Achilles Rupture
Original Editors - Sam Verhelpen as part of the Vrije Universiteit Brussel Evidence-based Practice Project
Top Contributors - Yannick Goubert, Sam Verhelpen, Kim Jackson, Thorvald De Saeger, Rachael Lowe, Mariam Hashem, Shaimaa Eldib, Admin, Nick Libotton, Daphne Dörge, Uchechukwu Chukwuemeka, Tarina van der Stockt, Andeela Hafeez, Lucinda hampton, Lynn De Saegher, Magdalena Hytros, Wanda van Niekerk, Sweta Christian, 127.0.0.1, Yelena Gesthuizen, Evan Thomas, Oyemi Sillo, Claire Knott, Jess Bell, Olajumoke Ogunleye, Robin Tacchetti, Alexandre Lheureux, Franca Ebomah, Kardelen Aktas, WikiSysop, Vidya Acharya, Naomi O'Reilly, Daphne Jackson and Mandy Roscher
Introduction[edit | edit source]
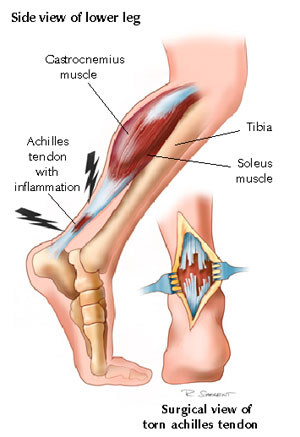
The Achilles Tendon is the strong fibrous band that attaches the calf muscles to the calcaneus bone.
- A rupture of the Achilles Tendon (ATR) is a common pathology being the most commonly ruptured tendon in the human body.[1] [2]
- Achilles tendinopathy has a detrimental effect on physical and mental well-being[3][4].
- The main causes of the rupture can be: overstretching of the heel during recreational sports; a forceful plantar flexion of the heel; or a fall from a height[5].
Clinically Relevant Anatomy[edit | edit source]
The Achilles Tendon
- Longest and strongest tendon in the whole human body and consists of strong, inelastic fibrous connective tissue.[6]
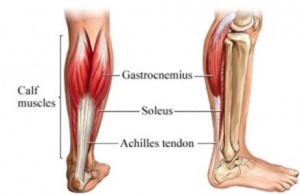
- Is the insertion of the soleus and gastrocnemius muscles and connects these muscles to the calcaneal tuberosity.
- The calf muscle is the main plantar flexors of the ankle.
Epidemiology[edit | edit source]
There has been a rise in the numbers of Achilles Tendon ruptures over the years [7]that have been associated with the increased numbers of obesity and of recreational sports[8].
- The incidence is 7 per 100 000 per year but goes up to 15 to 25 per 100 000 per year for (recreational) athletes, with a peak incidence at the age of 30 to 50 years[9][10].
- It affects mostly 'middle-aged weekend warriors' but this aetiology accounts for only about 70% of such injuries.
- An Achilles Tendon rupture occurs more frequently among men than women[11].
Aetiology[edit | edit source]
The inherent characteristics, function, and blood supply of the Achilles Tendon predispose it to both acute and chronic rupture.
- In the situation of an acute rupture, patients are usually engaged in athletic activities[11], accounting for 68 % of injuries[12].
- It is common in stop-and-go sports such as badminton, soccer, volleyball, basketball, tennis, racquetball, squash as eccentric movement puts an enormous amount of stress on the tendon.
There are some conditions that predispose to rupture with research suggesting that injuries in this patient population are more likely to be missed on first examination[12]. These include:
- The natural ageing process[12].
- Participation in recreational sports
- Obesity[12].
- Use of some commonly prescribed medications such as fluoroquinolone and steroids.
- Poor running mechanics.
- Altered biomechanics such as flat foot (pes planus), high foot arch (pes cavus), and leg length discrepancy.
Characteristics/Clinical Presentation:[edit | edit source]
Three categories of indirect injury that may result in rupture are[5]:
- Pushing off with a weight-bearing forefoot while also extending the knee, as occurs at the beginning of a sprint, running, and some forms of jumping
- Sudden and unexpected dorsiflexion of the ankle, which may occur when a person slips off a chair or a ladder, when stumbling into a hole, or suddenly falling forward
- Violent dorsiflexion of a plantar-flexed foot when one falls from a height.
A complete rupture of the Achilles Tendon will show the following characteristics:
- At the moment of rupture, the sharp pain will be felt as if the patient was stabbed in the heel with a dagger[13][14][15][1][16][9].
- Often the rupture will coincide with a loud crack or pop sound.[13][16]
- When palpating the tendon, a gap may be felt.[13][14][15]
- The back of the heel will be swollen.[13][14][15]
- Decreased active plantar flexion of the ankle.[9]
- Increased passive dorsiflexion
- Inability to heel raise
- Impaired gait
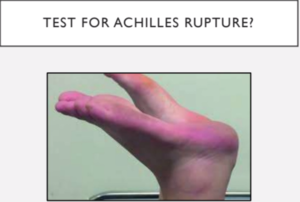
- A positive outcome of the calf muscle squeeze test or Thompson Test.
- Some patients will have a history of tendinopathy in the heel or a prior cortisone injection.[13][14][15]
Chronic Presentation (32% of injuries)[12]
- In most of the available literature, an Achilles Tendon rupture is described as chronic if it occurs at least 4 to 6 weeks after injury[5]. The symptoms of chronic Achilles Tendon rupture include pain, decreased strength, fatigue, and ankle stiffness.[17] A correct distinction needs to be made because the treatments differ.
Differential Diagnosis[edit | edit source]
- Acute Achilles Tendon peritendinitis
- Gastrocnemius tear
- Calf muscle strain or rupture
- Posterior tibialis stress syndrome
- Fracture
- Posterior tibialis tendon injuries
- Peroneal injuries
Classification[edit | edit source]
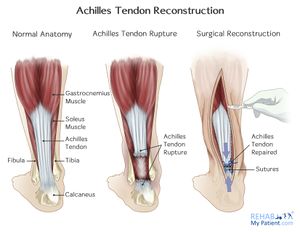
Achilles tendon tears have traditionally been grouped into 4 types[18] according to the severity of the tear and degree of retraction - management often related to this type of classification:
- Type I: partial ruptures ≤50% - was typically treated with conservative management
- Type II: complete rupture with tendinous gap ≤3 cm - was typically treated with end-end anastomosis
- Type III: complete rupture with tendinous gap 3 to 6 cm - often required tendon/synthetic graft
- Type IV: complete rupture with a defect of >6 cm (neglected ruptures) - often required tendon/synthetic graft and gastrocnemius recession.
However, as Helene Simpson[19] notes, the latest research suggests that we cannot base our management decisions on the size of a tear or gap. She notes that whenever an Achilles tendon has a tear, we should treat the tendon as if 100% of the fibres are gone regardless of the actual size of the gap or the percentage of the fibres involved. Decisions regarding surgery or conservative management are guided by a number of factors beyond the size of a gap, including the patient's medical history, their level of activity, affordability etc.[19]
Examination[edit | edit source]
Observation[edit | edit source]
For the inspection of an Achilles Tendon rupture, the therapist may observe the patient in several positions:
- Standing - to look for fallen arches (flat feet) and other postural complications.
- Laying - usually on the front. This can be used to observe the tendon more closely for thickening, redness, swelling, and nodules.
- Walking and running - to look for overpronation.
- Swelling: a swollen ankle can point to a rupture of the Achilles Tendon.
Palpation[edit | edit source]
The Achilles Tendon is easily palpable. When palpating along the entire length of the tendon, a gap may be present.
Active Movements[edit | edit source]
In this part of the examination, the therapist asks the patient to fulfil some active movements which can aid in the diagnosis of a tendon rupture.
There are several active movements:
- Observing the gait pattern can be an important indication for a possible rupture. A patient with an Achilles Tendon rupture can possibly not make a plantar flexion of his ankle. So if the plantar flexion movement in the walking phase is hindered and painful, it can be an indication of an Achilles rupture. A patient with an Achilles rupture will show over-pronation of the injured ankle. The patient will also show a lack of push-off at the end of the stance phase as a result of the dysfunction of the Gastrocnemius and Soleus muscles.
- Instructing the patient to stand on his/her toes for making a plantar flexion. This will be impossible if the patient has an Achilles Tendon rupture.
- Ask the patient to actively plantarflex the ankle.
- Every active movement containing a plantar flexion of the heel will be almost, if totally not impossible.
Special Tests[edit | edit source]
There exist several special tests for the observation of an Achilles Tendon rupture:
- Thompson Test - this test is especially useful for diagnosing complete Achilles tendon ruptures and less useful for the diagnosis of partial Achilles Tendon rupture.
- Matles Test - the patient lies in a prone position and is asked to actively flex the knee through 90 degrees. The therapist observes the feet and ankles throughout the movement. The test is negative when the foot displays slight plantarflexion; the test is positive if the footfalls into the neutral position or the movement result in dorsiflexion. Maffulli reports a sensitivity of 0.88 [1] and considered the most reliable test [19].
- Achilles Tendon Total Rupture (ATR-score) - the Achilles Tendon rupture-score is an important questionnaire that refers to the limitations/difficulties a patient with a tendon rupture will face. [20][9]
- Realtime Achilles ultrasound Thompson test - this test is as the Thompson test, but under ultrasound visualisation. It can be used by surgeons with minimal training in ultrasonography. It provides improved diagnostic characteristics compared with static ultrasound. [13]:
The reason Achilles Tendon rupture is often missed in the emergency department is because the squeeze test and ultrasound imaging were found to be not reliable in the diagnosis. Matles test is considered to be the most reliable test[19].
Outcome Measures[edit | edit source]
The outcome measures used to evaluate functional results following an Achilles Tendon rupture can be broadly divided into two types:
- Objective measures: parameters directly registered by the physiotherapist, such as ankle range of motion (ROM) or calf muscle strength measurements. These objective data, derived from the patient’s physical examination, have traditionally formed the basis of functional assessment following an Achilles Tendon rupture.[16][14][20]
- Patient-reported measures: over the past two decades, it has become increasingly recognized that the patient’s own appraisal of outcome is of the most important when judging the results of treatment[20].
The best choice of outcome tools for reporting the results of treatment in patients with foot and ankle disorders remains uncertain and controversial. Nevertheless, on the basis of the available evidence, a patient treated for an Achilles Tendon rupture should be assessed with a disease-specific measure, such as the
- ATRS[20][9] in combination with a generic measure, such as the SF-36 [17][13].
- The 36-item Short Form (SF-36) is a commonly used instrument for measuring the Health-Related Quality of Life, it is a valid and reliable tool. The SF-36 has been proven useful in monitoring population health, estimating the burdens of different diseases, monitoring outcomes in clinical practice, and evaluating medical treatment effects.[13]
- These patient-reported outcome scales focus on the patient’s perception of his/her health status, which has to be considered as the most important indicator of the success of treatment.
- Patient-reported outcome scales should be complemented by objective indicators of function, such as muscle strength [1][5], calf muscle endurance [21] and return to previous activity level, in order to obtain a complete picture of the effect of the treatment[20]
Management[edit | edit source]
There is still considerable controversy as the most optimal treatment plan. The Debate is about nonoperative vs surgical repair for acute ruptures, minimally invasive vs traditional open repair, and early functional rehabilitation protocols instead of a more traditional rehabilitation program are only a few of the arguments that continue to exist in the realm of treatment.
Historically, interventions have been dependent on personal factors such as age, desire to return to sport and individual preference[22]. An operative repair was considered to reduce the risk of a future re-rupture by sewing the torn ends of the injured Achilles Tendon together followed by immobilisation in a plaster of Paris from 6 up to 12 weeks depending on the used surgical technique, but wound infection presented a possible complication such as scar adhesions, loss of sensation, deep vein thrombosis (DVT), and infection. Therefore younger persons were recommended to choose the operative repair[23][24] and elderly, patients with co-morbidities such as diabetes, and peripheral neuropathies, and less active patients were recommended a conservative approach with immobilisation in a cast.
Post surgically, early weight-bearing and early ankle mobilisation are now widely accepted[25]. However more recently, it has been demonstrated that a conservative and accelerated functional rehabilitation approach is more effective than a surgical approach[26][27].
Wu et al[26], showed that when functional rehabilitation was used, the effect of a non-surgical intervention was similar to surgical treatment regarding the incidence of a range of motion deficit, a future chance of re-rupture, calf circumference and functional outcomes and also the incidence of other complications was reduced. Willits et al found all measured outcomes of nonoperative treatment with a functional rehabilitation protocol were acceptable and were clinically similar to those for operative treatment, in addition, this study suggests that the application of an accelerated-rehabilitation nonoperative protocol avoids serious complications related to surgical management[27].
Surgical Management[edit | edit source]
There are a variety of approaches to the surgical management of this injury and contention exists over the surgical approach (open or percutaneous)[28]. There is a difference between surgery for chronic and acute Achilles Tendon rupture.
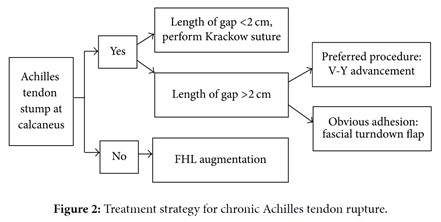
Chronic Achilles Tendon rupture[edit | edit source]
By evaluating the presence or absence of Achilles Tendon stumps and the gap length of the rupture, different surgical options (V-Y advancement, gastrocnemius fascial turndown flap, Plantaris tendon removal, and Achilles Tendon scraping[29] or Flexor hallucis longus tendon transfer) can be selected for tendon repair.
Acute Achilles Tendon rupture[edit | edit source]
Due to a high complication rate after open surgical repair, including wound infection, abnormal sensation, adhesion and thrombosis new techniques which require much smaller incisions have been developed. Minimal invasive techniques and percutaneous repair become more and more common because they reduce complications and have both a good outcome.
Read more about surgical management on this page
Sural Nerve entrapment in the stitching and Tibial nerve involvement are common complications following surgical, specifically endoscopic operations.
- Patients complain of pain often on the lateral side of the ankle in the early post-operative rehabilitation.
- Neural assessment can help you to determine the nature of pain. Often this pain settles in time but it's important not to ignore it to avoid further complications[19].
Management[edit | edit source]
Evidence suggests good outcomes with conservative management of ruptured Achilles[30]. Studies found out with conservative management that strength of the tendon was very comparable with operative treatment and also low re-rupture rate provided that the rupture was identified early within 48 hours of injury.
Between 2011 and 2017 a number of meta-analyses investigating the evidence of Achilles rupture conservative management were published [31] [32]. The findings of these studies found the key to successful outcomes was early rehabilitation and early mobilisation. So when we compare surgery to the conservative regime, it's whether or not early rehabilitation was included.[19]
The aim of non-operative means of treatment is to restore and maintain contact between the two ends of the ruptured Achilles Tendon to facilitate healing. Conservative treatment regimens vary greatly but commonly involve immobilisation with rigid casting or functional bracing. Gulati et al[28] describe the conservative approach to be this, "the foot is initially placed in full equinus (30° namely full plantarflexion). The foot is then brought into neutral sequentially over a period of 8-12 wk. Once ankle position permits it, weight-bearing is allowed. There is currently no clinical consensus on whether the cast should extend above the knee or if a below-knee cast is sufficient".[28]
Conservative - Accelerated Functional Rehabilitation Approach[edit | edit source]
Regardless of the depth and size of rupture, if the patient is compliant and agrees to follow early mobilisation strictly conservative management is advisable[19].
Despite the increasing supported for accelerated rehabilitation regimes both in surgical and non-surgical situations, there is still no consensus regarding the most preferable protocol, time of start and type of exercises[33].
Physiotherapy interventions should be all avoided for the first two weeks while the patient is asked to avoid any kind of dorsiflexion and immobilise their foot in a boot or plaster of Paris in 30 ° plantar flexion[19]. Weight-bearing is advised to be avoided in the first two weeks.
However, in some cases, depending on the condition of the surgical treatment, the patient may start to lose approximately 5 kg of weight with a 30 degree plantar flexion boot within 24 hours after surgery. This weight is carried out by pressing on the scale under the supervision of a doctor. Afterwards, the patient can get ready for physical therapy with crutches and boots, with enough support to 'balance'. Quadriceps isometric exercises from the 24-hour period after surgery (due to the tendency of the quadriceps muscle to lose tone quickly). This period is managed with ankle pumping exercises (to prevent edema formation and reduce the resulting edema) and 15 minutes of cold applications every 2 hours.
After two weeks, the patients are encouraged to take their boot off for five minutes every hour or two to do specific exercises. The emphasis is on improving plantar flexion mobility and gradually improving the strength into plantarflexion at this stage. Dorsi-flexion stretches, and neutral position are still not allowed.
Week 4-week 8: gradually lower the wedge of the boot inserted until the foot reaches neutral at week 10 depending on the surgical technique and the presence of co-morbidities.[19]
Early rehabilitation principals:
- Strengthening the foot core
- Avoiding Achilles Tendon stretch: a slightly tight tendon at the end of week 8-10 is much better than overlengthened tendon that doesn't generate sufficient energy and can possibly put the patient at risk of re-rupture[19]
- Gait re-education; looking through all the Lower limb joints and correcting any faulty pattern such as knee hyperextension and reduced Gluteal activation.
- Plantar flexion Strengthening: by isometric and sustained heel raises starting on both legs then slowly progressing on a single leg. Holding on one leg and lowering down on the other. Once the patient is able to perform heel raises on one leg throughout the ROM in a controlled manner you can start working on the endurance by doing four sets of six up to 24 repetitions or up to twenty repetitions in am minute[19]. Progress into eccentric loading by doing heel raises off the edge of a box. This can help to build up the tension and the strength In the tendon.
Running and fast walking can be introduced when the patient can comfortably do a single heel raise[19].
Tibialis Posterior work with Tibialis Anterior and the Peroneal muscles to maintain the foot core strength when progressing into a single-leg stance during the gait. If they are not working properly, the Achilles tendon and the calf muscle will be overloaded.
With conservative management, it's recommended to see your patient once a week to follow up and encourage commitment to the early rehabilitation and exercises for better outcomes. Unlike surgical treatment where the patient gets six then 12 weeks follow-ups to remove the boot.
Rehabilitation doesn't end the minute the patient can get their heel off the ground. An assessment of the patient's function, return to work, and return to sports of applicable should follow. It's recommended to follow up with your patient for 12 months
The re-rupture is highly evident in the first year but it can happen later so you want to make sure your patient is fit and integrated into his normal lifestyle.
Post-surgical protocols which promote early weight-bearing and mobilisation have been developed by Brumann et al[34]and Braunstein et al[35].
See the following protocols:
Traditional Approach[edit | edit source]
Rehabilitation depends on the initial management approach taken - surgical or non-surgical. However, the patient will normally wear a plaster cast for immobilisation or a below-knee dorsal brace which allows the ankle to make a plantar flexion to start early mobilisation. After the cast or brace is removed rehabilitation is mainly focused on firstly improving the range of movement of the ankle, later it is focused on increasing the muscle strength and muscle coordination. A return to activities should be expected at 4-6 months of therapy, but the rate of rehabilitation greatly depends on the quality of the treatment and the motivation of the patient.
In general physical therapy can start immediately with general exercises for the affected lower limb:
Once the cast or brace is removed, start with gentle passive mobilisation of the ankle and the subtalar joints and active ROM exercises. After two weeks of physiotherapy, progressive resistance exercises are added. Possible exercises for the patient are
- Active flexion/extension of the ankle
- Ankle circles (clockwise and counterclockwise)
- Hip abduction
- Straight leg raise
- Standing hamstring curl
- Cycling on a stationary bicycle
8-12 Weeks After Surgery[edit | edit source]
Gait training exercises can be started, followed by activity-specific movements. The patient can start with Theraband exercises by starting from the lowest resistance and work up from there for regaining strength. The patient should also continue with the previous exercises.
- Ankle range of motion: plantarflexion and dorsiflexion to 90°: 2 x 8 repetitions
- Ankle range of motion: inversion and eversion
- Ankle range of motion: pronation and supination: 2 x 8 repetitions
- One leg standing balance exercise : 3 × 30 seconds
- Standing heel-rise (2 × 3 seconds tempo) : 3 × 10 repetitions
12-24 Weeks After Surgery[edit | edit source]
The first set of exercises can now be executed with ankle weights. The following exercises can be added to the training program, but also basic exercises (described above) should still be executed :
- Calf stretch
- Heel raises
- Single leg balancing
- Walk on toes with support to start with (if needed): 2 × 5 meters
- Standing heel-rise is performed with increased weight on injured leg: 5 × 10 repetitions
- Heel-rise in a supine position with flexed legs (with increased weight on the injured leg): 2 × 15 repetition
- Leg press with one leg at a time (10 repetitions maximum): 2 × 10 repetitions
- Balance exercises on a trampoline: 2 × 45 seconds
- Walk/jog on a trampoline: 2 × 45 seconds
- Cross trainer: 1 min and 45 seconds
- Lunges (only with injured leg in front): 2 × 10 repetitions
Starting From Week 14 Until the End of the Therapy[edit | edit source]
The patient is able to run approximately 14 weeks after the injury or surgery (always consider the guidance of the surgeon!).
- Running on even ground is allowed when the patient can perform 5 single-legged heel-rises with approximately 90% of the height of the uninjured leg.
- Jogging upwards on stairs is allowed if the patient can walk 5 meters on their toes without the heel falling down.
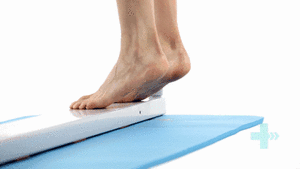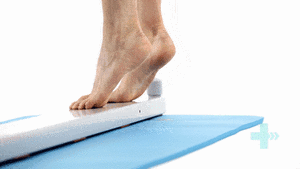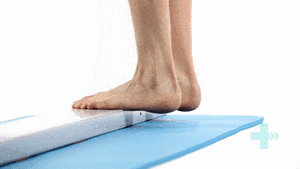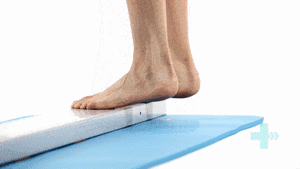
The last step after surgery is eccentric exercise. During the eccentric part (lowering the heel), the patient has full weight on the injured foot, and during the concentric part (raising on tiptoe) only the non-injured foot is used [13].
- The patient takes place on a step, standing with full body weight on the forefoot of both feet, the knees are extended. Then he is asked to go stand on his/her toes and to raise the non-injured leg so that his/her body weight is on his injured leg. Now the patient slowly lowers the heel. In this way, the calf muscle eccentrically guides the motion and is eccentrically trained.
- When the patient can perform this exercise without discomfort, he/she can increase the load by adding books or other weight to a backpack or to perform the exercise with a flexed knee.
When treated with an eccentric training program, the patient is more likely to be able to return faster to sport. The eccentric exercises should reduce pain and tendon thickness and should improve the function of the tendon (and muscles). The eccentric calf-muscle exercises, as described below, should be executed twice daily for 12 weeks. The exercise program consists of 1-3sets of 15 repetitions per exercise, according to the improvement of the patient[13].
But not all patients benefit equally from an eccentric exercise program. It’s also proven that these exercises are less effective in sedentary people in comparison to athletes[15].
End of the Therapy[edit | edit source]
- After completing the rehabilitation program, a new examination of the tendon healing and functions is required
- If needed, a new referral for further physiotherapy sessions can be provided to the patient.
- Gradual return to sports is recommended. For example, before participating to contact sports, the patient should wait at least 6–9 months after the injury[16][27].
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 Maffulli N, Longo UG, Gougoulias N, Denaro V. Ipsilateral free semitendinosus tendon graft transfer for reconstruction of chronic tears of the Achilles tendon. BMC musculoskeletal disorders. 2008 Dec;9(1):1-9.
- ↑ Utashima D, Matsumura N, Suzuki T, Iwamoto T, Ogawa K, Park D, Kwon Y, Lim C, Cho TJ, Shin CH, Choi IH. Treatment of acute Achilles tendon rupture. Clinics in Orthopedic Surgery. 2020 Mar;12(1):1-8.
- ↑ Ceravolo ML, Gaida JE, Keegan RJ. Quality-of-life in achilles tendinopathy: an exploratory study. Clinical Journal of Sport Medicine. 2020 Sep 1;30(5):495-502.
- ↑ Morgan GE, Martin R, Williams L, Pearce O, Morris K. Objective assessment of stiffness in Achilles tendinopathy: a novel approach using the MyotonPRO. BMJ open sport & exercise medicine. 2018 Nov 1;4(1):e000446.
- ↑ 5.0 5.1 5.2 5.3 Flint JH, Wade AM, Giuliani J, Rue JP. Defining the terms acute and chronic in orthopaedic sports injuries: a systematic review. The American journal of sports medicine. 2014 Jan;42(1):235-41.
- ↑ Tarantino D, Palermi S, Sirico F, Corrado B. Achilles tendon rupture: mechanisms of injury, principles of rehabilitation and return to play. Journal of functional morphology and kinesiology. 2020 Dec 17;5(4):95.
- ↑ Myhrvold SB, Brouwer EF, Andresen TK, Rydevik K, Amundsen M, Grün W, Butt F, Valberg M, Ulstein S, Hoelsbrekken SE. Nonoperative or Surgical Treatment of Acute Achilles’ Tendon Rupture. New England Journal of Medicine. 2022 Apr 14;386(15):1409-20.
- ↑ Kauwe M. Acute Achilles tendon rupture: clinical evaluation, conservative management, and early active rehabilitation. Clinics in podiatric medicine and surgery. 2017 Apr 1;34(2):229-43.
- ↑ 9.0 9.1 9.2 9.3 9.4 American college of foot and ankle surgeons/ foot health artikel. Achilles Tendon Rupture (2016 ). Available from: https://www.foothealthfacts.org/conditions/achilles-tendon-rupture (Accessed 19 April 2020) (level of evidence: 2)
- ↑ De Jonge S, Van den Berg C, De Vos RJ, Van Der Heide HJ, Weir A, Verhaar JA, et al. Incidence of midportion Achilles tendinopathy in the general population. Br J Sports Med. 2011;45(13):1026-8.
- ↑ 11.0 11.1 Vosseller JT, Ellis SJ, Levine DS, Kennedy JG, Elliott AJ, Deland JT, et al. Achilles tendon rupture in women. Foot & ankle international. 2013;34(1):49-53. (level of evidence: 2)
- ↑ 12.0 12.1 12.2 12.3 12.4 Raikin SM, Garras DN, Krapchev PV. Achilles tendon injuries in a United States Population. Foot Ankle Int. 2013;34:475–480. doi: 10.1177/1071100713477621.(level of evidence: 2A)
- ↑ 13.0 13.1 13.2 13.3 13.4 13.5 13.6 13.7 13.8 13.9 Maffulli N. Rupture of the Achilles tendon. J Bone Joint Surg Am.1999;81(7):1019-36. (level of evidence: 2A)
- ↑ 14.0 14.1 14.2 14.3 14.4 Saglimbeni A, Fulmer C. Achilles tendon injuries and tendonitis. Medscape 2009. Available from: http://emedicine.medscape.com/article/309393-overview [accessed 29 May 2014] (level of evidence: 2)
- ↑ 15.0 15.1 15.2 15.3 15.4 Jacobs B, Lin D, Schwartz E. Achilles tendon rupture. Medscape 2009. Available from: http://emedicine.medscape.com/article/85024-overview [accessed 29 May 2014] (level of evidence: 2)
- ↑ 16.0 16.1 16.2 16.3 Gravlee J, Hatch R. Achilles tendon rupture: a challenging diagnosis. J Am Board Fam Med. 2000;13(5): 371-373 (level of evidence: 2)
- ↑ 17.0 17.1 Kingsley P. Achilles tendon rupture in atypical patient populations. Emerg Nurse. 2016;23(10):34–37. doi:10.7748/en.23.10.34.s24
- ↑ Kuwada GT. Classification of tendo Achillis rupture with consideration of surgical repair techniques. J Foot Surg. 1990;29 (4): 361-365.
- ↑ 19.00 19.01 19.02 19.03 19.04 19.05 19.06 19.07 19.08 19.09 19.10 19.11 Simpson H. Achilles Tendon Rupture Management Course. Plus, 2020.
- ↑ 20.0 20.1 20.2 20.3 20.4 Berkson E. Achilles tendon rupture. Quincy medical center. 2008. Available from: http://achillesblog.com/files/2008/03/achilles_tendon_rupture_mass_gen.pdf (Accessed 21 April 2020) (level of evidence: 2)
- ↑ Sman AD, Hiller CE, Imer A, Ocsing A, Burns J, Refshauge KM. Design and Reliability of a Novel Heel Rise Test Measuring Device for Plantarflexion Endurance. Biomed Res Int. 2014; 2014: 391646. Doi: 10.1155/2014/391646
- ↑ Metzl JA, Ahmed CS, Levine WN. The ruptured Achilles tendon: operative and non-operative treatment options. Curr Rev Musculoskelet Med. 2008; 1:161–164 (level of evidence: 1)
- ↑ Lewis N, Quitkin HM. Strength analysis and comparison of the Teno fix tendon repair system with the two-strand modified Kessler repair in the Achilles tendon. Foot Ankle Int. 2003;24(11):857–60 (level of evidence: 2)
- ↑ Lansdaal JR, Goslings JC, Reichart M, Govaert GA, van Scherpenzeel KM, Haverlag R, et al. The results of 163 Achilles tendon ruptures treated by a minimally invasive surgical technique and functional after treatment. Injury. 2007;38(7):839–44. (level of evidence: 2)
- ↑ Brumann M, Baumbach SF, Mutschler W, Polzer H. Accelerated rehabilitation following Achilles tendon repair after acute rupture–Development of an evidence-based treatment protocol. Injury. 2014;45(11):1782-90. (level of evidence: 1)
- ↑ 26.0 26.1 Wu Y, Lin L, Li H, Zhao Y, Liu L, Jia Z, et al. Is surgical intervention more effective than non-surgical treatment for acute Achilles tendon rupture? A systematic review of overlapping meta-analyses. International Journal of Surgery. 2016; 36(Pt A):305-311. Doi: 10.1016/j.ijsu.2016.11.014 (level of evidence: 1)
- ↑ 27.0 27.1 27.2 Willits K, Amendola A, Bryant D, Mohtadi NG, Giffin JR, Fowler P, et al. Operative versus nonoperative treatment of acute Achilles tendon ruptures: a multicenter randomized trial using accelerated functional rehabilitation. JBJS. 2010;92(17):2767-75. (level of evidence: 1b)
- ↑ 28.0 28.1 28.2 Gulati V, Jaggard M, Al-Nammari SS, Uzoigwe C, Gulati P, Ismail N, et al. Management of achilles tendon injury: a current concepts systematic review. World journal of orthopedics. 2015;6(4):380. (level of evidence: 1)
- ↑ Masci L, Spang C, van Schie HT, Alfredson H. Achilles tendinopathy—do plantaris tendon removal and Achilles tendon scraping improve tendon structure? A prospective study using ultrasound tissue characterisation. BMJ open sport & exercise medicine. 2015;1(1):e000005.
- ↑ Zhang H, Tang H, He Q, Wei Q, Tong D, Wang C, Wu D, Wang G, Zhang X, Ding W, Li D. Surgical versus conservative intervention for acute Achilles tendon rupture: a PRISMA-compliant systematic review of overlapping meta-analyses. Medicine. 2015 Nov;94(45).
- ↑ Willits K, Amendola A, Bryant D, Mohtadi NG, Giffin JR, Fowler P, Kean CO, Kirkley A. Operative versus nonoperative treatment of acute Achilles tendon ruptures: a multicenter randomized trial using accelerated functional rehabilitation. JBJS. 2010 Dec 1;92(17):2767-75.
- ↑ Erickson BJ, Mascarenhas R, Saltzman BM, Walton D, Lee S, Cole BJ, Bach Jr BR. Is operative treatment of Achilles tendon ruptures superior to nonoperative treatment? A systematic review of overlapping meta-analyses. Orthopaedic Journal of Sports Medicine. 2015 Apr 17;3(4):2325967115579188.
- ↑ Challoumas D, Clifford C, Kirwan P, Millar NL. How does surgery compare to sham surgery or physiotherapy as a treatment for tendinopathy? A systematic review of randomised trials. BMJ Open Sport & Exercise Medicine. 2019;5(1):e000528.
- ↑ Brumann M, Baumbach SF, Mutschler W, Polzer H. Accelerated rehabilitation following Achilles tendon repair after acute rupture-Development of an evidence-based treatment protocol. Injury. 2014; 45: 1782–1790 (level of evidence: 1a)
- ↑ Braunstein M, Baumbach SF, Boecker W, Carmont MR, Polzer H. Development of an accelerated functional rehabilitation protocol following minimal invasive Achilles tendon repair. Knee Surgery, Sports Traumatology, Arthroscopy. 2015;26:846–853 (level of evidence: 2a)