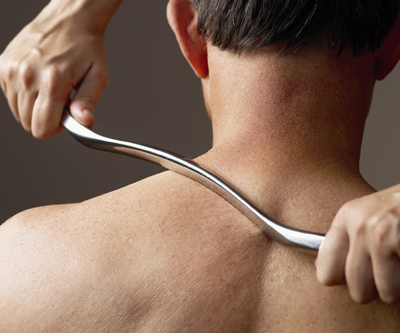
Instrument Assisted Soft Tissue Mobilization
Original Editor - Mohamed Kassim Abdul Wahab
Top Contributors - Mohamed Kassim Abdul Wahab, Fatemah Ali Fairouz, Lilian Ashraf, Admin, Kim Jackson, Aminat Abolade, WikiSysop, Claire Knott, Lucinda hampton, 127.0.0.1, Tony Lowe and Laura Ritchie
Introduction[edit | edit source]
Instrument assisted soft tissue mobilization (IASTM) is a skilled myofascial intervention used for soft-tissue treatment. It is based on the principles of James Cyriax cross-friction massage.[1]
It is applied using instruments that are usually made of stainless steel with bevelLed edges and contours that can conform to different body anatomical locations and allows for deeper penetration.[2] It is used for the detection and treatment of soft tissue disorders.[3]
A proposed description for IASTM is “a skilled intervention that includes the use of specialized tools to manipulate the skin, myofascia, muscles, and tendons by various direct compressive stroke techniques”. [1]
The technique itself is said to have evolved from Gua sha which is a method used in Chinese medicine.[4] Gua sha uses instruments with smoothed edges to scrape the skin till red blemishes occur. However, Gua sha has different rationale, goals and application method from IASTM.[1]
How does it work?[edit | edit source]
Instruments effectively break down fascial restrictions and scar tissue. The ergonomic design of these instruments provides the clinician with the ability to locate restrictions and allows the clinician to treat the affected area with the appropriate amount of pressure.
The introduction of controlled microtrauma to affected soft tissue structure causes the stimulation of local inflammatory response. Microtrauma initiates reabsorption of inappropriate fibrosis or excessive scar tissue and facilitates a cascade of healing activities resulting in remodelLing of affected soft tissue structures. Adhesions within the soft tissue which may have developed as a result of surgery, immobilization, repeated strain or other mechanisms, are broken down allowing full functional restoration to occur.[5][6][7]
Conditions For Which IASTM is Usually Used[edit | edit source]
- Medial Epicondylitis, Lateral Epicondylitis
- Carpal Tunnel Syndrome
- Neck Pain
- Plantar Fascitis
- Rotator Cuff Tendinitis
- Patellar Tendinitis
- Tibialis Posterior Tendinitis
- Heel Pain /Achilles Tendinitis
- DeQuervain's Syndrome
- Post-Surgical and Traumatic Scars
- Myofascial Pain and Restrictions
- Musculoskeletal Imbalances
- Chronic Joint Swelling Associated with Sprains/Strains
- Ligament Sprains
- Muscle Strains
- Non-Acute Bursitis
- RSD (Reflex Sympathetic Dystrophy)
- Back Pain
- Trigger Finger
- Hip Pain (Replacements)
- IT Band Syndrome
- Shin Splints
- Chronic Ankle Sprains
- Acute Ankle Sprains (Advanced Technique)
- Scars (Surgical, Traumatic)
Contraindications[edit | edit source]
- Open wound (unhealed suture site)
- Unhealed fracture
- Thrombophlebitis
- Uncontrolled hypertension
- Patient intolerance/hypersensitivity
- Hematoma
- Osteomyelitis
- Myositis ossificans
- Hemophilia [9]
Precautions[edit | edit source]
- Anti-coagulant medications
- Cancer
- Varicose veins
- Burn scars
- Acute inflammatory conditions
- Kidney dysfunction
- Inflammatory condition secondary to infection
- Rheumatoid arthritis
- Pregnancy [9]
IASTM Physiology & Benefits[edit | edit source]
Physiological Mechanism[edit | edit source]
Studies have addressed the benefits of IASTM at the cellular level. The inflammatory response initiated through micro trauma to the affected tissues results in increased fibroblast proliferation, collagen synthesis, maturation and the remodelling of unorganized collagen fibre matrix following IASTM application. Which result in a breakdown of scar tissues, adhesions and facial restrictions.[1][2]
Fibroblast is considered the most important cell in the extracellular matrix (ECM). The repair, regeneration and maintenance of soft tissue take place in the ECM. The fibroblast synthesizes the ECM, which includes collagen, elastin and proteoglycans, among many other essential substances. Fibroblasts have the ability to react as mechanotransducers, which means they are able to detect biophysical strain (deformation) such as compression, torque, shear and fluid flow, and create a mechanochemical response.
Gehlsen et al investigated the effects of 3 separate IASTM pressures on rat Achilles tendons.[10] They concluded that fibroblast production is directly proportional to the magnitude of IASTM pressure used by the clinician. Davidson et al supported Gehlsen et al. by concluding that IM significantly increased fibroblast production in rat Achilles tendons by using electron microscopy to analyze tissue samples following IM application.[11]
Davidson et al. found morphologic changes in the rough endoplasmic reticulum following IM application. Thus, indicating micro trauma to damaged tissues, resulting in an acute fibroblast response.[11]
IASTM have a neurophysiological effect as it stimulates mechanosensitive neurons through skin deformation by the instrument. Mechanosensitive neurons include mechanoreceptors which are responsible for two-point discrimination and mechano-nociceptors which are responsible for pain perception.
A study by Weiqing Ge, found the IASTM changed the neural activity of the large mechanoreceptor neurons affecting the two-point discrimination. Another study by Scott W. Cheatham et al, studies the effect of IASTM on DOMS (delayed onset muscle soreness) and the results found a decrease in the area of 2 point discrimination suggesting improved local tactile sense through mechanoreceptors stimulation and a decrease in the pain pressure threshold which suggest that light IASTM modulated the nociceptors ( small pain fibres) activity.[3][12]
IASTM affects the vascular response to the injured soft tissue, through increasing the blood flow. As evident by Loghmani et al, who studied the effect of IASTM on the knee MCL in rats, and found an increase in tissue perfusion and increase in the proportion of arteriole-sized blood vessels in the treated leg.[13]
Clinical Benefits[edit | edit source]
Studies have also showed clinical benefits of IASTM showing improvements in range of motion, strength and pain perception following treatment. Melham et al found that IASTM significantly improved range of motion in a college football player following 7 weeks of IASTM and physical therapy.[14] Melham et al. found that scar tissue surrounding the lateral malleolus was reduced and remodelled structurally following IASTM application. Wilson et al found improvement in pain reduction and impairment scale at 6 & 12 weeks following IASTM application for patellar tendonitis.[15]
Benefits to the Therapist[edit | edit source]
IASTM provide clinicians with a mechanical advantage, thus preventing over-use to the hands, it provides deeper tissue penetration with less compressive forces to the interphalangeal joints of the clinician’s hand.[2] Snodgrass SJ surveyed physical therapists and found that after spinal pain, the second most common cause for absenteeism from work was overuse of the thumb. Ninety-one percent of physiotherapists using some sort of massage had to modify their treatment techniques because of thumb pain.[16]
Also, it increases the vibratory perception of the physical therapist’s hand holding the instrument to altered soft tissue properties such as tissues restrictions or adhesions. So the therapist is able to detect soft tissue irregularities easier.[3]
Types of Tools[edit | edit source]
There are many companies for IASTM such as RockTape®, HawkGrips®, Graston®, Técnica Gavilán®, Functional and Kinetic Treatment with Rehab (FAKTR)®, Adhesion Breakers®, augmented soft-tissue mobilization or ASTYM®, and Fascial Abrasion Technique™. Each company has its own treatment approach with different instruments designs.[1]
IASTM can be made from varying materials including stainless steel, titanium, plastic, buffalo horn, stone, quartz, and jade. The most common IASTM instruments used are stainless steel.[2][1]
Practical Application [edit | edit source]
IASTM can’t be done by itself, it must be combined with motion and strengthening program to enhance the tissues remodelling.
When IASTM is applied to goes through 6 steps
- Examination
- Warm-up is done for 10-15 mins by light jogging, elliptical machine, stationary bike or an upper body ergometer
- IASTM, done at 30-60 degrees angle for 40-120 seconds
- Stretching, 3 reps for 30 seconds
- Strengthening, high repetitions with low load exercise
- Cryotherapy, 10-20 min[13]
It is important to disinfect the instrument between patients to avoid transfer of infections. It is recommended to disinfect the instrument with intermediate-level disinfectants (e.g. isopropyl alcohol), then wash it with soap and water to remove any residuals of the chemical disinfectant off the instrument. If the tools contacts blood, bodily fluids, mucous membranes, or non-intact skin then disinfecting it with high-level disinfectant should be done.[1]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 Cheatham SW, Baker R, Kreiswirth E. Instrument assisted soft-tissue mobilization: A commentary on clinical practice guidelines for rehabilitation professionals. International journal of sports physical therapy. 2019 Jul;14(4):670.
- ↑ 2.0 2.1 2.2 2.3 Lambert M, Hitchcock R, Lavallee K, Hayford E, Morazzini R, Wallace A, Conroy D, Cleland J. The effects of instrument-assisted soft tissue mobilization compared to other interventions on pain and function: a systematic review. Physical Therapy Reviews. 2017 Mar 4;22(1-2):76-85.
- ↑ 3.0 3.1 3.2 Ge W, Roth E, Sansone A. A quasi-experimental study on the effects of instrument assisted soft tissue mobilization on mechanosensitive neurons. Journal of physical therapy science. 2017;29(4):654-7.
- ↑ Nazari G, Bobos P, MacDermid JC, Birmingham T. The effectiveness of Instrument-Assisted soft tissue mobilization in athletes, participants without extremity or spinal conditions, and individuals with upper extremity, lower extremity, and spinal conditions: a systematic review. Archives of Physical Medicine and Rehabilitation. 2019 Sep 1;100(9):1726-51.
- ↑ Fowler S, Wilson JK, Sevier TL. Innovative approach for the treatment of cumulative trauma disorders. Work. 2000 Jan 1;15(1):9-14.
- ↑ Wilson JK, Sevier TL, Helfst R, Honing EW, Thomann A. Comparison of rehabilitation methods in the treatment of patellar tendinitis. Journal of Sport Rehabilitation. 2000 Nov 1;9(4):304-14.
- ↑ Thomas L. Sevier, M.D. Gale M. Gehlsen, Ph.D. Sue A. Stover, P.T. Julie K.Wilson M.S.A. Form of Augmented Soft Tissue Mobilization In the Treatment of Lateral Epicondylitis.Medicine and science in sports and exercise.1995;27(5).
- ↑ Prohealthsys. What is IASTM? - Dr. Nikita Vizniak prohealthsys.com. Available from: https://www.youtube.com/watch?v=65e-mp3Xjh0 [last accessed 3/11/2020]
- ↑ 9.0 9.1 Cheatham SW, Lee M, Cain M, Baker R. The efficacy of instrument assisted soft tissue mobilization: a systematic review. The Journal of the Canadian Chiropractic Association. 2016 Sep;60(3):200.
- ↑ Gehlsen GM, Ganion LR, Helfst RO. Fibroblast responses to variation in soft tissue mobilization pressure. Medicine and science in sports and exercise. 1999 Apr;31(4):531.
- ↑ 11.0 11.1 Davidson CJ, Ganion LR, Gehlsen GM, Verhoestra BE, Roepke JE, Sevier TL. Rat tendon morphologic and functional changes resulting from soft tissue mobilization. Medicine and science in sports and exercise. 1997 Mar 1;29(3):313-9.
- ↑ Cheatham SW, Kreiswirth E, Baker R. Does a light pressure instrument assisted soft tissue mobilization technique modulate tactile discrimination and perceived pain in healthy individuals with DOMS?. The Journal of the Canadian Chiropractic Association. 2019 Apr;63(1):18.
- ↑ 13.0 13.1 Kim J, Sung DJ, Lee J. Therapeutic effectiveness of instrument-assisted soft tissue mobilization for soft tissue injury: mechanisms and practical application. Journal of exercise rehabilitation. 2017 Feb;13(1):12.
- ↑ Melham TJ, Sevier TL, Malnofski MJ, Wilson JK, Helfst Jr RH. Chronic ankle pain and fibrosis successfully treated with a new noninvasive augmented soft tissue mobilization technique (ASTM): a case report. Medicine and science in sports and exercise. 1998 Jun 1;30(6):801-4.
- ↑ Wilson JK, Sevier TL, Helfst R, Honing EW, Thomann A. Comparison of rehabilitation methods in the treatment of patellar tendinitis. Journal of Sport Rehabilitation. 2000 Nov 1;9(4):304-14.
- ↑ Snodgrass SJ, Rivett DA. Thumb pain in physiotherapists: potential risk factors and proposed prevention strategies. Journal of Manual & Manipulative Therapy. 2002 Oct 1;10(4):206-17.