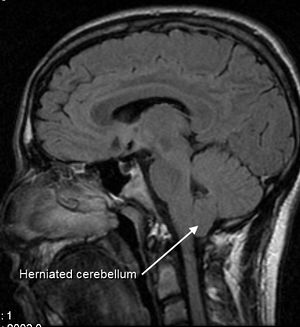
Arnold Chiari Malformation
Introduction[edit | edit source]
Arnold Chiari Malformation, also known as Chiari type II malformation, is one of a group of brain malformations affecting the cerebellum[1]. Named after Hans Chiari and Julius Arnold, the pathologists who first described the group of malformations[2]. This condition is almost always associated with myelomeningocele, the most serious form of spina bifida.
Clinically Relevant Anatomy[edit | edit source]
Normally the cerebellum and parts of the brain stem sit in an indented space at the lower rear of the skull, above the foramen magnum (a funnel-like opening to the canal). When part of the cerebellum is located below the foramen magnum, it is called a Chiari malformation. In Arnold Chiari Malformation, both cerebellar and brain stem tissue protrude into the foramen magnum and the cerebellar vermis (the nerve tissue that connects the two halves of the cerebellum) may be only partially complete or absent.
This condition has skull, dural, brain, spinal, and spinal cord manifestations, including the downward displacement of the medulla, fourth ventricle, and cerebellum into the cervical spinal canal, as well as elongation of the pons and fourth ventricle, probably due to a relatively small posterior fossa[3].
The brainstem is elongated and displaced into the opening of the base of the skull and into the top of the spinal canal[4]. It is often kinked. The brainstem, cranial nerves and lower portion of the cerebellum may be stretched or compressed. This means that any of the functions controlled by these areas may be affected;
Clinical Presentation[edit | edit source]
Many people with Arnold Chiari malformation have no obvious symptoms. Compressive mechanisms are thought to cause symptoms, but it is likely that stretching of abnormally placed cranial nerves may provoke symptoms. In babies, the most common symptoms are a weak or absent cry, breathing difficulties, including stridor, arching of the neck, failure to thrive and feeding or swallowing difficulties. a weak cry, gagging or vomiting, arm weakness, a stiff neck, developmental delays, and an inability to gain weight.
Blockage of cerebrospinal fluid (CSF) flow may cause the formation of a syrinx, which can lead to syringomyelia. Central cord symptoms such as hand weakness, sensory loss, and, in severe cases, paralysis may occur.
Common symptoms people with Chiari Type II malformations might experience are:
- headaches (usually at the back of the head and often made worse by coughing, sneezing or straining)
- neck pain
- dizziness and balance problems
- hearing loss and/or tinnitus
- muscle weakness and paralysis
- visual problems and nystagmus
- swallowing difficulties
- dysesthesia in the limbs
- problems with hand coordination and fine motor skills.
Diagnostic Procedures[edit | edit source]
The key tests for diagnosis of Arnold Chiari Malformation are MRI and CT scans[5]. An MRI will show the abnormal CSF flow and configuration and position of the brain and spinal cord[6]. Antenatal ultrasound imaging shows an indentation of the frontal bone with an abnormally shaped cerebellum[7].
Differential Diagnosis[edit | edit source]
The main differential diagnosis is the type of Chiari malformation.
- Chiari I malformation does not have a myelomeningocoele.
- Chiari III has an occipital and/or high cervical encephalocele.
- Chiari IV has severe cerebellar hypoplasia without displacement of the cerebellum through the foramen magnum.
Epidemiology[edit | edit source]
It used to be said that Chiari malformations are rare, but with routine use of MR imaging, Chiari malformation is discovered with increasing frequency. Chiari II is found in all children with myelomeningocele, although less than one-third develop symptoms referable to this malformation[8].
Physiotherapy Management[edit | edit source]
Physiotherapy can help with many of the symptoms caused by Arnold Chiari Malformation:
- Vestibular Rehabilitation is indicated when patients have vestibular problems
- Conservative physiotherapy soft tissue techniques may be of benefit for cervical pain
- Soft tissue techniques may be of benefit for headaches
Surgical Interventions[edit | edit source]
- myelomeningocele repair and management of neurogenic bladder
- ventricular shunting - hydrocephalus usually requires shunting and can improve the cranial nerve and brainstem function
- craniovertebral decompression may be required in neonates with brainstem dysfunction if hydrocephalus is not present, or if symptoms and signs do not improve with shunting. Some older patients with hindbrain herniation or syringohydromyelia may also benefit from ventricular shunts.
Prognosis[edit | edit source]
Many with Type I CM do not show symptoms and do not know they have the condition. Symptoms vary among individuals, Individuals who have severe Chiari malformation and have undergone surgery see a reduction in their symptoms, Even though paralysis may be permanent[9]
Resources[edit | edit source]
See resources on the Chiari Malformations page for links to useful items by the Brain & Spine Foundation.
References[edit | edit source]
- ↑ Koehler PJ. Chiari's description of cerebellar ectopy (1891). With a summary of Cleland's and Arnold's contributions and some early observations on neural-tube defects. J Neurosurg. Nov 1991;75(5):823-6
- ↑ Schijman (2004). "History, anatomic forms, and pathogenesis of Chiari malformations". Child's nervous system 20 (5): 323
- ↑ Truivit CL, Backovich A. Disorders of brain development. In: Atlas SW, ed. Magnetic Resonance Imaging of the Brain and Spine. 2nd ed. Philadelphia, Pa: Lippincott-Raven; 1996.
- ↑ Stevenson KL. Chiari Type II malformation: past, present, and future. Neurosurg Focus. Feb 15 2004;16(2):E5.
- ↑ Curnes JT, Oakes WJ, Boyko OB. MR imaging of hindbrain deformity in Chiari II patients with and without symptoms of brainstem compression. AJNR Am J Neuroradiol. 10 (2): 293-302
- ↑ Pillay PK, Awad IA, Little JR, Hahn JF. Symptomatic Chiari malformation in adults: a new classification based on magnetic resonance imaging with clinical and prognostic significance. Neurosurgery. May 1991;28(5):639-45
- ↑ El gammal T, Mark EK, Brooks BS. MR imaging of Chiari II malformation. AJR Am J Roentgenol. 1988;150 (1): 163-70
- ↑ Dias M. Myelomeningocoele. In: Choux M, Di Rocco C, Hockley A, Walker M. Pediatric Neurosurgery. London: Churchill Livingston; 1999:33-61.
- ↑ National institute of neurological disorders and stroke. Available from https://www.ninds.nih.gov/Disorders/All-Disorders/Chiari-Malformation-Information-Page#disorders-r3 (accessed on 30/9/2020)