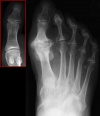
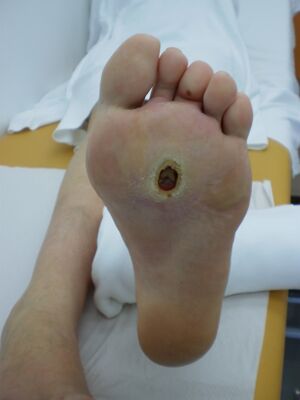
The Aged Foot
Original Editors - Scott Buxton
Top Contributors - Scott Buxton, Lucinda hampton, Kim Jackson, 127.0.0.1, Lauren Lopez and Khloud Shreif
Introduction[edit | edit source]
Foot problems are common place in people over the age of 75[1]. Foot impairment contributes to falls, immobility, the progression of frailty and can lead to a quicker progression towards dependence and not independence[2].
The average moderately active person take around 7,500 step/day. If you maintain that daily average and live until 80 years of age, you'll have walked about 216,262,500 steps in your lifetime. Thos works out that the average person (with average stride) living until 80 will walk a distance of around 177,028 km or 110,000 miles.[3]
The management of the aged foot is typically aimed at achieving comfort through the reduction of pain as well as increasing mobility. Both ultimately preventing dependence and reduce the need and demand for other services. Thankfully most common issues can be treated successfully by Podiatrists as well as Physiotherapists. The aim of this article is highlight the common issues as well as basic methods of management.
Epidemiology[edit | edit source]
It is estimated that around 80% of older people have foot problems however many of these people do not seek medical attention[4][5]. Multiple studies in many countries have found the same, older people do not seek help for foot problems even when something can be done about it[6].
The most common foot problems tend to be nail problems, calluses, bunions, corns, hallux valgus, generalised pain, swollen feet and circulatory problems[7]. Most of these issues derive from poorly fitting shoes, obesity and chonic conditions such as diabetes, cardiovascular disease or osteoporosis[8].
Common Problems[edit | edit source]
The problems listed below are not all physiotherapy ameanable however it is important that physiotherapists are aware of them and how they can affect an older person. In particular all of these issues can contribute to a multifactorial picture of falls.
Toenail Issues[edit | edit source]
Toenail issues arise because of many issues but the largest contributor is likely the fact that cutting is difficult. See Toenail Issues in Older Persons
Bunion[edit | edit source]
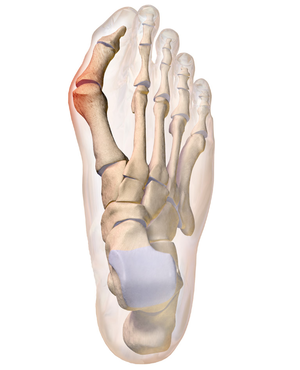
Foot width and length often increases with age in addition to peripheral swelling which often occurs throughout the day[9]. This change in shape can lead to misshapen joints resulting in pressure changes in the skin leading to bunions. A bunion is a bony deformity of the joint at the base of the big toe. The main sign is the big toe pointing towards the other toes on the same foot causing a swollen bumpy lump on the medial aspect of the foot. This causes a painful callus to form which could potentially develop into a sore[10].
Symptoms include: a swollen, bony bump on the outside edge of your foot; pain and swelling over your big toe joint that's made worse by pressure from wearing shoes; hard, callused and red skin caused by your big toe and second toe overlapping; sore skin over the top of the bunion.
Hallux Valgus[edit | edit source]
Hallux Valgus is the most common foot deformity. It is a progressive foot deformity in which the first metatarsophalangeal (MTP) joint is affected and is often accompanied by significant functional disability and foot pain and reduced quality of life.[11][12]
Corn / Callus[edit | edit source]
As well as being caused by bunions ill-fitting shoes and the deterioration of fat pads can lead to pressure areas. This is called a corn or callus. They are circular masses of tissue which form on the outside of the toes, usually the outer ones, which is painful on direct pressure. They are usually caused by ill-fitting shoes and deterioration of fats pads.
Ankle Osteoarthritis[edit | edit source]
Ankle OA: Compared with knee and hip, there is a substantially lower rate of primary ankle OA.
Gout[edit | edit source]
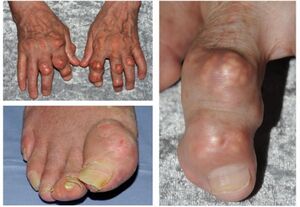
Gout is a crystal-induced arthritis, in which monosodium urate (MSU) crystals precipitate within joints and soft tissues and elicit a highly inflammatory but localized response. Gout is often described as a burning pain and can be extremely severe in nature with an attack lasting upwards of a week. During this period of immobility an elderly person can lose a significant amount of independence and may require help to function.
In many frail elderly people gout can often be interpreted as something more severe such as a fracture or infective arthritis. This is because a flare of a disorder can knock those who have 'just about been coping' with all of their other morbidity over the edge. With their body now unable to cope with a new complaint they often become immobile and unable to function as before.
Hallux Rigidus[edit | edit source]
Hallux Rigidus is a progressive disorder. The toe’s motion is decreased over time. Some causes are faulty function or biomechanics and structural abnormalities which can lead to OA.
Rheumatoid Arthritis[edit | edit source]
Rheumatoid arthritis (RA) is a systematic autoimmune inflammatory disease and results in persistent inflammation of synovial tissue especially of the wrists, hands and feet. Individuals with RA are 8 times more likely to have functional disability compared with adults in the general population from the same community.
Diabetic Foot Ulcers[edit | edit source]
15-20% of diabetics will develop a diabetic foot ulcer in their lifetime and effective monitoring is essential to prevent further issues developing alongside[13]. Up to 50% of patients with neuropathy never experience symptoms, so absence of neuropathic symptomatology must never be associated with absence of risk of foot ulceration.
Skin[edit | edit source]
As you age skin becomes thinner, loses fat, takes longer to heal and is more prone to damage.
Obesity[edit | edit source]
15% of men and 28% of women over 60 are obese and this has a significant effect on the biomechanics of the feet. Obese elderly tend to have a higher incidence of foot pain because of structural changes and this also has implications for day to day life, mobility and general well-being. They tend to have larger foot dimensions, thicker plantar fat pads under the heels, a lower hallux and overall foot strength. These contribute to generating a higher overall force, a greater plantar contact time with a greater contact area therefore greater pressure-time. Therefore providing interventions to combat their obesity ensures a reduction in foot pain, an increase in independence and better overall quality of life[14].
Management[edit | edit source]
It is important that with older people you remember to think about the person as a whole and in terms of their frailty and falls risk.
Prevention
- Regular Checks. Long-term conditions increase the likelihood of developing issues particularly those disorders which affect circulation. The signs of deterioration are subtle and therefore long-term vascular issues need to be monitored. It is essential that alongside regular check-ups those most vulnerable seek primary care advice as soon as any new issues arise such as blisters, cracks or obvious changes. Prevention is the best protection, you do this with your eyes, why is it different for your feet?
- Nails. As we age it is increasingly difficult to reach our toe nails but cutting them should not go to the wayside. Poorly looked after nails can become ingrown and infected resulting in pain and immobility. The nails get long, press against shoes, the pressure causes sores, the sores become infected and then ulcerated. You look after your fingernails, why not your toenails?
- Skin Quality. As we age our skin becomes dry, cracked, have a reduced circulation and a reduction in fat pad absorption. Once the dryness and cracked skin with sores sets in they are a rife place for infection. Cellulitis is common in elderly people and frequently reoccurs. You care about the skin on your face, why not your feet?
- Correct Footwear. Optimum alignment and weight distribution is essential to keep joints and soft tissues working effectively. A good pair of closed heel flat shoes with good shock absorption promotes good walking posture and balance whislt reducing any risk of chaffing or rubbing. Additionally they should be roomy enough to allow for minor swelling which occurs during the day. Why do you think runners spend so much on good quality running shoes?
Essential Care[edit | edit source]
Some basic essential care points can make all the different for elderly people[15].
- Ideally daily washing
- A good and thorough drying routine
- Avoiding talcum powder
- Fresh socks
- Moisturising the feet avoiding over apllication between the toes
- Routinely buying new footwear and minimal use of slipper
Ulcers[edit | edit source]
See the diabetic foot.
Gout[edit | edit source]
Aside from the management of hyperuricemia and the pharmocology-side of the treatment physiotherapy is important. Patient education, optimising mobility and lifestyle modification are essential parts of the holistic gout management plan.
It is important that the elderly person with gout remains as active as possible during the attack of symptoms as the rest of their muscular system will atrophy and it may be difficult to get the muscle bulk and function back afterwards. Seated or weightbearing exercise plans are a suitable options alongside provision of mobility aids. For those elderly able to attend outpatient clinics ultrasound therapy may also be an option. As gout is an inflammatory disorder don't forget the efficacy of ice.
It is also that the person avoids alcohol, highly calorific food, sea food in the long term and if applicable to them, optimisie their BMI. This will reduce the risk of ongoing flares[16].
Toenails[edit | edit source]
Owning individual nail clippers and files prevents corss contamination of infections along with regular washing and maintenance[9]. Toenail cutting services may be an alternative option to those unable to cut their own nails.
Overall it is not always the physiotherapists job to manage the nail conditions however, basic advice is always worth sharing with the patient. The main thing to be aware of is that elderly patients might complain of common nail changes and dystrophies that cause pain, affect daily activities, are of cosmetic concern. Awareness of these conditions is essential for onward referral to optimally manage the issues.
Skin[edit | edit source]
Keeping feet moisturised is an essential part of caring for aged skin which is prone to drying out.
Bunions[edit | edit source]
A bunion may only need treatment if it is severe and causing significant pain and alteration to daily life. Non-surgical options incluse pain killers, bunion pads and orthotics all alongside appropriate footwear. It is important to be aware that surgery is the only way to correct a bunion and is not for cosmetic reasons alone[17]. The surgical options include an osteotomy, which is removal of the problematic part of the bone alongside correction of any soft tissue deformity which has occurred. Arthrodesis is also an option. This is when the metatarsophalangeal joint is fused and is only recommended in severe joint degeneration.
References[edit | edit source]
- ↑ Clarke M. Trouble with feet. In: Clark M ed.fckLROccasional papers on Social Administration NofckLR29. London: Bell, 1969.
- ↑ Ebrahim SBJ, Sainsbury R, Watson S. FootfckLRproblems of the elderly: a hospital survey. BMJfckLR1981; 283: 949–50.
- ↑ SnowBrains. How Far Does the Average Human Walk in a Lifetime? [ONLINE] http://snowbrains.com/brain-post-how-far-does-the-average-human-walk-in-a-lifetime/ [Accessed 21/03/17 @19:20]
- ↑ Harvey I et al (1997) Foot morbidity and exposure to chiropody: population based study. The BMJ; 315: 7115, 1054-1055.
- ↑ Evans G. The Aged Foot. Reviews in Clinical Gerontology. 2002:12;175-180.
- ↑ BJ Munro and JR Steele (1998) Foot-care awareness. A survey of persons aged 65 years and older. Journal of the American Podiatric Medical Association: May 1998, Vol. 88, No. 5, pp. 242-248.
- ↑ NEW SOUTH WALES DEPARTMENT OF HEALTH PODIATRYfckLRSURVEY STEERING COMMITTEE: Podiatry Survey: SurveyfckLRof Foot Problems in Households and Health InstitutionsfckLRin NSW, State Health Publication No. (CDB) 91-fckLR31, Department of Health, Sydney, 1991
- ↑ Health in Aging. Foot Problems. [ONLINE] Accessed from http://www.healthinaging.org/aging-and-health-a-to-z/topic:foot-problems/ [23/03/2017]
- ↑ 9.0 9.1 Woodrow P et al (2005) Foot care for non-diabetic older people. Nursing Older People; 17: 8, 31-32.
- ↑ NHS Direct. Bunions. [ONLINE] Accessed from: http://www.nhs.uk/conditions/Bunion/Pages/Introduction.aspx [23/03/2017].
- ↑ González-Martín C, Alonso-Tajes F, Pérez-García S, Seoane-Pillado MT, Pértega-Díaz S, Couceiro-Sánchez E et al. Hallux valgus in a random population in Spain and its impact on quality of life and functionality. Rheumatol Int. 2017;37(11):1899-1907.
- ↑ Mortka K, Lisiński P. Hallux valgus—a case for a physiotherapist or only for a surgeon? Literature review. Journal of physical therapy science. 2015;27(10):3303-7.
- ↑ Frykberg RG et al (1998) Role of neuropathy and high foot pressures in diabetic foot ulceration. Diabetes Care; 21: 10, 1054-1055.
- ↑ Steele, J. Mickle, K. Munro, B. 2009. Fat flat frail feet: how does obesity affect the older foot. XXII Congress of the International Society of Biomechanics.
- ↑ Soliman A, Brogan M (2014) Foot assessment and care for older people. Nursing Times; 110: 50, 12-15.
- ↑ Chowalloor PV, Keen HI, Inderjeeth CA. Gout in the elderly. OA Elderly Medicine 2013 Aug 01;1(1):2.
- ↑ Bunion. NHS Choices. [ONLINE] http://www.nhs.uk/Conditions/Bunion/Pages/Treatment.aspx Accessed 29/03/2017.