Polyarteritis Nodosa
Original Editors - Josh Bixler from Bellarmine University's Pathophysiology of Complex Patient Problems project.
Top Contributors - Josh Bixler, Lucinda hampton, Admin, Kim Jackson, Elaine Lonnemann, Sehriban Ozmen, 127.0.0.1, Laura Ritchie, Wendy Walker, Mariam Hashem and WikiSysop
Introduction[edit | edit source]
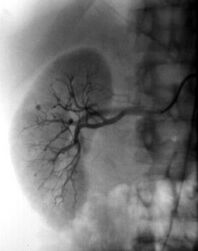
Polyarteritis nodosa (PAN) is a systemic inflammatory necrotising vasculitis involving small to medium-sized arteries.[1] The inflammation, which affects the entire arterial wall, typically manifests where the arteries branch and ultimately the affected vessel tissues become necrotic.[2][3] As the outer and inner layers of the artery swell, blood clots can form and potentially damage various organs and tissues in the body such as the liver, kidneys, heart, GI tract, testes, and muscles.[4] Polyarteritis nodosa left untreated is usually fatal, often due to progressive renal failure or gastrointestinal complications.[1]
Watch this 2 minute video for a good summary PAN.
Etiology[edit | edit source]
The cause of PAN remains unknown, but there does appear to be a link to drug reactions, viral infections, and the body's immune system. Adverse drug reactions to iodide or pencillin, or indiviudals with active hepatitis B or C appear to be at a higher risk for developing this disease.[3]
Epidemiology[edit | edit source]
- More common in males and usually occurs in 5th to 7th decades.
- 20-30% of patients are hepatitis B antigen positive.
Characteristics/Clinical Presentation[edit | edit source]
Patients can present with systemic and/or focal symptoms.
- Systemic signs and symptoms are usually non-specific, including fever, malaise and weight loss.
- Localised symptoms are due to ischaemia and infarction of affected tissues and organs, usually renal arteries.
Listed below are some of the most common symptoms associated with this disease, affecting the skin, joints, brain, nerves, heart, digestive tract, liver, and kidneys:
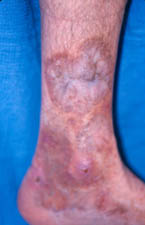
- Rashes with raised patches along arteries, discoloration of fingers or toes, blotches that appear purple[2][6]
- Joint pain and inflammation, muscle aches and pain[2][3]
- Fever, headaches, strokes, seizures[2][3]
- Weakness, numbness, tingling, or hand or foot paralysis[2]
- Angina and myocardial infarctions[2]
- Peritonitis (infection of the abdomen), nausea, vomiting, bloody diarrhea, intestinal tears, and rapid weight loss[2]
- Liver damage and failure[2][3]
- Hypertension, edema, decreased output of urine, urine with high levels of protein[2][6]
Medications[edit | edit source]
Typically corticosteroids and drugs that suppress the immune system are prescribed. One such steroid is prednisone, which allows the affected individual some pain relief and can help stop the disease from causing more damage. Also, to further address the inflammation, cyclophosphamide (immunosuppressant) is often prescribed in combination with the prednisone.[2] If the cause of polyarteritis nodosa is related to a hepatitis infection, and the inflammation has been limited, anti-viral medication along with plasmapheresis is used to combat the infection.[7]
Diagnosis[edit | edit source]
Currently there is not a single gold standard test for diagnosing an individual with PAN, rather a cluster of tests and criteria are used to do so. Patient history, blood testing, biopsies from affected sites, and angiograms are all common procedures used to direct the physician with their diagnosis. [8]
Management[edit | edit source]
Polyarteritis nodosa, fatal if untreated, requires prompt treatment with corticosteroids and/or cyclophosphamide. This treatment may result in remission, and a remission/cure in 90% of patients.[1] If the individual is also affected with hepatitis B, treatment becomes much more complex as these medications can make the hepatitis B infection worse. If hepatitis B is present as well, the current thought is to treat the vasculitis for two weeks using prednisone, and then undergo plasmapharesis while addressing the infection using anti-viral therapy.[9]
Surgery may be necessary if the affected individual present with appendicitis, cholecystitis, pancreatitis, infarction of the digestive tract, hemorrhage, or bowel perforation.[10] Poor outcomes are typically seen with these surgeries with the exception of the procedures for appendicitis or cholecystitis, which have outcomes similiar to those not affected by the disease.[10]
Emerging treatments for PAN:[11]
- Use of intravenous immunoglobulin (IVIG) for those individuals who don't have hepatitis B infection, yet don't respond to conventional treatment.
- Use of anti-tumor necrosis factor (TNF)-alpha therapy for more resistant forms of this disease.
- Use of B-cell therapy for those individuals who don't repsond to the conventional treatment.
- Use of iterferon alfa for those individuals with PAN and the hepatitis B virus in mild/moderate cases.
<span style="display: none;" id="1301761018092S" />
Physical Therapy Management[edit | edit source]
The current best treatment for PAN primarily consists of medical management with the use of the corticosteroids and immunosuppressant drugs. Patients that present in one's clinic with the aforementioned signs and symptoms should be referred to their physician. With the nature of the disease, many systems are affected and currently there is no practice pattern for which PAN falls under in the Guide to Physical Therapy Practice (2nd ed.). However, once the patient is medically stable, a physical therapist can help address limitations the individual may be experiencing due to the multiple system involvement. As PAN affects each individual differently, a physical therapist can work with this patient based on their unique needs, and ultimately towards helping them achieve their personal goals and activities of daily living.
Differential Diagnosis[edit | edit source]
- Other vasculitides for example microscopic polyangiitis.
- Rheumatoid vasculitis
- Systemic lupus erythematosus (SLE)
- Churg-Strauss syndrome[1]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 Radiopedia Polyarteritis nodosa Available:https://radiopaedia.org/articles/polyarteritis-nodosa-1 (accessed 23.1.2023)
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 2.8 2.9 Merck Manual: polyarteritis nodosa. http://www.merckmanuals.com/home/sec05/ch069/ch069b.html (accessed 22 Feb 2011).
- ↑ 3.0 3.1 3.2 3.3 3.4 Cedars-Sinai: polyarteritis nodosa. http://www.cedars-sinai.edu/Patients/Health-Conditions/Polyarteritis-Nodosa.aspx (accessed 22 Feb 2011).
- ↑ Goodman CC, Fuller KS. Pathology: Implications for the Physical Therapist. 3rd edition. St. Louis, Missouri: Saunders Elsevier, 2009.
- ↑ Kote's Medical Animations. Polyarteritis nodosa made easy . Available from: https://www.youtube.com/watch?v=YrOejvJ2WyI [last accessed 23.1.2023]
- ↑ 6.0 6.1 MedlinePlus Medical Encyclopedia: polyarteritis nodosa. http://www.nlm.nih.gov/medlineplus/ency/article/001438.htm (accessed 22 Feb 2011).
- ↑ PubMed Health: polyarteritis nodosa. http://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0002410 (accessed 22 Feb 2011).
- ↑ Lightfoot RW Jr, Michel BA, Bloch DA, Hunder GG, Zvaifler NJ, McShane DJ, et al. The American College of Rheumatology 1990 criteria for the classification of polyarteritis nodosa. Arthritis Rheum 1990;33:1088-93.
- ↑ Johns Hopkins Vasculitis Center: polyarteritis nodosa. http://www.hopkinsvasculitis.org/types-vasculitis/polyarteritis-nodosa (accessed 22 Feb 2011).
- ↑ 10.0 10.1 Guillevin, L. Treatment of classic polyarteritis nodosa in 1999. Nephrol Dial Transplant.1999;14:2077-2079.
- ↑ BMJ Evidence Centre: emerging treatments for polyarteritis nodosa. http://bestpractice.bmj.com/best-practice/monograph/351/treatment/emerging.html (accessed 1 Apr 2011).