Gout
Original Editors - Maggie Kraemer from Bellarmine University's Pathophysiology of Complex Patient Problems project.
Top Contributors - Maggie Kraemer, Admin, Lucinda hampton, Shaimaa Eldib, Fitim Cami, Kim Jackson, Simisola Ajeyalemi, Elaine Lonnemann, WikiSysop and Wendy Walker
Introduction[edit | edit source]
Gout is a characteristically intense acute inflammatory reaction that erupts in response to articular deposits of monosodium urate (MSU) crystals[1]. It usually presents with intermittent painful attacks followed by long periods of remission[2]. Most patients with gout have other comorbidities. The prevalence of gout is higher among individuals with chronic diseases such as hypertension, chronic kidney disease, diabetes, obesity, congestive heart failure, and myocardial infarction .[3] [4][5]
Epidemiology[edit | edit source]
Gout typically occurs in those above 40 years. There is a strong male bias of 20:1, with this bias more pronounced in younger and middle-aged adults. In the elderly, the gender distribution is more equal. Rarely seen in children (< 10% of all cases)[3] [6]
Risk Factors[edit | edit source]
The single most important risk factor is sustained hyperuricaemia, which can be caused by overproduction or underexcretion of urate. Hyperuricemia is abnormally high levels of uric acid in the blood. People with higher serum urate levels are not only at an elevated risk for gout flare-ups but will also have more frequent flare-ups over time.
Other factors implicated for gout and/or hyperuricemia: older age, male sex, obesity, a purine diet, alcohol, medications, comorbid diseases, and genetics. Offending medications include diuretics, low-dose aspirin, ethambutol, pyrazinamide, and cyclosporine. Genome-wide association studies (GWAS) have found several genes that are associated with gout.
- Dietary sources that can contribute to hyperuricemia and gout include consumption of animal food such as seafood (e,g., shrimp, lobster), organs (e.g., liver, and kidney), and red meat (pork, beef).
- Some drinks like alcohol, sweetened beverages, sodas, and high-fructose corn syrup may also contribute to this disease[4]
Pathology[edit | edit source]
The pathology is characterised by monosodium urate crystals deposition in periarticular soft tissues. Synovial fluid is a poor solvent for monosodium urate hence crystallisation occurs at low temperatures.
There are five recognised stages of gout:
- Asymptomatic hyperuricaemia
- Acute gouty arthritis
- Intercritical gout (between acute attacks)
- Chronic tophaceous gout
- Gouty nephropathy[3]
Characteristics/Clinical Presentation[edit | edit source]
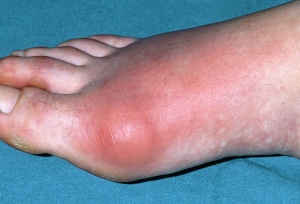
Acute gouty arthritis presents with a monoarticular red, inflamed, swollen joint, typically in the lower limb, classically affecting the first metatarsophalangeal joint. Often occurs during sleep, and may go on to involve more than one joint, becoming an oligoarthropathy or rarely, a polyarthropathy.
The acute phase usually last less than 10 days. within 7-10 days.
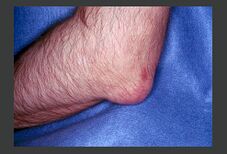
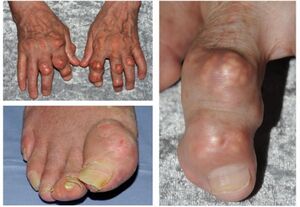
Patients with chronic uncontrolled hyperuricaemia, eg chronic kidney disease, may develop chronic tophaceous gout. In chronic tophaceous gout, there are solid urate crystal collections (tophi) and chronic inflammatory and destructive changes in surrounding connective tissue. Tophi are typically yellow-white in colour, non-tender, and are typically located within the articular structures, bursae, or the ears[3].
Management[edit | edit source]
The acute gout attacks are painful and potentially disabling, needing immediate treatment. The optimal therapy is towards controlling pain and inflammation.
- Acute flare ups: Management aims at decreasing the inflammation and the resulting pain. The physician should start the treatment within the first 24 hours of onset to reduce the severity and duration of the flare-up. Rest with topical application of ice packs can combined with non-steroidal anti-inflammatory drugs, colchicine, or systemic glucocorticoids. The length of the treatments should be at least 7 to 10 days to prevent rebound flare-ups.[4]
- Patients with recurrent attacks, tophi, urate arthropathy, or renal damage and to symptomatic patients with very high serum uric acid levels should start urate lowering therapy (ULT). In the long-term xanthine oxidase inhibitors (e.g. allopurinol or febuxostat), uricosuric drugs (e.g. probenecid), or uricase agents (e.g. pegloticase) may be used to reduce urate levels and prevent further acute flares[2].
- Tophaceous gout can also be managed with surgical excision of symptomatic lesions.
Non-pharmacologic : Patients with gout are encouraged to modify their lifestyles to prevent future attacks. Diet recommendations include reducing alcohol consumption, limiting purine-rich foods (meat, seafood, high fructose corn syrup, and sweetened soft drinks), and substituting low-fat or non-fat dairy products for their higher fat content counterparts. Weight loss and adequate hydration will also help reduce gout flare-up frequency[4].[7]
Diagnosis[edit | edit source]
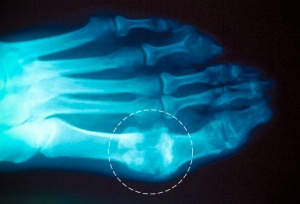
Synovial Fluid Analysis: Monosodium urate crystal identification remains the gold standard for gout diagnosis. Gout flare is marked by the presence of MSU crystals in synovial fluid obtained from affected joints of bursas visualized by direct examination of a fluid sample using compensated polarized light microscopy.[4]
Physical Therapy Management [edit | edit source]
The physical therapist should be aware that any patient with a history of gout, hyperuricemia, and/or a septic joint presentation should be referred for medical evaluation prior to treatment.[6]
During acute exacerbations the physical therapist should focus on reinforcement of management program and splinting, orthotics, or other assistive devices to protect the affected joint(s). [6]
A 2002 study in the Journal of Rheumatology found that the use of cryotherapy to alleviate the pain associated with acute bouts of gout may be effective. [8]
During intercritical phases physical therapists may offer assistance with maintenance of ROM, strength, and function. The physical therapist can also assist the patient in the creation of a suitable exercise routine and keeping their weight under control. [6][9]
Pseudogout[edit | edit source]
Pseudogout, also known as pyrophosphate Calcium pyrophosphate dihydrate disease (CPPD), is defined by the co-occurrence of arthritis with evidence of CPPD deposition within the articular cartilage. it is characterized by sudden, painful swelling in one or more of the joints. These episodes can last for days or weeks. The most commonly affected joint is the knee. It isn't clear why crystals form in the joints and cause pseudogout, but the risk increases with age. Treatments can help relieve pain and reduce inflammation[10].
- It is a form of arthritis that occurs 1/8th as often as gout.
- Symptoms are very similar to gout; however, the knee joint is primarily affected.
- Diagnosis is made by aspiration of synovial fluid.[11][12]
The difference between pseudogout and gout is outlined in below video.
Case Reports[edit | edit source]
One case report that presents interesting implications for the physical therapist involves an elderly patient with lumbar spondylodiscal pathology secondary to her polyarticular gout. [13]
Interesting case report involving a middle aged man that developed symptoms of gout during a hospitalization. [14]
Case report of a patient whose tophi were limiting the FDS tendon. [15]
Case report involving presentation and differential diagnosis of acute monoarthritis. [16]
A series of case reports that examine some of the negative effects of Colchicine as a form of pharmacological management. [17]
References[edit | edit source]
- ↑ Cronstein BN, Terkeltaub R. The inflammatory process of gout and its treatment. Arthritis Research & Therapy. 2006 Apr;8(1):1-7 Available: .https://arthritis-research.biomedcentral.com/articles/10.1186/ar1908#Abs1 (accessed 15.5.2022)
- ↑ 2.0 2.1 Drug and Therapeutics Bulletin. Latest guidance on the management of gout. Available: https://www.bmj.com/content/362/bmj.k2893(accessed 15.5.2022)
- ↑ 3.0 3.1 3.2 3.3 Radiopedia Gout Available: https://radiopaedia.org/articles/gout(accessed 14.5.2022)
- ↑ 4.0 4.1 4.2 4.3 4.4 Fenando A, Widrich J. Gout (podagra).Available:https://www.ncbi.nlm.nih.gov/books/NBK546606/ (accessed 14.5.2022)
- ↑ Joseph Kaplan, MD, MS, FACEP Attending Physician, Department of Emergency Medicine, Martin Army Community Hospital, Fort Benning, Georgia
- ↑ 6.0 6.1 6.2 6.3 Goodman CC, Fuller KS. Pathology: Implications for the Physical Therapist. 3rd ed. Saint Louis, MO: Saunders; 2009.
- ↑ Primatesta P, Plana E, Rothenbacher D. Gout treatment and comorbidities: a retrospective cohort study in a large US managed care population. BMC musculoskeletal disorders. 2011 Dec;12(1):103.
- ↑ Schlesinger N, Detry MA, Holland BK, Baker DG, Beutler AM, Rull M, Hoffman BI, Schumacher HR Jr. Local ice therapy during bouts of acute gouty arthritis. J Rheumatol 2002; 29(2): 331-334
- ↑ Gout. National Institute of Arthritis and Musculoskeletal and Skin Diseases. December 2006. http://www.niams.nih.gov/Health_Info/Gout/default.asp. Accessed March 2010.
- ↑ Mayo clinic Pseudogout Available: https://www.mayoclinic.org/diseases-conditions/pseudogout/symptoms-causes/syc-20376983(accessed 15.5.2022)
- ↑ Goodman C, Snyder T. Differential Diagnosis for Physical Therapists: Screening for Referral. St. Louis, Missouri: Saunders Elsevier, 2007.
- ↑ Wheeless, C R. Pseudogout and Chondrocalcinosis. Wheeless' Textbook of Orthopaedics. November 2008. www.wheelessonline.com/image9/cppd2.jpg. Accessed March 2010.
- ↑ Lagier R, Gee W M. Spondylodiscal erosions due to gout: anatomicoradiological study of a case. Annals of the Rheumatic Diseases. 1983 June; 42(3): 350-353.
- ↑ Dhoble A, Balakrishnan V, Smith R. Chronic tophaceous gout presenting as acute arthritis during an acute illness: a case report. Cases Journal. 2008; 1: 238.
- ↑ Sano K, et. al. Atypical Triggering at the Wrist due to Intratendinous Infiltration of Tophaceous Gout. Springer Hand. 2009 March; 4(1): 78-80.
- ↑ Ma L, Cranney A, and Holroyd-Leduc J. Acute monoarthritis: What is the cause of my patient's painful swollen joint. CMAJ. 2009 January; 180(1): 59-65.
- ↑ Morris I, Varughese G, and Mattingly P. Colchicine in acute gout. BMJ. 2003 November; 327(7426): 1275-1276.