongh, Laura Van Der Perren, Areeba Raja, Ine Wittevrongel, Kim Jackson, Gwen Wyns, Jeroen Verwichte, Lucinda hampton, Evan Thomas, Anouk Van den Bossche, Joao Costa, Claire Knott and Khloud Shreif
Introduction[edit | edit source]
Slipping rib syndrome (SRS) is characterized by pain in the lower chest or upper abdominal region caused by intercostal nerve impingement as a result of abnormal movement of false ribs (8-12) related to unstable costal cartilaginous attachments[1][2][3]
Slipping rib syndrome goes by many names, including:
- Clicking rib
- Displaced ribs
- Rib tip syndrome
- Costal margin syndrome
- Floating rib syndrome
- Nerve nipping
- Painful rib syndrome
- Slipping-rib-cartilage syndrome
- Gliding ribs
- Traumatic intercostal neuritis
- Twelfth rib syndrome
- Cyriax syndrome
- Interchondral subluxation, among others.[1][4][5]
Epidemiology[edit | edit source]
Slipping rib syndrome is a rare condition that affects both men and women of all ages. A review of slipping rib syndrome by Gress et al states that the available evidence relating to the epidemiology is often conflicting and anecdotal.[6]
- It is considered to be a rare syndrome and accounts for approximately five percent of all musculoskeletal chest pain in primary care. [1][7]
- May occur at any age, more common in middle-aged women, and is a relatively uncommon, but recognized cause of recurrent lower chest and/or upper abdomen pain in adolescents. [8][9][10]
- It’s been reported in people as young as 7 years and as old as 86, but it mostly affects middle-aged people.[1][4]
Clinically Relevant Anatomy[edit | edit source]
The slipping rib syndrome is a condition affecting the false ribs.
There are 3 types of ribs:
- Ribs which are attached to the sternum by costosternal joints and ligaments (true ribs - 1-7th)
- Ribs which are connected to each other through a weaker cartilaginous or fibrous band (false ribs – 8-10th)
- Ribs which aren’t attached to the sternum or to each other (floating ribs – 11-12th)
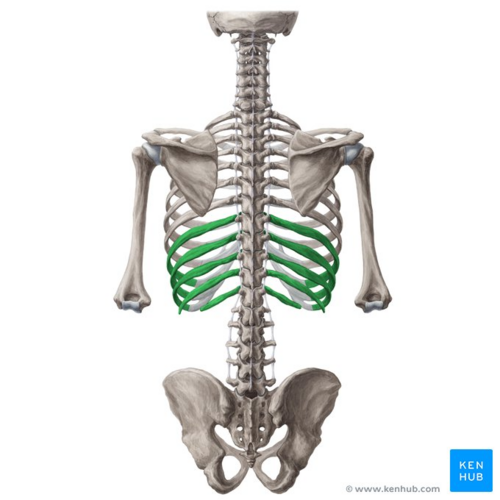
The condition arises from hypermobility of the anterior ends of the false rib costal cartilages, which often leads to slipping of the affected rib under the superior adjacent rib. This slippage or movement can lead to an irritation of the intercostal nerve, strain of the intercostal muscles, sprain of the lower costal cartilage, or general inflammation in the affected area. Because of their weak connection, there is increased mobility and greater susceptibility to trauma [11][12]. Anterior rib hypermobility is also likely to cause problems in the posterior thoracic area, because it’s a closed system [11].
Image: False ribs (highlighted in green) - posterior view [13]
Pathophysiology[edit | edit source]
Subluxation of the rib tips caused by disrupted articulation causes ends of ribs to curl up inside and impinge on the intercostal nerves. The impingement causes the pain as the result of repeated irritation of the intercostal nerves.[7][14][15] [16][17]
Etiology[edit | edit source]
It can be caused by:
- Congenital anomaly of the chest wall[14]
- The destruction of the fibrous articulation of the rib or their cartilage portion[14]
- Hypermobility of the costal cartilages of the false ribs[4][7]
Risk Factors[edit | edit source]
Following factors can contribute to the risk of developing SRS[4]
- overuse
- direct trauma that causes the pain.
- Sudden extension or flexion, repeated one-sided weight bearing or exercise such as throwing a ball, vigorous swimming, or swinging a bat.
Clinical Presentation[edit | edit source]
Slipping rib syndrome is presented through the following characteristics [11][15][18][19]
- Intense pain in the lower chest or upper abdomen above the costal margin, mostly at the height of the 8th, 9th and 10th ribs (false ribs).
- A tender spot on the costal margin
- Reproduction of the pain by pressing the tender spot or by external influences
- Signs and symptoms are usually unilateral, however there are also cases where patients reported bilateral pain.
Signs and Symptoms[edit | edit source]
Following signs and symptoms can be observed:[4][14][8][11][17][18][20][21][22][23][24][25][26][27][28][29][30][31][32][33][34][35][36][37][38][39]
- Upper abdominal and lower anterior chest wall pain.
- Flank pain
- Tenderness over the affected costal margins
- Clicking, popping or slipping sensation can also be present.
- Pain was preceded by certain activities such as sitting, leaning forward, and interestingly she found that using a swing machine was especially likely to produce discomfort.
- Pain associated with slipping rib syndrome has distinct characteristics which can be used in identifying the syndrome:
- Intermittent sharp stabbing pain followed by a constant monotonous pain that may last from several hours to many weeks.
- Range of severity of pain varies from being a minor nuisance, moderately severe to interfering with activities of daily living.
- May also be reported to radiate from the costochondral area to the chest or to the same level in the back .
- Exacerbated by certain postures and movements: lying or turning in bed, rising from a chair, driving, stretching, reaching, lifting, bending, twisting the trunk, coughing, walking, or bearing loads.
- May affect sporting activities involving trunk movements and deep breathing, but in particular running, horseback riding, arm abduction, or swimming. Pain may be severe enough to make patients stop playing sports.
- Visceral innervation converges at the same spinal cord levels as slipping ribs and intercostal nerves and this close association of the intercostal nerves and the sympathetic system may also cause a variety of somatic and visceral complaints, such as biliary or renal colic.
Physical Examination[edit | edit source]
The physiotherapist looks for an association between certain movements or postures and pain intensity (signs and symptoms), determines if the patient has experienced recent trauma (not always present), constrained posture, or previous abdominal surgery and reproduces the symptoms (eg, pain, clicking) [11][40][41][42]
- Palpation - At physical examination, the most common finding in a case of slipping rib syndrome is the tenderness above the costal margin. The physiotherapist can reproduce chest pain by palpation.
- A painful click is sometimes felt over the tip of the involved costal cartilage with certain movements.
- The Hooking manoeuvre - positive test.[18][19][24][43]
Diagnostic Procedures[edit | edit source]
Diagnosing SRS is the main challenge, which is based on the careful patient history, physical examination, and knowledge of its existence. [16] [44] However, following procedures can be use for diagnosis:[4][11][16][17][31][42][45][46]
- Hooking maneuvre: Reproduce the symptoms. This is a relatively simple clinical test where the clinician places his or her fingers under the lower costal margin and pulls the hand in an anterior direction. Pain or clicking indicates a positive test
- Intercostal nerve blocks can be performed after positive hooking manoeuvre, to confirm the diagnosis.
- Dynamic ultrasound of the ribs can be performed with valsalva, coughing, twisting, crunch and push manoeuvres to diagnose SRS.
Outcome Measures[edit | edit source]
- The physiotherapist can reproduce chest pain by palpation of the ribs and chest wall [11].
- Hooking manoeuvre[11][19][28][41]
- Patient-specific functional scale ( PSFS)[47].
- The Global rating of change (GROC) - To measure the patient’s subjective rate of improvement, the GROC has been stated to be reliable [48].
Differential Diagnosis[edit | edit source]
The differential diagnosis of slipping rib syndrome includes a variety of conditions[1][16][17][35][37]
- Cholecystitis
- Esophagitis
- Gastric ulcers
- Stress fractures
- Muscle tears
- Pleuritic chest pain
- Bronchitis
- Asthma
- Costochondritis, or Tietze syndrome
- Appendicitis
- Heart conditions
- Bone metastases
- Hepatosplenic issues
- Peptic ulcer
- Renal colic
- Pancreatitis
Management[edit | edit source]
In some cases, slipping rib syndrome resolves on its own without treatment if not, the choice of treatment depends on the severity of patient’s symptoms. There are different approaches in Conservative and non-conservative management that can be taken into account when treating SRS.[1][49][50][51]
Non-conservative Management[edit | edit source]
If the condition persists or causes severe pain, surgery may be recommended. Following surgical procedures can be done [1][2][16][17][35][44][52]
- Partial rib resection can be done to alleviate the symptoms. Following video demonstrates the surgical procedure:
- Minimally Invasive Repair of Adult Slipped Rib Syndrome Without Costal Cartilage Excision .
- Vertical rib plating with bioabsorbable plates significantly decreased the rate of recurrence in our early experience.
Conservative Management[edit | edit source]
Conservative management includes the following:[4][50]
- Rest.
- Avoiding strenuous activities.
- Applying heat or ice to the affected area.
- Oral medications like NSAIDS.
- Topical analgesics.
- Physical Therapy.
- Nerve blocks.
Activities to Avoid[edit | edit source]
Reassurance of the benign nature of the disease combined with explanation and advice concerning postural avoidance[42] [54]Following activities should be avoided:[55]
- Heavy lifting.
- Twisting.
- Pushing.
- Pulling.
Oral Medications[edit | edit source]
- Acetaminophen (Tylenol)[1]
- Nonsteroidal anti-inflammatory drug (NSAID)[35][50], such as ibuprofen (Advil, Motrin IB) or naproxen (Aleve)[1]
Intercostal Nerve Blocks[edit | edit source]
If the pain continues despite taking a painkiller following can be done to elicit the symptoms:[1][4][30][35][56]
- A corticosteroid injection to help reduce the swelling
- An intercostal nerve block (an injection of an anesthetic in the intercostal nerve) to relieve pain
Physical Therapy Management[edit | edit source]
- Manual therapy: manipulation of the costovertebral joint and electric stimulation can help manage the pain, but probably no long term relief [11].
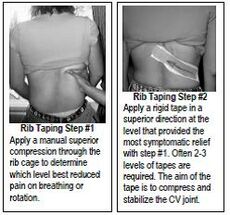
- Taping of ribs can possibly provide some temporary relief. To decide on the location and direction of taping, apply a manual superior compression force through the postero-lateral aspect of the rib cage. Now ask the patient to take in a deep breath or rotate. If the patient notes a significant improvement in symptoms, then apply the tape at that level [57].
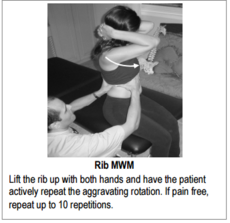
- Rib mobilization with movement (MWM) as proposed by Brian Mulligan. The range of motion and pain level are evaluated. A cranial glide is applied over the lateral as3pect of the rib above the painful region. While sustaining this rib elevation (unloading), the patient is asked to rotate again while ROM and pain are once again evaluated. If there is no change, the technique is repeated on a rib above or below. If MWM on a rib at a specific level is found to reduce or eliminate the pain, it is repeated 10 times [57].
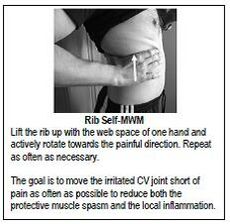
- A home program of self MWM may be provided. Instruction: “lift the rib up with the web space of one hand and actively rotate towards the painful direction, repeat as often as necessary”. The goal is to move the irritated costovertebral joint without pain as often as possible to reduce both the protective muscle spasm and the local inflammation [57]
Clinical Bottom Line[edit | edit source]
- The Slipping rib syndrome is an often under diagnosed disease for which sometimes comprehensive diagnostic evaluation is performed.
- Knowledge of the slipping rib syndrome can lead to quick and simple diagnosis and prevent months or years of chronic complaints.
- The impingement can cause severe constant pain and a slipping sensation provoked by several movements.
- It can also lead to an irritation of the intercostal nerve or problems to structures in that area.
- Knowledge of the syndrome is important; it can lead to quick and simple diagnosis.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 1.7 1.8 1.9 Healthline Slipping Rib Syndrome Available from:https://www.healthline.com/health/slipping-rib-syndrome#symptoms (last accessed 6.5.2020)
- ↑ 2.0 2.1 Panka CT, Tchebegna PY. Cyriax syndrome in a young male professional soccer player: A case report. South African Journal of Sports Medicine. 2020;32(1):1-2.
- ↑ Holmes JF. Slipping rib cartilage: with report of cases. The American Journal of Surgery. 1941 Oct 1;54(1):326-38.
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 4.6 4.7 McMahon LE. Slipping rib syndrome: a review of evaluation, diagnosis and treatment. InSeminars in Pediatric Surgery 2018 Jun 1 (Vol. 27, No. 3, pp. 183-188). WB Saunders.
- ↑ Patel N, John JK, Pakeerappa P, Aiyer R, Zador LN. Slipping rib syndrome: case report of an iatrogenic result following video-assisted thoracic surgery and chest tube placement. Pain Management. 2021 May;11(5):555-9.
- ↑ Gress K, Charipova K, Kassem H, Berger AA, Cornett EM, Hasoon J, Schwartz R, Kaye AD, Viswanath O, Urits I. A Comprehensive Review of Slipping Rib Syndrome: Treatment and Management. Psychopharmacology Bulletin. 2020 Oct 15;50(4 Suppl 1):189.
- ↑ 7.0 7.1 7.2 Gress K, Charipova K, Kassem H, Berger AA, Cornett EM, Hasoon J, Schwartz R, Kaye AD, Viswanath O, Urits I. A Comprehensive Review of Slipping Rib Syndrome: Treatment and Management. Psychopharmacology bulletin. 2020 Oct 15;50(4 Suppl 1):189.
- ↑ 8.0 8.1 Porter GE. Slipping rib syndrome: an infrequently recognized entity in children: a report of three cases and review of the literature. Pediatrics. 1985 Nov;76(5):810-3.
- ↑ Lum-Hee N, Abdulla AJ. Slipping rib syndrome: an overlooked cause of chest and abdominal pain. International journal of clinical practice. 1997 Jun 1;51(4):252-3.
- ↑ Turcios NL. Slipping rib syndrome in an adolescent: an elusive diagnosis. Clinical Pediatrics. 2013 Sep;52(9):879-81.
- ↑ 11.0 11.1 11.2 11.3 11.4 11.5 11.6 11.7 11.8 Udermann B.E. et al.; Slipping Rib Syndrome in a Collegiate Swimmer: A Case Report; J Athl Train, 2005 (LoE 3B)
- ↑ McBeath A.A. et al.; The rib-tip syndrome; J. Bone Joint Surg. Am., 57 (1975), pp. 795–797 (LoE 3A)
- ↑ False ribs (highlighted in green) - posterior view image - © Kenhub https://www.kenhub.com/en/library/anatomy/the-ribs
- ↑ 14.0 14.1 14.2 14.3 Romano R, Gavezzoli D, Gallazzi MS, Benvenuti MR. A new sign of the slipping rib syndrome?. Interactive CardioVascular and Thoracic Surgery. 2022 Feb;34(2):331-2.
- ↑ 15.0 15.1 SANGHANI RR, ZESTOS MM, THOMAS ST. A CAse RepoRt of slipping Rib syndRome: An UnCommon And UndeRdiAgnosed CAUse of AbdominAl pAin.
- ↑ 16.0 16.1 16.2 16.3 16.4 Hussain A. Diagnosing and treating Slipping Rib Syndrome: An unusual case of undiagnosed pain for 5 years. COPD. 2020.
- ↑ 17.0 17.1 17.2 17.3 17.4 Fu R, Iqbal CW, Jaroszewski DE, Peter SD. Costal cartilage excision for the treatment of pediatric slipping rib syndrome. Journal of pediatric surgery. 2012 Oct 1;47(10):1825-7.
- ↑ 18.0 18.1 18.2 Scott EM, Scott BB. Painful rib syndrome--a review of 76 cases. Gut. 1993 Jul 1;34(7):1006-8.
- ↑ 19.0 19.1 19.2 Keoghane SR, Douglas J, Pounder D. Twelfth rib syndrome: a forgotten cause of flank pain. BJU international. 2009 Mar;103(5):569-70.
- ↑ Cranfield KA, Buist RJ, Nandi PR, Baranowski AP. The twelfth rib syndrome. Journal of pain and symptom management. 1997 Mar 1;13(3):172-5.
- ↑ Mooney DP, Shorter NA. Slipping rib syndrome in childhood. Journal of pediatric surgery. 1997 Jul 1;32(7):1081-2.
- ↑ Arroyo JF, Vine R. Slipping rib syndrome: don't be fooled. Geriatrics. 1995;50(3):46-9.
- ↑ Copeland GP, Machin DG, Shennan JM. Surgical treatment of the ‘slipping rib syndrome’. British journal of surgery. 1984 Jul;71(7):522-3.
- ↑ 24.0 24.1 Saltzman DA, Schmitz ML, Smith SD, Wagner CW, Jackson RJ, Harp S. The slipping rib syndrome in children. Pediatric Anesthesia. 2001 Nov 9;11(6):740-3.
- ↑ Machin DG, Shennan JM. Twelfth rib syndrome: a differential diagnosis of loin pain. British Medical Journal (Clinical research ed.). 1983 Aug 27;287(6392):586.
- ↑ Van Delft EA, Van Pul KM, Bloemers FW. The slipping rib syndrome: a case report. International Journal of Surgery Case Reports. 2016 Jan 1;23:23-4.
- ↑ Mynors J.M. et al.; Clicking rib; Lancet, 1 (1973), p. 674 (LoE 1B)
- ↑ 28.0 28.1 Bass J. et al.; Slipping Rib Syndrome; Journal of the National Medical Association, 1979;71(9):863-865. (LoE 4)
- ↑ Cyriax E, et al., On various conditions that may simulate the referred pains of visceral disease and a consideration of these from the point of view of cause and effect, Practitioner, 1919
- ↑ 30.0 30.1 Germanovich A;Ferrante FM. “Multi-Modal Treatment Approach to Painful Rib Syndrome: Case Series and Review of the Literature.” Pain Physician, vol. 19, no. 3, 2016,
- ↑ 31.0 31.1 Kumar R, Ganghi R, Rana V, Bose M. The painful rib syndrome. Indian Journal of Anaesthesia. 2013 May;57(3):311.
- ↑ Davies-Colley R. Slipping rib. British Medical Journal. 1922 Mar 18;1(3194):432.
- ↑ Arya S, Verma AK, Gupta BK, Hifzur M, Gupta S, Singh N. Twelfth rib syndrome-an often missed differential diagnosis of hypogastric and lumbar pain: case series. Int J Reprod Contracept Obstet Gynecol. 2014 Mar 1;3:263-5.
- ↑ Mazzella A, Fournel L, Bobbio A, Janet-Vendroux A, Lococo F, Hamelin EC, Icard P, Alifano M. Costal cartilage resection for the treatment of slipping rib syndrome (Cyriax syndrome) in adults. Journal of Thoracic Disease. 2020 Jan;12(1):10.
- ↑ 35.0 35.1 35.2 35.3 35.4 Kamal YA. Slipping rib syndrome: A neglected cause of hypochondrial pain. Formosan Journal of Surgery. 2019 Nov 1;52(6):229.
- ↑ Migliore M, Signorelli M, Caltabiano R, Aguglia E. Flank pain caused by slipping rib syndrome. The Lancet. 2014 Mar 1;383(9919):844.
- ↑ 37.0 37.1 Turcios NL. Slipping rib syndrome: an elusive diagnosis. Paediatric Respiratory Reviews. 2017 Mar 1;22:44-6.
- ↑ Hughes KH. Painful rib syndrome: a variant of myofascial pain syndrome. AAOHN Journal. 1998 Mar;46(3):115-20.
- ↑ Bong J, Healey D. Slipping rib syndrome. Journal of Medical Imaging and Radiation Oncology. 2021 May 30.
- ↑ Meuwly JY, Wicky S, Schnyder P, Lepori D. Slipping rib syndrome: a place for sonography in the diagnosis of a frequently overlooked cause of abdominal or low thoracic pain. Journal of ultrasound in medicine. 2002 Mar;21(3):339-43.
- ↑ 41.0 41.1 Fam AG, Smythe HA. Musculoskeletal chest wall pain. CMAJ: Canadian Medical Association Journal. 1985 Sep 1;133(5):379.
- ↑ 42.0 42.1 42.2 Khan NA, Waseem S, Ullah S, Mehmood H. Slipping rib syndrome in a female adult with longstanding intractable upper abdominal pain. Case Reports in Medicine. 2018 Jul 2;2018.
- ↑ Ronga A, Vaucher P, Haasenritter J, Donner-Banzhoff N, Bösner S, Verdon F, Bischoff T, Burnand B, Favrat B, Herzig L. Development and validation of a clinical prediction rule for chest wall syndrome in primary care. BMC family practice. 2012 Dec;13(1):1-9.
- ↑ 44.0 44.1 Hansen AJ, Toker A, Hayanga J, Buenaventura P, Spear C, Abbas G. Minimally Invasive Repair of Adult Slipped Rib Syndrome Without Costal Cartilage Excision. The Annals of thoracic surgery. 2020 Sep 1;110(3):1030-5.
- ↑ Foley CM, Sugimoto D, Mooney DP, Meehan III WP, Stracciolini A. Diagnosis and treatment of slipping rib syndrome. Clinical Journal of Sport Medicine. 2019 Jan 1;29(1):18-23.
- ↑ Van Tassel D, McMahon LE, Riemann M, Wong K, Barnes CE. Dynamic ultrasound in the evaluation of patients with suspected slipping rib syndrome. Skeletal Radiology. 2019 May;48(5):741-51.
- ↑ Westrick RB, Zylstra E, Issa T, Miller JM, Gerber JP. Evaluation and treatment of musculoskeletal chest wall pain in a military athlete. International Journal of Sports Physical Therapy. 2012 Jun;7(3):323.
- ↑ Proulx AM, Zryd TW. Costochondritis: diagnosis and treatment. American family physician. 2009 Sep 15;80(6):617-20.
- ↑ Telford KM. Slipping rib syndrome. Canadian Medical Association Journal. 1950 May;62(5):463.
- ↑ 50.0 50.1 50.2 Davelaar CM. A Clinical Review of Slipping Rib Syndrome. Current Sports Medicine Reports. 2021 Mar 1;20(3):164-8.
- ↑ Fares MY, Dimassi Z, Baydoun H, Musharrafieh U. Slipping rib syndrome: solving the mystery of the shooting pain. The American journal of the medical sciences. 2019 Feb 1;357(2):168-73.
- ↑ McMahon LE, Salevitz NA, Notrica DM. Vertical rib plating for the treatment of slipping rib syndrome. Journal of Pediatric Surgery. 2021 Oct 1;56(10):1852-6.
- ↑ reference
- ↑ Gregory PL, Biswas AC, Batt ME. Musculoskeletal problems of the chest wall in athletes. Sports Medicine. 2002 Apr;32(4):235-50.
- ↑ “Slipping Rib Syndrome.” Ucsfhealth.org, 25 Mar. 2020,
- ↑ Ayloo A, Cvengros T, Marella S. Evaluation and treatment of musculoskeletal chest pain. Primary Care: Clinics in Office Practice. 2013 Dec 1;40(4):863-87.
- ↑ 57.0 57.1 57.2 Bahram J. et al.; Ribs don’t sublux, ribs don’t “go out” … so what’s going on?; Advanced Physical Therapy Education Institute, 2015 (LoE: 4)
- ↑ Rib MWM. [Accessed 16 May 2020]