Core Stability
Original Editor - Sem Bras
Top Contributors - Sheik Abdul Khadir, Katherine Knight, Lucinda hampton, Khloud Shreif, George Prudden, Sem Bras, Vanessa Rhule, Yagdutt Yagdutt, Admin, WikiSysop, Kim Jackson, Wanda van Niekerk and Venus Pagare
Introduction[edit | edit source]
The core is the centre of our body and it functions to stabilize the trunk while the arms and legs move during functional movements. When we view it this way, we see that the core actually includes:
- Muscles that stabilize the hips.
- The system of muscles that make up the torso (on the front, the sides, and the back of the body).
- Muscles that stabilize the shoulders.[1]
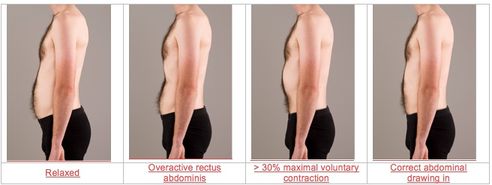
Image 1 and 2: Examples of core exercises: plank; abdominal drawing in maneuver (Figure 2).
The importance of the core relate to its function ie sparing the spine from excessive load and transfer force from the lower body to the upper body and vice versa.
- Having a strong, stable core helps us to prevent injuries and allows us to perform at our best.
- In order to protect the back, ideally we want to create 360 degrees of stiffness around the spine as we move, run, jump, throw, lift objects and transfer force throughout our body.
- We do this when all of the muscles in our hips, torso and shoulders work together[1][2]
Clinically relevant anatomy[edit | edit source]
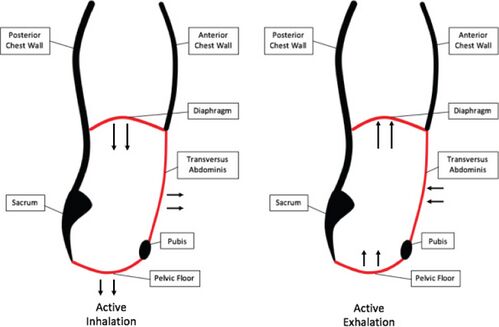
The core is a box structure made up of the abdominal muscles in the front and the sides, the paraspinal and gluteal muscles at the back, the diaphragm at the roof, and the pelvic floor and the hip girdle muscles as the floor. The abdominal muscles create a rigid cylinder around the spine during movement and provide stability.
Image 3: Abdominal canister
The inner core muscles include:
- Pelvic floor. The increased effort by the abdominal muscles can only increase intra-abdominal pressure during spinal movement if there is co-contraction of the pelvic floor musculature.
- Transversus abdominis. The activity of the Transversus abdominis is recorded during the entire range of flexion and extension of the spine. This co-activation of the abdominal muscles during spinal movement is needed to maintain spinal stability.[1]
- Internal Abdominal Obliques
- Multifidus. The multifidus, which is deeper, has direct attachments to the spinal segments, and allows stabilization of the motion segment during lifting and rotational movements of the spine. The deeper uni segment muscles being close to the axis of the spine act as force transducers. Higher concentrations of muscle spindles are located in the smaller uni-segmental muscles
- Diaphragm
- Some literature also includes the deep fibres of the psoas and the deep hip rotators as part of the inner core.
The outer core muscles or the global muscles are also referred to as the “movers” and include:
- Rectus abdominis .
- External obliques: Involved in rotational movements. Do not have a direct attachment to the spinal segment, unable to stabilize the individual segments.
- Erector spinae: Involved in lifting. Do not have a direct attachment to the spinal segment, unable to stabilize the individual segments.
- Quadratus lumborum
- Hip muscle groups
Change in Motor Patterns due to Pain
The neural subsystem anticipates the loading of the spine and activates contraction of the transverse abdominis and multifidus muscle ahead of the loading.[3] When there is a delay in the contraction of the multifidus, the larger and global superficial muscles eg erector spinae contract to compensate for the delay in increasing the stiffness of the lumbar spine.[3]
- In individual with low back pain due to impaired proprioceptive deficits this biofeedback is delayed leading to excessive stress on structures of low back. Due to pain there is further proprioceptive deficit leading to a vicious cycle of pain and disability[4]
- There is strong evidence supporting the effectiveness of treatment aimed at normalizing this function by way of specific motor control training, and specific muscle activation[5].
Physiotherapy Assessment[edit | edit source]
1. Local / deep muscles: Assessment of the function of the local/deep muscles is analogous with providing treatment. An understanding of the normal response is required for the abdominal drawing-in maneuver (transversus abdominis), isometric activation of multifidus, normal breathing (diaphragm), and pelvic floor activation[6].
2.Global/superficial muscles: There is a wide range of outcome measures for the dysfunction of the global muscles regarding core stability/motor control. Examples include: [8]
- Prone instability test
- Prone extension endurance test (Biering-Sorenson paraspinal endurance strength)
- Side bridge endurance test (quadratus lumborum endurance strength)
- Pelvic bridging
- Leg lowering test (lower abdominal strength)
- Curl-up Test
- Hip external rotation strength
- Modified Trendelenburg test (single leg squat with observation in the frontal plane)
- Single leg squat in the sagittal plane
- Single leg squat in the transverse plane
Clinical prediction rules identifying people (with low back problems) likely to respond to specific motor control/specific muscle activation of the local muscles [9]:
- Younger age (<40)
- Greater general flexibility (hamstring length greater than 90°, postpartum)
- Positive prone instability test
- Presence of aberrant movement during spinal range of motion (painful arc of motion, abnormal lumbopelvic rhythm, and using arms on thighs for support)
Physiotherapy Treatment[edit | edit source]
Treatment focuses on retraining Motor Control.
- Local/deep muscles: People with significant pathology where there is local muscle dysfunction, are likely to retrain a specific motor control before moving into more global training.[10]
- Global /superficial muscles: It is important for practitioners/sports personnel attempting to global/superficial muscle strength to have a clear understanding of any pathoanatomical problems that may be positively or negatively affected by such exercise. Ideally, all of these exercises should be done with correct lumbopelvic posture and control of the local/deep muscles. With most of these exercises duration of hold and repetitions can be varied (depending on the aim of the retraining/strengthing program) provided the exercise is done with good control.
Examples of exercises to improve the motor control /core stability of the lumbar spine. See Core Strengthening for a more in depth read.
Crunches- Lie supine on the floor with your knees bent, arms crossed over your chest and the feet flat on the floor. Then lift your shoulders from the ground and curl your stomach. Avoid a full sit up and ensure the low back remains in contact with the floor.
Obliques crunches - As per a normal crunch but leading with one shoulder towards the opposite knee (alternate sides each repetition).
Plank - see link
Bridges - Lie supine with your knees bent and the feet flat on the floor. Lift your pelvis off the ground while supporting on your feet and shoulders. The bridge can be progressed by lifting one foot off the ground end extending the knee.
Hamstring raises/ Bird Dog leg only- Balance on your hands and knees with your back flat and your arms/thighs perpendicular to the floor. Raise one leg behind you until it is horizontal. Alternate.
Superman – As per a hamstring raise but progress by lifting the opposite arm to a horizontal position at the same time. Alternate.
Leg raises - Lie on your back with your legs straight and your arms by your sides. Then lift one leg 4 inches of the ground. Your back has to stay flat on the floor. Don’t allow it to arch. Alternate. The exercise can be progressed by lifting both legs at the same time.
Hundreds - Lie on your back with your legs straight and your arms by your sides. Then lift both legs so that they form a right angle in the hip and knees. Lift your arm straight a few inches off the ground. Focus on keeping your hips and legs completely still and your back flat.
There are also multiple exercises that can be performed with a physioball. The exercises were proven to have a greater gain of torso balance and neural activity than regular floor exercises.[17]
Summary[edit | edit source]
There is no single muscle or single exercise for low back problems and motor control/core stability as a treatment. At a minimum practitioners/sports personnel should be aware of key concepts in motor control and exercise and follow an evidence-based approach to exercise prescription.
Currently, there is strong evidence for specific motor control/specific muscle activation in isolation, progressing to more global and functional exercises.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 Nastionwide Children's Core Stability Available: https://www.nationwidechildrens.org/family-resources-education/700childrens/2018/07/core-stability(accessed 2.1.2022)
- ↑ 4. Panjabi MM. The stabilizing system of the spine. Part II. Neutral zone and stability hypothesis. J Spinal Disord. 1992;5:383-9.
- ↑ 3.0 3.1 Studnicka K, Ampat G. Lumbar Stabilization. StatPearls [Internet]. 2021 Jan 29.Available:https://www.ncbi.nlm.nih.gov/books/NBK562179/ (accessed 2.1.2022)
- ↑ Lin J, Halaki M, Rajan P, Leaver A. Relationship Between Proprioception and Pain and Disability in People With Non-Specific Low Back Pain. A Systematic Review With Meta-Analysis. Spine J. 2019;44(10):E606–17.
- ↑ Cosio-Lima LM, Reynolds KL, Winter C, Paolone V, Jones MT. Effects of physioball and conventional floor exercises on early phase adaptations in back and abdominal core stability and balance in women. The Journal of Strength & Conditioning Research. 2003 Nov 1;17(4):721-5. Available:http://fitnessmais.com.br/download/treinamento-funcional(2)/Instability_15.pdf (accessed 3.1.2022)
- ↑ Akuthota V, Ferreiro A, Moore T, Fredericson M. Core stability exercise principles. Current sports medicine reports. 2008 Jan 1;7(1):39-44.
- ↑ daney20. 02 Activating & Training Multifidus Muscle Contractions. Available from: http://www.youtube.com/watch?v=fUU0pGZ0v_U[last accessed 26/1/2020]
- ↑ Lederman E. The myth of core stability. Journal of bodywork and movement therapies. 2010 Jan 1;14(1):84-98.
- ↑ Hicks GE, Fritz JM, Delitto A, McGill SM. Preliminary development of a clinical prediction rule for determining which patients with low back pain will respond to a stabilization exercise program. Archives of physical medicine and rehabilitation. 2005 Sep 1;86(9):1753-62..
- ↑ Stanton R, Reaburn PR, Humphries B. The effect of short-term Swiss ball training on core stability and running economy. The Journal of Strength & Conditioning Research. 2004 Aug 1;18(3):522-8.
- ↑ YOURHEP. Trunk Curl.mov . Available from: http://www.youtube.com/watch?v=SHsDnDwNjec[last accessed 2/2/2021]
- ↑ Passion4Profession. How to Plank . Available from: http://www.youtube.com/watch?v=TvxNkmjdhMM[last accessed 2/2/2021]
- ↑ Bird and Dog leg Only. Available from you tube: https://youtu.be/p5YSSeXdA88.[Last accessed on 15/11/2021]
- ↑ Performance Training Systems. Quadruped alternating Arm & Leg Extensions | Bird Dog .Available from: http://www.youtube.com/watch?v=gGy0wINNWxk[last accessed 2/2/2021]
- ↑ EkhartYoga.Single Leg raises for Leg and Ab strength Yoga. Available from: http://www.youtube.com/watch?v=gSi8z1gIdC8[last accessed 2/2/2021]
- ↑ Howcast.How to Do The Hundred | Pilates Workout.Availablefrom:http://www.youtube.com/watch?v=UaqpuUzs1i8[last accessed 2/2/2021]
- ↑ Cosio-Lima LM, Reynolds KL, Winter C, Paolone V, Jones MT. Effects of physioball and conventional floor exercises on early phase adaptations in back and abdominal core stability and balance in women. The Journal of Strength & Conditioning Research. 2003 Nov 1;17(4):721-5.