Ankle Impingement
Original Editors Heather Hughes
Top Contributors - Laura Ritchie, Yarne Leuckx, Admin, Christine Utskot, Angela Dempski, Heather Hughes, Lucas De Bondt, Karina Leahy, Alicia shugart, Rachael Lowe, Kim Jackson, Simisola Ajeyalemi, Charlotte Moreau, Fasuba Ayobami, Thomas Albaugh, Thibault Casier, Khloud Shreif, Olajumoke Ogunleye, Evan Thomas, Naomi O'Reilly, WikiSysop, 127.0.0.1, Thomas De Meersman, Rucha Gadgil, Wanda van Niekerk and Jess Bell
Definition/Description[edit | edit source]
Ankle impingement is defined as pain in the ankle due to impingement in one of two areas: anterior (anterolateral and anteromedial) and posterior (posteromedial).[1] Location of pain is referenced from the tibiotalar (talocrural) joint.[2] Anterior ankle impingement generally refers to entrapment of structures along the anterior margin of the tibiotalar joint in terminal dorsiflexion. Posterior ankle impingement results from compression of structures posterior to the tibiotalar and talocalcaneal articulations during terminal plantar flexion.[3] Pain is caused by mechanical obstruction due to osteophytes and/or entrapment of various soft tissue structures due to inflammation, scarring or hypermobility. The condition is common in athletes, especially soccer players, distance runners and ballet dancers.[4] Noted in athletes whose sports necessitated sudden acceleration, jumping, and extremes of dorsiflexion or plantar flexion.[5] Historically, it has been called "athlete's ankle" and "footballer's ankle".[6]
Clinical Relevant Anatomy[edit | edit source]
Talocrural Joint[edit | edit source]
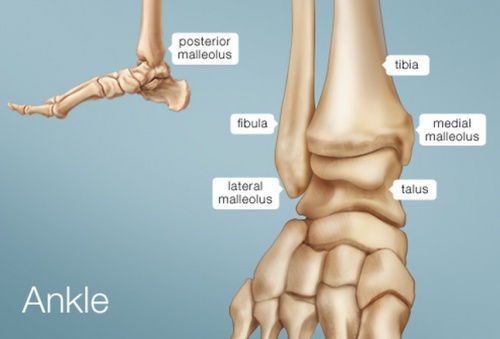
The ankle joint is a synovial hinge joint comprised of hyaline covered articular surfaces of the talus, the tibia as well as the fibula, allowing up to 20 degrees dorsiflexion and 50 degrees plantarflexion. The distal ends of the tibia and fibula are held together firmly by ligaments of the medial (Deltoid) and lateral ligament complexes of the ankle. The ligaments hold the tibia and fibula into a deep bracket-like shape in which the talus sits.
- The ROOF of the joint is the distal inferior surface of the tibia
- The MEDIAL SIDE of the joint is formed of the medial malleolus of the tibia
- The LATERAL SIDE of the joint is formed of the lateral malleolus of the fibula
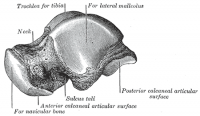
The articular part of the talus looks like a cylinder and fits snugly into the bracket provided by the syndesmosis of the tibia and fibula, when looking down upon the talus the articular surface is wider anteriorly than posteriorly. Subsequently this increases the congruent, stable nature of this joint when it is in dorsiflexion. As this is a synovial joint, a membrane is present as well as a fibrous membrane providing the same functions as any other synovial joint synovial membrane.
Subtalar Joint[edit | edit source]
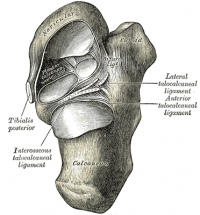
The Subtalar joint is also known as the Talocalcaneal joint and is between:
- The large posterior calcaneal facet on the inferior surface of the talus; and
- The corresponding posterior facet on the superior surface of the calcaneus
This joint, due to its orientation, allows the movements of inversion (0-35 degrees) and eversion (0-25 degrees), broken down this must mean the joint allows some amount of glide and rotation. It is known as a simple synovial condyloid joint. There are a large number of strong ligaments supporting the joint.
Epidemiology/Etiology[edit | edit source]
Impingement syndromes in the ankle include a broad spectrum of pathology with varying etiologies. Although no official classification exists, these syndromes are generally defined by the particular anatomic area involved. Specifically: anterior, anterolateral, anteromedial, posterior, posteromedial, posterolateral.[7]
Ankle impingement is a common condition occurring secondary to sprain or repeated microtrauma.[8]
Anterior Impingement (AI)[edit | edit source]
Often know as "athlete's ankle" or "footballer's ankle" is caused by repeated dorsiflexion, microtrauma, and repeated inversion injury causing damage to anteromedial structures such as the articular cartilage. It is further classified into Anteromedial & Anterolateral Impingement[2]. Coincident chondral and osteochondral lesions may be found in patients with AI.[9] It can also be seen after nonsporting injuries, especially fractures about the ankle and foot. There appears to be an association with a subtle cavus foot (high arched foot) and ankle instability.[10]
Anterior intra-articular soft tissues may contribute to impingement in isolation or in conjunction with bony lesions. A triangular soft tissue mass composed primarily of adipose and synovial tissues exists in the anterior joint space. These tissues are compressed after 15° of dorsiflexion in asymptomatic individuals. Anterior osteophytes may limit the space available for this soft tissue and exacerbate its entrapment, resulting in chronic inflammation, synovitis, and capsuloligamentous hypertrophy. In patients with anterior impingement, pain and a range of motion limitation may be secondary to impingement of this soft tissue.[7][11]
- Anteromedial Impingement: Hypothesized etiology includes: inversion ankle sprains; repetitive dorsiflexion resulting in spurs; repetitive capsular traction causing the formation of osteophytes, and chronic microtrauma to the anterior joint area. However, the cause remains unknown with the above theories mentioned in the literature.
- Anterolateral Impingement: May be caused by inversion ankle sprains causing inflammation and scar formation or reactive synovitis. May also be due to forced plantarflexion and supination which can tear anterolateral capsular tissues.[2]
Posterior Impingement (PI)[edit | edit source]
Often known as "dancer's heel", is generally insidious in nature, occurring in athletes who routinely plantarflex, such as ballet dancers, jumping athletes, and those who kick.[2] Posterior ankle impingement is a common cause of chronic ankle pain.[12]May be caused by bony or soft tissue impingement, specifically flexor hallucis longus irritation, thickening of the posterior capsule, synovitis, inversion trauma/sprain, forced plantarflexion causing anterior sheering of the tibia, hypertrophy of the os trigonum impacting the posterior tibia. Also known as os trigonum syndrome and posterior tibiotalar compression syndrome.[13] The os trigonum is the most common cause of symptomatic posterior ankle impingement.[12]
- Posteromedial impingement: Chronic posteromedial pain is mostly caused by scar tissue that consists of the posterior fibres. When there’s an ankle inversion trauma, with the ankle in plantar flexion, the fibres of the posterior ligament become compressed.[14] The structures involved in posteromedial ankle impingement include the posteromedial tibiotalar capsule and posterior fibres of the tibiotalar ligament. Their location between the talus and medial malleolus predisposes to the entrapment during supination. The subsequent fibrosis and thickening of the injured posterior tibiotalar ligament and posteromedial capsule cause impingement between the medial wall of the talus and posterior margin of the medial malleolus, resulting in formation of collagenous and fibrous meniscoid lesions and synovitis at the posteromedial ankle.[15]
- Posterolateral impingement: This injury is caused by the Posterior Talofibular Ligament (also called the Posterior intermalleolar ligament). However, this ligament is an anatomic variant, it is present in 56% of the population. During a plantar flexion, the PTL will entrap and then finally torn.[16]
Characteristics/Clinical Presentation[edit | edit source]
People suffering from anterior/posterior ankle impingement were found to have moderate to severe limitation in activities of daily living due to pain.[17]Symptoms development may be insidious or in response to sudden injury.[5]
Anterior[edit | edit source]
Anterior ankle pain accompanied by a 'blocking sensation' in dorsiflexion. May also present with palpable soft tissue swelling over anterior joint.[5] As anterior impingement becomes chronic, additional symptoms may include instability; limited ankle motion; and pain with squatting, sprinting, stair climbing, and hill climbing. Normal gait may be unaffected.[2]
- Anterolateral: Patients experience anterolateral ankle pain that is intensified with supination or pronation of the foot, anterolateral point tenderness, pain with a single-leg squat, and swelling.[5] Patients may have a history of ankles sprains or chronic ankle instability and now present with constant lateral ankle pain upon ambulation.
- Anteromedial: A good portion of these patients will have chronic anteromedial pain that is intensified by dorsiflexion, tender to palpation over anteromedial joint line, soft tissue swelling, and decreased ROM into forced dorsiflexion as well as supination.[8]
Posterior[edit | edit source]
Patients have posterior ankle pain intensified by forced plantarflexion or dorsiflexion. May also have joint line tenderness of the posterior tibiotalar joint (not involving the achilles tendon)[5]. The ankle has a limited plantar flexion and a ligamentous instability with thickening of the soft tissue.[2]
- Posteromedial: A key clinical finding for a patient with a posteromedial impingement is tenderness to the posteromedial aspect upon inversion with the ankle in plantar flexion. Tenderness is most seen in passive ankle inversion and passive plantar flexion. There is also pain in the posteromedial region of the ankle.[2] This helps to differentiate from pain that comes from a tibialis posterior abnormality.[5]
- Posterolateral: A patient with a posterolateral impingement has the feeling of ankle locking and has pain at the posterior side of the ankle. The impingement is preceded by an acute inversion injury with plantar flexion. The ligament ( posterior talofibular) is compressed and torn, this leads to an hypertrophy of this ligament. This injury is the most common in sports with a repetitive plantar flexion (e.g. ballet, soccer, volleyball).
Athletes affected by posterior impingement may attempt to compensate for the loss of plantar flexion by assuming an inverted foot position this may predispose to:
- frequent ankle sprains
- calf sprain
- contractures
- planter foot pain
- toe curling
Differential Diagnosis[edit | edit source]
| Anterior ankle pain[17][18] |
|
| Posterior ankle pain[18][20] |
|
| Medial ankle pain[18] |
|
| Lateral ankle pain[18] |
|
Diagnostic Procedures[edit | edit source]
Chronic ankle pain, swelling, and limitation of ankle dorsiflexion are common complaints. Imaging is valuable for diagnosis of the bony impingement but not for the soft tissue impingement, which is based on clinical findings.[3]
Conventional radiography is usually the first imaging technique performer and allows assessment of any potential bone abnormality, particularly in anterior and posterior impingement. Computed tomography (CT) and isotope bone scanning have been largely superseded by magnetic resonance (MR) imaging. MR imaging can demonstrate osseous and soft-tissue edema in anterior or posterior impingement. MR imaging is the most useful imaging modality in evaluating suspected soft-tissue impingement.[19] Also ultrasound is accurate in diagnosing soft tissue impingement lesions within the anterolateral aspect of the ankle and can evaluate associated ligament injuries and differentiate the disease from bony impingement.[3]
Outcome Measures[edit | edit source]
All contain evidence regarding score interpretation including content validity, construct validity, reliability, and responsiveness.[21]
- The Lower Extremity Function Scale (LEFS) was created to be a broad region-specific measure appropriate for individuals with musculoskeletal disorders of the hip, knee, ankle, or foot. Can be used to evaluate disorder of one or both lower extremities and consist of 20 items that specifically address the domains of activity and participation. Scores range from 0-80 with the lower the score representing a greater the disability.
- The Foot Function Index (FFI) is viewed as an instrument tool to measure function in patients with rheumatoid arthritis, however, the authors claim there is no specific disease relation to rheumatoid arthritis in this assessment. The FFI is a region specific instrument for pathologies in the older population and consists of 23 items grouped into 3 sub-scales, including activity limitation, disability, and pain subscales. A lower FFI score represents a higher level of function.
- The Foot and Ankle Ability Measure (FAAM) was developed as a region-specific instrument to comprehensively assess physical performance among individuals with a range of leg, foot, and ankle musculoskeletal disorders. Used to detect changes in self-reported function over time, as well as to evaluate the effectiveness of a specific intervention being delivered by a clinician. Instrument is divided into 2 separately scored subscales, that include activities of daily living and a sports sub-scale.
- The Foot Health Status Questionnaire (FHSQ) region specific instrument that was developed for individuals undergoing surgical treatment in a podiatry practice for common foot conditions. This questionnaire takes 5 minutes to complete and consists of 4 sub-scales, including pain, function, footwear, general foot health. This questionnaire can be used by researcher and clinicians to identify changes in foot health status in response to therapeutic and surgical interventions.
- The Sports Ankle Rating System (QOL) is a self-reported and clinician completed assessment tool with 3 outcome measures that include a QOL measure, clinical rating score, and single numeric evaluation. The QOL measure, used to assess an athlete’s QOL after an ankle injury, contains 5 sub-scales that include symptoms, work and school activities, recreation and sports activities, activities of daily living, and lifestyle.
Examination[edit | edit source]
The physical examination should include inspection of the ankle for swelling, erythema, and alignment, joint effusion, or soft tissue edema.[22] Gait analysis may reveal asymmetry and malalignment as people can compensate for limited ankle DF in many ways. From a proximal compensation, runners can shorten their step length, have an early heel rise, or reduce their knee flexion. It can also be compensated for more distally by increasing pronation in order to allow more DF in the midfoot.
The bone and soft tissue structures are systematically palpated to assess for localized tenderness. While anterior or anterolateral tenderness is characteristic in anterior impingement, posterior impingement signs can be more difficult to elicit and localize, as structures are deeper. Posteromedial ankle tenderness with resisted plantar flexion of the first metatarsophalangeal joint is more consistent with FHL pathology, while posterolateral tenderness with forced ankle plantar flexion is more likely to involve pathology associated with the trigonal process.[7]
Passive and active ranges of motion of the joints bilaterally are measured, including dorsiflexion, plantar flexion, subtalar, and midfoot motions. Laterally, the peroneal tendon is assessed for tenderness, deformity, or subluxation. The sural nerve is evaluated for sensitivity. Posteriorly, the Achilles tendon is assessed for fusiform enlargement or retrocalcaneal bursitis. Medially, the tibial nerve is evaluated for tarsal tunnel syndrome, and the posterior tibial tendon’s function is assessed. The anterior drawer and talar tilt tests of the tibiotalar joint are performed to exclude ankle instability. Finally, a straight leg raise test in the seated or supine position may be done to exclude an L5 or S1 radiculopathy.[7]
Anterior ankle impingement Examination[23][edit | edit source]
5 or more present: Sen= .94 Spec=.75 +LR=3.76 -LR=.08
- pain with activities
- anterolateral ankle joint tenderness
- recurrent joint swelling
- anterolateral pain with forced dorsiflexion and eversion (Impingement sign: Sens=.95 Spec=.88 +LR=7.91 -LR=.06) [24]
- pain during single leg squat
- lack of lateral ankle instability
Additional tests:[12]
- An anterior drawer test for lateral ankle instability (Sen= .86 Spec= .74 +LR .22 and -LR .0018)
- The Silfverskiöld test for an isolated gastrocnemius contracture. The test is considered positive when ankle dorsiflexion is greater with the knee in flexion than in extension. MRI sensitivity = 39% Physical Examination sensitivity = 94% [23]
- Forced dorsiflexion
Posterior Ankle Impingement Examination[25][edit | edit source]
- Loss of mobility, accompanied by pain in posterior aspect of ankle
- pain with forced plantarflexion
- Prominent posterior talar processes
- Hyperplantar flexion test
Additional tests:[26]
- Deep pressure palpation of the posteromedial joint line: positive => tenderness
- Laxity tests (anterior drawer and inversion)
- Manual strength test: Anterior tibialis, Peroneus complex, Gastrosoleus complex
- Flexibility tests: Achilles tendon, Hamstring
- Forced Plantarflexion
- Forced Inversion
Medical Management[edit | edit source]
Diagnosis[27][edit | edit source]
- Standard radiographs
- MRI for soft tissue swelling and extent of injury
- Diagnostic injection is a local anesthetic administered into joint capsule and soft tissue, if injection relieved the symptoms it is a positive test.
Surgery[edit | edit source]
It is considered after conservative treatment has been tried first, at least 3 months.[6] El-Sayed et al states that arthroscopy is a useful method to treat patients with anterolateral impingement, results at follow-up showed 85% improved completely according to JSSF.[6] Chirugie et al showed VAS and AOFAS score improved significantly and 79% of patients returned to prior level of sport that had posterior ankle impingement.[28] Murawski et al showed 93% satisfaction, AOFAS and SF 36v2 significantly improved ~ 68% that had anteromedial impingement.[27] However, if athletic patients want to return to athletic activity promptly, then surgical intervention can be recommended early in the treatment process. The surgical approach and technique vary by the anatomic region and pathology involved[7].
Surgical methods include debridement, osteophyte removal, meniscoid lesion excision, partial capsulectomy, flexor hallux longus release, and chondroplasty of tibia may be performed.[29][30]
Complications include infection; neuropraxia; arthrofibrosis; complex regional pain syndrome and fibular nerve irritation.[27][28][30]
Anterior ankle impingement:
Surgical goals for the treatment of anterior impingement involve removing the offending pathologic lesion contributing to the symptoms. This may involve resection or debridement of bony lesions, soft tissue lesions, or both.[7]
Posterior ankle impingement:
Similarly, the surgical goal of treating posterior impingement involves resection of the causative anatomy. Most commonly, symptom relief is achieved by excision of a painful trigonal process or os trigonum, with debridement of surrounding inflammatory or hypertrophic soft tissues. Posterior pathology can be targeted through an open lateral, open medial, or endoscopic approach. A lateral approach allows for more direct access to the trigonal process with less risk to the medial neurovascular bundle. A medial approach allows for concomitant FHL pathology to be addressed more easily.[7]
Post-op:
For the posterior ankle impingement a compression bandage is applied after surgery and patients are allowed to be weight bearing as tolerated immediately after surgery. Patients may also begin ranging their ankle as tolerated. The goal of early ROM and weight bearing is to prevent post-operative stiffness and hopefully limit the delay in return to sport. Typically, ankle immobilisation is not necessary, unless patients had more significant osseous injury, which may require modifications of the above protocol.[31]
Medical Protocol: NWB in boot ~3 days, WBAT day 3, elevation for swelling, NSAIDs, ankle pumps, suture removal 10-14 days post-op, and refer to physical therapy.[32]
Physical Therapy Management[edit | edit source]
Treatment focuses on increasing available joint space for more mobility and less pain during activity. Nonsurgical treatment remains the initial approach to the management of both anterior and posterior impingement syndromes, despite limited evidence of its efficacy. For acute symptoms, a period of rest and an avoidance of provocative activities are recommended. In chronic cases, shoe modifications, including heel lift orthoses to prevent dorsiflexion, have been utilised.[7]
Patients should be treated conservatively after an inversion sprain of the ankle for at least 6 months.[5] They should be treated conservatively after an inversion injury of the ankle, with adequate joint rehabilitation, peroneal strengthening, and muscle balancing.[33] Patients who do not respond to conservative management may require operative intervention.[31]
Anterior Impingement[edit | edit source]
- Distraction manipulation
- A/P and lateral talocrural glides
- A/P distal fibula glides
- Cuboid whip (for those with decreased pronation)
- HEP: self A/P and lateral mobilisation, single leg balance, lunge dorsiflexion stretch, progressive ankle resistance exercises
- Lateral ankle stability protocols[34][35][36]
| Exercise 1 Basic exercise: Walking slowly back and forth on a balance board (1 step = 3 seconds). The contralateral leg swings through and nearly touches the ground |
Exercise 2: Basic exercise: Single leg (knee and hip flexed) stance on exercise mat with the contralateral leg flexed. Lower and raise the body. Distribute load on the foot. Only small knee movements to the left and right are allowed. |
Exercise 3: |
Exercise 4: Basic exercise: Maintain balance in single-leg stance elevating the contralateral leg against resistance of an elastic strap. Hold 30 seconds each leg. |
Exercise 5: Basic exercise: Maintain balance in single leg stance on inversion-eversion tilt board. The contralateral leg rested on an inclined surface nearly without being loaded. |
| Variation 1: Walking faster than before on the balance board. Way back: slowly with same execution as above. |
Variation 1: Single limb stance as above opposite to a partner. A ball is passed to the partner. After catching the ball the position is controlled for 2 seconds. Pass the ball back and forth |
Variation 1: Jump from one leg to the other on an exercise mat with a partner. Disturb each other during the flight phase (hand contact) and control the landing and stance for 4 seconds. |
Variation 1: Maintain balance in single leg stance ( eyes closed) elevating the contralateral leg against resistance of an elastic strap. |
Variation 1: Maintain balance in single leg stance on inversion-eversion tilt board. The contralateral leg rested on an inclined surface nearly without being loaded. This with a partner. Pass a ball and control stance after catching the ball. |
| Variation 2: Stance on a balance board. The contralateral leg moves a ball that lies on the ground in circles. Focus on the supporting leg. |
Variation 2: Single leg stance on a soft mat. Balance a ball on the dorsum of the dorsum of the elevated contralateral foot. |
Variation 2: Jump from one leg to the other on an soft exercise mat with a partner. Disturb each other during the flight phase (hand contact) and control the landing and stance for 4 seconds. |
Variation 2: Maintain balance in single leg stance moving the contralateral leg sideways against resistance of an elastic strap. Evert the lateral edge of the contralateral toot. |
Variation 2: |
All of these exercises can be performed on the different perturbations. For peroneal strengthening, a Thera-band can be used in this exercises.[37][38]
Posterior Impingement[edit | edit source]
- Plantarflexion mobilisation
- P/A talocrural mobilisation
- Rear-foot distraction manipulation
- Proprioceptive work - wobble board
- Peronei strengthening
- Isometric and eccentric exercises to strengthen and stretch the lower-leg muscles.[39]
- exercises to improve deep muscle action during plantarflexion. By using the deep muscles, the talus is shifted forward during plantarflexion, what will reduce the impact of the os trigonum on the posterior tibia.[39]
- HEP: Achilles tendon stretching, Single leg balance, lunge dorsiflexion stretch, progressive ankle resistance exercises[40]
- Protective dorsiflexion taping[16]
Prevention[edit | edit source]
Protective ankle dorsiflexion taping is recommended with the belief that it prevents posterior ankle impingement.[41] There is no consensus as to whether ankle support can interfere with normal function instead of reducing the pain and dysfunction caused by sports injury. While posterior impingement may be reduced by protective ankle dorsiflexion taping, but it also reduced the ankle plantar-flexion movement.[20]
Clinical Bottom Line[edit | edit source]
Ankle impingement is common within certain populations of athletes who repeatedly dorsiflex or plantarflex and/or have a history of inversion ankle sprains and other microtrauma. Current literature favours surgical intervention as treatment. There is a limited amount of high quality evidence for conservative management. Physical therapy should include manual therapy and exercise that aim to increase mobility of the ankle joint and decrease pain with ambulation.
References[edit | edit source]
- ↑ McClinton, S. Regis University. Ankle impingement sydromes: diagnosis and treatment. Available at: https//connect.regis.edu/p38686942/. Accessed on July 9, 2011.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 Robinson P. Impingement syndromes of the ankle. European Radiology [serial online]. December 2007;17(12):3056-3065
- ↑ 3.0 3.1 3.2 Vaseenon, Tanawat, and Annunziato Amendola. "Update on anterior ankle impingement.” Current reviews in musculoskeletal medicine 5.2 (2012): 145-150. http://link.springer.com/article/10.1007/s12178-012-9117-z
- ↑ Murawski C, Kennedy J. Anteromedial impingement in the ankle joint: outcomes following arthroscopy. American Journal of Sports Medicine [serial online]. October 2010;38(10):2017-2024. Available from: CINAHL Plus with Full Text, Ipswich, MA. Accessed July 9, 2011.
- ↑ 5.0 5.1 5.2 5.3 5.4 5.5 5.6 van den Bekerom, Michel PJ, and Eric EJ Raven. "The distal fascicle of the anterior inferior tibiofibular ligament as a cause of tibiotalar impingement syndrome: a current concepts review." Knee Surgery, Sports Traumatology, Arthroscopy 15.4 (2007): 465-471.
- ↑ 6.0 6.1 6.2 El-Sayed A. Arthroscopic treatment of anterolateral impingement of the ankle. Journal of Foot Ankle Surgery [serial online]. May 2010;49(3):219-223. Available from: CINAHL Plus with Full Text, Ipswich, MA. Accessed July 2, 2011.
- ↑ 7.0 7.1 7.2 7.3 7.4 7.5 7.6 7.7 Lavery, Kyle P., et al. "Ankle impingement." Journal of Orthopaedic Surgery and Research 11.1 (2016): 97. https://josr-online.biomedcentral.com/articles/10.1186/s13018-016-0430-x
- ↑ 8.0 8.1 Marquirriain J. Posterior “ankle impingement syndrome.” J AM Acad Orthop Surg. 2005 Oct; 13(6): 365-71 http://journals.lww.com/jaaos/Abstract/2005/10000/Posterior_Ankle_Impingement_Syndrome.1.aspx
- ↑ Rasmussen S, Hjorth Jensen C: Arthroscopic treatment of impingement of the ankle reduces pain and enhances function. Scand J Med Sci Sports 2002;12(2):69-72)
- ↑ Sports health: A Multidisciplinary Approach. Medial Impingement of the Ankle in Athletes. American Orthopaedic Society for Sports Medicine.
- ↑ Paul G. Talusan, MD, Jason Toy, MD, Joshua L. Perez, Matthew D. Milewski, MD, John S. Reach, Jr, MSc, MDAnterior Ankle Impingemeproprexnt: Diagnosis and Treatment: J Am Acad Orthop Surg 2014;22: 333-339
- ↑ 12.0 12.1 12.2 Sandro Giannini, Roberto Buda, Massimiliano Mosca, Alessandro Parma and Francesco Di Caprio,Posterior ankle impingement, Foot Ankle Int 2013 34: 459
- ↑ Wiegerinck JI, Vroemen JC, van Dongen TH, Sierevelt IN, Maas M, van Dijk CN. The posterior impingement view: an alternative conventional projection to detect bony posterior ankle impingement. Arthroscopy. 2014;30(10):1311-1316. doi:10.1016/j.arthro.2014.05.006
- ↑ Sandro Giannini, Roberto Buda, Massimiliano Mosca, Alessandro Parma and Francesco Di Caprio,Posterior ankle impingement, Foot Ankle Int 2013 34: 459
- ↑ Paul G. Talusan, MD, Jason Toy, MD, Joshua L. Perez, Matthew D. Milewski, MD, John S. Reach, Jr, MSc, MDAnterior Ankle Impingemeproprexnt: Diagnosis and Treatment: J Am Acad Orthop Surg 2014;22: 333-339
- ↑ 16.0 16.1 Sandro Giannini, Roberto Buda, Massimiliano Mosca, Alessandro Parma and Francesco Di Caprio,Posterior ankle impingement, Foot Ankle Int 2013 34: 459
- ↑ 17.0 17.1 Paul G. Talusan, MD, Jason Toy, MD, Joshua L. Perez, Matthew D. Milewski, MD, John S. Reach, Jr, MSc, MDAnterior Ankle Impingemeproprexnt: Diagnosis and Treatment: J Am Acad Orthop Surg 2014;22: 333-339
- ↑ 18.0 18.1 18.2 18.3 Goode L. Ankle Differential Diagnosis. Office of Inspector General. July 2006: 1-2.
- ↑ 19.0 19.1 Russo A1, Zappia M, Reginelli A, Carfora M, D'Agosto GF, La Porta M, Genovese EA, Fonio P. “Ankle impingement: a review of multimodality imaging approach.” Musculoskelet Surg. 2013 Aug;97 Suppl 2:S161-8. https://www.ncbi.nlm.nih.gov/pubmed/23949938
- ↑ 20.0 20.1 Konstantinos Tsitskaris, Rowland Illing, Charles House, and Michael J Oddy “Osteoid osteoma as a cause of anterior ankle pain in a runner” BMJ Case Rep. 2014. http://casereports.bmj.com/content/2014/bcr-2014-204365.abstract
- ↑ Wiegerinck JI, Vroemen JC, van Dongen TH, Sierevelt IN, Maas M, van Dijk CN. The posterior impingement view: an alternative conventional projection to detect bony posterior ankle impingement. Arthroscopy. 2014;30(10):1311-1316. doi:10.1016/j.arthro.2014.05.006
- ↑ Paul G. Talusan, MD, Jason Toy, MD, Joshua L. Perez, Matthew D. Milewski, MD, John S. Reach, Jr, MSc, MDAnterior Ankle Impingemeproprexnt: Diagnosis and Treatment: J Am Acad Orthop Surg 2014;22: 333-339
- ↑ 23.0 23.1 Liu S, Nuccion S, Finerman G. Diagnosis of anterolateral ankle impingement: comparison between magnetic resonance imaging and clinical examination. American Journal of Sports Medicine [serial online]. May 1997;25(3):389-393. Available from: CINAHL Plus with Full Text, Ipswich, MA. Accessed July 15, 2011.
- ↑ Molloy S, Solan M, Bendall S. Synovial impingement in the ankle: a new physical sign. Journal of Bone Joint Surgery, British Volume [serial online]. April 2003;85B(3):330-333. Available from: CINAHL Plus with Full Text, Ipswich, MA. Accessed July 15, 2011
- ↑ Albisetti W, Ometti M, Pascale V, De Bartolomeo O. Clinical evaluation and treatment of posterior impingement in dancers. American Journal of Physical Medicine Rehabilitation [serial online]. May 2009;88(5):349-354. Available from: CINAHL Plus with Full Text, Ipswich, MA. Accessed July 18, 2011
- ↑ Coull R, Raffiq T, James LE, Stephens MM. Open treatment of anterior impingement of the ankle. J Bone Joint Surg Br. 2003;85(4):550-553. doi:10.1302/0301-620x.85b4.13871
- ↑ 27.0 27.1 27.2 Murawski C, Kennedy J. Anteromedial impingement in the ankle joint: outcomes following arthroscopy. American Journal of Sports Medicine [serial online]. October 2010;38(10):2017-2024. Available from: CINAHL Plus with Full Text, Ipswich, MA. Accessed July 9, 2011.
- ↑ 28.0 28.1 Galla M, Lobenhoffer P. Technique and results of arthroscopic treatment of posterior ankle impingement. Foot Ankle Surgery (Elsevier Science) [serial online]. June 2011;17(2):79-84. Available from: CINAHL Plus with Full Text, Ipswich, MA. Accessed July 2, 2011.
- ↑ Meislin R, Rose D, Parisien J, Springer S. Arthroscopic treatment of synovial impingement of the ankle. American Journal of Sports Medicine [serial online]. March 1993;21(2):186-189. Available from: CINAHL Plus with Full Text, Ipswich, MA. Accessed July 9, 2011.
- ↑ 30.0 30.1 Hussan A. Treatment of anterolateral impingements of the ankle joint by arthroscopy. Knee Surg Sports Traumatol Arthrosec. 2007; 15:150-1154. Accessed July 15,2011.
- ↑ 31.0 31.1 Yasui, Youichi, et al. "Posterior ankle impingement syndrome: A systematic four-stage approach." World Journal of Orthopedics 7.10 (2016): 657. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5065672/ (Level of Evidence: 2a)
- ↑ Coetzee J, Ebeling P. Arthroscopic Ankle Debridement Rehabilitation Protocol Website. Available at: http://www.tcomn.com/images/wmimages/onlineforms/Arthroscopic_Ankle_Debridement.pdf. Accessed July 15, 2011.
- ↑ McClinton, S. Regis University. Ankle impingement sydromes: diagnosis and treatment. Available at: https//connect.regis.edu/p38686942/. Accessed on July 9, 2011.
- ↑ Eils E, Schröter R, Schröder M, Gerss J, Rosenbaum D. Multistation proprioceptive exercise program prevents ankle injuries in basketball [published correction appears in Med Sci Sports Exerc. 2011 Apr;43(4):741]. Med Sci Sports Exerc. 2010;42(11):2098-2105. doi:10.1249/MSS.0b013e3181e03667
- ↑ Mattacola CG, Lloyd JW. Effects of a 6-week strength and proprioception training program on measures of dynamic balance: a single-case design. J Athl Train. 1997;32(2):127-135.
- ↑ Verhagen E, van der Beek A, Twisk J, Bouter L, Bahr R, van Mechelen W. The effect of a proprioceptive balance board training program for the prevention of ankle sprains: a prospective controlled trial. Am J Sports Med. 2004;32(6):1385-1393. doi:10.1177/0363546503262177
- ↑ Smith BI, Docherty CL, Simon J, Klossner J, Schrader J. Ankle strength and force sense after a progressive, 6-week strength-training program in people with functional ankle instability. J Athl Train. 2012;47(3):282-288. doi:10.4085/1062-6050-47.3.06
- ↑ Baker AG, Webright WG, Perrin DH. Effect of a “T-band” kick training protocol on postural sway. Journal of Sport Rehabilitation 1998;7:122–7
- ↑ 39.0 39.1 W. Albisetti, M. Ometti, V. Pascale, O. De Bartolomeo “Clinical Evaluation and Treatment of Posterior Impingement in Dancers.” American Journal of Physical Medicine and Rehabilitation 2008; 88:349–354. http://journals.lww.com/ajpmr/Abstract/2009/05000/Clinical_Evaluation_and_Treatment_of_Posterior.1.aspx
- ↑ Reischl SF, Noceti-Dewit LM. Current Concepts of Orthopaedic Physical Therapy. 2nd ed. The goot and ankle: Physical therapy patient management utilizing current evidence. APTA Independent Study Guide 16.2.11.
- ↑ Sasadai, Junpei, et al. "The Effect of Ankle Taping to Restrict Plantar Flexion on Ball and Foot Velocity During an Instep Kick in Soccer." Journal of sport rehabilitation 24.3 (2015)